Diagnostic efficacy of ultrasound before minimally invasive cholelithiasis and the risk factors of postoperative recurrence in patients with cholecystolithiasis
-
摘要:
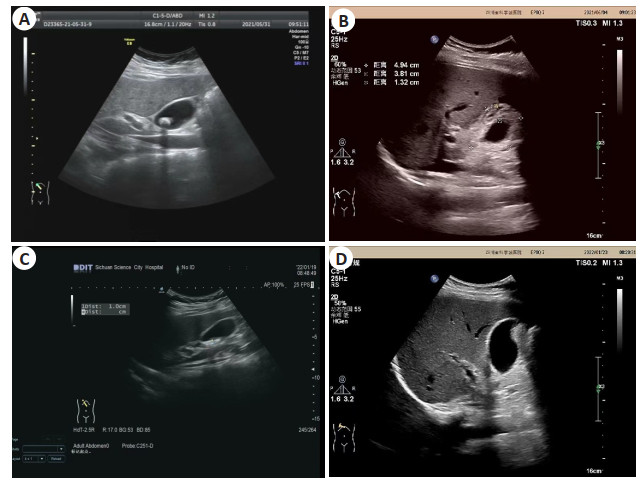
目的 分析胆囊结石患者微创保胆取石术前彩色多普勒超声(CDFI)诊断效能及术后复发的高危因素。 方法 选取2017年1月~2020年1月本院收治的90例拟行微创保胆取石术的胆囊结石患者为研究对象,所有患者在术前均接受CDFI检查,观察胆囊结石患者CDFI表现,并以手术结果为金标准,采用Kappa检验评价其诊断结果的一致性,采用ROC曲线评估CDFI诊断胆囊结石的效能,计算曲线下面积;术后随访2年,统计胆囊结石复发情况,采用单因素和多因素Logistic回归分析影响患者术后复发的高危因素。 结果 术前,胆囊内结石表现为不规则形、圆形或类圆形低信号影;胆囊保肝取石术后,大小约4.9 cm×1.8 cm,壁增厚,约1.3 cm,内壁见点状强回声附着,后方伴彗星尾,腔内透声好,胆囊未见明显积液;90例患者中,金标准诊断显示阳性81例,阴性9例,CDFI诊断显示阳性74例,阴性16例,其诊断结果与手术一致性较好(Kappa值=0.524);ROC曲线显示,CDFI诊断胆囊结石的曲线下面积为0.840,敏感度为90.12%,特异性为77.78%;术后随访2年,有12例患者复发,单因素和多因素Logistic回归分析结果显示,胆石症家族史、胆囊壁厚度、结石数量均是影响胆囊结石患者术后复发的高危因素(P < 0.05)。 结论 CDFI对胆囊结石患者微创保胆取石术前诊断具有较好的效能,胆石症家族史、胆囊壁厚度、结石数量均是胆囊结石患者术后复发的高危因素。 Abstract:Objective To analyze the diagnostic efficacy of preoperative color Doppler flow image (CDFI) and the risk factors of postoperative recurrence in patients with cholecystolithiasis with minimally invasive cholelithotomy. Methods A total of 90 patients with cholecystolithiasis who were proposed to undergo minimally invasive gallbladder-preserving lithotomy treated in our hospital from January 2017 to January 2020 were selected. All patients underwent CDFI examination before surgery, and the manifestations of CDFI in patients with cholecystolithiasis were observed. Using surgical results as the gold standard, Kappa test was used to evaluate the consistency of the diagnostic results, ROC curve was used to evaluate the efficacy of CDFI in diagnosing gallbladder stones, and AUC was calculated. Follow-up for 2 years after operation, the recurrence of cholecystolithiasis was counted, and univariate and multivariate Logistic regression was used to analyze the high-risk factors for postoperative recurrence. Results Before operation, the gallbladder stones were irregular, round or quasi-round low signal shadows. After gallbladder hepatoprotective lithotripsy, the size was about 4.9 cm ×1.8 cm, the wall was thickened, with the thickness of 1.3 cm, and the inner wall saw dot strong echo attachment, rear accompanied by the comet tail, good sound in the cavity, gallbladder did not see obvious effusion. Among the 90 patients, 81 cases were positive and 9 cases were negative by gold standard diagnosis, 74 cases were positive and 16 cases were negative by CDFI diagnosis, the diagnostic results were in good agreement with surgery (Kappa value=0.524). The ROC curve showed that the AUC of CDFI in diagnosing gallstones was 0.840, with a sensitivity of 90.12% and a specificity of 77.78%. After 2 years of postoperative follow-up, there were 12 cases had relapsed. Univariate and multivariate Logistic regression analysis showed that the family history of cholelithiasis, the thickness of the gallbladder wall, and the number of stones were all high risk factors for postoperative recurrence in patients with cholecystolithiasis (P < 0.05). Conclusion CDFI has a good effect on the preoperative diagnosis of cholecystolithiasis patients with minimally invasive gallbladder-preserving lithotomy. Family history of cholelithiasis, thickness of gallbladder wall, and number of stones are high risk factors for postoperative recurrence in patients with cholecystolithiasis. -
表 1 胆囊结石CDFI检查诊断情况
Table 1. CDFI diagnosis of gallstones (n)
CDFI 金标准 合计 Kappa 阳性 阴性 阳性 73 2 74 阴性 10 7 16 0.524 合计 81 9 90 CDFI: 彩色多普勒超声. 表 2 胆囊结石患者术后复发高危因素单因素分析
Table 2. Univariate analysis of risk factors for postoperative recurrence of gallstone patients [n(%)]
项目 未复发组(n=78) 复发组(n=12) t/χ2 P 性别 0.0207 0.649 男 38(48.72) 5(41.67) 女 40(51.28) 7(58.33) 年龄(岁, Mean±SD) 47.59±7.11 47.25±6.82 0.155 0.877 BMI(kg/m2, Mean±SD) 23.82±1.68 23.59±1.57 0.445 0.657 胆石症家族史 9.084 0.003 有 12(15.38) 7(58.33) 无 66(84.62) 5(41.67) 饮食情况 0.260 0.878 荤 17(21.79) 3(25.00) 混 43(55.13) 7(58.33) 素 18(23.08) 2(16.67) 胆囊壁厚度(mm) 5.301 0.021 < 4 56(71.79) 4(33.33) ≥4 22(28.21) 8(66.67) 结石大小(mm) 0.335 0.563 < 8 30(38.46) 3(25.00) ≥8 48(61.54) 9(75.00) 结石数量 5.654 0.017 单发 48(61.54) 3(25.00) 多发 30(38.46) 9(75.00) 结石成分 0.310 0.856 胆固醇型 20(25.64) 3(25.00) 胆色素型 33(42.31) 6(50.00) 混合型 25(32.05) 3(25.00) 合并基础疾病 5.812 0.016 是 21(26.92) 8(66.67) 否 57(73.08) 4(33.33) 表 3 胆囊结石患者术后复发高危因素多因素Logistic回归分析
Table 3. Multivariate Logistic regression analysis of risk factors for postoperative recurrence of gallstone patients
项目 β SE Wald χ2 OR P 95% CI 胆石症家族史 3.051 1.473 4.290 21.136 0.039 1.178~379.206 胆囊壁厚度 1.325 0.558 5.638 3.762 0.018 1.260~11.231 结石数量 2.020 0.677 8.903 7.538 0.003 2.000~28.415 合并基础疾病 0.879 0.520 2.857 2.408 0.092 0.869~6.674 -
[1] 钱英, 田应彪, 王玉和. 胆囊结石的形成及常用药物的研究进展[J]. 现代医药卫生, 2018, 34(5): 720-2. https://www.cnki.com.cn/Article/CJFDTOTAL-XYWS201805026.htm [2] Zhang Y, Peng J, Li XL, et al. Endoscopic- laparoscopic cholecystolithotomy in treatment of cholecystolithiasis compared with traditional laparoscopic cholecystectomy[J]. Surg Laparosc Endosc Percutan Tech, 2016, 26(5): 377-80. doi: 10.1097/SLE.0000000000000305 [3] Fishman DS, Chumpitazi BP, Raijman I, et al. Endoscopic retrograde cholangiography for pediatric choledocholithiasis: assessing the need for endoscopic intervention[J]. World J Gastrointest Endosc, 2016, 8(11): 425-32. doi: 10.4253/wjge.v8.i11.425 [4] 卓世鹏, 李建明, 冯伟静. 微创保胆取石与腹腔镜手术对胆结石患者胃肠功能及预后的影响[J]. 海南医学, 2020, 31(3): 316-8. https://www.cnki.com.cn/Article/CJFDTOTAL-HAIN202003013.htm [5] 凌永霞. 彩色多普勒超声在胆囊结石诊断中的应用价值[J]. 医疗装备, 2020, 33(5): 24-5. https://www.cnki.com.cn/Article/CJFDTOTAL-YLZB202005014.htm [6] Huang WN, Chen LB, Xu N, et al. Diagnostic value and safety of color Doppler ultrasound-guided transthoracic core needle biopsy of thoracic disease[J]. Biosci Rep, 2019, 39(6): BSR20190104. doi: 10.1042/BSR20190104 [7] 汪劲松, 卢慧鸣, 王小凤. 超声对胆囊结石腹腔镜术前患者的筛查及粘连判断[J]. 中国现代普通外科进展, 2019, 22(7): 554-5, 559. https://www.cnki.com.cn/Article/CJFDTOTAL-PWJZ201907016.htm [8] Editorial Board of Chinese Journal of Digestion; . 中国慢性胆囊炎、胆囊结石内科诊疗共识意见(2014年, 上海)[J]. 临床肝胆病杂志, 2015, 31(1): 795-9. https://xuewen.cnki.net/CCND-JFRB202211070012.html [9] Shabanzadeh DM, Sørensen LT, Jørgensen T. Gallstone disease and mortality: a cohort study[J]. Int J Public Health, 2017, 62(3): 353- 60. doi: 10.1007/s00038-016-0916-7 [10] Shabanzadeh DM. Incidence of gallstone disease and complications [J]. Curr Opin Gastroenterol, 2018, 34(2): 81-9. doi: 10.1097/MOG.0000000000000418 [11] Zhu L, Wu X, Sun ZY, et al. Compressed-sensing accelerated 3- dimensional magnetic resonance cholangiopancreatography[J]. Invest Radiol, 2018, 53(3): 150-7. doi: 10.1097/RLI.0000000000000421 [12] Garg B, et al. Evaluation of biliary complications on magnetic resonance cholangiopancreatography and comparison with direct cholangiography after living-donor liver transplantation[J]. Clin Radiol, 2017, 72(6): 518. e9-518. e15. doi: 10.1016/j.crad.2016.12.019 [13] Hajjar R, Létourneau A, Henri M, et al. Cholecystocolonic fistula with a giant colonic gallstone: the mainstay of treatment in an acute setting[J]. J Surg Case Rep, 2018, 2018(10): 278. [14] 张杰, 张宁英, 马淑梅. 磁共振成像与彩色多普勒超声诊断胆道结石临床价值比较[J]. 实用肝脏病杂志, 2020, 23(5): 747-50. https://www.cnki.com.cn/Article/CJFDTOTAL-GBSY202005037.htm [15] 陈玲玲. 彩色多普勒超声诊断胆囊结石的诊断效能[J]. 现代诊断与治疗, 2022, 33(3): 427-30. https://www.cnki.com.cn/Article/CJFDTOTAL-XDZD202203039.htm [16] Yang MF, Shi Y. Diagnostic value of ultrasound combined with MRI in cholecystolithiasis: a protocol for systematic review and meta analysis[J]. Medicine, 2021, 100(19): e25896. [17] Panda N, Chang Y, Chokengarmwong N, et al. Gallstone pancreatitis and choledocholithiasis: using imaging and laboratory trends to predict the likelihood of persistent stones at cholangiography[J]. World J Surg, 2018, 42(10): 3143-9. [18] 王红伟, 刘江伟, 王伟智, 等. 新疆汉族、维吾尔族患者保胆取石术后结石复发的危险因素分析[J]. 中华普通外科学文献: 电子版, 2018, 12(6): 388-92. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHPD201806006.htm [19] 刘永茂, 李之令, 刘江伟, 等. 微创保胆术后胆囊结石、息肉复发相关因素分析[J]. 山东医药, 2017, 57(23): 94-6. https://www.cnki.com.cn/Article/CJFDTOTAL-SDYY201723030.htm [20] 刘强, 陈士水, 邵慧成, 等. 保胆取石术后结石复发的相关影响因素分析[J]. 中国普通外科杂志, 2018, 27(8): 983-8. https://www.cnki.com.cn/Article/CJFDTOTAL-ZPWZ201808011.htm [21] 李骜, 刘江伟, 张东. 内镜微创保胆取石术后胆囊结石复发的研究进展[J]. 肝胆胰外科杂志, 2019, 31(9): 573-7. https://www.cnki.com.cn/Article/CJFDTOTAL-GDYW201909017.htm [22] Kokoroskos N, et al. Gallbladder wall thickness as a predictor of intraoperative events during laparoscopic cholecystectomy: a prospective study of 1089 patients[J]. Am J Surg, 2020, 220(4): 1031-7. [23] 司宇光, 张国超. 胆囊结石合并胆总管结石病人LC联合LCHTD术后结石复发情况及其影响因素分析[J]. 蚌埠医学院学报, 2018, 43 (2): 223-6. https://www.cnki.com.cn/Article/CJFDTOTAL-BANG201802025.htm -







 下载:
下载: