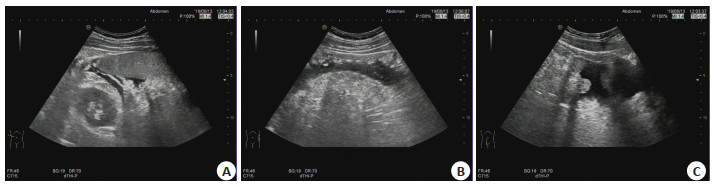
Application of ultrasound-guided percutaneous drainage catheterization for moderately severe acute pancreatitis
-
摘要:
目的 评估经皮穿刺置管引流在中度重症急性胰腺炎(MSAP)治疗中应用时机的选择对患者结局和并发症方面的影响。 方法 纳入2017年7月~2021年4月在广东省第二人民医院住院的113例MSAP患者,根据其是否行超声引导下经皮穿刺置管引流术(PCD)分为早期PCD组、晚期PCD组以及对照组,记录患者基本资料(年龄、性别、BMI、病因),比较3组临床结局(转为重症急性胰腺炎(SAP)患者人数、转外科手术患者人数、死亡患者人数)、实验室检查指标(白细胞计数、血清淀粉酶、C反应蛋白、血钙)、临床疗效时间指标(全身炎症反应时间、腹痛时间、肠鸣音恢复时间、饮食恢复时间和总住院时间)、不良事件(腹腔感染、腹腔内出血、导管堵塞)及并发症(胰腺假性囊肿、胰腺脓肿、腹腔间室综合征及多器官组织衰竭)。 结果 早期PCD组及晚期PCD组治疗成功率高于对照组,而死亡率、转为SAP患者率、外科手术率低于对照组,且早期PCD组治疗成功率高于晚期PCD组(P < 0.05);PCD组的全身炎症反应时间、肠鸣音恢复时间和住院时间少于对照组,且早期PCD组的全身炎症反应时间及住院时间明显少于晚期PCD组(P < 0.05);PCD组白细胞计数、血清淀粉酶、C反应蛋白和血钙的改善均优于对照组,且早期PCD组的血清淀粉酶及C反应蛋白的改善优于晚期PCD组(P < 0.05);PCD组并发症胰腺假性囊肿、胰腺脓肿、腹腔间室综合征及多器官组织衰竭明显低于对照组(P < 0.05),且早期PCD组的腹腔间室综合征及多器官组织衰竭明显低于晚期PCD组,3组腹腔感染及出血差异无统计学意义。 结论 对MSAP患者来说,晚期等待积聚物形成包裹后再进行PCD并不会产生任何额外的好处。早期PCD治疗可有效提高MSAP患者治疗成功率,减少住院时间及并发症。 Abstract:Objective To evaluate the impact of the timing of percutaneous catheterization and drainage in the treatment of moderately severe acute pancreatitis (MSAP) on patient outcomes and complications. Methods A total of 113 patients with MSAP who were hospitalized in the Second People's Hospital of Guangdong Province from July 2017 to April 2021 were enrolled. According to whether they underwent ultrasound-guided percutaneous catheter drainage (PCD), they were divided into early PCD group, late PCD group and control group, and the basic data of the patients were recorded (age, gender, BMI, etiology), compared the three groups of clinical outcomes (number of patients converted to severe acute pancreatitis, number of patients converted to surgery, number of patients who died), laboratory test indicators (white blood cell count, serum amylase, CRP and blood calcium), clinical efficacy time indicators (systemic inflammatory response time, abdominal pain time, bowel sound recovery time, diet recovery time and total hospital stay), adverse events (abdominal infection, intra-abdominal hemorrhage, catheter blockage) and complications Symptoms (pancreatic pseudocyst, pancreatic abscess, abdominal compartment syndrome, and multiple organ tissue failure). Results The treatment success rate of the early PCD group and the late PCD group was significantly higher than that of the control group, while the mortality, the rate of severe acute pancreatitis patients, and the surgical operation rate were significantly lower than those of the control group, and the treatment success rate of the early PCD group was significantly higher than that of the late PCD group (P < 0.05); The systemic inflammatory response time, bowel sound recovery time and hospital stay in the PCD group were less than those in the control group, and the systemic inflammatory response time and hospital stay in the early PCD group were significantly less than those in the late PCD group (P < 0.05); The improvement of white blood cell count, serum amylase, CRP and blood calcium in the PCD group was better than that of the control group, and the improvement of serum amylase and CRP in the early PCD group was better than that in the late PCD group (P < 0.05); PCD The complications of pancreatic pseudocyst, pancreatic abscess, abdominal compartment syndrome and multiple organ tissue failure in the control group were significantly less than those in the control group (P < 0.05), and the early PCD group had significantly less abdominal compartment syndrome and multiple organ tissue failure In the advanced PCD group, there was no significant difference in abdominal infection and bleeding among the three groups. Conclusion For patients with MSAP, waiting for the buildup to form a package at a later stage before proceeding with PCD does not produce any additional benefits. Early PCD treatment can effectively improve the success rate of MSAP patients, reduce hospitalization time and complications. -
表 1 患者临床结局比较
Table 1. Comparison of clinical outcomes [n(%)]
组别 转外科手术率 转SAP患者率 死亡率 成功率 早期PCD(n=38) 3(7.89)a 3(7.89)a 1(2.63)a 31(81.58)ab 晚期PCD(n=35) 3(8.57)a 8(22.86) 5(14.29) 19(54.29)a 对照组(n=40) 13(32.50) 13(32.50) 8(20.00) 6(15.00) χ2/Fisher 10.898 7.132 - 35.009 P 0.004 0.028 0.045 < 0.001 aP < 0.05 vs对照组; bP < 0.05 vs晚期PCD组; SAP: 重症急性胰腺炎; PCD: 经皮穿刺置管引流. 表 2 患者临床疗效时间指标比较
Table 2. Comparison of clinical efficacy time indicators (d, Mean±SD)
组别 全身炎症反应时间 腹痛时间 肠鸣音恢复时间 饮食恢复时间 住院时间 早期PCD(n=38) 8.86±1.26ab 5.81±0.98 3.42±0.86a 2.25±0.56 25.82±1.52ab 晚期PCD(n=35) 9.93±1.31a 5.92±1.47 3.59±0.99a 2.43±0.66 31.08±1.66a 对照组(n=40) 10.94±0.86 6.35±1.40 5.81±0.77 2.51±0.60 38.13±2.45 F 31.516 1.857 90.194 1.906 397.060 P < 0.001 0.161 < 0.001 0.154 < 0.001 aP < 0.05 vs对照组; bP < 0.05 vs晚期PCD组. 表 3 患者主要并发症比较
Table 3. Comparison of the main complications of the three groups [n(%)]
组别 胰腺假性囊肿 胰腺脓肿 腹腔间室综合征 多器官组织衰竭 早期PCD(n=38) 2(5.26)a 1(2.63)a 3(7.89)ab 2(5.26)ab 晚期PCD(n=35) 2(5.71)a 1(2.86)a 11(31.43)a 9(25.71)a 对照组(n=40) 12(30.00) 9(22.50) 24(60.00) 22(55.00) χ2 12.786 fisher 11.484 23.615 P 0.002 0.004 0.003 < 0.001 aP < 0.05 vs对照组; bP < 0.05 vs晚期PCD组. 表 4 3组不良事件比较
Table 4. Comparison of adverse events in the three groups [n(%)]
组别 腹腔感染 腹腔内出血 引流管堵塞 早期PCD(n=38) 3(7.89) 3(7.89) 3(7.89) 晚期PCD(n=35) 3(8.57) 3(8.57) 4(11.42) 对照组(n=40) 4(10.00) 5(12.50) 0(0.00) χ2/Fisher - - 0.000 P 1.000 0.789 1.000 -
[1] 黄荣柏, 胡锡琮. 重症急性胰腺炎手术时机选择的发展与演变[J]. 中国普通外科杂志, 2006, 15(6): 460-3. doi: 10.3969/j.issn.1005-6947.2006.06.017 [2] Majdoub A, Bahloul M, Ouaz M, et al. Severe acute biliary pancreatitis requiring Intensive Care Unit admission: Evaluation of severity score for the prediction of morbidity and mortality[J]. Int J Crit Illn Inj Sci, 2016, 6(3): 155-6. doi: 10.4103/2229-5151.190653 [3] Peery AF, Dellon ES, Lund J, et al. Burden of gastrointestinal disease in the United States: 2012 update[J]. Gastroenterology, 2012, 143 (5): 1179-87. e3. doi: 10.1053/j.gastro.2012.08.002 [4] 中华医学会消化病学分会胰腺疾病学组, 《中华胰腺病杂志》编委会, 《中华消化杂志》编委会. 中国急性胰腺炎诊治指南(2019年, 沈阳) [J]. 临床肝胆病杂志, 2019, 35(12): 2706-11. https://www.cnki.com.cn/Article/CJFDTOTAL-LCGD201912016.htm [5] 胡元佳, 张厚德, 肖鹏, 等. 中度急性胰腺炎的异质性分析[J]. 胃肠病学和肝病学杂志, 2017, 26(7): 754-7. doi: 10.3969/j.issn.1006-5709.2017.07.010 [6] 殷涛, 王春友. 再谈坏死性胰腺炎手术干预方式和时机的个体化[J]. 中华外科杂志, 2019, 57(10): 721-4. doi: 10.3760/cma.j.issn.0529-5815.2019.10.001 [7] Zerem E, Imamović G, Sušić A, et al. Step- up approach to infected necrotising pancreatitis: a 20-year experience of percutaneous drainage in a single centre[J]. Dig Liver Dis, 2011, 43(6): 478-83. doi: 10.1016/j.dld.2011.02.020 [8] Vege SS, Gardner TB, Chari ST, et al. Low mortality and high morbidity in severe acute pancreatitis without organ failure: a case for revising the Atlanta classification to include "moderately severe acute pancreatitis"[J]. Am J Gastroenterol, 2009, 104(3): 710-5. http://europepmc.org/abstract/med/19262525 [9] Zerem E, Imamovic G, Omerović S, et al. Randomized controlled trial on sterile fluid collections management in acute pancreatitis: should they be removed?[J]. Surg Endosc, 2009, 23(12): 2770-7. doi: 10.1007/s00464-009-0487-2 [10] van Baal MC, van Santvoort HC, Bollen TL, et al. Systematic review of percutaneous catheter drainage as primary treatment for necrotizing pancreatitis[J]. Br J Surg, 2011, 98(1): 18-27. http://www.onacademic.com/detail/journal_1000033782894910_3531.html [11] Mortelé KJ, Girshman J, Szejnfeld D, et al. CT-guided percutaneous catheter drainage of acute necrotizing pancreatitis: clinical experience and observations in patients with sterile and infected necrosis[J]. AJR Am J Roentgenol, 2009, 192(1): 110-6. doi: 10.2214/AJR.08.1116 [12] Solanki R, Thumma V. The role of image guided percutaneous drainage in multidisciplinary management of necrotizing pancreatitis[J]. Trop Gastrology, 2013, 34(1): 25-30. doi: 10.7869/tg.2012.87 [13] Bank JS, Adler DG. Endoscopic Ultrasound- Guided Drainage of Pancreatic Fluid CollectionsInterv Endosc Ultrasound, 2019. DOI: 10.1007/978-3-319-97376-0_1. [14] Cui ML, Kim KH, Kim HG, et al. Incidence, risk factors and clinical course of pancreatic fluid collections in acute pancreatitis[J]. Dig Dis Sci, 2014, 59(5): 1055-62. doi: 10.1007/s10620-013-2967-4 [15] Mouli VP, Sreenivas V, Garg PK. Efficacy of conservative treatment, without necrosectomy, for infected pancreatic necrosis: a systematic review and meta-analysis[J]. Gastroenterology, 2013, 144(2): 333-40. e2. doi: 10.1053/j.gastro.2012.10.004 [16] 刘航, 黄卫, 冯予希, 等. 经皮穿刺置管引流在重症急性胰腺炎治疗中应用时机的选择对患者预后影响[J]. 中华内分泌外科杂志, 2020, 14(3): 199-203. doi: 10.3760/cma.j.issn.115807-20190815-00164 [17] Arvanitakis M, Delhaye M, Bali MA, et al. Pancreatic- fluid collections: a randomized controlled trial regarding stent removal after endoscopic transmural drainage[J]. Gastrointest Endosc, 2007, 65(4): 609-19. doi: 10.1016/j.gie.2006.06.083 [18] Bellam BL, Samanta J, Gupta P, et al. Predictors of outcome of percutaneous catheter drainage in patients with acute pancreatitis having acute fluid collection and development of a predictive model[J]. Pancreatology, 2019, 19(5): 658-64. doi: 10.1016/j.pan.2019.05.467 [19] Isaji S, Takada T, Mayumi T, et al. Revised Japanese guidelines for the management of acute pancreatitis 2015: revised concepts and updated points[J]. J Hepatobiliary Pancreat Sci, 2015, 22(6): 433-45. doi: 10.1002/jhbp.260 [20] Balthazar EJ, Ranson JH, Naidich DP, et al. Acute pancreatitis: prognostic value of CT[J]. Radiology, 1985, 156(3): 767-72. doi: 10.1148/radiology.156.3.4023241 [21] Navalho M, Pires F, Duarte A, et al. Percutaneous drainage of infected pancreatic fluid collections in critically ill patients: correlation with C-reactive protein values[J]. Clin Imaging, 2006, 30 (2): 114-9. doi: 10.1016/j.clinimag.2005.09.026 [22] 王玉柱, 张莉, 秦涛, 等. 重症急性胰腺炎的个体化诊治体会[J]. 中国普通外科杂志, 2011, 20(3): 312-3. https://www.cnki.com.cn/Article/CJFDTOTAL-ZPWZ201103036.htm [23] 李晓明, 于晶, 王丰艳. 重症急性胰腺炎伴明显腹腔积液腹腔穿刺引流的最佳时间窗及预后[J]. 临床与病理杂志, 2021, 41(7): 1535-40. https://www.cnki.com.cn/Article/CJFDTOTAL-WYSB202107015.htm [24] 苏江林, 黄竹, 孙红玉, 等. 腹腔引流穿刺时机对重症急性胰腺炎患者预后的影响[J]. 中华肝胆外科杂志, 2018, 24(10): 692-7. doi: 10.3760/cma.j.issn.1007-8118.2018.10.009 [25] Trikudanathan G, Wolbrink DRJ, van Santvoort HC, et al. Current concepts in severe acute and necrotizing pancreatitis: an evidence-based approach[J]. Gastroenterology, 2019, 156(7): 1994-2007. e3. doi: 10.1053/j.gastro.2019.01.269 [26] Garg PK, Madan K, Pande GK, et al. Association of extent and infection of pancreatic necrosis with organ failure and death in acute necrotizing pancreatitis[J]. Clin Gastroenterol Hepatol, 2005, 3(2): 159-66. doi: 10.1016/S1542-3565(04)00665-2 [27] 安宏达, 孙备. 重症急性胰腺炎救治的难点与困惑[J]. 中华胰腺病杂志, 2020, 20(5): 325-7. doi: 10.3760/cma.j.cn115667-20200721-00115 -







 下载:
下载: