Factors influencing preoperative ultrasound suspicion of lymph node metastasis in the lateral cervical region of papillary thyroid cancer
-
摘要:
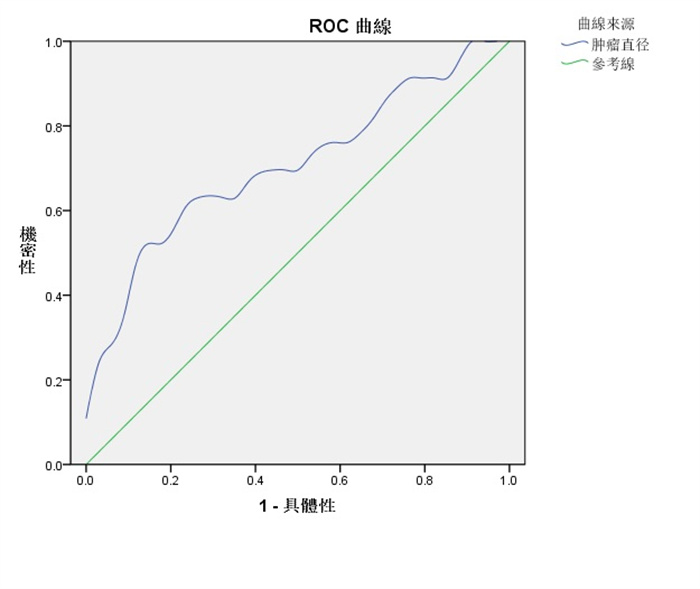
目的 探讨术前超声可疑甲状腺乳头状癌颈侧区淋巴结转移(LLNM)的相关影响因素。 方法 选取2010年1月~2021年1月于我院行门诊甲状腺常规超声检查高度怀疑甲状腺乳头状癌(PTC)患者80例,通过术前超声检查并接受手术治疗,术后经病理证实为PTC。通过术后病理分为颈侧区淋巴结转移组(LLNM组,n=46)、未发生颈侧区淋巴结转移组(NLLNM组,n=34),收集其临床特征与超声声像图特征,采用多因素Logistic分析术前超声可疑LLNM相关的独立因素,ROC曲线计算分析患者肿瘤直径预测LLNM的最佳临界值。 结果 单因素分析显示两组患者的性别、被膜侵犯、淋巴门、中央区淋巴结转移、肿瘤直径、微钙化及结节纵横比差异均有统计学意义(P < 0.05)。多因素分析显示男性、发生被膜侵犯、中央区淋巴结转移、肿瘤直径、结节微钙化均是与LLNM相关的独立危险因素。ROC曲线表明患者肿瘤直径曲线截断点为1.404 cm,对LLNM诊断的敏感度为52.2%、特异性为88.2%,曲线下面积为0.709。 结论 男性、发生被膜侵犯、中央区淋巴结转移、肿瘤直径≥1.404 cm、结节微钙化对甲状腺乳头状癌颈侧区淋巴结转移具有重要预测价值,关注上述危险因素,可增加颈侧区淋巴结的检出率。 Abstract:Objective To investigate the factors associated with preoperative ultrasound suspicion of lymph node metastasis (LLNM) in the lateral cervical region of papillary thyroid cancer. Methods From January 2010 to January 2021, our hospital line gland regular ultrasound examination of 80 patients with high suspicion of PTC were selected and treated with preoperative ultrasound and confirmed to have PTC by postoperative pathology. 80 patients were divided into a group with lymph node metastasis in the lateral cervical region (LLNM group, n=46) and a group without lymph node metastasis in the lateral cervical region (NLLNM group, n=34). NLLNM group, n=34), their clinical features and ultrasound sonographic features were collected, Independent factors related to preoperative ultrasound suspicion of LLNM were analyzed by multifactor Logistic analysis. The best critical value of LLNM was calculated from ROC curve by patient tumor diameter prediction. Results Univariate analysis showed statistically significant differences (P < 0.05) in gender, film violation, lymph node transfer, tumor diameter, and tumor diameter, nodule microcalification in the central area, and nodules of nodules were independent risk factors associated with LLNM. The ROC curve showed a tumour diameter cut-off point of 1.404 cm, with a sensitivity of 52.2% and specificity of 88.2%, and an area under the curve of 0.709. Conclusion Male, film violation, lymph node transfer, tumor diameter ≥1.404 cm, nodule microcetocrification on the lymph node metastasis of thyroid pillar carcinoma neck side zone has important predictive value, and attention to the above risk factors may increase the detection rate of the lymph nodes of the lateral cervical region. -
Key words:
- thyroid papillary carcinoma /
- lymph nodes of the neck /
- ultrasound examination /
- factors
-
表 1 PTC患者基本临床特征
Table 1. Basic clinical characteristics of PTC patients[n(%)]
临床特征 n (%) 年龄(岁,Mean±SD) 44.62±10.63 性別 女性 53 (66.25) 男性 27 (33.75) 手术方式 全切 52 (65.0) 近全切 8(10.0) 侧腺叶+峡部切除 20 (25.0) 肿瘤直径(cm, Mean±SD) 1.33±0.77 淋巴结转移 N0 28 (35.0) N1 52 (65.0) 术前血清促甲状腺激素水平(U/mL,Mean±SD) 3.47±2.64 淋巴结转移分组 中央区+颈侧区 28 (35.0) 中央区 11 (13.75) 颈侧区 17(21.25) 被膜侵犯 是 20 (25.0) 否 60 (75.0) 淋巴门 缺失 37 (46.25) 正常 43 (53.75) 合并桥本甲状腺炎 是 28 (35.0) 否 52 (65.0) 表 2 PTC患者基本临床特征的单因素分析
Table 2. Univariate analysis of basic clinical characteristics of PTC patients [n(%)]
临床特征 LLNM组(n=46) NLLNM组(n=34) χ2/t P 年龄(岁,Mean±SD) 42.65±11.32 45.67±12.03 1.149 0.254 性別 16.431 < 0.001 女性 22 (47.83) 31 (91.18) 男性 24 (52.17) 3 (8.82) 被膜侵犯 11.526 0.001 是 18(39.13) 2 (5.88) 否 28 (60.87) 32(94.12) 淋巴门 4.594 0.032 缺失 26 (56.52) 11 (32.35) 正常 20 (43.48) 23 (67.65) 合并桥本甲状腺炎 2.161 0.142 是 13 (28.76) 15 (44.12) 否 33 (71.74) 19 (55.88) 术前血清促甲状腺激素浓度(U/mL, Mean±SD) 3.56±2.07 3.24±2.33 0.648 0.519 LLNM: 颈侧区淋巴结转移;NLLNM:未发生颈侧区淋巴结转移. 表 3 PTC患者超声声像图特征的单因素分析
Table 3. Univariate analysis of ultrasonic image characteristics in patients with PTC[n(%)]
超声声像图特征 LLNM组 NLLNM组 χ2/t P 中央区淋巴结转移 6.363 0.012 是 28 (60.87) 11 (32.35) 否 18(39.13) 23 (67.65) 肿瘤直径(cm,Mean±SD) 1.53±0.88 1.04±0.51 2.903 0.005 结节位置 0.269 0.604 上极 18(39.13) 13 (38.23) 中部 14 (30.43) 9 (26.47) 下极 9 (19.58) 8 (23.54) 峡部 5 (10.86) 4(11.76) 回声 2.096 0.295 低回声 44 (95.65) 30 (88.24) 等回声 2 (4.35) 3 (8.82) 高回声 0 (0) 1 (2.94) 边界 0.223 0.637 光整 4 (8.70) 2 (5.88) 不光整 42 (91.30) 32(94.12) 微钙化 14.819 < 0.001 是 40 (86.96) 16(47.06) 否 6(13.04) 18 (52.94) 结节纵横比 4.684 0.030 > 1 11 (23.91) 16(47.06) < 1 35 (76.09) 18 (52.94) 结节血流 0.978 0.323 无 3 (6.52) 4(11.77) 低 28 (60.87) 21 (61.76) 中 11 (23.92) 6 (17.65) 高 4 (8.69) 3 (8.82) 表 4 相关变量赋值表
Table 4. Related variable assignment table
变量 赋值方法 因变量 LLNM组为1;NLLNM组为0 性別 女性=1;男性=0 被膜侵犯 是=1;否=0 淋巴门 缺失=1;正常=0 中央区淋巴结转移 是=1;否=0 肿瘤直径 采用实际值 微钙化 是=1;否=0 结节纵横比 > 1为1, < 1为0 表 5 PTC患者LLNM的多因素分析
Table 5. Multivariate analysis of PTC patients
影响因素 β SE Wald P OR 95%CI 性別 -2.108 0.834 6.234 0.013 0.125 (0.024, 0.639) 被膜侵犯 1.952 0.955 4.177 0.041 7.041 (1.083, 45.755) 淋巴门 0.275 0.707 0.151 0.698 1.316 (0.329,5.263) 中央区淋巴结转移 1.674 0.768 4.745 0.029 5.331 (1.183, 24.030) 肿瘤直径 1.232 0.555 4.935 0.026 3.429 (1.156, 10.172) 微钙化 1.805 0.827 4.767 0.029 6.081 (1.203, 30.738) 结节纵横比 -0.425 0.719 0.346 0.555 0.654 (0.160, 2.677) 常量 -2.110 1.335 2.496 0.114 0.121 -
[1] Abdullah MI, Junit SM, Ng KL, et al. Papillary thyroid cancer: genetic alterations and molecular biomarker investigations[J]. Int J Med Sci, 2019, 16(3): 450-60. doi: 10.7150/ijms.29935 [2] 叶磊, 朱亚娟, 丁作鹏, 等. 甲状腺乳头状癌侧颈区淋巴结转移的相关独立危险因素[J]. 分子影像学杂志, 2021, 44(3): 447-51. doi: 10.12122/j.issn.1674-4500.2021.03.06 [3] Lan XB, Bao H, Ge XY, et al. Genomic landscape of metastatic papillary thyroid carcinoma and novel biomarkers for predicting distant metastasis[J]. Cancer Sci, 2020, 111(6): 2163-73. doi: 10.1111/cas.14389 [4] Lewiński A, Adamczewski Z, Zygmunt A, et al. Correlations between molecular landscape and sonographic image of different variants of papillary thyroid carcinoma[J]. J Clin Med, 2019, 8(11): 1916. doi: 10.3390/jcm8111916 [5] 张伟红, 闫红莲, 魏云, 等. 超声检查诊断甲状腺癌合并淋巴结转移的临床研究[J]. 实用癌症杂志, 2021, 36(6): 954-8. doi: 10.3969/j.issn.1001-5930.2021.06.022 [6] 胡磊, 余盛敬, 王才善, 等. 多因素Logistic分析单灶甲状腺微小乳头状癌中央区淋巴结转移的危险因素[J]. 川北医学院学报, 2020, 35 (3): 453-7. doi: 10.3969/j.issn.1005-3697.2020.03.025 [7] Yu J, Deng Y, Liu T, et al. Lymph node metastasis prediction of papillary thyroid carcinoma based on transfer learning radiomics [J]. Nat Commun, 2020, 11(1): 4807. doi: 10.1038/s41467-020-18497-3 [8] 陈浩, 周永泽, 向远航, 等. 细针穿刺细胞学检查与细针穿刺洗脱液甲状腺球蛋白检测在甲状腺乳头状癌患者颈部淋巴结转移诊断中的价值[J]. 中华实用诊断与治疗杂志, 2022, 36(2): 190-2. https://www.cnki.com.cn/Article/CJFDTOTAL-HNZD202202019.htm [9] 傅迎霞, 张羽, 朱红, 等. 甲状腺乳头状癌颈侧区淋巴结转移的危险因素及影像诊断价值评估[J]. 医学影像学杂志, 2021, 31(8): 1287- 92. https://www.cnki.com.cn/Article/CJFDTOTAL-XYXZ202108008.htm [10] Li F, Pan DH, He Y, et al. Using ultrasound features and radiomics analysis to predict lymph node metastasis in patients with thyroid cancer[J]. BMC Surg, 2020, 20: 315. doi: 10.1186/s12893-020-00974-7 [11] Suh CH, Baek JH, Choi YJ, et al. Performance of CT in the preoperative diagnosis of cervical lymph node metastasis in patients with papillary thyroid cancer: a systematic review and meta-analysis [J]. AJNR Am J Neuroradiol, 2017, 38(1): 154-61. doi: 10.3174/ajnr.A4967 [12] 邱贝, 赵波, 董烨尧, 等. 甲状腺乳头状癌颈部侧区淋巴结转移的临床危险因素[J]. 河南医学研究, 2019, 28(10): 1749-52. doi: 10.3969/j.issn.1004-437X.2019.10.007 [13] Liu CX, Xiao C, Chen JJ, et al. Risk factor analysis for predicting cervical lymph node metastasis in papillary thyroid carcinoma: a study of 966 patients[J]. BMC Cancer, 2019, 19: 622. doi: 10.1186/s12885-019-5835-6 [14] Nie XL, Tan Z, Ge MH, et al. Risk factors analyses for lateral lymph node metastases in papillary thyroid carcinomas: a retrospective study of 356 patients[J]. Arch Endocrinol Metab, 2016, 60(5): 492-9. doi: 10.1590/2359-3997000000218 [15] 魏玉心. 甲状腺乳头状癌颈侧区淋巴结转移的相关危险因子研究[J]. 中国现代普通外科进展, 2020, 23(10): 786-8. https://www.cnki.com.cn/Article/CJFDTOTAL-PWJZ202010007.htm [16] 杨英, 王刚, 黄卫飞, 等. 甲状腺乳头状癌超声征象与颈侧区淋巴结转移的相关因素分析[J]. 临床超声医学杂志, 2018, 20(6): 388-92. doi: 10.3969/j.issn.1008-6978.2018.06.011 [17] Mao JX, Zhang QH, Zhang HY, et al. Risk factors for lymph node metastasis in papillary thyroid carcinoma: a systematic review and meta-analysis[J]. Front Endocrinol (Lausanne), 2020, 11: 265. doi: 10.3389/fendo.2020.00265 [18] 郑福庆, 张立永, 王波, 等. 甲状腺乳头状癌颈侧区淋巴结转移的危险因素研究进展[J]. 中华普通外科学文献: 电子版, 2020, 14(5): 384-7. doi: 10.3877/cma.j.issn.1674-0793.2020.05.018 [19] 乌云图, 金山, 刘友胜, 等. 中央区淋巴结转移强度对甲状腺乳头状癌颈侧区淋巴结转移的临床意义[J]. 中华内分泌外科杂志, 2021, 15 (1): 41-6. [20] 安程程, 张卫健, 朱金海, 等. 多灶性甲状腺乳头状癌的临床病理特点及颈部淋巴结转移规律[J]. 分子影像学杂志, 2019, 42(4): 490-4. doi: 10.12122/j.issn.1674-4500.2019.04.17 -







 下载:
下载: