Mortality rate and risk factors for 59740 hospitalized patients with diabetes mellitus
-
摘要:
目的了解住院糖尿病患者的病死率,分析死亡相关因素。 方法回顾分析1998~2009年北京某医院内分泌科住院糖尿病患者的资料,并分析不同性别、住院次数、住院时间以及糖尿病类型的病死率。 结果59740例住院糖尿病患者中,死亡1283例,总体病死率为2.1%(男性2.2%,女性2.0%)。死亡组患者的人均住院次数和住院时间均大于存活组患者。不同类型的糖尿病患者的病死率也存在较明显差异。其中急性并发症糖尿病患者病死率2.8%,其次是2型糖尿病患者的病死率2.4%,病死率最低的是1型糖尿病患者(1.1%)。 结论住院次数、住院时间及糖尿病类型反映患者病情严重程度,是住院糖尿病患者病死相关因素。 Abstract:Objective To investigate the mortality rate of diabetic inpatients and the death-relating factors in a tertiary hospital. Methods Information of the hospitalized diabetic patients administered at the Department of Endocrinology between 1998and 2009 were retrospectively analyzed. Types of diabetes, hospital days and hospital visits were collected relating to patients’death status. Results Among the 59740 diabetic patients, 1283 died, with a mortality rate of 2.1% (2.2% in men and 2.0% inwomen). Average number of hospital visits and hospital days were significantly higher in death group than that in survivalgroup. Mortality rate was 2.8% for the patients with acute complication, 2.4% for the type 2 diabetic patients, and 1.1% forthose with type 1 diabetes. Conclusion Types of diabetes, hospital visits and hospital days are death-relating factors inhospitalized diabetic patients. -
Key words:
- diabetes mellitus /
- inpatient /
- mortality /
- risk factors
-
表 1 59740名糖尿病住院患者统计表
男性 女性 平均年龄(岁) 中位年龄(岁) 总数 例数 39965 19775 63.27 64.41 59740 存活组 39196 19261 62.98 64.04 58457 死亡组 879 404 73.75 75.7 1283 病死率 2.20% 2.00% - - 2.10% 表 2 59740名糖尿病住院患者分类表
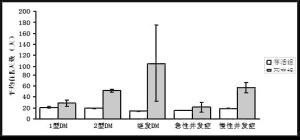
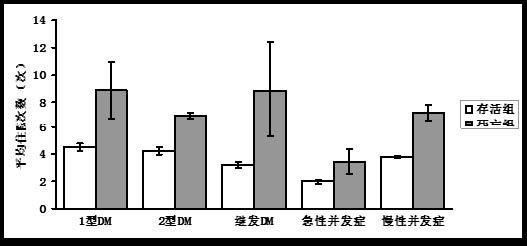
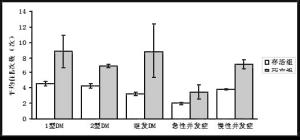
1 型糖尿病 2 型糖尿病 继发糖尿病 急性并发症 慢性并发症 总数 例数 830 44310 1217 956 12427 59740 存活组 821 43251 1200 929 12256 58457 死亡组 9 1059 17 27 171 1283 病死率 1.10% 2.40% 1.40% 2.80% 1.40% 2.10% 表 3 平均住院时间与住院次数(95% CI)
平均住院次数(次) 平均住院时间(d) 存活组 4.06(4.01~4.10) 18.5(18.29~18.71) 死亡组 7.01(6.60~7.41) 51.81(44.81~58.74) Z值 -20.816 -12.617 P值 0 0 -
[1] Whiting DR, Guariguata L, Weil C, et al. IDF diabetes Atlas: global estimates of the prevalence of diabetes for 2011 and 2030[J]. Diabetes Res Clin Pract, 2011, 94(3): 311-21. doi: 10.1016/j.diabres.2011.10.029 [2] Yang SH, Dou KF, Song WJ. Prevalence of diabetes among men and women in China[J]. N Engl J Med, 2010, 362(25): 2425-6. doi: 10.1056/NEJMc1004671 [3] Xu Y, Wang LM, He J, et al. Prevalence and control of diabetes in Chinese adults[J]. JAMA, 2013, 310(9): 948-58. doi: 10.1001/jama.2013.168118 [4] 范丽凤, 张小群, 朱筠茵. 糖尿病教育对接受胰岛素治疗患者的影响 [J]. 中华糖尿病杂志, 2000, 8(3): 148-51. http://www.cnki.com.cn/Article/CJFDTOTAL-ZGTL200003007.htm [5] 唐光敏, 余叶蓉, 王艳丽. 华西医院1996-2004年住院成人糖尿病患者病死率及死因分析[J]. 中国糖尿病杂志, 2008, 16(10): 598-600. [6] 徐静, 易兰兰, 徐琳, 等. 住院糖尿病患者死因分析[J]. 陕西医学杂志, 2005, 34(7): 807-9. http://www.cnki.com.cn/Article/CJFDTOTAL-SXYZ200507016.htm [7] Currie CJ, Poole CD, Evans M, et al. Mortality and other important Diabetes-Related outcomes with insulin vs other antihyperglycemic therapies in type 2 diabetes[J]. J of Clin Endocrin Metabolism, 2013, 98(2): 668-77. doi: 10.1210/jc.2012-3042 [8] 牟学晶, 任欣欣, 赵海潞. 胰岛素治疗的系统风险[J]. 临床合理用药杂志, 2014, 7(20): 12-4. http://www.cnki.com.cn/Article/CJFDTOTAL-PLHY201420011.htm [9] Mussig K, Staiger H, Kantartzis K, et al. Type 2 diabetes mellitus and risk of malignancy: is there a strategy to identify a subphenotype of patients with increased susceptibility to endogenous and exogenous hyperinsulinism[J]. Diabet Med, 2011, 28(3): 276-86. http://cn.bing.com/academic/profile?id=1979351664&encoded=0&v=paper_preview&mkt=zh-cn [10] Turchin A, Matheny ME, Shubina M, et al. Hypoglycemia and clinical outcomes in patients with diabetes hospitalized in the general ward[J]. Diabetes Care, 2009, 32(8): 1153-7. http://cn.bing.com/academic/profile?id=2121191655&encoded=0&v=paper_preview&mkt=zh-cn [11] Nice SS, Liu B. Hypoglycemia and risk of death in critically ill patients[J]. N Engl J Med, 2012, 367(12): 1108-18. doi: 10.1056/NEJMoa1204942 [12] [13] Pratipanawatr, T. Smoking and death in Thai diabetic patients:the Thailand Diabetic Registry cohort[J]. J Med Assoc Thai, 2013, 96 (3): 280-7. http://cn.bing.com/academic/profile?id=2221177556&encoded=0&v=paper_preview&mkt=zh-cn -






 下载:
下载: