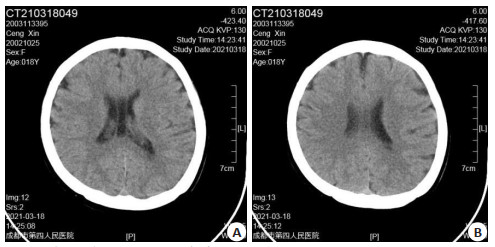
Relationship between the changes of head CT scan parameters and cognitive function abnormalities in patients with early-onset schizophrenia
-
摘要:
目的 探讨早发精神分裂症患者头颅CT扫描参数的变化与患者认知功能异常的关系。 方法 选取我院80例首发精神分裂症患者作为病例组,另选取年龄及性别等因素匹配的80例体检志愿者作为对照组,患者的诊断时间为2017年2月~2021年3月,两组研究对象均愿意接受头颅CT扫描,对比两组研究对象CT检查发现的脑结构异常、脑叶参数、认知功能评分,采用相关性分析法探讨脑结构异常、脑叶参数与患者认知功能的相关性。 结果 病例组的皮质型、髓质型、皮髓质混合型、脑萎缩总体发生率均显著高于对照组(P < 0.05);病例组的额叶平均CT值低于对照组(P < 0.05);两组在颞叶、顶叶、枕叶的CT值差异无统计学意义(P>0.05);病例组的信息处理速度、注意/警觉性、工作记忆、社会认知、总体认知得分上低于对照组(P < 0.05);两组词语记忆、视觉学习、推理与问题解决的得分差异无统计学意义(P>0.05);病例组脑萎缩患者的信息处理速度、注意/警觉性、工作记忆、社会认知、总体认知得分上低于未发生脑萎缩患者(P < 0.05);两组词语记忆、视觉学习、推理与问题解决的得分差异无统计学意义(P>0.05);病例组额叶CT值与信息处理速度、工作记忆、社会认知、总体认知得分呈正相关(P < 0.05)。 结论 早发精神分裂症患者头颅CT扫描可发现患者脑萎缩的检出率明显增加,额叶CT值降低,这些变化与患者认知功能受损存在密切关系。 Abstract:Objective To explore the relationship between the changes of head CT scan parameters and cognitive function abnormalities in patients with early-onset schizophrenia. Methods We selected 80 first-onset schizophrenia patients (case group), 80 physical examination volunteers (control group) with basically matched factors such as age and gender. The diagnosis time of the patients was February 2017 to March 2021. The patients acceptted head CT scans. We compared the brain structure abnormalities, brain lobe parameters, and cognitive function scores found in the CT examination of the two groups. The correlation analysis was used to explore the correlation between brain structure abnormalities, brain lobe parameters and patients' cognitive functions. Methods The overall incidence of cortical, medullary, mixed cortical and medullary, and brain atrophy in the case group were significantly higher than those in the control group (P < 0.05). The average CT value of the frontal lobe of the case group was lower than the control group (P < 0.05). Two groups had no significant difference in CT values in the temporal lobe, parietal lobe, and occipital lobe (P>0.05). The scores of attention/alertness, working memory, social cognition, and overall cognition were lower than those of the control group (P < 0.05). Two groups had scores on word memory, visual learning, reasoning and problem solving(P>0.05). The information processing speed, attention/alertness, working memory, social cognition, and overall cognition scores of patients with brain atrophy in the case group were lower than those without brain atrophy(P < 0.05). The two groups had no significant differences in the scores of word memory, visual learning, reasoning and problem solving (P>0.05). The frontal lobe CT value of the case group and the speed of information processing, working memory, social Cognition and overall cognition scores were positively correlated (P < 0.05). Conclusions CT scan of the brain of patients with early-onset schizophrenia can find that the detection rate of brain atrophy is significantly increased. CT value of the frontal lobe is decreased. These changes are closely related to the impaired cognitive function of the patient. -
Key words:
- first episode /
- schizophrenia /
- head CT scan /
- abnormal cognitive function
-
表 1 病例组和对照组的基线资料比较
Table 1. Baseline data comparison of the case and control groups[n=80, n(%)]
一般资料 病例组 对照组 t/x2 P 年龄(岁,Mean±SD) 37.6±8.2 39.0±7.7 -1.113 0.267 BM(kg/m2, Mean±SD) 24.1±2.5 23.8±2.1 0.822 0.412 性別 0.901 0.343 男 44(55.00) 38(47.50) 女 36(45.00) 42(52.50) 吸烟 0.795 0.373 是 19(23.75) 24(30.00) 否 61(76.25) 56(70.00) 饮酒 0.735 0.391 是 11(13.75) 15(18.75) 否 69(86.25) 65(81.25) 高血压 1.060 0.303 是 6(7.50) 3(3.75) 否 74(92.50) 77(96.25) 糖尿病 0.526 0.468 是 3(3.75) 5(6.25) 否 77(96.25) 75(93.75) 冠心病 2.025 0.155 是 2(2.50) 0(0) 否 78(97.50) 80(100.00) 文化程度 2.992 0.393 小学 11(13.75) 8(10.00) 初中 28(35.00) 25(31.25) 高中 34(42.50) 33(41.25) 大专及以上 7(8.75) 14(17.50) 表 2 病例组和对照组的脑萎缩检出率比较
Table 2. Comparison of brain atrophy detection rates in the case and control groups[n=80, n(%)]
组別 病例组 对照组 X2 P 皮质型 18(22.50) 0(0.00) 20.282 < 0.001 髓质型 11(13.75) 2(2.50) 6.782 0.009 皮、髓质混合型 16(20.00) 0(0.00) 17.778 < 0.001 小脑萎缩 3(3.75) 1(1.25) 1.026 0.311 脑萎缩 48(60.00) 3(3.75) 58.284 < 0.001 表 3 病例组和对照组的脑叶平均CT值比较
Table 3. Comparison of brain atrophy detection rates in the case and control groups [Hu, n=80, Mean±SD]
位置 病例组 对照组 t P 额叶 33.67±3.04 35.11±3.15 -2.942 0.004 颞叶 33.50±2.84 32.86±2.90 1.410 0.160 顶叶 33.56±3.72 34.21±3.60 -1.123 0.263 枕叶 33.70±3.54 33.48±3.40 0.401 0.689 表 4 病例组和对照组的认知功能评分比较
Table 4. Comparison of cognitive function scores in case and control groups (score, n=80, Mean±SD)
维度 病例组 对照组 t P 信息处理速度 47.66±4.40 57.28±5.37 -12.394 < 0.001 注意/警觉性 46.84±4.71 56.76±5.51 -12.240 < 0.001 工作记忆 47.03±5.20 57.74±6.18 -11.860 < 0.001 同语记忆 49.81±4.83 51.10±5.54 -1.570 0.118 视觉学习 49.74±5.54 51.64±5.72 -2.134 0.034 推理与问题解决 50.88±5.82 52.58±6.25 -1.780 0.077 社会认知 47.33±6.12 54.89±6.60 -7.513 < 0.001 认知总分 48.15±6.37 55.14±5.95 -7.173 < 0.001 表 5 发生脑萎缩与未发生脑萎缩患者的认知功能评分比较
Table 5. Comparison of cognitive function scores in patients with brain atrophy and no brain atrophy (score, Mean±SD)
维度 脑萎缩(n=48) 非脑萎缩(n=32) t P 信息处理速度 45.20±4.28 50.11±4.25 -5.041 < 0.001 注意/警觉性 45.11±4.55 48.93±4.63 -3.653 < 0.001 工作记忆 45.03±5.13 50.70±4.95 -4.911 < 0.001 词语记忆 49.50±4.64 50.20±4.70 -0.658 0.513 视觉学习 49.31±5.30 50.11±5.38 -0.657 0.513 推理与问题解决 50.46±5.68 51.36±5.64 -0.696 0.488 社会认知 45.46±5.71 50.70±6.08 -3.918 < 0.001 认知总分 46.32±6.11 51.70±5.86 -3.921 < 0.001 表 6 病例组额叶CT值与认知功能的相关性分析
Table 6. Correlation Analysis
维度 额叶CT值 r P 信息处理速度 0.616 < 0.001 注意/警觉性 0.288 0.071 工作记忆 0.463 0.001 词语记忆 0.116 0.336 视觉学习 0.128 0.318 推理与问题解决 0.064 0.594 社会认知 0.572 < 0.001 认知总分 0.559 < 0.001 -
[1] 黄昌华, 张全中. CT在偏执型首发精神分裂症患者中的应用及影像特点分析[J]. 武汉大学学报: 医学版, 2019, 40(4): 629-32. https://www.cnki.com.cn/Article/CJFDTOTAL-HBYK201904023.htm [2] 熊敏荣, 顾国强, 孙云峰, 等. 精神分裂症患者脑萎缩CT特点及危险因素分析[J]. 中国药物与临床, 2019, 19(15): 2569-71. https://www.cnki.com.cn/Article/CJFDTOTAL-YWLC201915025.htm [3] 闫旭, 罗锦秀, 徐勇, 等. 精神分裂症患者常见头颅CT表现及相关分析[J]. 中国药物与临床, 2014, 14(9): 1284-5. https://www.cnki.com.cn/Article/CJFDTOTAL-YWLC201409065.htm [4] 张全中, 鲁际, 林红, 等. 80例难治性精神分裂症的脑部CT分析与临床特征[J]. 国际精神病学杂志, 2017, 44(3): 443-5, 453. https://www.cnki.com.cn/Article/CJFDTOTAL-GWYJ201703019.htm [5] 于玲, 曾勇, 赵心灵, 等. 首发精神分裂症患者血清MIF、EGF水平与认知功能相关性[J]. 中华行为医学与脑科学杂志, 2018, 27(9): 793-7. doi: 10.3760/cma.j.issn.1674-6554.2018.09.005 [6] 王潇, 张燕, 孙梦夕, 等. 青少年精神分裂症首次发病患者脑灰质体积与认知功能的相关性[J]. 临床精神医学杂志, 2016, 26(6): 365-7. doi: 10.3969/j.issn.1005-3220.2016.06.002 [7] Mohammadzadeh A, Azadi S, King S, et al. Childhood trauma and the likelihood of increased suicidal risk in schizophrenia[J]. Psychiatry Res, 2019, 275: 100-7. doi: 10.1016/j.psychres.2019.03.023 [8] 美国精神医学学会编. 张道龙等译. 精神障碍诊断与统计手册[M]. 北京: 北京大学出版社, 2016: 12-13. [9] 唐光健, 秦乃姗. 现代全身CT诊断学[M]. 3版. 北京: 中国医药科技出版社, 2013: 11-12. [10] Kilicaslan EE, Esen AT, Kasal MI, et al. Childhood trauma, depression, and sleep quality and their association with psychotic symptoms and suicidality in schizophrenia[J]. Psychiatry Res, 2017, 258: 557-64. doi: 10.1016/j.psychres.2017.08.081 [11] Lo WA, Ki- Yan Mak D, Ming- Cheuk Wong M, et al. Achieving better outcomes for schizophrenia patients in Hong Kong: Strategies for improving treatment adherence[J]. CNS Neurosci Ther, 2021, 27(Suppl 1): 12-9. doi: 10.1111/cns.13375 [12] Zhao X, Tian L, Yan J, et al. Abnormal rich- club organization associated with compromised cognitive function in patients with schizophrenia and their unaffected parents[J]. Neurosci Bull, 2017, 33(4): 445-54. doi: 10.1007/s12264-017-0151-0 [13] Wu ZW, Shi H, Chen DC, et al. BDNF serum levels and cognitive improvement in drug- naive first episode patients with schizophrenia: a prospective 12- week longitudinal study[J]. Psychoneuroendocrinology, 2020, 122(5): 104879. http://www.sciencedirect.com/science/article/pii/S0306453020303024 [14] Kuperberg G, Heckers S. Schizophrenia and cognitive function[J]. Curr Opin Neurobiol, 2000, 10(2): 205-10. doi: 10.1016/S0959-4388(00)00068-4 [15] Habtewold TD, Rodijk LH, Liemburg EJ, et al. A systematic review and narrative synthesis of data- driven studies in schizophrenia symptoms and cognitive deficits[J]. Transl Psychiatry, 2020, 10(1): 244. doi: 10.1038/s41398-020-00919-x [16] Rizvi S, Khan AM, Saeed H, et al. Schizophrenia in DiGeorge syndrome: a unique case report[J]. Cureus, 2018, 10(8): 3142-3. http://www.onacademic.com/detail/journal_1000040895691810_2ec7.html [17] Chou PH, Huang CJ, Sun CW. The potential role of functional nearinfrared spectroscopy as clinical biomarkers in schizophrenia[J]. Curr Pharm Des, 2020, 26(2): 201-17. doi: 10.2174/1381612825666191014164511 [18] Picard H, Amado I, Mouchet- Mages S, et al. The role of the cerebellum in schizophrenia: an update of clinical, cognitive, and functional evidences[J]. Schizophr Bull, 2008, 34(1): 155-72. http://www.onacademic.com/detail/journal_1000037536880310_6b17.html [19] James A, Joyce E, Lunn D, et al. Abnormal frontostriatal connectivity in adolescent- onset schizophrenia and its relationship to cognitive functioning[J]. Eur Psychiatry, 2016, 35: 32-8. doi: 10.1016/j.eurpsy.2016.01.2426 [20] 张全中, 林红, 黄昌华. 80例难治性精神分裂症的脑部CT分析与临床特征[J]. 中国健康心理学杂志, 2018, 26(1): 3-5. https://www.cnki.com.cn/Article/CJFDTOTAL-JKXL201801002.htm [21] 袁传荣, 潘炳华, 汪爱妩. 精神分裂症患者脑部透明隔腔的CT表现特征[J]. 上海医药, 2019, 40(16): 26-7, 33. doi: 10.3969/j.issn.1006-1533.2019.16.008 [22] Zhang XY, Yang M, Du XD, et al. Glucose disturbances, cognitive deficits and white matter abnormalities in first- episode drug-naive schizophrenia[J]. Mol Psychiatry, 2020, 25(12): 3220-30. doi: 10.1038/s41380-019-0478-1 [23] 王海龙, 金洪民, 白明, 等. 社区精神分裂症患者康复期需求与患者家庭负担的关系[J]. 中国健康心理学杂志, 2016, 24(7): 969-72. https://www.cnki.com.cn/Article/CJFDTOTAL-JKXL201607004.htm -







 下载:
下载: