Comparison of single and dual phase of enhanced CT diagnostic values in thyroid nodules
-
摘要:
目的 比较单、双期CT增强对甲状腺结节的诊断价值,探索最佳扫描方案。 方法 按纳入及排除标准,选取我院2020年1月~2022年6月因甲状腺结节行平扫及双期CT增强的153个病例,共171枚结节,单期CT增强组取延迟50 s的图像序列作诊断,双期CT增强组取延迟25 s和50 s两组图像序列作诊断。主要评价指标为甲状腺结节良恶性诊断的准确率、结节特征的显示率、阳性淋巴结的显示率及结节的强化特点。 结果 单、双期CT增强对甲状腺结节良恶性的诊断准确率差异无统计学意义(P=0.152),对甲状腺结节的边缘、形态、包膜、密度、钙化、淋巴结等特征的显示差异均无统计学意义(P>0.05)。不同密度的良恶性的甲状腺结节在两组间差异无统计学意义(P=0.418)。双期CT增强的强化方式在良恶性甲状腺结节之间差异无统计学意义(P=0.075)。 结论 单、双期CT增强对甲状腺结节的诊断价值无明显差异,单期CT增强辐射剂量低,适合临床推广和应用。 Abstract:Objective To compare the diagnostic value of single and dual phase of enhanced CT in thyroid nodules, and explore the best scanning scheme. Methods A total of 171 nodules in 153 patients were included from January 2020 to June 2022 according to inclusion and exclusion criteria. Image sequence with a delay of 50 seconds was taken for diagnosis in the group of single phase of enhanced CT, then image sequences with a delay of 25 and 50 seconds were taken for diagnosis in the group of dual phase of enhanced CT. Diagnostic accuracy of benign and malignant thyroid nodules, characteristics of thyroid nodules, positive lymph node and enhanced CT features of thyroid nodules in two scanning schemes were the main evaluation indicators. Results There was no statistical significance in diagnostic accuracy of benign and malignant thyroid nodules between single and dual phase of enhanced CT. There was no statistical significance in edge, morphology, capsule, density, calcification and lymph node of thyroid nodules between two scanning scheme. There was no statistical significance in different densities of benign and malignant thyroid nodules between two scanning scheme. There was no statistical significance in enhancement mode of benign and malignant thyroid nodules in dual phase of enhanced CT. Conclusion There is no significant difference in the diagnostic value of single and dual phase of enhanced CT in thyroid nodules, and single phase of enhanced CT would be more suitable for clinical promotion and application by its lower radiation dose. -
Key words:
- thyroid nodule /
- phase of CT enhancement /
- diagnostic value /
- computed tomography
-
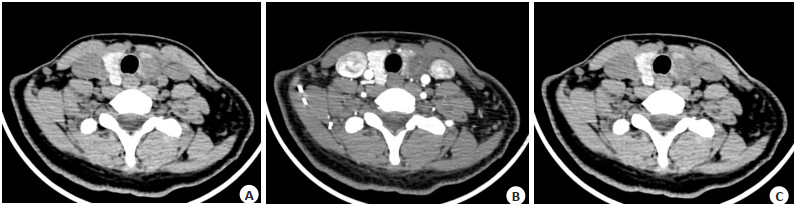
图 3 甲状腺左叶乳头状癌,边缘模糊的簇状钙化,转移性淋巴结囊变、钙化(箭头)
Figure 3. Clustered calcification with fuzzy edges and calcified metastatic lymph node with cystic degeneration (arrows) in Papillary thyroid carcinoma. A: Axial image of plain CT; B: Coronal image of Ⅰ phase enhanced CT; C: Coronal image of Ⅱ phase enhanced CT.
表 1 单、双期CT增强甲状腺结节良恶性诊断准确率比较
Table 1. Comparison of single and dual phase of enhanced CT's diagnostic accuracy in differentiate benign and malignant thyroid nodules (n)
Dual-phase CT enhancement Single-phase CT enhancement Total + - + 129 16 145 - 8 18 26 Total 137 34 171 +: Correct diagnosis; -: Incorrect diagnosis. 表 2 单、双期CT增强甲状腺结节特征的比较
Table 2. Comparison of thyroid nodules'features in single and dual phase of enhanced CT (n)
Dual-phase CT Single-phase CT enhancement P + - Edge 0.115 + 69 14 - 6 82 Morphology 0.481 + 65 11 - 7 88 Capsule 0.388 + 53 8 - 4 106 Density 0.077 + 101 12 - 4 54 Calcification 0.167 + 37 13 - 6 25 Lymph node 0.344 + 26 7 - 3 135 +: Positive signs; -: Negative signs. 表 3 单、双期CT增强中甲状腺不同密度的良恶性结节比较
Table 3. Comparison of thyroid nodules with different densities and properties in single and dual phase of enhanced CT (n)
Group High-density benign nodules Equal or low-density benign nodules High-density malignant nodules Equal or low-density malignant nodules Single-phase CT enhancement 16 61 5 89 Dual-phase CT enhancement 9 68 3 91 χ2 2.840 P 0.418 表 4 双期CT增强甲状腺良、恶性结节强化方式比较
Table 4. Comparison of benign and malignant thyroid nodules' enhancement mode in dual phase of enhanced CT (n)
Group Progressive enhancement Withdrawal enhancement Continuous enhancement Benign nodules 12 61 4 Malignant nodules 28 60 6 χ2 5.169 P 0.075 -
[1] Pool C, Walter V, Bann D, et al. Molecular characterization of tumors meeting diagnostic criteria for the non- invasive follicular thyroid neoplasm with papillary-like nuclear features (NIFTP)[J]. Virchows Arch, 2019, 474(3): 341-51. doi: 10.1007/s00428-018-02512-6 [2] Cameselle- Teijeiro JM, Eloy C, Sobrinho- Simões M. Pitfalls in challenging thyroid tumors: emphasis on differential diagnosis and ancillary biomarkers[J]. Endocr Pathol, 2020, 31(3): 197-217. doi: 10.1007/s12022-020-09638-x [3] Roh JL, Park JY, Park CI. Total thyroidectomy plus neck dissection in differentiated papillary thyroid carcinoma patients: pattern of nodal metastasis, morbidity, recurrence, and postoperative levels of serum parathyroid hormone[J]. Ann Surg, 2007, 245(4): 604-10. doi: 10.1097/01.sla.0000250451.59685.67 [4] Adam MA, Pura J, Goffredo P, et al. Presence and number of lymph node metastases are associated with compromised survival for patients younger than age 45 years with papillary thyroid cancer [J]. J Clin Oncol, 2015, 33(21): 2370-5. doi: 10.1200/JCO.2014.59.8391 [5] 韩志江, 谢乐斯, 魏培英, 等. CT对甲状腺乳头状癌被膜侵犯及颈部淋巴结转移的预测价值[J]. 中华放射学杂志, 2021, 55(7): 723-8. doi: 10.3760/cma.j.cn112149-20200527-00748 [6] Lee DH, Kim YK, Yu HW, et al. Computed tomography for detecting cervical lymph node metastasis in patients who have papillary thyroid microcarcinoma with tumor characteristics appropriate for active surveillance[J]. Thyroid, 2019, 29(11): 1653- 9. doi: 10.1089/thy.2019.0100 [7] 中华医学会放射学分会头颈学组. 甲状腺结节影像检查流程专家共识[J]. 中华放射学杂志, 2016, 50(12): 911-5. doi: 10.3760/cma.j.issn.1005-1201.2016.12.003 [8] Schork M, Williams G. Number of observations required for the comparison of two correlated proportions[J]. Commun Stat Simul Comput, 1980, 9(4): 349-57. doi: 10.1080/03610918008812161 [9] Machin D, Campbell M, Fayers P, et al. Sample Size Tables for Clinical Studies, 2nd Edition[M]. Malden: Blackwell Science, 1997. [10] 周健, 赖旭峰, 韩志江, 等. 多种CT征象对甲状腺良、恶性结节的预测价值[J]. 中华全科医师杂志, 2018, 17(1): 44-9. [11] 刘嘉, 夏旭良, 肖科, 等. 双期CT增强联合三维重建技术在甲状腺肿瘤定性诊断中的应用[J]. 分子影像学杂志, 2022, 45(1): 66-70. doi: 10.12122/j.issn.1674-4500.2022.01.13 [12] 韩志江, 包凌云, 陈文辉. 甲状腺及甲状旁腺病变影像比较诊断学[M]. 北京: 人民卫生出版社, 2016: 173-318. [13] 夏晓娜, 黄召弟, 任庆国, 等. CT双期增强扫描对182枚甲状腺良恶性结节的诊断价值[J]. 山东大学学报(医学版), 2021, 59(7): 57-62. [14] 卜锐, 杨娜, 夏春娟, 等. 甲状腺乳头状癌超声特征与颈部转移性淋巴结之间的关系[J]. 医学影像学杂志, 2020, 30(7): 1157-60. [15] 田兆荣, 孙杰, 杨建平, 等. 能谱CT虚拟平扫联合多模型迭代重建算法在甲状腺图像质量及辐射剂量中的应用[J]. 中国医学影像学杂志, 2022, 30(2): 129-33, 138. [16] 刘尼军, 周欣, 李江涛. 结节性甲状腺肿多层螺旋CT诊断及鉴别诊断[J]. 陕西医学杂志, 2018, 47(5): 627-9, 632. [17] 梁莅芒, 孙中婷. 甲状腺良恶性结节的CT表现分析[J]. 中国医师杂志, 2020, 22(11): 1730-3. [18] Makino T, Orita Y, Tachibana T, et al. Computed tomography findings for diagnosing follicular thyroid neoplasms[J]. Acta Med Okayama, 2018, 72(6): 577-81. [19] Han ZJ, Shu YY, Lai XF, et al. Value of computed tomography in determining the nature of papillary thyroid microcarcinomas: evaluation of the computed tomographic characteristics[J]. Clin Imaging, 2013, 37(4): 664-8. doi: 10.1016/j.clinimag.2012.12.005 [20] Lee KH, Kim DW, Baek JW, et al. Comparison of computed tomography features between follicular neoplasm and nodular hyperplasia[J]. Cancer Imaging, 2016, 16(1): 31. doi: 10.1186/s40644-016-0089-x [21] 黄玉娃, 朱新进, 靳仓正, 等. 钙化征在CT诊断甲状腺良、恶性结节中的价值[J]. 分子影像学杂志, 2018, 41(4): 448-51. doi: 10.12122/j.issn.1674-4500.2018.04.07 [22] 陈海桃, 郑穗生, 邹立巍, 等. CT对甲状腺良恶性钙化结节的鉴别诊断价值[J]. 中国现代医学杂志, 2019, 29(6): 61-4. [23] Feng JW, Yang XH, Wu BQ, et al. Predictive factors for central lymph node and lateral cervical lymph node metastases in papillary thyroid carcinoma[J]. Clin Transl Oncol, 2019, 21(11): 1482-91. [24] Haugen BR, Alexander EK, Bible KC, et al. 2015 American thyroid association management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: the American thyroid association guidelines task force on thyroid nodules and differentiated thyroid cancer[J]. Thyroid, 2016, 26(1): 1-133. [25] 赵佳正, 王海滨, 韩志江, 等. 甲状腺未分化癌临床和CT特征分析[J]. 中华内分泌外科杂志, 2020, 14(4): 305-9. [26] 莫威行, 周健, 韩志江, 等. 高强化对甲状腺CT双期增强扫描良恶性结节性质判断的价值[J]. 浙江中西医结合杂志, 2016, 26(8): 739-41, 684. -







 下载:
下载: