Dynamic contrast-enhanced MRI and diffusion-weighted MRI can improve diagnostic efficacy of benign and malignant breast lesions
-
摘要:
目的 分析乳腺癌MRI动态增强(DCE)与扩散加权成像(DWI)的影像学特点及联合诊断的效能。 方法 回顾性收集2018年6月~2022年8月我院收治的230例乳腺癌患者作为恶性组,选取同期在我院接受检查和治疗的252例乳腺良性病变患者作为良性组,所有患者均经手术治疗或病理穿刺活检确诊。统计乳腺良恶性病变患者DCE-MRI、DWI的影像学特点,统计DCE-MRI、DWI单独及联合对乳腺良恶性病变患者诊断 结果 ,采用ROC曲线分析DCE-MRI、DWI单独及联合对乳腺癌的诊断效能。结果恶性组病灶形状为分叶状、不规则形(43.04%、45.65%),边缘毛刺(48.70%),内部不均匀强化、簇集状强化、分支强化(20.87%、38.70%、36.09%),时间-信号强度曲线类型Ⅲ型(43.04%)患者占比高于良性组(33.33%、15.48%、12.70%、8.33%、14.29%、19.05%、3.57%,P < 0.05)。DCE-MRI、DWI单独及联合诊断乳腺良性和恶性病变分别187例、215例、239例和166例、193例、218例,检出率分别为74.21%、85.32%、94.84%和72.17%、83.91%、94.78%,DWI单独及DCE-MRI、DWI联合诊断乳腺良性和恶性病变检出率高于DCE-MRI单独诊断,DCE-MRI、DWI联合诊断高于DWI单独诊断(P < 0.05)。DWI单独及DCE-MRI、DWI联合诊断乳腺良性和恶性病变的敏感度(83.91%、94.78%)、特异性(85.32%、94.84%)、曲线下面积(0.846、0.948)均高于DCE-MRI单独诊断(72.17%、74.21%、0.732),DCE-MRI、DWI联合诊断高于DWI单独诊断(P < 0.05)。 结论 DCE-MRI、DWI诊断乳腺良恶性病变具有特异的影像学特点,两者联合可有效提高对乳腺良恶性病变的诊断效能,具有较好的应用价值。 Abstract:Objective To analyze the imaging characteristics of dynamic contrast-enhanced MRI (DCE- MRI) and diffusion-weighted imaging (DWI) of breast cancer and the efficacy of combined diagnosis. Methods The clinical data of 230 patients with breast cancer admitted to our hospital from June 2018 to August 2022 were retrospectively collected as the malignant group, and the clinical data of 252 patients with benign breast lesions who were examined and treated in our hospital during the same period were selected as the benign group. All patients were diagnosed by surgery or pathological puncture biopsy. The imaging characteristics of DCE-MRI and DWI in patients with benign and malignant breast lesions were counted, and the diagnostic results of DCE- MRI and DWI alone and in combination were counted. ROC curve was used to analyze the diagnostic efficacy of DCE- MRI and DWI alone and in combination for breast cancer. Results In the malignant group, the lesions were lobulated and irregular (43.04%, 45.65%), with marginal burrs (48.70%), internal heterogeneous enhancement, cluster enhancement and branching enhancement (20.87%, 38.70%, 36.09%), and the proportion of patients with TIC type Ⅲ (43.04%) was higher than that in benign group (33.33%, 15.48%, 12.70%, 8.33%, 14.29%, 19.05%, 3.57%, P < 0.05). DCE-MRI and DWI alone and jointly diagnosed benign and malignant breast lesions in 187 cases, 215 cases, 239 cases, 166 cases, 193 cases and 218 cases respectively, and the detection rates were 74.21%, 85.32%, 94.84% and 72.17%, 83.91%, 94.78%, respectively. The detection rate of benign and malignant breast lesions diagnosed by DWI alone and DCE-MRI combined with DWI was higher than that by DCE- MRI alone, and that by DCE- MRI combined with DWI was higher than that by DWI alone (P < 0.05).The sensitivity (83.91%, 94.78%), specificity (85.32%, 94.84%) and area under the curve (0.846, 0.948) of DWI alone and DCE-MRI combined with DWI in diagnosing benign and malignant breast lesions were higher than those of DCE- MRI alone (72.17%, 74.21%, 0.732), the combined diagnosis of DCE-MRI and DWI was higher than that of DWI alone (P < 0.05). Conclusion DCE-MRI and DWI have specific imaging characteristics in the diagnosis of benign and malignant breast lesions. The combination of DCE-MRI and DWI can effectively improve the diagnostic efficiency of benign and malignant breast lesions and had good application value. -
图 2 患者女,41岁,发现乳房肿块2周
Figure 2. A 41-year-old female patient, breast lump found 2 weeks ago. A: On T2WI, nodular signal was slightly higher in the upper quadrant of the right outer breast, the size was about 20 mm×16 mm×21 mm, the boundary was clear, and the lesion edge showed shallow lobular changes and burr changes. B: T1WI showed slightly low signal; C: DWI showed high signal; D: ADC value decreased; E: The enhancement scan showed uneven enhancement; F-G: The enhancement curve with mass as the area of interest showed rapid rise and slow decline type (TIC Ⅲ type).
表 1 乳腺良恶性病变患者DCE-MRI及DWI的影像学特点比较
Table 1. Comparison of imaging characteristics of DCE-MRI and DWI in patients with benign and malignant breast lesions [n(%)]
Imaging features Benign group(n=252) Malignant group(n=230) χ2/Z P Lesion shape 87.688 < 0.001 Circle or oval 129(51.19) 26(11.30) Lobulate 84(33.33) 99(43.04) Irregular shape 39(15.48) 105(45.65) Edge 74.376 < 0.001 Burr 32(12.70) 112(48.70) Irregularity 111(44.05) 104(45.22) Smooth 109(43.25) 14(6.09) Perifocal edema 48(19.05) 35(15.22) 1.238 0.266 Skin thickening 21(8.33) 16(6.96) 0.322 0.571 Papillary involvement 41(16.27) 24(10.43) 3.509 0.061 Axillary lymph node enlargement 122(48.41) 103(44.78) 0.637 0.425 Internal reinforcement 15.407 < 0.001 Uniform strengthening 84(33.33) 10(4.35) Uneven strengthening 21(8.33) 48(20.87) Point hardening 63(25.00) 0(0.00) Cluster enhancement 36(14.29) 89(38.70) Branch reinforcement 48(19.05) 83(36.09) TIC type 107.760 < 0.001 Type Ⅰ 160(63.49) 40(17.39) Type Ⅱ 83(32.94) 91(39.57) Type Ⅲ 9(3.57) 99(43.04) DWI signal 3.784 0.483 High homogeneity signal 83(32.94) 74(32.17) High signal inhomogeneity 112(44.44) 119(51.74) Uniformity and other signals 11(4.37) 0(0.00) Inhomogeneity and other signals 6(2.38) 7(3.04) Low homogeneity signal 17(6.75) 8(3.48) Low signal inhomogeneity 23(9.13) 22(9.57) TIC: Time-signal intensity curve; DWI: Diffusion-weighted imaging. 表 2 DCE-MRI、DWI单独及联合对乳腺癌的诊断结果比较
Table 2. Comparison of DCE-MRI and DWI alone and in combination with the diagnosis of breast cancer (n)
Imaging method Pathology results Grand total Malignancy Benign DCE-MRI Malignancy 166 65 231 Benign 64 187 251 Grand total 230 252 482 DWI Malignancy 193 37 230 Benign 37 215 252 Grand total 230 252 482 Combined Malignancy 218 13 231 Benign 12 239 251 Grand total 230 252 482 DCE-MRI: Dynamic contrast-enhanced MRI. 表 3 DCE-MRI、DWI单独及联合对乳腺癌的诊断效能比较
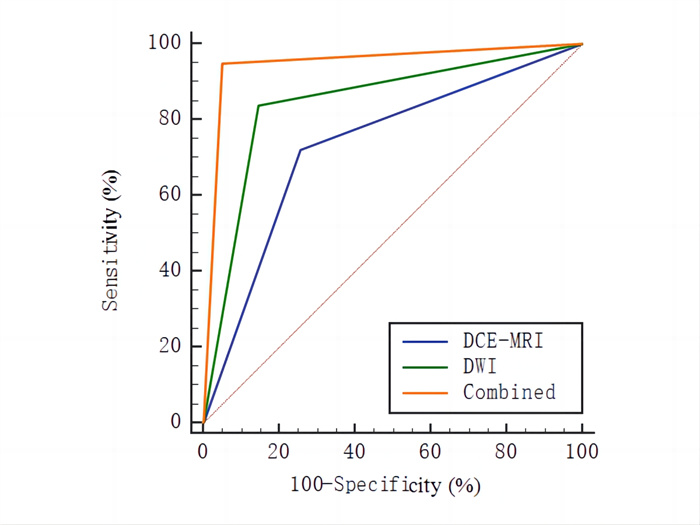
Table 3. Comparison of the diagnostic performance of DCE-MRI and DWI alone and in combination on breast cancer
Imaging method Sensitivity(%) Specificity(%) AUC 95% CI DCE-MRI 72.17 74.21 0.732 0.690-0.771 DWI 83.91* 85.32* 0.846* 0.811-0.877 Combined 94.78*# 94.84*# 0.948*# 0.924-0.966 *P < 0.05 vs DCE-MRI; #P < 0.05 vs DWI; AUC: Area under the curve. -
[1] Grabher BJ. Breast cancer: evaluating tumor estrogen receptor status with molecular imaging to increase response to therapy and improve patient outcomes[J]. J Nucl Med Technol, 2020, 48(3): 191-201. doi: 10.2967/jnmt.119.239020 [2] 孙瑞红, 王翔, 沈丽娟, 等. 乳腺癌患者MRI体素内不相干运动成像中感兴趣区选择方法对参数一致性的影响[J]. 中国癌症杂志, 2019, 2(9): 700-8. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGAZ201909005.htm [3] 吴佩琪, 赵可, 吴磊, 等. 基于扩散加权成像和动态增强MRI的影像组学特征与乳腺癌分子分型的关系初探[J]. 中华放射学杂志, 2018, 52(5): 338-43. https://www.cnki.com.cn/Article/CJFDTOTAL-YWLC201923008.htm [4] 黎国屏, 王松鹤. 实用临床乳腺病学[M]. 北京: 中国医药科技出版社, 2002: 178-183. [5] 王建华, 王红昆, 李辉, 等. 1.5T MRI结合数字化X线钼靶在乳腺癌诊断、TNM分期及疗效评估中的应用价值[J]. 中国医师杂志, 2019, 21(1): 134-6. https://www.cnki.com.cn/Article/CJFDTOTAL-CTMR202305044.htm [6] Komorowski AS, Pezo RC. Untapped"-omics": the microbial metagenome, estrobolome, and their influence on the development of breast cancer and response to treatment[J]. Breast Cancer Res Treat, 2020, 179(2): 287-300. doi: 10.1007/s10549-019-05472-w [7] Corso G, Magnoni F. Hereditary breast cancer: translation into clinical practice of recent American Society of Clinical Oncology, American Society of Radiation Oncology, and Society of Surgical Oncology recommendations[J]. Eur J Cancer Prev, 2020, 30(4): 311-4. [8] 许帮彦, 吴天斌, 陆建良, 等. MRI对乳腺癌的诊断效能及其征象和分子生物学标记物的相关性[J]. 中国妇幼保健, 2021, 36(15): 3636-9. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFYB202115069.htm [9] 于晓军, 陈永升, 王春艳, 等. MRI表现及ADC直方图对预测乳腺浸润性导管癌脉管浸润的价值[J]. 临床放射学杂志, 2020, 39(2): 294-8. https://www.cnki.com.cn/Article/CJFDTOTAL-LCFS202002017.htm [10] 孙恒翠, 郭依廷, 姚刚, 等. 乳腺癌MRI动态增强征象与免疫组化指标间的相关性分析[J]. 医学影像学杂志, 2022, 32(7): 1170-4. https://www.cnki.com.cn/Article/CJFDTOTAL-XYXZ202207019.htm [11] 杨晶, 杨国财, 刘金昊. 动态增强MRI定量参数与乳腺癌生物因子的相关性[J]. 中国介入影像与治疗学, 2018, 15(2): 86-9. https://www.cnki.com.cn/Article/CJFDTOTAL-JRYX201802010.htm [12] 单嫣娜, 龚向阳, 丁忠祥, 等. 动态增强MRI影像组学特征预测乳腺癌腋窝淋巴结转移的价值[J]. 中华放射学杂志, 2019, 53(9): 742-7. [13] 罗益贤, 马捷, 刘永光, 等. 动态增强MRI对乳腺癌新辅助化疗的疗效评价及预测[J]. 中国医学物理学杂志, 2019, 36(7): 794-9. https://www.cnki.com.cn/Article/CJFDTOTAL-YXWZ201907010.htm [14] 王倩, 刘万花, 王瑞, 等. 3.0T动态增强MRI定量参数、表观扩散系数与乳腺癌预后因子及分子分型的相关性[J]. 中国医学影像学杂志, 2019, 27(7): 517-21. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYYZ201907011.htm [15] 佟颖, 米楠, 张荣, 等. 磁共振扩散加权成像(DWI)评估进展期乳腺癌患者新辅助化疗近期疗效及病理变化的价值研究[J]. 影像科学与光化学, 2020, 38(2): 307-12. https://www.cnki.com.cn/Article/CJFDTOTAL-GKGH202002024.htm [16] 邢健, 汤洋, 李奇, 等. 3.0T磁共振弥散加权成像表观扩散系数与乳腺癌病理类型分级相关性的临床价值研究[J]. 中国CT和MRI杂志, 2020, 18(10): 54-7, 83. https://www.cnki.com.cn/Article/CJFDTOTAL-CTMR202010017.htm [17] 张晖, 王勇, 赵庆秋, 等. 高场强磁共振灌注成像联合扩散加权成像对肉芽肿性乳腺炎与乳腺癌的鉴别诊断研究[J]. 河北医药, 2020, 42(4): 512-6. https://www.cnki.com.cn/Article/CJFDTOTAL-HBYZ202004007.htm [18] 詹茸婷, 陈兵, 王晓东, 等. 动态增强MRI联合DWI对非肿块型乳腺癌与肉芽肿性乳腺炎的鉴别诊断价值[J]. 磁共振成像, 2018, 9(12): 948-52. https://www.cnki.com.cn/Article/CJFDTOTAL-CGZC201812013.htm [19] 李金红, 陈志忠. 磁共振动态增强扫描时间-信号强度曲线联合磁共振扩散加权成像表观扩散系数在乳腺癌诊断中的应用价值[J]. 中国妇幼保健, 2021, 36(6): 1423-6. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFYB202106066.htm [20] 牛微, 罗娅红, 于韬, 等. 基于动态对比增强MRI的肿瘤血流动力学及形态学特征预测乳腺癌术后复发时间的价值[J]. 中华放射学杂志, 2020, 54(3): 209-14. [21] 张俊杰, 杨晓棠, 杜笑松, 等. 隐匿性乳腺癌的MRI表现及临床病理特征[J]. 中华肿瘤杂志, 2018, 40(1): 40-5. https://www.cnki.com.cn/Article/CJFDTOTAL-YXYY201911014.htm [22] 张启川, 熊廷伟, 张曦, 等. 新辅助化疗后乳腺癌瘤床MRI表现与病理对比研究[J]. 局解手术学杂志, 2019, 28(7): 529-32. https://www.cnki.com.cn/Article/CJFDTOTAL-JJXZ201907005.htm [23] 柏晓茹, 郑建, 罗娅红. 不同分子亚型乳腺癌患者MRI定量增强参数比较[J]. 中国CT和MRI杂志, 2021, 19(12): 78-80. https://www.cnki.com.cn/Article/CJFDTOTAL-CTMR202112025.htm [24] 谢海涛, 张洋, 黎庶, 等. 乳腺癌的MRI影像特征与PTEN和PCNA表达的相关性研究[J]. 解剖科学进展, 2019, 25(2): 139-41, 145. https://www.cnki.com.cn/Article/CJFDTOTAL-JPKX201902008.htm [25] 罗红兵, 杨定彬, 王春华, 等. 三阴性乳腺癌与Luminal A型乳腺癌的MRI背景实质强化差异比较[J]. 中国医学影像学杂志, 2022, 30(8): 770-5. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYYZ202208004.htm [26] 杨培, 常晓丹, 付姣慧, 等. DCE-MRI参考区域模型联合DWI对lu-minal型乳腺癌的应用研究[J]. 放射学实践, 2018, 33(7): 688-93. https://www.cnki.com.cn/Article/CJFDTOTAL-FSXS201807012.htm -







 下载:
下载: