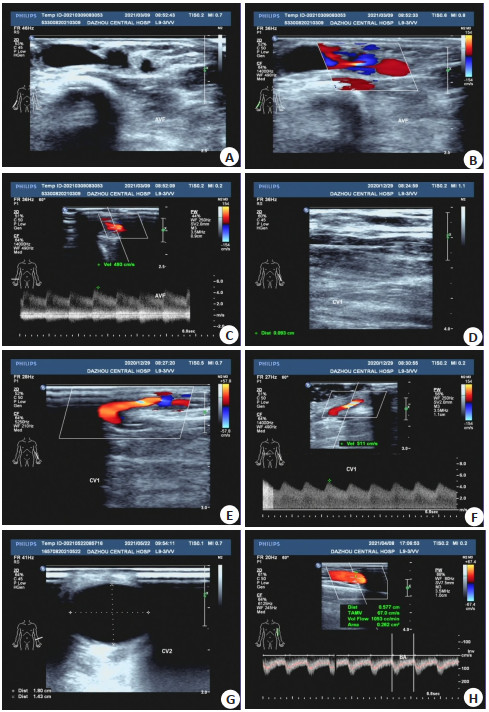
Ultrasonographic monitoring of hemodynamics in patients with arteriovenous fistula and the value of evaluating the maturity of internal fistula
-
摘要:
目的 分析彩色多普勒超声对评估动静脉内瘘(AVF)患者血流动力学和内瘘成熟程度的应用价值。 方法 回顾性选取2019年2月~2020年4月于本院首次进行动静脉内瘘手术的143例血液透析患者的临床资料。对所有患者行手术前后彩色多普勒超声检查,观察患者手术前后相关血流动力学指标及桡动脉和头静脉血流量、血管直径。术后6周,观察患者成熟情况并分析与头静脉血流动力学的关系。 结果 术后1、3、6周,患者的收缩期峰值流速、舒张期峰值流速均明显高于术前(P < 0.05),阻力指数明显低于术前(P < 0.05),桡动脉和头静脉的血流量和血管直径均明显大于术前(P < 0.05);且术后1、3、6周患者的收缩期峰值流速、舒张期峰值流速及桡动脉和头静脉的血流量、血管直径比较,差异无统计学意义(P>0.05),阻力指数在术后1、3、6相邻时间点均有统计学意义(P < 0.05);术后6周,143例患者AVF成熟度为69.23%(99/143),成熟组头静脉收缩期峰值流速、舒张期峰值流速、血管直径和血流量均明显大于未成熟组(P < 0.05),阻力指数明显小于未成熟组(P < 0.05);术后6周头静脉血流量预测AVF成熟的ROC曲线显示,ROC曲线下面积为0.938,预测AVF成熟的临界值为387.98 mL/min。 结论 彩色多普勒超声可通过反应相关血流动力学参数评估动静脉内瘘患者的内瘘成熟程度。 Abstract:Objective To analyze the value of ultrasound in evaluating hemodynamics and maturity of internal arteriovenous fistula (AVF). Methods The clinical data of 143 hemodialysis patients who underwent the first operation of venous fistula in our hospital from February 2019 to April 2020 were selected retrospectively. All patients were examined by color Doppler ultrasound before and after operation, and the related hemodynamic indexes, blood flow and diameter of radial artery and cephalic vein were observed before and after operation. Six weeks after operation, the maturity of the patients was observed and the relationship between Internal fistula maturity and Cephalic vein hemodynamics was analyzed. Results At 1 week, 3 weeks and 6 weeks after operation, the peak systolic velocity and diastolic peak velocity were significantly higher than those before operation, while the RI was significantly lower than that before operation(P < 0.05). The blood flow and diameter of radial artery and cephalic vein were significantly larger than those before operation(P < 0.05). There was no significant difference in peak systolic velocity, diastolic peak velocity, blood flow and diameter of radial artery and cephalic vein at 1 week, 3 weeks and 6 weeks after operation. Six weeks after operation, the maturity of AVF was 69.23%, peak systolic velocity, diastolic peak velocity, diameter and blood flow of cephalic vein in mature group were significantly higher than those in immature group(P < 0.05). RI was significantly lower than that in immature group(P < 0.05). ROC curve for predicting AVF maturity at 6 weeks after operation showed that the area under ROC curve was 0.938, and the critical value for predicting AVF maturity was 387.98 mL/min. Conclusion Color Doppler ultrasound can be used to evaluate the maturity of internal arteriovenous fistula in patients with arteriovenous fistula. -
Key words:
- ultrasound /
- arteriovenous fistula /
- hemodynamics /
- maturity of internal fistula /
- evaluation value
-
表 1 143例患者手术前后血流动力学指标比较
Table 1. Comparison of hemodynamic indexes in 143 patients before and after operation(Mean±SD)
时间 PSV(cm/s) EDV(cm/s) RI值 术前 66.49±8.23 23.16±4.28 0.70±0.11 术后1周 138.15±13.26* 75.26±7.71* 0.51±0.13*# 术后3周 140.52±16.49* 77.39±7.09* 0.46±0.11*# 术后6周 142.73±11.05* 79.06±5.16* 0.36±0.08*# *P < 0.05 vs术前;#P < 0.05 vs组内相邻时间点;PSV收缩期峰值流速;EDV:舒张期峰值流速;RI:阻力指数. 表 2 143例患者手术前后桡动脉和头静脉血流量和血管直径比较
Table 2. Comparison of blood flow and diameter of radial artery and cephalic vein in 143 patients before and after operation(Mean±SD)
时间 桡动脉血流量(mL/min) 桡动脉血管直径(mm) 头静脉血流量(mL/min) 头静脉直径(mm) 术前 87.33±4.16 2.48±0.68 89.70±13.26 2.90±0.53 术后1周 759.16±65.46* 3.42±0.87* 159.19±10.33* 3.78±0.94* 术后3周 771.52±54.16* 3.54±0.96* 261.76±13.07* 3.97±0.85* 术后6周 783.63±69.17* 3.62±0.75* 264.11±14.42* 4.11±0.59* *P < 0.05 vs术前. 表 3 143例患者AVF成熟情况与头静脉血流动力学的关系
Table 3. Relationship between AVF maturity and Cephalic vein hemodynamics in 143 patients(Mean±SD)
组別 PSV(cm/s) EDV(cm/s) RI值 血管直径(mm) 血流量(mL/min) 成数组(n=99) 166.15±9.21 94.16±8.72 0.31±0.05 4.08±0.59 461.16±67.49 未成熟组(n=44) 91.41±8.78 40.03±9.82 0.43±0.08 2.97±0.64 303.46±58.19 t 45.424 32.940 10.904 10.115 13.000 P < 0.001 < 0.001 < 0.001 < 0.001 < 0.001 -
[1] Levin A. Improving global kidney health: international society of nephrology initiatives and the global kidney health atlas[J]. Ann Nutr Metab, 2018, 72(Suppl 2): 28-32. http://smartsearch.nstl.gov.cn/paper_detail.html?id=961a608b4ada31bab9e8754052d8edfc [2] 史井波, 梅峰. 慢性肾脏病导致心血管疾病相关机制进展[J]. 世界最新医学信息文摘, 2018, 18(68): 64-6. https://www.cnki.com.cn/Article/CJFDTOTAL-WMIA201868028.htm [3] Khan S, Rosner MH. Peritoneal dialysis for patients with end-stage renal disease and liver cirrhosis[J]. Perit Dial Int, 2018, 38(6): 397-401. doi: 10.3747/pdi.2018.00008 [4] 王慧, 孙秀丽, 吴红梅, 等. 新建立自体动静脉内瘘首次穿刺时间对内瘘预后影响的系统评价和Meta分析[J]. 中国血液净化, 2018, 17(2): 107-13. doi: 10.3969/j.issn.1671-4091.2018.02.008 [5] Robbin ML, Greene T, Allon M, et al. Prediction of arteriovenous fistula clinical maturation from postoperative ultrasound measurements: findings from the hemodialysis fistula maturation study[J]. J Am Soc Nephrol, 2018, 29(11): 2735-44. doi: 10.1681/ASN.2017111225 [6] 苑欣, 菅梅, 陈琼. 彩色多普勒超声在血液透析患者动静脉内瘘并发症防治中的价值[J]. 中国医学影像技术, 2018, 34(10): 1490-3. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYXX201810018.htm [7] Nauta L, Voorzaat BM, Rotmans JI, et al. Endovascular salvage of non-maturing autogenous arteriovenous fistulas by using angioplasty and competitive vein embolization[J]. J Vasc Access, 2020, 21(5): 615-22. doi: 10.1177/1129729819895185 [8] Chemla E, Velazquez CC, D'Abate F, et al. Arteriovenous fistula construction with the VasQTM external support device: a pilot study[J]. J Vasc Access, 2016, 17(3): 243-8. doi: 10.5301/jva.5000527 [9] 肖佳, 赵华, 刘书馨. 动静脉内瘘血流量对维持性血液透析患者心功能的影响[J]. 中国中西医结合肾病杂志, 2020, 21(5): 403-7. doi: 10.3969/j.issn.1009-587X.2020.05.007 [10] Kazemzadeh GH, Bazrafshan M, Kamyar MM, et al. Efficacy of using non-tunneled dialysis catheters during arteriovenous fistula till its maturation: a retrospective study[J]. Urol J, 2019, 16(6): 578- 80. http://www.ncbi.nlm.nih.gov/pubmed/31376144 [11] Bashar K, Conlon PJ, Kheirelseid EA, et al. Arteriovenous fistula in dialysis patients: Factors implicated in early and late AVF maturation failure[J]. Surgeon, 2016, 14(5): 294-300. doi: 10.1016/j.surge.2016.02.001 [12] 王勇, 李呈芹. 血管CT联合彩色多普勒超声检查不同成熟程度动静脉内瘘的价值[J]. 中国CT和MRI杂志, 2018, 16(10): 140-2. doi: 10.3969/j.issn.1672-5131.2018.10.045 [13] 朱一枫, 李晶晶, 张艺, 等. 两种超声标准评估动静脉内瘘成熟的效能[J]. 肾脏病与透析肾移植杂志, 2020, 29(1): 26-30. doi: 10.3969/j.issn.1006-298X.2020.01.005 [14] 贾洪波, 张先东, 王铁铮, 等. 彩色多普勒超声在诊断下肢深静脉血栓形成后继发性动静脉瘘形成中的临床价值[J]. 医学影像学杂志, 2020, 30(8): 1479-81. https://www.cnki.com.cn/Article/CJFDTOTAL-XYXZ202008043.htm [15] Venkatnarayanan R, Dogra PM, Bavdekar R, et al. Primary failure of autogenous arteriovenous fistula: critical analysis[J]. Indian J Nephrol, 2020, 30(6): 382-90. doi: 10.4103/ijn.IJN_214_19 [16] 朱军涛, 刘帝, 刘烨歆, 等. 单中心血液透析患者血管通路的现状及影响因素分析[J]. 中国血液净化, 2019, 18(7): 503-6. doi: 10.3969/j.issn.1671-4091.2019.07.010 [17] Tang WJ, Mat Saad AZ. Autogenous forearm loop arteriovenous fistula creation[J]. J Vasc Access, 2018, 19(2): 191-4. doi: 10.5301/jva.5000801 [18] 熊良伟, 张祥贵. 成熟自体动静脉内瘘失功的慢性危险因素研究[J]. 中国血液净化, 2018, 17(5): 329-34. doi: 10.3969/j.issn.1671-4091.2018.05.010 [19] Li SQ, Zhu ML, Suo ST, et al. Assessment of the hemodynamics of autogenous arteriovenous fistulas with 4D phase contrast-based flow quantification MRI in dialysis patients[J]. J Magn Reson Imaging, 2020, 51(4): 1272-80. doi: 10.1002/jmri.26936 [20] 赵楠, 姚磊, 张浩然, 等. 彩色多普勒超声对自体动静脉内瘘成型术血流动力学和内瘘成熟情况的临床价值[J]. 中国医学装备, 2018, 15 (3): 75-8. doi: 10.3969/J.ISSN.1672-8270.2018.03.020 [21] 李霞, 龚雄, 熊晓芬, 等. 不同血管的血流量对动静脉内瘘功能的评估价值[J]. 中国临床医生杂志, 2020, 48(2): 164-6. doi: 10.3969/j.issn.2095-8552.2020.02.013 -







 下载:
下载: