CT and MRI signs and diagnostic value of skull base bone invasion in nasopharyngeal carcinoma
-
摘要:
目的 探讨鼻咽癌颅底骨质侵犯的CT与MRI征象及其诊断价值。 方法 选取2018年4月~2022年7月我院收治的130例鼻咽癌患者作为研究对象。均采用CT及MRI进行检查。统计病理结果,以定性诊断为金标准,记录CT、MRI对颅底骨质侵犯的诊断结果,采用ROC曲线分析CT及MRI检查对鼻咽癌颅底骨质侵犯的诊断价值。 结果 130例患者经病理活检显示均为鳞状细胞癌,其中有88例分化性非角化型鳞癌,13例分化性角化型鳞癌,29例未分化性鳞癌。定性诊断共检出颅底骨质侵犯98例,检出率为75.38%,CT检查共检出颅底骨质侵犯80例,检出率为61.54%,MRI检查共检出颅底骨质侵犯97例,检出率为74.62%,MRI检查检出率高于CT检查(P < 0.05)。MRI检查对鼻咽癌颅底骨质侵犯的诊断敏感度、特异度、准确度分别为95.92%、90.62%、94.62%,均高于CT检查的76.53%、84.37%、78.46%(P < 0.05)。 结论 相比于CT检查,MRI检查对鼻咽癌颅底骨质侵犯的检出率更高,具有较高诊断价值。 Abstract:Objective To explore the CT and MRI signs and value of diagnostic in skull base bone invasion in nasopharyngeal carcinoma. Methods A total of 130 patients with nasopharyngeal carcinoma treated in our hospital from April 2018 to July 2022 were selected as the research subjects. All patients were performed with CT and MRI. The pathological results were counted, qualitative diagnosis was taken as the gold standard, the diagnostic results of CT and MRI for skull base bone invasion were recorded. ROC curve was used to analyze the diagnostic value of CT and MRI for skull base bone invasion of nasopharyngeal carcinoma. Results All 130 patients had squamous cell carcinoma by biopsy, including 88 cases of differentiated non keratinized squamous cell carcinoma, 13 cases of differentiated keratinized squamous cell carcinoma, and 29 cases of undifferentiated squamous cell carcinoma. A total of 98 cases of skull base bone invasion were detected by qualitative diagnosis, with a detection rate of 75.38%. 80 cases of skull base bone invasion were detected by CT, with a detection rate of 61.54%. 97 cases of skull base bone invasion were detected by MRI, with a detection rate of 74.62%. The detection rate of MRI examination was higher than that of CT examination (P < 0.05). The diagnostic sensitivity, specificity and accuracy of MRI examination for skull base bone invasion of nasopharyngeal carcinoma were 95.92%, 90.62%, 94.62%, respectively, which were higher than 76.53%, 84.37%, 78.46% of CT examination (P < 0.05). Conclusion Compared with the CT examination, MRI examination has a higher detection rate of skull base bone invasion in nasopharyngeal carcinoma, which has higher diagnostic value. -
图 2 患者1影像学表现
Figure 2. Image findings of patient 1. A: On T1WI, irregular mixed slightly long T1 slightly signal and unclear boundary could be seen in the posterior wall of nasopharynx, bilateral nasal cavity, right maxillary sinus, bilateral ethmoid sinus and sphenoid sinus; B: T1 enhanced showed uneven enhancement of the lesion; C-D: CT examination found that the right maxillary sinus peripheral wall, sphenoid sinus, ethmoid sinus and medial orbital wall were damaged and invaded.
图 3 患者2影像学表现
Figure 3. Image findings of patient 2. A-B: On CT, soft tissue density shadow could be seen in the left nasopharyngeal cavity, left maxillary sinus and sphenoid sinus, the boundary between the lesion and adjacent bone was unclear, and adjacent bone continuity was interrupted; C-D: On T2WI, irregular mixed slightly long T2 signals could be seen in the left nasopharynx cavity, left maxillary sinus and sphenoid sinus, the boundary was unclear, and the enhancement scan showed obvious uneven enhancement.
表 1 CT对颅底骨质侵犯的诊断结果
Table 1. Diagnostic results of CT for skull base bone invasion (n)
CT examination Qualitative diagnosis Total Positive Negative Positive 75 5 80 Negative 23 27 50 Total 98 32 130 表 2 MRI对颅底骨质侵犯的诊断结果
Table 2. Diagnostic results of MRI for skull base bone invasion (n)
MRI examination Qualitative diagnosis Total Positive Negative Positive 94 3 97 Negative 4 29 33 Total 98 32 130 表 3 CT、MRI检查对鼻咽癌颅底骨质侵犯的诊断价值分析
Table 3. Analysis of diagnostic value of CT and MRI examination for skull base bone invasion in nasopharyngeal carcinoma
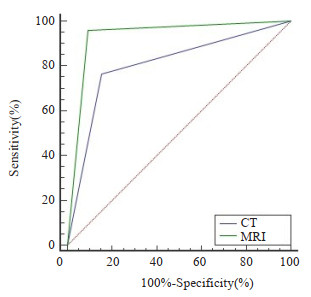
Examination AUC 95% CI Sensitivity(%) Specificity(%) Accuracy(%) CT 0.805 0.726-0.869 76.53 84.37 78.46 MRI 0.933* 0.875-0.969 95.92* 90.62* 94.62* *P < 0.05 vs CT examination. -
[1] Chu SA, Chen TB, Chen HJ, et al. Gamma knife radiosurgery as a salvage treatment for nasopharyngeal carcinoma with skull base and intracranial invasion (T4b)[J]. Life (Basel), 2022, 12(11): 1880. [2] 李少朋, 程传东, 邓克学. MRI与CT诊断鼻咽癌颅底骨质侵犯的临床价值比较[J]. 磁共振成像, 2020, 11(12): 1167-9, 1185. doi: 10.12015/issn.1674-8034.2020.12.019 [3] 占杨, 王鹏, 唐作华, 等. 双能量CT在评估鼻咽癌颅底骨侵犯中的价值研究[J]. 中国医学计算机成像杂志, 2022, 28(1): 32-7. https://www.cnki.com.cn/Article/CJFDTOTAL-YJTY202201006.htm [4] 贾春雷, 乔俏, 韩凝, 等. 诊断级CT系统对鼻咽癌患者调强放射治疗中摆位误差的评估[J]. 中国医科大学学报, 2020, 49(1): 87-90. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGYK202001020.htm [5] 冯妹妹, 饶艳莺, 林家豪, 等. 磁共振零回波时间序列评估鼻咽癌颅底骨质侵犯的诊断价值[J]. 肿瘤学杂志, 2021, 27(11): 915-21. doi: 10.11735/j.issn.1671-170X.2021.11.B004 [6] 徐海欢, 黄伟彪, 陈科权, 等. 磁共振成像/CT图像融合与CT图像勾画鼻咽癌患者调强适形放疗靶区准确性比较[J]. 临床军医杂志, 2022, 50(12): 1282-4. https://www.cnki.com.cn/Article/CJFDTOTAL-JYGZ202212021.htm [7] 钱秋平. CT与MRI诊断鼻咽癌局部侵犯的价值探讨[J]. 癌症进展, 2018, 16(6): 773-5. https://www.cnki.com.cn/Article/CJFDTOTAL-AZJZ201806031.htm [8] 中国医师协会放射肿瘤治疗医师分会, 中华医学会放射肿瘤治疗学分会. 中国鼻咽癌放射治疗指南(2020版)[J]. 中华肿瘤防治杂志, 2021, 28(3): 167-77. doi: 10.16073/j.cnki.cjcpt.2021.03.01 [9] 李猛, 牟兴宇, 卢彦祺, 等. 99Tcm-MDP骨显像SUV值在鼻咽癌颅底侵犯诊断价值初步研究[J]. 标记免疫分析与临床, 2019, 26(5): 781-5, 829. https://www.cnki.com.cn/Article/CJFDTOTAL-BJMY201905015.htm [10] 彭德新, 周锋江, 陈志萍, 等. 1.5T与3.0T MRI在初诊鼻咽癌放疗前应用的初步对比分析[J]. 实用癌症杂志, 2020, 35(8): 1288-90, 1293. doi: 10.3969/j.issn.1001-5930.2020.08.018 [11] 敬云华, 吕俭霞, 程平, 等. 社会支持在鼻咽癌患者自我感受负担和心理痛苦间的调节作用[J]. 成都医学院学报, 2022, 17(5): 639-44. https://www.cnki.com.cn/Article/CJFDTOTAL-CDYU202205021.htm [12] Bossi P, Chan AT, Licitra L, et al. Nasopharyngeal carcinoma: ESMO-EURACAN Clinical Practice Guidelines for diagnosis, treatment and follow-up[J]. Ann Oncol, 2021, 32(4): 452-65. [13] 顾大勇, 黄生富, 宗丹, 等. 磁共振弥散加权成像对鼻咽癌放疗后颈部淋巴结复发早期诊疗的临床价值[J]. 中华放射肿瘤学杂志, 2019, 28(8): 571-4. [14] 章钰梅, 巩贯忠, 曹秀娟, 等. 基于CT/MRI/PET-CT进行鼻咽癌大体肿瘤区及淋巴结勾画的对照研究[J]. 中华放射医学与防护杂志, 2021, 41(9): 653-8. [15] 龚修云, 金风, 甘家应, 等. MRI/CT融合图像勾画局部晚期鼻咽癌诱导化疗后靶区对放疗计划的影响[J]. 贵州医科大学学报, 2018, 43(3): 314-9. https://www.cnki.com.cn/Article/CJFDTOTAL-GYYB201803014.htm [16] 朱书田, 徐慧琴, 陈灯运, 等. 18F-FDG和18F-FMISO PET/CT显像评价甘氨双唑钠对鼻咽癌的放射增敏作用的研究[J]. 安徽医科大学学报, 2019, 54(3): 474-8. https://www.cnki.com.cn/Article/CJFDTOTAL-YIKE201903028.htm [17] 谢辉, 胡海芹, 张见芳, 等. 应用锥形束CT研究鼻咽癌调强放射治疗计划靶区的增长[J]. 中国医学装备, 2021, 18(3): 29-32. https://www.cnki.com.cn/Article/CJFDTOTAL-YXZB202103007.htm [18] 高路, 刘青峰, 谢克北, 等. CBCT与CTVision图像引导放射治疗技术在鼻咽癌放射治疗摆位误差校正中的应用差异[J]. 中国医学装备, 2019, 16(12): 69-72. https://www.cnki.com.cn/Article/CJFDTOTAL-YXZB201912020.htm [19] 高欣, 周丽娟, 徐孝秋, 等. 动态对比增强磁共振成像定量参数直方图分析与鼻咽癌临床分期的相关性初步研究[J]. 实用放射学杂志, 2019, 35(10): 1590-4. [20] 孙家元, 高文霞, 倪建, 等. 动态对比增强磁共振成像对鼻咽癌临床分期的诊断价值评价[J]. 现代肿瘤医学, 2020, 28(24): 4339-42. https://www.cnki.com.cn/Article/CJFDTOTAL-SXZL202024028.htm [21] 唐爽, 林灿洁, 潘志格, 等. MRI表观扩散系数在诊断鼻咽癌颈部小淋巴结转移瘤及勾画放疗靶区中的应用效果[J]. 广西医学, 2018, 40(17): 1949-51, 1954. https://www.cnki.com.cn/Article/CJFDTOTAL-GYYX201817009.htm [22] 孙增勇, 苏娜, 王冰, 等. MRI对鼻咽癌调强放疗患者腮腺脂质含量时间演变的初步研究[J]. 医学影像学杂志, 2021, 31(12): 2014-7. https://www.cnki.com.cn/Article/CJFDTOTAL-XYXZ202112008.htm [23] 王晓莉, 丁婷, 余婷. 以放射敏感性为基础的T3、T4期鼻咽癌个体化颅底同期加量放射的治疗[J]. 昆明医科大学学报, 2020, 41(10): 91-5. https://www.cnki.com.cn/Article/CJFDTOTAL-KMYX202010017.htm [24] Zhang YM, Chen MN, Gao JM, et al. A predictive scoring model for short-term local recurrent nasopharyngeal carcinoma based on magnetic resonance imaging[J]. Cancer Biother Radiopharm, 2019, 34(2): 76-84. [25] 凌鑫, 张培栋, 汪娟. MRI联合CT诊断鼻咽癌患者早期颅底骨侵犯的价值及其对临床决策的影响[J]. 中国耳鼻咽喉头颈外科, 2019, 26(4): 187-90. https://www.cnki.com.cn/Article/CJFDTOTAL-EBYT201904005.htm [26] 玉贵永, 邹良群, 阮国柱. 锥形束CT在鼻咽癌调强放射治疗中摆位误差对危及器官及靶区剂量分布的影响研究[J]. 中国医学装备, 2018, 15(10): 36-9. https://www.cnki.com.cn/Article/CJFDTOTAL-YXZB201810011.htm -







 下载:
下载: