Contrast-enhanced ultrasound is more accurate in diagnosing breast BI-RADS 4a nodules than elastography
-
摘要:
目的 分析超声造影和弹性成像在乳腺BI-RADS 4a类结节中的诊断价值。 方法 纳入我院2019年1月~2023年2月经常规超声检测诊断为BI-RADS 4a类的患者115例,对每个病灶进行分析,以病理结果为金标准,构建超声造影评分和弹性成像两种诊断方法的ROC曲线,比较两种方法对乳腺BI-RADS 4a类结节良恶性诊断的价值。 结果 115例患者中,良性病灶87例,恶性病灶28例。超声造影评分和弹性成像两种诊断方法Kappa值小,一致性较差(P=0.258)。以病理结果作为金标准,造影评分的诊断价值更高(敏感度、特异性及准确度分别为0.812、0.976、0.956),与金标准之间的一致性较弹性成像更高。超声造影评分的诊断曲线下面积为0.976,高于弹性成像数值(0.784)。两种不同诊断方法显示恶性结节患者的年龄较良性患者偏高,结节最大直径偏大。 结论 超声造影方法较弹性成像能明显提高乳腺BI-RADS 4a类结节良恶性诊断的准确率,降低术前活检的风险,值得临床推广。 -
关键词:
- 超声造影 /
- 弹性成像 /
- 乳腺BI-RADS 4a类结节
Abstract:Objective To compare the diagnostic value of ultrasonic elastography and contrast-enhanced ultrasound in the diagnosis of breast BI-RADS 4a nodules. Method A total of 115 patients diagnosed as BI-RADS category 4a by routine ultrasonic detection in our hospital from January 2019 to February 2023 were included. Each lesion was analyzed, and pathological diagnosis were taken as the gold standard to construct diagnostic ROC curves of the two detection methods. The value of the two methods in the diagnosis of benign and malignant breast BI-RADS 4a nodules of BI-RADS was compared. Results Among 115 patients, there were 87 benign lesions and 28 malignant lesions. The Kappa values of ultrasonic elastography and contrast-enhanced ultrasound scores were small and inconsistent (P=0.258). Using pathological results as the gold standard, contrast score had higher diagnostic value (sensitivity, specificity and accuracy were 0.812, 0.976 and 0.956, respectively), and was more consistent with the gold standard than elastic imaging. The area under the diagnostic curve of contrast-enhanced ultrasound score was 0.976, higher than the value of elastic imaging (0.784). Three different diagnostic methods showed that the age of patients with malignant nodules was higher than that of patients with benign nodules, and the maximum diameter of nodules was larger. Conclusion Compared with ultrasonic elastography, contrast-enhanced ultrasound can significantly improve the accuracy of benign and malignant diagnosis of breast BI-RADS 4a nodules of BI-RADS, reduce the risk of preoperative biopsy, and is worthy of clinical promotion. -
图 1 乳腺BI-RADS 4a类结节常规超声、弹性成像及超声造影声像图
Figure 1. Ultrasonography, elastography and contrast-enhanced ultrasound of BI-RADS 4a. A: Two-dimensional ultrasound showed irregular hypoechoic nodules in the lower quadrant of the left breast; B: Elastic imaging shell 2.0, elastic value: 135 kPa; C: Contrast-enhanced ultrasound showed homogeneous high-enhancement, and the range of enhancement was not increased. The score of contrast-enhanced ultrasound was 1. Postoperative pathology: fibroadenoma with adenosis.
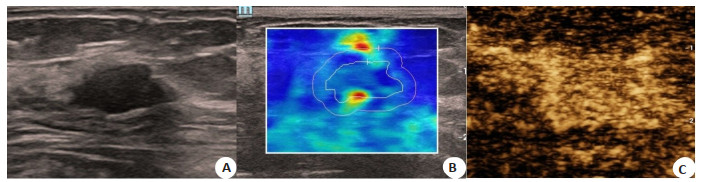
图 2 乳腺BI-RADS 4a类结节常规超声、弹性成像及超声造影声像图
Figure 2. Ultrasonography, elastography and contrast-enhanced ultrasound of BI-RADS 4a. A: Two-dimensional ultrasound showed irregular hypoechoic nodule in upper quadrant of right breast; B: Elastic imaging shell 2.0, elastic value: 86 kPa; C: Contrast-enhanced ultrasound showed early enhancement, high enhancement, enlarged range, spiculation sign around, and other large radial vessels in and around, and the contrast score was 5. Postoperative pathology: invasive carcinoma.
表 1 弹性值、造影评分结果比较
Table 1. Comparison of SWE and CEUS score (n)
CEUS score SWE Total Paired χ2 test Consistency check Malignant Benign P Kappa P Malignant 16 16 32 0.361 0.123 0.258 Benign 20 63 83 Total 36 79 115 SWE: Shear wave elastography 表 2 弹性值、造影评分两种诊断方法与病理诊断乳腺良恶性结节结果比较
Table 2. Comparison of SWE and CEUS score with pathological diagnosis of benign and malignant breast lesions (n)
Methods Diagnostic results Pathological results Total Malignant(n=28) Benign(n=87) SWE Malignant 17 19 36 Benign 11 68 79 CEUS score Malignant 26 6 32 Benign 2 81 83 CEUS: Contrast-enhanced ultrasound. 表 3 弹性值与造影评分对乳腺结节的诊断价值
Table 3. The diagnostic value of SWE and CEUS score for breast lesions
Diagnostic value SWE CEUS score Prevalence 0.313 0.278 Actual prevalence 0.243 0.243 Sensitivity 0.607(0.407, 0.779) 0.812(0.63, 0.921) Specificity 0.782(0.678, 0.860) 0.976(0.908, 0.996) Positive predictive value 0.47(0.308, 0.643) 0.929(0.75, 0.99) Negative predictive value 0.861(0.760, 0.925) 0.931(0.85, 0.972) Accuracy 0.686 0.956 Positive likelihood ratio 2.78(1.692, 4.569) 33.72(8.49, 133.92) Negative likelihood ratio 0.503(0.315, 0.802) 0.192(0.09, 0.395) Diagnostic odds ratio 0.67 1.212 Youden index 0.314 0.875 -
[1] Bae S, Jung S, Jung E, et al. Clinical characteristics and prognosis of pregnancy-associated breast cancer: poor survival of luminal B subtype[J]. Oncology, 2018, 95(3): 163-9. doi: 10.1159/000488944 [2] Ding YN, Chen XG, Zhang QJ, et al. Historical trends in breast Cancer among women in China from age-period-cohort modeling of the 1990-2015 breast Cancer mortality data[J]. BMC Public Health, 2020, 20(1): 1280. doi: 10.1186/s12889-020-09375-0 [3] Tang L, Wang YQ, Chen PP, et al. Clinical use and adjustment of ultrasound elastography for breast lesions followed WFUMB guidelines and recommendations in the real world[J]. Front Oncol, 2022, 12: 1022917. doi: 10.3389/fonc.2022.1022917 [4] Liu WY, Zhu YK, Ye L, et al. Establishment of an orthotopic prostate cancer xenograft mouse model using microscope-guided orthotopic injection of LNCaP cells into the dorsal lobe of the mouse prostate[J]. BMC Cancer, 2022, 22(1): 1-12. doi: 10.1186/s12885-021-09033-7 [5] Park AY, Kwon M, Woo OH, et al. A prospective study on the value of ultrasound microflow assessment to distinguish malignant from benign solid breast masses: association between ultrasound parameters and histologic microvessel densities[J]. Korean J Radiol, 2019, 20(5): 759. doi: 10.3348/kjr.2018.0515 [6] Huang SJ, Ye XQ, Yang KE, et al. The significance of dual-mode elastography in the diagnosis of breast lesions by physicians with different levels of experience[J]. Quant Imaging Med Surg, 2022, 12(2): 1438-49. doi: 10.21037/qims-21-636 [7] Cui YY, He NA, Ye XJ, et al. Evaluation of tissue stiffness around lesions by sound touch shear wave elastography in breast malignancy diagnosis[J]. Ultrasound Med Biol, 2022, 48(8): 1672-80. doi: 10.1016/j.ultrasmedbio.2022.04.219 [8] Cheng M, Tong W, Luo J, et al. Value of contrast-enhanced ultrasound in the diagnosis of breast US-BI-RADS 3 and 4 lesions with calcifications[J]. Clin Radiol, 2020, 75(12): 934-41. doi: 10.1016/j.crad.2020.07.017 [9] 米拉·也尔兰, 张海见, 胡峙珩, 等. 超声影像组学对BI-RADS 4a类不规则乳腺结节良恶性的鉴别价值[J]. 分子影像学杂志, 2023, 46(1): 12-20. doi: 10.12122/j.issn.1674-4500.2023.01.03 [10] Liu Q, Tang L, Chen M. Ultrasound strain elastography and contrast-enhanced ultrasound in predicting the efficacy of neoadjuvant chemotherapy for breast cancer: a nomogram integrating ki‐67 and ultrasound features[J]. J Ultrasound Med, 2022, 41(9): 2191-201. doi: 10.1002/jum.15900 [11] Golatta M, Pfob A, Büsch C, et al. The potential of combined shear wave and strain elastography to reduce unnecessary biopsies in breast cancer diagnostics-An international, multicentre trial[J]. Eur J Cancer, 2022, 161: 1-9. doi: 10.1016/j.ejca.2021.11.005 [12] 张意珍, 黄品同, 洪玉蓉, 等. 超声造影与弹性成像联合评分对乳腺BI-RADS 4类病灶的应用价值[J]. 中华医学超声杂志: 电子版, 2019, 16(2): 120-5. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHCD201902009.htm [13] 邢博缘, 刘小慧, 赵云, 等. 超声弹性成像联合乳腺影像报告和数据系统(BI-RADS)分类诊断非肿块型乳腺癌[J]. 中国医学影像技术, 2021, 37(8): 1154-7. doi: 10.13929/j.issn.1003-3289.2021.08.009 [14] Li HE, Cheng CJ, Wang Y, et al. Combined diagnosis of ultrasonic elastography and BI-RADS classification increases diagnostic value in female patients with breast neoplasms[J]. Am J Transl Res, 2021, 13(10): 11758-63. [15] Watanabe T, Yamaguchi T, Okuno T, et al. Utility of B-mode, color Doppler and elastography in the diagnosis of breast cancer: results of the CD-CONFIRM multicenter study of 1351 breast solid masses[J]. Ultrasound Med Biol, 2021, 47(11): 3111-21. doi: 10.1016/j.ultrasmedbio.2021.07.009 [16] Sezgin G, Coskun M, Apaydin M, et al. The role of rare breast cancers in the false negative strain elastography results[J]. La Radiol Med, 2021, 126(3): 349-55. doi: 10.1007/s11547-020-01270-3 [17] 邹芳, 王爽. 乳腺癌超声造影联合BI-RADS分级与病理检查结果对比分析[J]. 影像科学与光化学, 2021, 39(4): 620-3. https://www.cnki.com.cn/Article/CJFDTOTAL-GKGH202104026.htm [18] 李丽环, 王帆. 超声造影及动态增强磁共振成像诊断乳腺非肿块样强化病变的价值[J]. 影像科学与光化学, 2021, 39(3): 381-5. https://www.cnki.com.cn/Article/CJFDTOTAL-GKGH202103008.htm [19] Depretto C, Borelli A, Liguori A, et al. Contrast-enhanced mammography in the evaluation of breast calcifications: preliminary experience[J]. Tumori, 2020, 106(6): 491-6. doi: 10.1177/0300891620919170 [20] Li J, Yuan MX, Yang L, et al. Correlation of contrast-enhanced ultrasound features with prognostic factors in invasive ductal carcinomas of the breast[J]. Jpn J Radiol, 2020, 38(10): 960-7. doi: 10.1007/s11604-020-00994-6 [21] Xu P, Yang M, Liu Y, et al. Breast non-mass-like lesions on contrast-enhanced ultrasonography: feature analysis, breast image reporting and data system classification assessment[J]. World J Clin Cases, 2020, 8(4): 700-12. doi: 10.12998/wjcc.v8.i4.700 [22] Lee NR, Oh HK, Jeong YJ. Clinical significance of ultrasound elastography and fibrotic focus and their association in breast cancer[J]. J Clin Med, 2022, 11(24): 7435. doi: 10.3390/jcm11247435 [23] Tao ZM, Qi HM, Ma YF. Diagnostic efficacy of ultrasound elastography and dynamic contrast-enhanced MR in benign and malignant breast masses[J]. Am J Transl Res, 2023, 15(4): 2870-7. [24] Kapetas P, Clauser P, Woitek R, et al. Quantitative multiparametric breast ultrasound[J]. Investig Radiol, 2019, 54(5): 257-64. doi: 10.1097/RLI.0000000000000543 -







 下载:
下载: