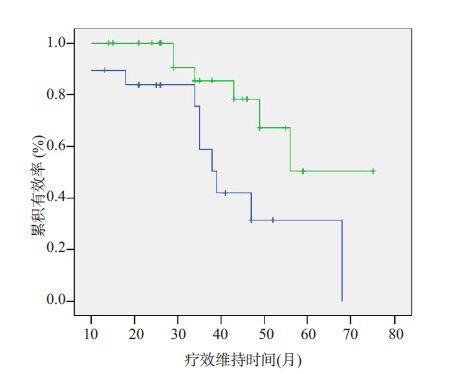
Kaplan-Meier analysis on the long-term effect for patients with patellar dislocation who underwent arthroscopy
-
摘要:
目的使用Kaplan-Meier分析法评价关节镜下复发性髌骨脱位三联修复术远期效果。 方法入选髌骨脱位患者69例髌骨脱位患者随机分为观察组(n=36)及对照组(n=33),分别给予关节镜下三联修复及普通双束解剖重建内侧髌股韧带治疗髌骨脱位。对以上患者进行为期5年的长期随访,比较手术前后外侧髌股角、Lysholm评分及疗效维持情况。 结果治疗前两组外侧髌股角及Lysholm评分均无组间差异(P >0.05);末次随访时,两组患者的外侧髌股角及Lysholm评分均显著大于/高于手术前,观察组上述两者显著大于/高于对照组(P<0.05)。两组分别有3及4例患者删失,删失率无统计学差异(P >0.05)。两组最长疗效维持时间分别为75及68个月;观察组的疗效维持时间的算术均数及中位数分别为58及54个月,而对照组分别为48及42个月。Kaplan-Meier分析显示两组患者的累积疗效维持率差异具有统计学意义(χ2=3.481,P=0.032)。结论关节镜下复发性髌骨脱位三联修复术远期效果优于普通双束解剖重建内侧髌股韧带法。 -
关键词:
- 髌骨脱位 /
- 关节镜;Kaplan-Meier分析 /
- 疗效维持时间 /
Abstract:Objective To make the Kaplan - Meier analysis evaluation under arthroscopy recurrent patellar dislocation (PD) thejoint prosthesis of long-term outcome. Methods We selected 69 patients with PD PD patients were randomly divided into observation group (n=36) and control group (n=33), were given under the arthroscope sanlian repair and ordinary double beam anatomic reconstruction of the medial patellofemoral ligament in the treatment of PD. For patients with more than 5 years of long-term follow-up, compared before and after operation of the lateral patellofemoral Angle, Lysholm scale effect and maintain. Results The two groups before treatment of the lateral patellofemoral Angle and Lysholm scale are no difference between groups (P >0.05); At the time of the last follow-up, two groups of patients of the lateral patellofemoral Angle and Lysholm score were significantly greater than/higher than before the operation, observation group had a significantly greater than/the above both higher than that of control group (P<0.05). Two groups there were 3 and 4 cases with delete, delete loss rate was no statistical difference (P >0.05). Two groups of curative effect to maintain time longest respectively in 75 and 68 months; The curative effect of observation group of arithmetic mean and the median time of 58 and 54 months respectively, and the control group of 48 and 42 months respectively. Kaplan and Meier analysis showed that the cumulative effect of two groups of patients maintain rate differences statistically significant (χ2=3.481, P=3.481). Conclusion The joint prosthesis under arthroscopy recurrent patellar dislocation long-term effect is superior to the ordinary double beam anatomic reconstruction of the medial patellofemoral ligament method. -
表 1 两组患者的一般情况及疗效比较(n, x±s)
分组 n 性别 年龄(岁) 外侧髌股角(°) Lysholm评分 男 女 手术前 末次随访 手术前 末次随访 观察组 36 13 23 33.27±6.19 2.62±2.13 8.41±3.04* 62.98±7.72 94.19±5.03* 对照组 33 9 24 34.58±5.34 2.59±2.21 6.92±2.37* 63.46±8.05 89.25±3.37* 统计量 χ2=1.152 -1.027 0.986 2.283 -1.192 5.883 P 0.164 0.184 1.025 0.026 0.827 0.013 与术前比较, *P <0.05. 表 2 两组患者疗效维持时间的比较(x±s, 月)
分组 例数 最长维持期(月) 疗效维持时间的算术均数(月) 疗效维持时间的中位数(月) 均数 标准误 95%可信区间 均数 标准误 95%可信区间 下限 上限 下限 上限 观察组 36 75+ 58.181 4.732 60.906 79.457 54.000 5.273 54.926 75.023 对照组 33 68 48.560 9.380 53.016 64.104 42.000 3.322 42.489 65.511 -
[1] Suganuma J, Mochizuki R, Inoue Y, et al. Arthroscopic evaluation of patellofemoral congruence with rotation of the knee joint and electrical stimulation of the quadriceps[J]. Arthroscopy, 2014, 30 (2): 214-21. [2] 刘阳, 郑江, 张明宇, 等. 半腱肌肌腱移植双束解剖重建治疗复发性髌骨脱位[J]. 中华骨科杂志, 2012, 32(2): 111-5. [3] 仲鹤鹤, 刘毅, 吴术红, 等. 关节镜辅助下自体肌腱重建内侧髌股韧带治疗复发性髌骨脱位的疗效[J]. 重庆医科大学学报, 2015, 40(8): 1151-5. [4] 戴祝, 尤迪, 廖瑛, 等. 髌骨复发性脱位伴陈旧性骨软骨骨折的治疗 [J]. 中国修复重建外科杂志, 2016, 30(1): 10-4. [5] 沈鹏程, 何耀华, 徐能, 等. 关节镜下“三联术”治疗复发性髌骨脱位[J]. 生物骨科材料与临床研究, 2013, 10(6): 51-3. [6] 褚秀成, 燕树义, 王林亮, 等. 双束解剖重建内侧髌股韧带治疗髌骨脱位的疗效分析[J]. 中国矫形外科杂志, 2015, 23(22): 2057-62. [7] 王毅飞, 郭卫, 沈丹华, 等. 骶骨原发骨肉瘤的外科治疗效果评价[J]. 中国脊柱脊髓杂志, 2015, 25(8): 739-45. [8] 湛世本, 麦鸿飞. 微创关节镜下三联手术方案治疗复发性髌骨脱位的临床评价[J]. 中国医师进修杂志, 2016, 20(1): 70-2. [9] 李思鸿, 李晓声, 陈铁柱, 等. 关节镜下自体半腱肌腱重建内侧髌股韧带联合Fulkerson截骨治疗复发性髌骨脱位[J]. 中国内镜杂志, 2015, 21(7): 723-7. [10] 邹重文, 汪群力, 陈奇. 改良式三联手术治疗复发性髌骨脱位的疗效分析[J]. 中国矫形外科杂志, 2014, 22(19): 1805-8. [11] 陈刚, 叶永杰, 银毅, 等. 关节镜下髌骨支持带调整术治疗青少年复发性髌骨脱位的近期疗效[J]. 中国内镜杂志, 2014, 20(1): 38-42. [12] 成欣, 江起庭, 杨国涛. 改良髌三联术治疗复发性髌骨脱位疗效分析 [J]. 实用手外科杂志, 2015, 10(3): 274-5. [13] Cerciello S, Lustig S, Costanzo G, et al. Medial retinaculum reefing for the treatment for patellar instability[J]. Knee Surg Sports Traumatol Arthrosc, 2014, 22(10): 2505-12. -






 下载:
下载: