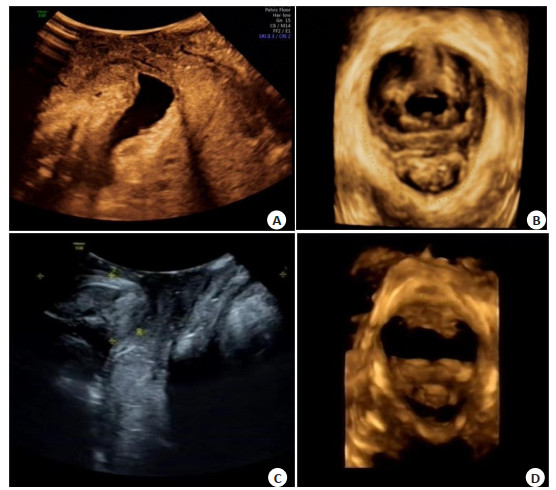
Four-dimensional pelvic floor ultrasound can evaluate the curative effect of electrical stimulation biofeedback in female patients with pelvic floor dysfunction
-
摘要:
目的 探讨基于盆底四维超声评估女性盆底肌功能障碍患者电刺激生物反馈治疗的疗效。 方法 选取2021年1月~2023年1月在我院收治的120例产后女性盆底肌功能障碍患者作为研究对象, 所有患者均予以电刺激生物反馈治疗4个疗程, 并在治疗前、治疗结束后行盆底四维超声检查。评估入组患者的临床疗效, 比较治疗前、治疗后盆底肌力分级、1 h尿垫试验、盆底肌收缩压、四维超声参数(静息时、Valsalva动作时)、膀胱颈移动度和尿道旋转角, 采用Pearson相关性分析治疗后膀胱颈移动度、尿道旋转角与盆底肌力分级、盆底肌收缩压的关系。 结果 120例患者经电刺激生物反馈治疗, 总有效率为84.17%。治疗后盆底肌力分级、盆底肌收缩压比治疗前明显升高, 1 h尿垫试验较之治疗前均明显下降, 差异均有统计学意义(P < 0.001)。治疗后肛提肌厚度(静息时、Valsalva动作时)较之治疗前均明显升高, 肛提肌裂孔左右径、肛提肌裂孔面积、膀胱后角、膀胱颈移动度、尿道旋转角较之治疗前均明显下降, 差异有统计学意义(P < 0.001)。治疗后膀胱颈移动度与盆底肌力分级、盆底肌收缩压呈负相关关系(r=-0.746、-0.781, P < 0.001);尿道旋转角与盆底肌力分级、盆底肌收缩压呈负相关关系(r=-0.779、-0.792, P < 0.001)。 结论 经盆底四维超声可以较好评估盆底肌功能障碍患者电刺激生物反馈治疗前后盆底肌功能, 值得临床推广。 Abstract:Objective To evaluate the curative effect of electrical stimulation biofeedback in female patients with pelvic floor dysfunction (PFD) based on four-dimensional pelvic floor ultrasound. Methods A total of 120 female patients with postpartum PFD who underwent electrical stimulation biofeedback for 4 courses in the hospital were enrolled as the research objects from January 2021 to January 2023.All underwent four-dimensional pelvic floor ultrasound examination before and after treatment.The clinical curative effect was evaluated.The grading of pelvic floor muscle strength, 1 h urine pad test, systolic blood pressure of pelvic floor muscle and four-dimensional ultrasound parameters (bladder neck movement and urethral rotation angle under rest and Valsalva maneuver state) were compared before and after treatment.The relationship between bladder neck movement, urethral rotation angle and grading of pelvic floor muscle strength, systolic blood pressure of pelvic floor muscle was analyzed by Pearson correlation analysis. Results In the 120 patients, total response rate of electrical stimulation biofeedback was 84.17%.After treatment, grading of pelvic floor muscle strength and systolic blood pressure of pelvic floor muscle were significantly increased, score of 1 h urine pad test was significantly decreased, the difference was statistically significant (P < 0.001).After treatment, levator ani thickness (under rest and Valsalva maneuver state) was significantly increased, left-right diameter and area of levator hiatus, posterior bladder angle, bladder neck movement and urethral rotation angle were significantly decreased, the difference was statistically significant (P < 0.001).After treatment, bladder neck movement was negatively correlated with grading of pelvic floor muscle strength and systolic blood pressure of pelvic floor muscle (r=-0.746, -0.781, P < 0.001), and urethral rotation angle was also negatively correlated with them (r=-0.779, -0.792, P < 0.001). Conclusion Four-dimensional pelvic floor ultrasound can better evaluate pelvic floor muscle function in PFD patients before and after electrical stimulation biofeedback. -
表 1 治疗前、治疗后盆底肌力分级、1 h尿垫试验和盆底肌收缩压比较
Table 1. Comparison of pelvic floor muscle strength grading, 1 h urine pad test and systolic blood pressure of pelvic floor muscle before and after treatment (n=120, Mean±SD)
Time Grading of pelvic floor muscle strength 1 h urine pad test (g) Systolic blood pressure of pelvic floor muscle (cmH2O) Before treatment 2.32±0.52 4.25±0.57 35.14±6.49 After treatment 3.14±0.68 1.36±0.31 41.88±5.72 t 10.493 48.791 8.534 P < 0.001 < 0.001 < 0.001 表 2 治疗前、治疗后静息时、Valsalva动作时四维超声参数比较
Table 2. Comparison of four-dimensional ultrasound parameters under rest and Valsalva maneuver state before and after treatment (n=120, Mean±SD)
Ultrasound parameters Before treatment After treatment t P Levator ani thickness Rest state 0.52±0.08 0.64±0.10 10.264 < 0.001 Valsalva maneuver state 0.50±0.06 0.59±0.08 9.859 < 0.001 left-right diameter of levator hiatus Rest state 3.75±0.65 3.24±0.78 5.502 < 0.001 Valsalva maneuver state 4.21±0.51 3.87±0.48 5.318 < 0.001 Area of levator hiatus (cm2) Rest state 23.14±3.52 19.35±3.69 8.141 < 0.001 Valsalva maneuver state 26.70±3.65 22.33±3.42 9.570 < 0.001 Posterior bladder angle (°) Rest state 112.37±20.46 80.34±16.58 13.323 < 0.001 Valsalva maneuver state 125.67±15.76 85.32±14.60 20.574 < 0.001 表 3 治疗前、治疗后膀胱颈移动度、尿道旋转角比较
Table 3. Comparison of bladder neck movement and urethral rotation angle before and after treatment (n=120, Mean±SD)
Time Bladder neck movement
(mm)Urethral rotation angle (°) Before treatment 21.66±5.64 38.10±6.25 After treatment 14.18±5.35 27.42±5.71 t 10.540 13.819 P < 0.001 < 0.001 表 4 治疗后膀胱颈移动度、尿道旋转角与盆底肌力分级、盆底肌收缩压的关系
Table 4. The relationship between bladder neck movement, urethral rotation angle and grading of pelvic floor muscle strength, systolic blood pressure of pelvic floor muscle after treatment
Detection parameters Grading of pelvic floor muscle strength Systolic blood pressure of pelvic floor muscle r P r P Bladder neck movement -0.746 < 0.001 -0.781 < 0.001 Urethral rotation angle -0.779 < 0.001 -0.792 < 0.001 -
[1] Aguilar-Zafra S, del Corral T, Vidal-Quevedo C, et al. Pelvic floor dysfunction negatively impacts general functional performance in patients with multiple sclerosis[J]. Neurourol Urodyn, 2020, 39(3): 978-86. doi: 10.1002/nau.24314 [2] 王慧兰, 朱倩, 王美燕, 等. 盆底肌肉锻炼联合电刺激生物反馈疗法治疗盆底功能障碍性疾病临床效果研究[J]. 中国实用妇科与产科杂志, 2023, 39(1): 115-8. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGSF202301024.htm [3] Zhong FL, Miao WB, Yu ZX, et al. Clinical effect of electrical stimulation biofeedback therapy combined with pelvic floor functional exercise on postpartum pelvic organ prolapse[J]. Am J Transl Res, 2021, 13(6): 6629-37. [4] 王莹, 鲁虹霞, 冯桂婷. 四维盆底超声在初产妇盆底功能障碍性疾病中的运用[J]. 重庆医学, 2020, 49(10): 1669-71, 1676. doi: 10.3969/j.issn.1671-8348.2020.10.028 [5] 顾小宁, 杨敏, 刘芳, 等. 经会阴盆底超声督导盆底肌肉训练在绝经后女性盆腔器官脱垂中的作用[J]. 中国超声医学杂志, 2018, 34(11): 1024-7. doi: 10.3969/j.issn.1002-0101.2018.11.022 [6] 阮飞娜, 杨俊娟, 郭华峰. 经会阴超声评价康复治疗对压力性尿失禁患者盆底功能和结构的影响[J]. 中国计划生育学杂志, 2018, 26(11): 1111-4. https://www.cnki.com.cn/Article/CJFDTOTAL-JHSY201811026.htm [7] 臧加英, 高波, 刘洋, 等. 盆底四维超声检测肛提肌裂孔前后径对压力性尿失禁女性患者盆底病变的评估价值[J]. 中国性科学, 2022, 31(4): 91-4. https://www.cnki.com.cn/Article/CJFDTOTAL-XKXZ202204023.htm [8] 朱兰, 郎景和. 女性盆底功能障碍性疾病[M]. 北京: 人民军医出版社, 2008: 43-4. [9] Alves FK, Riccetto C, Adami DB, et al. A pelvic floor muscle training program in postmenopausal women: a randomized controlled trial[J]. Maturitas, 2015, 81(2): 300-5. doi: 10.1016/j.maturitas.2015.03.006 [10] 闵洁, 彭国平. 经会阴三维盆底超声评估针灸对阴道分娩产妇压力性尿失禁康复治疗的应用价值[J]. 川北医学院学报, 2023, 38(2): 190-4. doi: 10.3969/j.issn.1005-3697.2023.02.011 [11] 张娜, 李红, 门月玲, 等. 1162例孕妇产后盆底功能障碍的发生率、影响因素及康复训练效果分析[J]. 中国妇幼保健, 2018, 33(7): 1469-72. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFYB201807009.htm [12] 徐捷, 李惠雯, 汪柏云, 等. 影响初产妇水中分娩产后近期盆底功能障碍的危险因素及对策[J]. 中国妇幼保健, 2022, 37(13): 2464-7. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFYB202213038.htm [13] 王娅菊, 付航, 杨汝丽, 等. 四维盆底超声在电刺激联合生物反馈结合盆底肌锻炼治疗压力性尿失禁疗效评估中的价值[J]. 中国中西医结合影像学杂志, 2021, 19(2): 158-60. https://www.cnki.com.cn/Article/CJFDTOTAL-JHYX202102016.htm [14] 邱少红, 潘碧琦, 郑秋萍, 等. 腹针联合电刺激生物反馈治疗产后女性性功能障碍的临床观察[J]. 中国性科学, 2019, 28(12): 103-5. https://www.cnki.com.cn/Article/CJFDTOTAL-XKXZ201912029.htm [15] 胡静, 袁钰宁, 程思. Kegel训练联合生物反馈电刺激治疗产后压力性尿失禁的疗效观察[J]. 徐州医科大学学报, 2021, 41(6): 103-5. https://www.cnki.com.cn/Article/CJFDTOTAL-XZYX202106015.htm [16] 甘会书, 王凤永, 温中琼, 等. 经会阴超声成像技术在女性盆底结构与功能评价中的应用价值[J]. 中国医疗设备, 2019, 34(4): 100-3. https://www.cnki.com.cn/Article/CJFDTOTAL-YLSX201904027.htm [17] 李宁, 阚艳敏, 王艺桦, 等. 多模态超声定量评估高龄产妇产后早期盆底结构和功能变化及诊断压力性尿失禁的价值研究[J]. 中国全科医学, 2022, 25(6): 706-13. https://www.cnki.com.cn/Article/CJFDTOTAL-QKYX202206011.htm [18] 成平, 王丹, 吴雅菲, 等. 膀胱颈位置和移动度诊断女性产后轻度压力性尿失禁的价值[J]. 广西医学, 2018, 40(21): 2552-4. https://www.cnki.com.cn/Article/CJFDTOTAL-GYYX201821012.htm [19] 苏明君, 黄海燕, 徐志清, 等. 低频电刺激联合盆底康复训练压力性尿失禁患者盆底肌力和排尿情况的影响[J]. 山西医药杂志, 2023, 52(2): 141-4. https://www.cnki.com.cn/Article/CJFDTOTAL-SXYY202302016.htm [20] 刘成成, 金永红, 左冬梅, 等. 三维盆底超声可动态观察初产妇早期盆底结构及功能的变化[J]. 分子影像学杂志, 2021, 44(5): 733-8. doi: 10.12122/j.issn.1674-4500.2021.05.01 [21] 李超, 李渊, 李芷茹, 等. 早期盆底肌肉训练及电刺激治疗对产后盆底康复影响的研究[J]. 中国康复, 2019, 34(1): 22-5. https://www.cnki.com.cn/Article/CJFDTOTAL-ZLKF201901007.htm -







 下载:
下载: