Efficacy of different cut-off values of Kaiser score in MRI diagnosis of breast lesions
-
摘要:
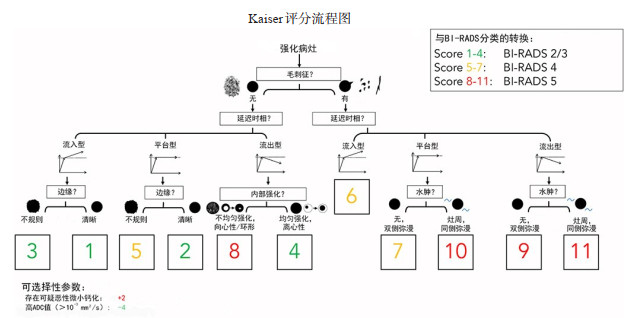
目的 研究诊断决策支持工具Kaiser评分系统中不同评分界值应用于乳腺病变MRI诊断中的效能,探索良恶性病变最佳参考评分界值从而避免过度的乳腺活检,并与传统的BI-RADS分类诊断标准进行诊断效能的比较。 方法 回顾并分析来自92例患者共101个术前行乳腺1.5 T MRI检查并被手术或穿刺病理证实的病灶的临床资料,由2位中级职称的影像科医生对所有病例独立根据Kaiser评分系统给出评分,探讨Kaiser评分系统应用于乳腺病变MRI中的诊断效能并与传统的BI-RADS分类诊断进行诊断效能比较,统计Kaiser评分在不同临界值下的敏感度、特异性和似然比,并分析2位阅片者之间的Kaiser评分一致性。 结果 92例患者共101个病灶,病理证实其中恶性病灶34个(33.66%),良性病灶67个(66.34%);应用Kaiser评分系统的曲线下面积值为0.969,BI-RADS分类的曲线下面积值为0.702,两种诊断方法的诊断效能差异有统计学意义(P < 0.01),分别使用临界值≥4、≥5、≥6做为良恶性病变的分界值,可以准确识别100.00%、100.00%、91.98%的恶性病变,特异度分别为79.10%、80.60%、88.06%,以高截断值≥7分作为判断良恶性病变的参考界值,可以正确识别79.41%的恶性病变,特异性为98.51%,阳性似然比为53.21。2位阅片者之间的Kaiser评分一致性良好(Kappa值=0.89,P < 0.01)。 结论 在乳腺病变MRI诊断中应用Kaiser评分对提高诊断准确性有益,同时以≥5为判断良恶性病变的诊断界值,可以获得最佳的综合诊断效能,针对特定诊断目标,在Kaiser评分中合理运用高诊断界值,可最大程度地避免过度乳腺活检。 Abstract:Objective To explore the efficacy of different cut-off values in Kaiser scoring system as diagnostic decision support tool in MRI diagnosis of breast lesions, and explore the best reference cut-off value of benign and malignant lesions so as to avoid excessive breast biopsy, and compare the diagnostic efficiency with the traditional BI-RADS classification diagnostic criteria. Methods The imaging data of 101 breast lesions from 92 patients examined by 1.5 T MRI before operation and confirmed by operation or puncture pathology were reviewed and analyzed. Two intermediate radiologist independently scored all cases according to Kaiser score system, to explore the diagnostic efficacy of Kaiser score system in MRI of breast lesions and compare it with traditional BI-RADS classification diagnosis. The sensitivity, specificity and likelihood ratio of Kaiser score under different critical values were calculated, and the consistency of Kaiser score between the two readers was analyzed. Results There were 101 lesions from 92 patients, including 34 malignant lesions (33.66%) and 67 benign lesions (66.34%). The AUC value of Kaiser score system was 0.969 and that of BI-RADS classification was 0.702. There was a significant difference between two diagnostic methods (P < 0.01). Using the critical value ≥4, ≥5 and ≥6 as the cut-off value of benign and malignant lesions, we could accurately identify 100.00%, 100.00% and 91.98% malignant lesions, and the specificity is 79.10%, 80.60% and 88.06%. Taking the high cut-off value of 7 as the reference cut-off value for judging benign and malignant lesions, we could correctly identify 79.41% of malignant lesions, with a specificity of 98.51% and a positive likelihood ratio of 53.21. The Kaiser scores of the two readers were consistent (Kappa=0.89, P < 0.01). Conclusion The application of Kaiser score in MRI diagnosis of breast lesions is beneficial to improve the diagnostic accuracy, taking ≥5 as the diagnostic threshold for judging benign and malignant lesions. The best comprehensive diagnostic efficiency could be obtained, and for specific diagnostic objectives, the reasonable use of high diagnostic threshold in Kaiser score could enhance diagnostic confidence and avoid excessive breast biopsy to the greatest extent. -
Key words:
- magnetic resonance imaging /
- malignant lesions of the breast /
- Kaiser score /
- BI-RADS
-
图 2 女,74岁,检查发现右乳肿物1周
A: T2WI-STIR; B: T1WI; C: MRI-DCE; D: MRI-DCE; E: TIC; F: 病理(HE染色, 10×40); 右侧乳腺内上、外上象限及中央区小叶节段强化, 增强扫描早期时相病灶缓慢强化, 延迟时相时间-信号曲线呈平台型; 病灶内部强化不均匀, 可见串环样强化, 右乳乳晕皮肤可见增厚, 并见较明显强化, Kaiser评分7分; 术后病理示: 高级别导管原位癌伴粉刺状坏死, 累及多个导管及乳腺小叶, 可见多灶浸润.
Figure 2. Female, 74 years old, examination revealed a right breast mass for a week.
表 1 Kaiser评分对乳腺良、恶性病变的诊断结果
Table 1. Kaiser score in the diagnosis of benign and malignant breast lesions (n)
Kaiser评分(分) 病理结果 合计 良性 恶性 1 25 0 25 2 11 0 11 3 17 0 17 4 1 0 1 5 5 3 8 6 7 4 11 7 0 6 6 8 0 6 6 9 0 7 7 10 1 5 6 11 0 3 3 总计 67 34 101 表 2 乳腺病变病理学诊断结果
Table 2. Pathological diagnosis of breast lesions [n(%)]
组别 病灶数 恶性 浸润性导管癌 28(27.72) 导管原位癌 5(4.95) 浸润性小叶癌 1(0.99) 良性 纤维腺瘤、纤维腺瘤样增生 25(24.75) 腺病 21(20.79) 炎性病变 12(11.88) 导管内乳头状瘤 6(5.94) 良性上皮增生 2(1.98) 良性叶状肿瘤 1(0.99) 表 3 在乳腺病变MRI中应用Kaiser评分不同截断值的诊断参数
Table 3. Diagnostic parameters of different cut-off values of Kaiser score in MRI of breast lesions (%)
评分界值(分) 诊断参数 敏感度 特异性 阳性似然比 阴性似然比 ≥1 100.00 0.00 1.00 - ≥2 100.00 37.31 1.60 0.00 ≥3 100.00 53.73 2.16 0.00 ≥4 100.00 79.10 4.79 0.00 ≥5 100.00 80.60 5.15 0.00 ≥6 91.18 88.06 7.64 0.10 ≥7 79.41 98.51 53.21 0.21 ≥8 61.76 98.51 41.38 0.39 ≥9 44.12 98.51 29.56 0.57 ≥10 23.53 98.51 15.76 0.78 ≥11 8.82 100.00 - 0.91 -
[1] Bennani-Baiti B, Baltzer PA. MR imaging for diagnosis of malignancy in mammographic microcalcifications: a systematic review and meta-analysis[J]. Radiology, 2017, 283(3): 692-701. doi: 10.1148/radiol.2016161106 [2] Bennani-Baiti B, Bennani-Baiti N, Baltzer PA. Diagnostic performance of breast magnetic resonance imaging in non-calcified equivocal breast findings: results from a systematic review and meta-analysis[J]. PLoS One, 2016, 11(8): e0160346. doi: 10.1371/journal.pone.0160346 [3] Houssami N, Ciatto S, Macaskill P, et al. Accuracy and surgical impact of magnetic resonance imaging in breast cancer staging: systematic review and meta- analysis in detection of multifocal and multicentric cancer[J]. J Clin Oncol, 2008, 26(19): 3248-58. doi: 10.1200/JCO.2007.15.2108 [4] Pinker K, Helbich TH, Morris EA. The potential of multiparametric MRI of the breast[J]. Br J Radiol, 2017, 90(1069): 20160715. doi: 10.1259/bjr.20160715 [5] Dietzel M, Baltzer PAT. How to use the Kaiser score as a clinical decision rule for diagnosis in multiparametric breast MRI: a pictorial essay[J]. Insights Imaging, 2018, 9(3): 325-35. doi: 10.1007/s13244-018-0611-8 [6] Jajodia A, Sindhwani G, Pasricha S, et al. Application of the Kaiser score to increase diagnostic accuracy in equivocal lesions on diagnostic mammograms referred for MR mammography[J]. Eur J Radiol, 2021, 134: 109413. doi: 10.1016/j.ejrad.2020.109413 [7] Zhang B, Feng LL, Wang L, et al. Kaiser score for diagnosis of breast lesions presenting as non-mass enhancement on MRI[J]. Nan Fang Yi Ke Da Xue Xue Bao, 2020, 40(4): 562-6. http://www.researchgate.net/publication/344203378_Kaiser_score_for_diagnosis_of_breast_lesions_presenting_as_non-mass_enhancement_on_MRI [8] Woitek R, Spick C, Schernthaner M, et al. A simple classification system (the Tree flowchart) for breast MRI can reduce the number of unnecessary biopsies in MRI-only lesions[J]. Eur Radiol, 2017, 27 (9): 3799-809. doi: 10.1007/s00330-017-4755-6 [9] Wengert GJ, Pipan F, Almohanna J, et al. Impact of the Kaiser score on clinical decision-making in BI-RADS 4 mammographic calcifications examined with breast MRI[J]. Eur Radiol, 2020, 30 (3): 1451-9. doi: 10.1007/s00330-019-06444-w [10] Milos RI, Pipan F, Kalovidouri A, et al. The Kaiser score reliably excludes malignancy in benign contrast-enhancing lesions classified as BI-RADS 4 on breast MRI high-risk screening exams[J]. Eur Radiol, 2020, 30(11): 6052-61. doi: 10.1007/s00330-020-06945-z [11] Marino MA, Clauser P, Woitek R, et al. A simple scoring system for breast MRI interpretation: does it compensate for reader experience?[J]. Eur Radiol, 2016, 26(8): 2529-37. doi: 10.1007/s00330-015-4075-7 [12] 张冰, 冯琳琳, 王琳, 等. Kaiser评分在乳腺非肿块强化病变诊断中的可行性研究[J]. 南方医科大学学报, 2020, 40(4): 562-6. https://www.cnki.com.cn/Article/CJFDTOTAL-DYJD202004019.htm [13] 安永玉, 刘畅, 张宏霞, 等. Kaiser评分对MRI乳腺影像报告与数据系统4类病灶的诊断价值[J]. 浙江医学, 2021, 43(5): 511-5. https://www.cnki.com.cn/Article/CJFDTOTAL-ZJYE202105013.htm [14] 陈园园, 张嫣, 王霞, 等. 肉芽肿性乳腺炎的MRI诊断[J]. 放射学实践, 2015, 30(2): 145-8. https://www.cnki.com.cn/Article/CJFDTOTAL-FSXS201502017.htm [15] 孟金丽, 初建国, 张丽娜, 等. 不同类型乳腺炎性疾病的MRI研究进展[J]. 临床放射学杂志, 2017, 36(11): 1726-9. https://www.cnki.com.cn/Article/CJFDTOTAL-LCFS201711049.htm [16] 张旭升, 郑晓林, 陈曌, 等. 小叶肉芽肿性乳腺炎MRI表现及与非肿块性乳腺癌鉴别[J]. 临床放射学杂志, 2013, 32(8): 1101-5. https://www.cnki.com.cn/Article/CJFDTOTAL-LCFS201308011.htm [17] Strigel RM, Rollenhagen J, Burnside ES, et al. Screening breast MRI outcomes in routine clinical practice: comparison to BI- RADS benchmarks[J]. Acad Radiol, 2017, 24(4): 411-7. doi: 10.1016/j.acra.2016.10.014 [18] Lee JM, Ichikawa L, Valencia E, et al. Performance benchmarks for screening breast MR imaging in community practice[J]. Radiology, 2017, 285(1): 44-52. doi: 10.1148/radiol.2017162033 [19] Grimm LJ, Anderson AL, Baker JA, et al. Interobserver variability between breast imagers using the fifth edition of the BI-RADS MRI lexicon[J]. Am J Roentgenol, 2015, 204(5): 1120-4. doi: 10.2214/AJR.14.13047 [20] El Khoury M, Lalonde L, David J, et al. Breast imaging reporting and data system (BI-RADS) lexicon for breast MRI: interobserver variability in the description and assignment of BI- RADS category[J]. Eur J Radiol, 2015, 84(1): 71-6. doi: 10.1016/j.ejrad.2014.10.003 [21] Stoutjesdijk MJ, Fütterer JJ, Boetes C, et al. Variability in the description of morphologic and contrast enhancement charac-teristics of breast lesions on magnetic resonance imaging[J]. Invest Radiol, 2005, 40(6): 355-62. doi: 10.1097/01.rli.0000163741.16718.3e [22] 孙笑芬, 邢伟, 俞胜男, 等. 对比增强能谱乳腺X线摄影量化评分对定性乳腺病灶的价值[J]. 临床放射学杂志, 2020, 39(9): 1738-42. https://www.cnki.com.cn/Article/CJFDTOTAL-LCFS202009015.htm -







 下载:
下载: