Application of ultrasound guided percutaneous transluminal angioplasty on arteriovenous fistula stenosis in hemodialysis patients
-
摘要:
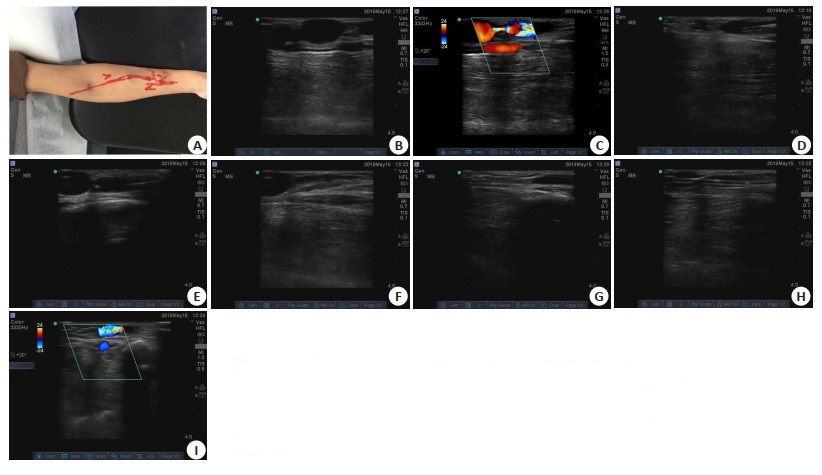
目的 探讨维持血液透析患者自体动静脉内瘘狭窄行经皮腔内血管成形术的应用。 方法 对2018年1月~2019年12月在本院进行血液透析并发动静脉内瘘狭窄的40例患者的临床资料进行回顾性分析,所有患者均在术前采用超声评估血管,术中采用超声指导经皮腔内血管成形术治疗,统计手术技术成功率、临床成功率、并发症发生情况,比较手术前后患者的血流指标。 结果 介入超声可清晰显示狭窄部位,引导内瘘狭窄行球囊扩张手术进程。经皮腔内血管成形术后彩超显示40例患者血管狭窄及血栓消失,治疗技术成功率100%,临床成功率100%。仅2例患者出现穿刺点皮下轻度血肿,所有患者均无严重并发症发生。术后动静脉内瘘狭窄处内径、透析血流量、内瘘血流量均较术前明显增加(P < 0.05)。 结论 超声引导下内瘘狭窄行腔内血管成形术具有较高的成功率及开通率,可作为一种安全有效的引导方法,具有一定的临床应用价值。 Abstract:Objective To investigate the application of ultrasound guided percutaneous transluminal angioplasty on arteriovenous fistula stenosis in maintenance hemodialysis patients. Methods The clinical data of 40 maintenance hemodialysis patients with arteriovenous fistula stenosis in our hospital from January 2018 to December 2019 were retrospectively analyzed. All patients accepted blood vessels assessment by ultrasound before operation, and underwent percutaneous transluminal angioplasty under ultrasound intervention guidance during operation. The technical success rate, clinical success rate and occurrence of complications were recorded, and the blood flow parameters before and after operation were compared. Results Ultrasound could clearly display the stenosis location, and guide the process of balloon dilatation for arteriovenous fistula stenosis. After percutaneous transluminal angioplasty, the color ultrasound showed that the stenosis and thrombosis disappeared in 40 patients, and both the technical success rate and clinical success rate were 100%. Only 2 cases had mild subcutaneous hematoma at the puncture site, and no serious complications occurred in all patients. The vessel diamete, hemodialysis blood flow and internal fistula blood flow of patients after operation were significantly higher than those before operation (P < 0.05). Conclusion Ultrasound guided percutaneous transluminal angioplasty has high success rate and vascular patency rate for arteriovenous fistula stenosis. Ultrasound can be used as a safe and effective guidance method, and is of certain clinical application value. -
Key words:
- hemodialysis /
- ultrasound /
- arteriovenous fistula /
- stenosis /
- percutaneous transluminal angioplasty
-
表 1 手术前后患者血管内径、透析血流量、内瘘血流量比较
Table 1. Comparison of vessel diamete, hemodialysis blood flow and internal fistula blood flow of patients before and after operation (n=40, Mean±SD)
组别 血管内径(mm) 内瘘血流量(mL/min) 透析血流量(mL/min) 术前 1.98±0.47 335.7±186.9 142.5±49.7 术后 4.76±0.69* 694.5±201.6* 251.6±36.9* *P < 0.05 vs术前. -
[1] Zhang L, Wang F, Wang L, et al. Prevalence of chronic kidney disease in China: a cross-sectional survey[J]. Lancet, 2012, 379 (9818): 815-22. doi: 10.1016/S0140-6736(12)60033-6 [2] 王德光, 郝丽, 戴宏, 等. 安徽省成人慢性肾脏病流行病学调查[J]. 中华肾脏病杂志, 2012(2): 101-5. doi: 10.3760/cma.j.issn.1001-7097.2012.02.004 [3] 张路霞, 王海燕. 中国慢性肾脏病的现状及挑战: 来自中国慢性肾脏病流行病学调查的启示[J]. 中华内科杂志, 2012, 2(7): 497-8. doi: 10.3760/cma.j.issn.0578-1426.2012.07.001 [4] 党彦龙, 徐玉祥, 李江. 维持性血液透析患者血清TM、CD62P、PAF表达水平与血管通路功能的关系[J]. 海南医学, 2021, 32(17): 2193-6. doi: 10.3969/j.issn.1003-6350.2021.17.005 [5] 蒋雪峰, 柳亿, 罗文荣. 超声引导下经皮血管成形术治疗血透患者动静脉内瘘狭窄的临床效果研究[J]. 浙江创伤外科, 2021, 26(4): 748-9. doi: 10.3969/j.issn.1009-7147.2021.04.072 [6] Sadaghianloo N, Jean-Baptiste E, Gaid H, et al. Early surgical thrombectomy improves salvage of thrombosed vascular accesses [J]. J Vasc Surg, 2014, 59(5): 1377-84. e2. doi: 10.1016/j.jvs.2013.11.092 [7] Campos RP, Do Nascimento MM, Chula DC, et al. Stenosis in hemodialysis arteriovenous fistula: evaluation and treatment[J]. Hemodial Int, 2006, 10(2): 152-61. doi: 10.1111/j.1542-4758.2006.00087.x [8] Gray RJ, Sacks D, Martin LG, et al. Reporting standards for percutaneous interventions in dialysis access[J]. J Vasc Interv Radiol, 2003, 14(9 pt 2): S433-42. http://www.fertstert.org/article/S1051-0443(07)61261-5/pdf [9] Yang CC, Yang CW, Wen SC, et al. Comparisons of clinical outcomes for thrombectomy devices with different mechanisms in hemodialysis arteriovenous fistulas[J]. Catheter Cardiovasc Interv, 2012, 80(6): 1035-41. doi: 10.1002/ccd.24408 [10] 卢松芳, 陈靖, 马鹏跃, 等. 超声引导下二次经皮腔内血管成形术治疗动静脉内瘘术后再狭窄效果观察[J]. 山东医药, 2020, 60(20): 55-7. doi: 10.3969/j.issn.1002-266X.2020.20.014 [11] 周青溢, 徐玉祥, 王科峰. 经皮腔内血管成形术后自体动静脉内瘘再狭窄与钙磷代谢紊乱相关性研究[J]. 中国药物与临床, 2021, 21 (11): 1841-4. https://www.cnki.com.cn/Article/CJFDTOTAL-YWLC202111001.htm [12] 罗茜, 刘洪. 超声引导PTA在动静脉内瘘狭窄中的应用研究[J]. 影像研究与医学应用, 2020, 4(2): 23-5. https://www.cnki.com.cn/Article/CJFDTOTAL-YXYY202002012.htm [13] 马孝芬, 刘乃全, 高树熹, 等. 超声引导下经皮球囊扩张血管成形术治疗自体动静脉内瘘狭窄的自身对照研究[J]. 中国临床医学影像杂志, 2021, 32(8): 561-4. https://www.cnki.com.cn/Article/CJFDTOTAL-LYYX202108008.htm [14] 倪志玲, 黎晓辉, 刘琴, 等. 超声引导和DSA引导下经皮腔内血管成形术治疗血液透析动静脉内瘘狭窄的对比分析[J]. 临床医学工程, 2019, 26(6): 721-2. doi: 10.3969/j.issn.1674-4659.2019.06.0721 [15] 梁英级, 吴静, 赵星卫, 等. 超声引导下经皮腔内血管成形术治疗动静脉内瘘狭窄的临床价值研究[J]. 中国实用医药, 2020, 15(35): 21-3. https://www.cnki.com.cn/Article/CJFDTOTAL-ZSSA202035007.htm [16] Lok CE, Huber TS, Lee T, et al. KDOQI clinical practice guideline for vascular access: 2019 update[J]. Am J Kidney Dis, 2020, 75(4 suppl 2): S1-164. http://www.sciencedirect.com/science/article/pii/S0272638619311370 [17] 王蕊, 朱莉敏, 李静, 等. 超声引导下动静脉内瘘球囊扩张术在维持性血液透析动静脉内瘘血管狭窄中的应用[J]. 医学影像学杂志, 2020, 30(10): 1898-901. https://www.cnki.com.cn/Article/CJFDTOTAL-XYXZ202010043.htm [18] 李伟龙, 胡波, 黄德绪, 等. 经皮腔内血管成形术治疗动静脉内瘘狭窄的疗效及影响因素[J]. 肾脏病与透析肾移植杂志, 2019, 28(3): 219-23. doi: 10.3969/j.issn.1006-298X.2019.03.004 [19] 刘军, 王琪, 张丽. 个案管理护理在血透患者动静脉内瘘狭窄行球囊扩张治疗中的应用分析[J]. 血栓与止血学, 2018, 24(2): 340-2. doi: 10.3969/j.issn.1009-6213.2018.02.060 [20] Asif A, Lenz O, Merrill D, et al. Percutaneous management of perianastomotic Stenosis in arteriovenous fistulae: results of a prospective study[J]. Kidney Int, 2006, 69(10): 1904-9. doi: 10.1038/sj.ki.5000358 [21] Aktas A, Bozkurt A, Aktas B, et al. Percutaneous transluminal balloon angioplasty in Stenosis of native hemodialysis arteriovenous fistulas: technical success and analysis of factors affecting postprocedural fistula patency[J]. Diagn Interv Radiol, 2015, 21(2): 160-6. doi: 10.5152/dir.2014.14348 [22] 金其庄, 王玉柱, 叶朝阳, 等. 中国血液透析用血管通路专家共识(第2版[) J]. 中国血液净化, 2019, 18(6): 365-81. doi: 10.3969/j.issn.1671-4091.2019.06.001 [23] Bachleda P, Janeckova J, Xinopulos P, et al. New hybrid procedures in treating occluded arteriovenous hemodialysis grafts[J]. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub, 2016, 160(1): 149-52. doi: 10.5507/bp.2015.068 [24] 陈松, 李晓颖, 于黔, 等. 尿毒症血液透析患者动静脉内瘘狭窄超声引导下PTA术后的疗效观察[J]. 中国超声医学杂志, 2018, 34(4): 342-6. doi: 10.3969/j.issn.1002-0101.2018.04.019 [25] Wakabayashi M, Hanada S, Nakano H, et al. Ultrasound-guided endovascular treatment for vascular access malfunction: results in 4896 cases[J]. J VascAccess, 2013, 14(3): 225-30. http://www.onacademic.com/detail/journal_1000040338883010_aa8a.html [26] 陆明晰, 冯剑, 蒋欣欣, 等. 超声引导下经皮腔内血管成形术治疗血液透析患者动静脉内瘘狭窄[J]. 中华肾脏病杂志, 2012(1): 63-4. doi: 10.3760/cma.j.issn.1001-7097.2012.01.015 [27] Arif A. 介入肾脏病学[M]. 北京: 科学出版社, 2016: 22. [28] 刘远浩, 郝国军, 唐斌. 超声引导下经皮腔内血管成形术与内瘘切除重建术治疗血液透析通路狭窄的临床研究[J]. 中国中西医结合肾病杂志, 2020, 21(8): 723-4, 754. doi: 10.3969/j.issn.1009-587X.2020.08.020 [29] 吕仁华, 王涌, 陈莉, 等. 自体动静脉瘘狭窄超声分型对经皮腔内血管成形术短期疗效的预测价值[J]. 同济大学学报: 医学版, 2021, 42 (1): 57-61. https://www.cnki.com.cn/Article/CJFDTOTAL-TJIY202101011.htm [30] Aurshina A, Ascher E, Hingorani A, et al. A novel technique for duplex-guided office-based interventions for patients with acute arteriovenous fistula occlusion[J]. J Vasc Surg, 2018, 67(3): 857-9. doi: 10.1016/j.jvs.2017.07.135 [31] 张宏涛, 阎磊, 高素华, 等. 评估超声引导下经皮腔内血管成形术治疗透析患者动静脉内瘘效果的最佳时机[J]. 中华肾脏病杂志, 2016 (9): 698-9. doi: 10.3760/cma.j.issn.1001-7097.2016.09.010 -







 下载:
下载: