Evaluation value of neoadjuvant chemotherapy in patients with non-small cell lung cancer based on tumor volume measured by CT
-
摘要:
目的 分析基于CT测量的肿瘤体积对非小细胞肺癌患者新辅助化疗疗效的评估价值。 方法 选取2019年5月~2020年5月在我院接受新辅助化疗的74例非小细胞肺癌患者,化疗后以病理结果为标准其分为有效组(n=51)和无效组(n=23),通过CT测量所有患者的肿瘤体积,并采用单因素和Logistic多因素回归分析其影响因素。 结果 化疗后,两组患者肿瘤体积小于化疗前(P < 0.05),有效组患者肿瘤体积小于无效前(P < 0.05)。两组患者化疗后6月生存率的差异无统计学意义(P > 0.05);化疗后1年,有效组患者生存率高于无效组(P < 0.05)。单因素分析结果显示:临床分期、分化程度以及化疗周期可能是肿瘤体积的影响因素(P < 0.05)。Logistic回归分析结果显示:临床分期、分化程度及化疗周期是非小细胞肺癌患者肿瘤体积的影响因素(P < 0.05)。ROC曲线分析结果表明肿瘤体积对非小细胞肺癌患者新辅助化疗疗效的预测价值,敏感度为0.732,特异性为0.800。 结论 基于CT测量的肿瘤体积对非小细胞肺癌患者新辅助化疗的疗效有一定的评估价值。 Abstract:Objective To analyze the evaluation value of neoadjuvant chemotherapy in patients with non-small cell lung cancer (NSCLC) based on tumor volume measured by CT. Methods Seventy- four patients with NSCLC who received neoadjuvant chemotherapy in our hospital from May 2019 to May 2020 were selected. After chemotherapy, they were divided into effective group (n=51) and ineffective group (n=23) based on pathological results. Tumor volume of all patients was measured by CT. Its influencing factors were analyzed by univariate and Logistic multivariate regression analysis. Results After chemotherapy, the tumor volume of 2 groups was significantly smaller than before chemotherapy (P < 0.05). The tumor volume of effective group was significantly smaller than before ineffective (P < 0.05). There was no significant difference in 6-month survival rate between 2 groups after chemotherapy (P > 0.05). One year after chemotherapy, the survival rate of effective group was significantly higher than that of ineffective group (P < 0.05). Univariate analysis showed that clinical stage, degree of differentiation and chemotherapy cycle were influencing factors of tumor volume (P < 0.05). Logistic regression analysis showed that clinical stage, differentiation degree and chemotherapy cycle were the influencing factors of tumor volume in patients with NSCLC (P < 0.05). ROC curve analysis showed that the sensitivity and specificity of tumor volume in predicting the efficacy of neoadjuvant chemotherapy in NSCLC patients were 0.732 and 0.800. Conclusion Tumor volume measured by CT has certain value in evaluating the efficacy of neoadjuvant chemotherapy in patients with NSCLC. -
Key words:
- CT /
- tumor volume /
- non-small cell lung cancer /
- neoadjuvant chemotherapy /
- assessment
-
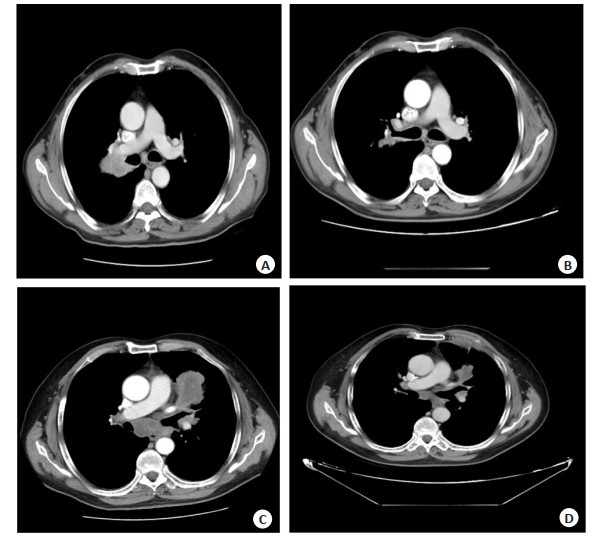
图 1 化疗前后非小细胞肺癌患者肺部CT图像
Figure 1. Lung CT images of NSCLC patients before and after chemotherapy. A: Right upper lung non-small cell lung cancer before chemotherapy; B: Right upper lung non-small cell lung cancer after chemotherapy; C: Before chemotherapy for non-small cell lung cancer of left upper lung; D: Left upper lung non-small cell lung cancer after chemotherapy.
表 1 化疗前后两组患者肿瘤体积大小及不同时期生存率比较
Table 1. Comparison of tumor size before and after chemotherapy and survival at different periods in the two groups
Index Time Effective group(n=51) Invalid group(n=23) t/χ2 P Gross tumor volume(cm3, Mean±SD) Before chemotherapy 83.21±5.29 82.25±5.43 0.717 0.476 After chemotherapy 55.25±4.14 80.86±5.02 23.030 < 0.001 Survival rate [n(%)] 6 months after chemotherapy 48(94.12) 20(86.96) 1.091 0.296 1 year after chemotherapy 37(60.78) 11(47.83) 4.252 0.039 表 2 影响肿瘤体积的单因素分析
Table 2. Univariate analysis affecting tumor volume [n(%)]
Index Withdrawal rate≥30%(n=53) Withdrawal rate < 30%(n=21) χ2 P Gender 0.182 0.669 Male 38(71.70) 14(66.67) Female 15(28.30) 7(33.33) Age (years) 0.113 0.737 ≥60 35(66.04) 13(61.90) < 60 18(33.96) 8(38.10) Clinical stages 10.441 0.001 Ⅰ designated time 23(43.40) 5(23.81) Ⅱ designated time 18(33.96) 3(14.29) Ⅲ designated time 12(55.64) 13(61.90) History of smoking 2.293 0.130 Have 25(47.17) 14(66.67) None 28(52.83) 7(33.33) Degree of differentiation 7.230 0.007 Low 18(33.96) 4(19.05) Middle 20(37.74) 4(19.05) High 15(28.30) 13(61.90) Chemotherapy cycle (years) 13.000 < 0.001 ≥1 43(81.13) 8(38.10) < 1 10(18.87) 13(61.90) Bronchial wall invasion 0.170 0.684 Have 20(37.74) 9(42.86) None 33(62.26) 12(57.14) 表 3 影响肿瘤体积的多因素Logistic回归分析
Table 3. Multivariate Logistic regression analysis affecting tumor volume
Index β SE Wald P OR 95% CI Clinical stages 0.53 0.21 8.460 0.012 1.699 1.126-2.564 Degree of differentiation 0.48 0.15 10.240 0.001 1.616 1.204-2.168 Chemotherapy cycle 0.51 0.18 8.028 0.005 1.170 1.655-2.370 -
[1] 张霞, 张毅, 欧阳伟炜, 等. 靶向治疗Ⅳ期非小细胞肺癌体积变化及放疗时机选择研究[J]. 中华放射肿瘤学杂志, 2020, 29(8): 633-8. [2] 高俊刚, 李阳, 叶佳俊, 等. 基于PET不同SUV阈值计算肺癌肿瘤代谢体积的方法比较[J]. 现代肿瘤医学, 2019, 27(21): 3887-90. https://www.cnki.com.cn/Article/CJFDTOTAL-SXZL201921036.htm [3] Miep A, der Drift V, MD, et al. Progress in standard of care therapy and modest survival benefits in the treatment of non-small cell lung cancer patients in the Netherlands in the last 20 years[J]. J Thorac Oncol, 2012, 7(2): 291-8. doi: 10.1097/JTO.0b013e31823a01fb [4] 解福友, 程刚, 刘斌. 增强CT联合肿瘤标志物对盐酸安罗替尼治疗非小细胞肺癌中的疗效评估分析[J]. 中国CT和MRI杂志, 2021, 19 (5): 26-9. https://www.cnki.com.cn/Article/CJFDTOTAL-CTMR202105009.htm [5] 祝令武. CT纹理分析对肺腺癌患者新辅助化疗预后的评估价值[J]. 河南医学研究, 2021, 30(31): 5901-4. https://www.cnki.com.cn/Article/CJFDTOTAL-HNYX202131048.htm [6] 李慧敏, 刘举珍. 18F-FDG PET/CT最大标准化摄取值及肿瘤标志物对可疑肺癌病灶病理类型的鉴别诊断价值[J]. 标记免疫分析与临床, 2019, 26(12): 1997-2002. https://www.cnki.com.cn/Article/CJFDTOTAL-BJMY201912005.htm [7] 李汝林, 张惠玲, 周德伟, 等. 术前多层螺旋CT增强扫描在老年非小细胞肺癌患者手术治疗中的应用价值[J]. 分子影像学杂志, 2021, 44(6): 945-9. doi: 10.12122/j.issn.1674-4500.2021.06.12 [8] 王海明, 李志彬, 齐学红, 等. CA125, CA153及CEA肿瘤标志物联合检测对非小细胞肺癌早期诊断的临床意义[J]. 影像研究与医学应用, 2018, 2(5): 103-4. https://www.cnki.com.cn/Article/CJFDTOTAL-YXYY201806057.htm [9] 雷新军, 涂建飞, 王慧梅, 等. 多模态CT检查联合肿瘤标志物评估塞来昔布联合调强放疗对晚期非小细胞肺癌的疗效[J]. 中国慢性病预防与控制, 2018, 26(12): 936-8. https://www.cnki.com.cn/Article/CJFDTOTAL-ZMXB201812016.htm [10] 刘超, 邓智勇. 非小细胞肺癌新辅助化疗疗效评价进展[J]. 分子影像学杂志, 2015, 38(3): 283-7. doi: 10.3969/j.issn.1674-4500.2015.03.37 [11] 王延虎, 汤晓斌, 耿长冉, 等. 非小细胞肺癌自适应放疗肿瘤和肺体积比值变化对肺受照剂量的影响[J]. 临床肺科杂志, 2018, 23(9): 1600-3. https://www.cnki.com.cn/Article/CJFDTOTAL-LCFK201809012.htm [12] 李晓雷, 徐俊, 胡欣, 等. 多中心多学科治疗模式下对局部晚期非小细胞肺癌患者的新辅助化疗疗效及预后影响的临床研究[J]. 东南大学学报: 医学版, 2018, 37(4): 667-72. https://www.cnki.com.cn/Article/CJFDTOTAL-NJTD201804024.htm [13] 刘炜, 李小毅, 薛华丹, 等. CT体积测量在进展期胃癌患者新辅助化疗疗效评价中的应用价值研究[J]. 癌症进展, 2010, 8(5): 420-4. https://www.cnki.com.cn/Article/CJFDTOTAL-AZJZ201005007.htm [14] 张春珍. 非小细胞肺癌新辅助化疗后肿瘤体积变化规律及其影响因素[J]. 现代肿瘤医学, 2016, 24(19): 3073-6. https://www.cnki.com.cn/Article/CJFDTOTAL-SXZL201619020.htm [15] 周悦乔, 林辉雄, 刘志强. 新辅助化疗对晚期非小细胞肺癌患者疗效及血清学指标影响的研究[J]. 癌症进展, 2018, 16(9): 1170-3. https://www.cnki.com.cn/Article/CJFDTOTAL-AZJZ201809028.htm [16] 邹灵俊, 陈洪波, 郭晓康, 等. 非小细胞肺癌新辅助化疗联合手术预后影响因素分析[J]. 中华肿瘤防治杂志, 2022, 29(3): 179-85. https://www.cnki.com.cn/Article/CJFDTOTAL-QLZL202203004.htm [17] 侯露, 蔡其君, 王璐, 等. 正电子发射断层显像技术在药物开发0期临床研究中的应用[J]. 今日药学, 2020, 30(2): 99-105. https://www.cnki.com.cn/Article/CJFDTOTAL-YAXU202002003.htm [18] 魏振强, 谢昊均, 苏晓东. 肿瘤体积对Ⅰ期非小细胞肺癌术后患者预后预测价值的研究[J]. 中国医药导报, 2018, 15(8): 104-7, 123. https://www.cnki.com.cn/Article/CJFDTOTAL-YYCY201808026.htm -







 下载:
下载: