Application value of 3.0T magnetic resonance imaging in carotid atherosclerotic plaque composition examination of ischemic stroke
-
摘要:
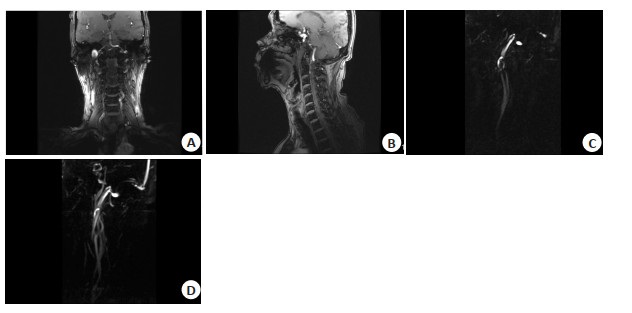
目的 探究3.0 T MRI在缺血性脑卒中颈动脉粥样硬化斑块成分检查中的临床应用。 方法 选择我院及上海交通大学附属第六人民医院2020年6月~2021年4月收治的62例因颈动脉粥样硬化所致的缺血性脑卒中患者作为研究对象。采用3.0 T MRI对所有患者颈动脉血管狭窄处的斑块成分及不同类型斑块的信号特征进行观察、分析,对比稳定斑块、不稳定斑块组成成分的差异。 结果 共发现颈动脉粥样硬化斑块119个,斑块分型:Ⅰ~Ⅱ型11个(9.24%),Ⅲ型31个(26.05%),Ⅳ~Ⅴ型24个(20.17%),Ⅵ型37个(31.09%),Ⅶ型16个(13.45%)。所有斑块在MRI上均表现为环形或偏心性管壁增厚,且部分伴有局部新月形或半月形信号突入管腔,不同成分斑块在MRI上的表现各有所不同。所有检出的颈动脉斑块中稳定斑块共计62个,不稳定斑块57个。稳定斑块和不稳定斑块出现钙化的差异无统计学意义(P > 0.05),不稳定斑块出现脂质核心、出血、血栓形成以及纤维帽破裂的比例高于稳定斑块,差异有统计学意义(P < 0.05)。 结论 3.0 T MRI能够对缺血性脑卒中患者的颈动脉粥样硬化斑块内部成分及稳定性作出准确评价,可为缺血性脑卒中的临床预测及病情评价提供重要参考。 Abstract:Objective To explore the clinical application of 3.0T MRI in carotid atherosclerotic plaque composition examination of ischemic stroke. Methods Sixty-two patients with ischemic stroke caused by carotid atherosclerosis in our hospital and Shanghai Jiaotong University affiliated sixth People's Hospital from June 2020 to April 2021 were selected. 3.0T MRI was used to observe and analyze the plaque composition and signal characteristics of different types of plaques in all patients with carotid artery stenosis. The difference between stable plaque and unstable plaque composition was compared. Results A total of 119 carotid atherosclerotic plaques were found in 62 patients. Patch classification: 11 cases were type Ⅰ-Ⅱ (9.24%), 31 cases were type Ⅲ (26.05%), 24 cases were type Ⅳ-Ⅴ (20.17%), 37 cases were type Ⅵ (31.09%), 16 cases were type Ⅶ (13.45%). All plaques showed annular or eccentric wall thickening on MRI, and some of them were accompanied by local crescent or semilunar signal penetrating into the lumen. The manifestations of plaques with different components were different on MRI. There were 62 stable plaques and 57 unstable plaques in all detected carotid plaques. There was no significant difference in the proportion of calcification between stable plaque and unstable plaque (P > 0.05). The proportion of lipid core, hemorrhage, thrombosis and fibrous cap rupture in unstable plaque was significantly higher than that in stable plaque (P < 0.05). Conclusion 3.0T MRI can accurately evaluate the internal composition and stability of carotid atherosclerotic plaques in patients with ischemic stroke. It provide important reference for clinical prediction and disease evaluation of ischemic stroke. -
表 1 3.0 T MRI扫描序列及参数
Table 1. 3.0 T MRI scanning sequence and parameters
扫描参数 3D-TOF FSE-T1WI FSE-T2WI PDWI TR(ms) 29 800 3000 3000 TE(ms) 2.1 8.9 13.1 57 FOV(cm) 14×14 14×14 14×14 14×14 层厚(mm) 2.0 2.0 2.0 2.0 层间距(mm) 1.0 1.0 1.0 1.0 矩阵 256×256 288×192 384×256 384×256 激励次数 1 2 2 2 3D-TOF: 三维时间飞跃法; FSE: 快速自旋回波; PDWI: 质子密度加权像. 表 2 不同成分斑块在MRI各序列上的信号表现
Table 2. Signal manifestions of plaques wity different components on MRI sequences
斑块成分 3D-TOF DIR-T1WI FSE-T2WI PDWI 脂质核心 等信号 等/稍低信号 稍低信号 等/稍低信号 出血 高信号 高信号 高信号 高信号 血栓 低信号 低信号 低信号 低信号 钙化 点条状低信号 点条状低信号 点条状低信号 点条状低信号 纤维帽破损 等/稍低信号 等/稍高信号 高信号 等/稍高信号 表 3 稳定性斑块和不稳定斑块的组成成分差异比较
Table 3. Comparison of composition differences between stable plaque and unstable plaque[n(%)]
斑块稳定性 含脂质核心 伴出血 形成血栓 含有钙化 纤维帽破裂 稳定斑块(n=62) 15(24.19) 7(11.29) 0(0.00) 12(19.35) 4(6.45) 不稳定斑块(n=57) 36(63.16) 23(40.35) 14(24.56) 15(26.32) 20(35.09) χ2 18.4107 13.3018 17.2585 0.8203 15.1254 P < 0.001 < 0.001 < 0.001 0.3651 < 0.001 -
[1] 王倩, 张亮. 颈动脉粥样硬化斑块与脑梗死关系的高分辨磁共振研究[J]. 中国实用神经疾病杂志, 2017, 20(17): 85-8. https://www.cnki.com.cn/Article/CJFDTOTAL-HNSJ201717029.htm [2] 李树强, 赵继泉, 杨侃荣, 等. 高分辨率磁共振成像在动脉粥样硬化斑块中的应用进展[J]. 海南医学, 2019, 30(12): 1596-9. doi: 10.3969/j.issn.1003-6350.2019.12.031 [3] Bassiouny HS, Sakaguchi Y, Mikucki SA, et al. Juxtalumenal location of plaque necrosis and neoformation in symptomatic carotid stenosis [J]. J Vasc Surg, 1997, 26(4): 585-94. doi: 10.1016/S0741-5214(97)70056-9 [4] 范存雷, 孙艳华, 陈少武, 等. 3.0T高分辨磁共振不同成像序列对大脑中动脉粥样硬化斑块成分分析[J]. 中国临床医学影像杂志, 2018, 29 (4): 234-7. doi: 10.3969/j.issn.1008-1062.2018.04.002 [5] Johansson E, Zarrinkoob L, WåhlinA, et al. Diagnosing carotinearoc clusion with phase-contrast MRI[J]. AJNR Am J Neuroradiol, 2021, 42(5): 927-9. doi: 10.3174/ajnr.A7076 [6] Cai JM, Hatsukami TS, Ferguson MS, et al. Classification of human carotid atherosclerotic lesions with in vivo multicontrast magnetic resonance imaging[J]. Circulation, 2002, 106(11): 1368-73. doi: 10.1161/01.CIR.0000028591.44554.F9 [7] 赵鑫, 夏章勇, 王晓婷, 等. 高分辨率磁共振评价颅内动脉粥样硬化性疾病的研究进展[J]. 中华老年心脑血管病杂志, 2017, 19(11): 1220-3. doi: 10.3969/j.issn.1009-0126.2017.11.027 [8] 陈潇祎, 庄仲, 赵锡海. 颈动脉粥样硬化斑块进展与脑缺血事件相关性的影像学研究进展[J]. 中国卒中杂志, 2017, 12(6): 538-43. doi: 10.3969/j.issn.1673-5765.2017.06.014 [9] 田霞, 张雪凤, 彭雯佳, 等. 三维高分辨率磁共振管壁成像在评估非狭窄性颅内动脉粥样硬化所致缺血性脑卒中复发中的价值[J]. 海军军医大学学报, 2022, 43(5): 511-8. https://www.cnki.com.cn/Article/CJFDTOTAL-DEJD202205004.htm [10] 白雪芹, 李秋平, 吕鹏, 等. 三维高分辨率磁共振血管壁成像用于研究颅内动脉粥样硬化斑块强化与缺血性卒中的关系[J]. 复旦学报: 医学版, 2018, 45(3): 341-6. doi: 10.3969/j.issn.1672-8467.2018.03.009 [11] Glisic M, Mujaj B, Rueda-Ochoa OL, et al. P4307Associations of endogenous estradiol and testosterone levels with plaque composition and risk of stroke in subjects with carotid atherosclerosis [J]. Eur Heart J, 2017, 38(suppl-1): ehx504.P4307. [12] 高鑫, 朱婉秋, 刘福军, 等. 高分辨血管MR成像对急性脑梗死患者大脑中动脉粥样硬化斑块的诊断价值[J]. 湖南师范大学学报: 医学版, 2020, 17(3): 69-72. https://www.cnki.com.cn/Article/CJFDTOTAL-HNYG202003022.htm [13] Ding HJ, Wang CG, Malkasian S, et al. Characterization of arterial plaque composition with dual energy computed tomography: a simulation study[J]. Int J Cardiovasc Imaging, 2021, 37(1): 331-41. doi: 10.1007/s10554-020-01961-y [14] 何思锦, 李颖彬, 张燕婷, 等. 采用高分辨率核磁共振评价颅内动脉粥样硬化斑块稳定性与卒中复发风险的关系[J]. 中国脑血管病杂志, 2017, 14(7): 351-5. https://www.cnki.com.cn/Article/CJFDTOTAL-NXGB201707004.htm [15] Benson JC, Cheek H, Aubry MC, et al. Cervical carotid plaque MRI: review of atherosclerosis imaging features and their histologic underpinnings[J]. Clin Neuroradiol, 2021, 31(2): 295-306. doi: 10.1007/s00062-020-00987-y [16] 孟志霞, 谭卫锋, 张亮. 磁共振成像对症状性颈动脉狭窄与粥样硬化斑块易损性的诊断价值[J]. 中国实用神经疾病杂志, 2017, 20(11): 65-7. https://www.cnki.com.cn/Article/CJFDTOTAL-HNSJ201711024.htm [17] 刘凯莉, 左春洁, 陈大有, 等. 彩色多普勒超声与CTA对脑梗死患者颈动脉粥样硬化斑块的形态特点和生物学特性的评估价值[J]. 湖南师范大学学报: 医学版, 2018, 15(2): 118-21. https://www.cnki.com.cn/Article/CJFDTOTAL-HNYG201802036.htm [18] Beddhu S, Boucher RE, Sun J, et al. Chronic kidney disease, atherosclerotic plaque characteristics on carotid magnetic resonance imaging, and cardiovascular outcomes[J]. BMC Nephrol, 2021, 22 (1): 69. [19] 张丹凤, 陈慧铀, 张卫东, 等. 高分辨率磁共振大脑中动脉粥样硬化斑块的分布及信号特点与脑梗死的关系[J]. 磁共振成像, 2017, 8(1): 4-7. https://www.cnki.com.cn/Article/CJFDTOTAL-CGZC201701004.htm [20] 彭少华, 王成伟. 老年颈动脉粥样硬化斑块患者磁共振检查结果与临床症状的相关性[J]. 中国老年学杂志, 2016, 36(19): 4749-51. https://www.cnki.com.cn/Article/CJFDTOTAL-ZLXZ201619034.htm [21] 曹文, 任翠龙, 孙艳霞. 常规超声、超声造影及超声弹性成像联合诊断高血压伴高同型半胱氨酸血症患者颈动脉粥样硬化斑块的价值[J]. 临床超声医学杂志, 2022, 24(8): 598-602. https://www.cnki.com.cn/Article/CJFDTOTAL-LCCY202208007.htm [22] 周晓梅, 任孝林, 周芯羽. 颈动脉易损斑块风险模型的构建及与急性脑梗死患者认知障碍和预后的关系[J]. 中国动脉硬化杂志, 2022, 30 (7): 606-10. https://www.cnki.com.cn/Article/CJFDTOTAL-KDYZ202207009.htm [23] Huang H, Virmani R, Younis H, et al. The impact of calcification on the biomechanical stability of atheroscleroticplaques[J]. Circulation, 2001, 103(8): 1051-6. [24] 徐贤, 具海月, 王新江, 等. 3T高分辨MR对颈动脉粥样硬化斑块表面钙化与斑块稳定性的量化分析[J]. 第二军医大学学报, 2008, 29 (12): 1483-6. https://www.cnki.com.cn/Article/CJFDTOTAL-DEJD200812018.htm [25] Huang S, Gong XJ, Guan S, et al. Clinical value of MRI T2-mapping quantitative assessment of carotid plaque[J]. Acta Radiol, 2020, 61 (8): 1021-5. -







 下载:
下载: