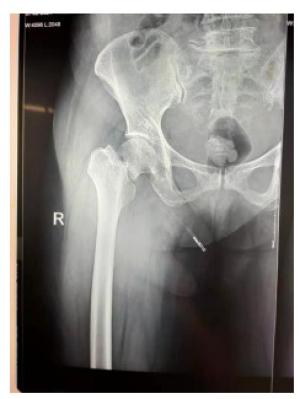
Risk factors for death within 1 year after surgery in elderly patients with hip fracture
-
摘要:
目的探讨高龄(≥80岁)老年髋部骨折患者术后1年内死亡的危险因素。 方法以2016~2019年204例经手术治疗的高龄髋部骨折患者作为研究对象,记录年龄、性别、术前合并疾病、骨折类型、麻醉方式、美国麻醉医师协会(ASA)评分、术前血红蛋白水平、术前白蛋白水平、术前血钙水平、住院时间等临床资料,以术后1年内死亡为观察结局。采用多因素logistic回归模型分析高龄老年髋部骨折患者术后1年内死亡的独立危险因素。 结果术后1年内,共有82例患者术后死亡,死亡率为40.2%。性别、BMI、骨折类型、麻醉方式、术前血红蛋白水平、术前血钙水平及住院时间不影响80岁患者髋关节术后死亡率,差异无统计学意义(P>0.05);年龄、术前合并疾病数量、ASA评分以及术前白蛋白水平是高龄老年髋部骨折患者术后1年内死亡的独立危险因素(P < 0.05)。 结论年龄、术前合并疾病数量、ASA评分、术前白蛋白水平是高龄老年髋部骨折患者术后1年内死亡的独立危险因素。 Abstract:ObjectiveTo explore the risk factors of death in elderly patients with hip fracture within 1 year after surgery. MethodsA total of 204 elderly hip fractures patients who underwent surgery treatment from 2016 to 2019 were selected. The clinical data were retrospectively collected, including age, gender, preoperative comorbidities, fracture type, anesthesia method, American Society of Anesthesiologists (ASA) score, preoperative hemoglobin, preoperative albumin, preoperative serum calcium, length of hospital stay were recorded, and death within 1 year after operation as the clinical outcome. Multivariate logistic regression model was used to analyze the independent risk factors of death within 1 year after surgery. ResultsA total of 82 patients died within 1 year after surgery, with a mortality rate of 40.2%. Gender, BMI, fracture type, anesthesia methods, preoperative hemoglobin, preoperative serum calcium and length of hospital stay did not affect the postoperative mortality of the hip in 80- year- old patients, and the difference was not significant (P>0.05). Age, number of preoperative complications, ASA score, and preoperative albumin were the independent risk factors for death within 1 year after surgery in elderly patients with hip fracture. ConclusionThe mortality rate of the elderly patients with hip fracture within 1 year after operation is relatively high. Age, preoperative comorbidities, ASA score, and preoperative albumin are the independent risk factors of 1-year mortality in elderly patients with hip fracture. -
Key words:
- advanced age /
- hip fracture /
- mortality /
- risk factors
-
表 1 高龄老年髋部骨折患者术后1年死亡危险因素的单因素分析结果
Table 1. Univariate analysis of risk factors for death in elderly patients with hip fracture at 1 year after operation (n=204)
因素 死亡率[n(%)] χ2 P 性别 1.387 0.239 男(n=72) 25 (34.7) 女(n=132) 57 (43.2) 年龄(岁) 11.096 0.001 < 85(n=111) 33 (29.7) ≥85(n=93) 49 (52.7) BMI(kg/m2) 0.078 0.779 < 24(n=127) 52 (40.9) ≥24(n=77) 30 (39.0) 医疗保险模式 1.070 0.301 城镇居民医保(n=145) 55 (37.9) 农村合作医疗(n=59) 27 (45.8) 合并疾病数量 5.012 0.025 ≤2种(n=140) 49 (35.0) >2种(n=64) 33 (51.6) 骨折类型 1.883 0.170 股骨颈骨折(n=104) 37 (35.6) 转子间骨折(n=100) 45 (45.0) ASA评分 11.508 0.001 Ⅰ~Ⅱ级(n=163) 56 (34.4) Ⅲ~Ⅳ级(n=41) 26 (63.4) 骨折至手术时间 2.154 0.142 ≤48 h(n=122) 44 (36.1) >48 h(n=82) 38 (46.3) 手术方式 0.812 0.367 内固定(n=155) 65 (41.9) 人工关节置换(n=49) 17 (34.7) 麻醉方式 0.114 0.735 全身麻醉(n=124) 51 (41.1) 局部麻醉(n=80) 31 (38.8) 血红蛋白(g/L) 1.076 0.300 < 120(n=133) 50 (37.6) ≥120(n=71) 32 (45.1) 白蛋白(g/L) 7.820 0.005 < 35(n=69) 37 (53.6) ≥35(n=135) 45 (33.3) 血钙(mmol/L) 3.595 0.058 < 2.25(n=55) 28 (50.9) ≥2.25(n=149) 54 (36.2) 住院时间(d) 1.912 0.167 < 10(n=66) 22 (33.3) ≥10(n=138) 60 (43.5) 表 2 高龄老年髋部骨折患者术后1年死亡危险因素的多因素分析结果
Table 2. Multivariate analysis of risk factors for death in elderly patients with hip fracture at 1 year after operation
变量 OR (95% CI) P 年龄(< 85岁vs ≥85岁) 1.686 (1.234~2.011) 0.005 术前合并疾病数量(≤2种vs >2种) 1.441 (1.130~1.744) 0.012 ASA评分(Ⅰ~Ⅱ级vs Ⅲ~Ⅳ级) 1.599 (1.227~1.988) 0.007 术前白蛋白(< 35 g/L vs ≥35 g/L) 0.800 (0.703~0.956) 0.041 -
[1] Wang K. Brief discussion on present status and future of joint replacement in China[J]. Chin J Joint Surg, 2015, 9: 12-4. [2] Dempsey KE, Ghazinouri R, Diez D, et al. Enhancing the quality of international orthopedic medical mission trips using the blue distinction criteria for knee and hip replacement centers[J]. BMC Musculoskelet Disord, 2013, 14: 275. doi: 10.1186/1471-2474-14-275 [3] Le Manach Y, Collins G, Bhandari M, et al. Outcomes after hip fracture surgery compared with elective total hip replacement[J]. JAMA, 2015, 314(11): 1159-66. doi: 10.1001/jama.2015.10842 [4] Jillian K, Kaushik B. Femoral Neck Fractures[M]. Treasure Island, StatPearls Publishing: 2021. [5] Fisher AA, Davis MW, Rubenach SE, et al. Outcomes for older patients with hip fractures: the impact of orthopedic and geriatric medicine cocare[J]. J Orthop Trauma, 2006, 20(3): 172-8. doi: 10.1097/01.bot.0000202220.88855.16 [6] Sexson SB, Lehner JT. Factors affecting hip fracture mortality[J]. J Orthop Trauma, 1987, 1(4): 298-305. doi: 10.1097/00005131-198701040-00005 [7] Chen JY, She GR, Luo SM, et al. Hemiarthroplasty compared with internal fixation for treatment of nondisplaced femoral neck fractures in elderly patients: a retrospective study[J]. Injury, 2020, 51(4): 1021-4. doi: 10.1016/j.injury.2020.02.098 [8] World Bank Group. World Development Indicators 2017[EB/OL].[2020-12-02]http://wdi.worldbank.org/tables. [9] Seong YJ, Shin WC, Moon NH, et al. Timing of hip-fracture surgery in elderly patients: literature review and recommendations[J]. Hip Pelvis, 2020, 32(1): 11-6. doi: 10.5371/hp.2020.32.1.11 [10] Gabriel RA, Waterman RS, Burton BN, et al. Patient health status and case complexity of outpatient surgeries at various facility types in the United States: an analysis using the National Anesthesia Clinical Outcomes Registry[J]. J Clin Anesth, 2021, 68: 110109. doi: 10.1016/j.jclinane.2020.110109 [11] Karademir G, Bilgin Y, Erşen AL, et al. Hip fractures in patients older than 75 years old: Retrospective analysis for prognostic factors[J]. Int J Surg, 2015, 24: 101-4. doi: 10.1016/j.ijsu.2015.11.009 [12] 李成宇, 张星晨, 郑欣, 等. 老年髋部骨折术后1年死亡率及死亡危险因素的分析[J]. 实用骨科杂志, 2017, 23(9): 802-6. https://www.cnki.com.cn/Article/CJFDTOTAL-SGKZ201709011.htm [13] 王培文, 李毅中, 林金矿, 等. 脆性髋部骨折的近期死亡率及相关危险因素研究[J]. 中华骨科杂志, 2014, 34(7): 730-5. doi: 10.3760/cma.j.issn.0253-2352.2014.07.006 [14] Boddaert J, Raux M, Khiami F, et al. Perioperative management of elderly patients with hip fracture[J]. Anesthesiology, 2014, 121(6): 1336-41. doi: 10.1097/ALN.0000000000000478 [15] 芮云峰, 鲁攀攀, 李荥娟, 等. 老年股骨转子间骨折患者术后死亡危险因素分析[J]. 中国修复重建外科杂志, 2019, 33(12): 1538-42. https://www.cnki.com.cn/Article/CJFDTOTAL-ZXCW201912014.htm [16] 许昊, 王培文. 老年骨质疏松患者髋部骨折发生及死亡危险因素分析[J]. 福建医药杂志, 2021, 43(1): 136-9. doi: 10.3969/j.issn.1002-2600.2021.01.050 [17] Bilsel K, Erdil M, Gulabi D, et al. Factors affecting mortality after hip fracture surgery: a retrospective analysis of 578 patients[J]. Eur J Orthop Surg Traumatol, 2013, 23(8): 895-900. doi: 10.1007/s00590-012-1104-y [18] 熊健斌, 彭伟秋, 孙宏志. 髋部骨折高龄患者术后死亡的相关因素回顾性分析[J]. 中国矫形外科杂志, 2014, 22(18): 1666-9. https://www.cnki.com.cn/Article/CJFDTOTAL-ZJXS201418012.htm [19] Radcliff TA, Henderson WG, Stoner TJ, et al. Patient risk factors, operative care, and outcomes among older community-dwelling male veterans with hip fracture[J]. J Bone Jo Surg Am Vol, 2008, 90 (1): 34-42. doi: 10.2106/JBJS.G.00065 [20] Schilling PL, Bozic KJ. Development and validation of perioperative risk-adjustment models for hip fracture repair, total hip arthroplasty, and total knee arthroplasty[J]. J Bone Jo Surg Am Vol, 2016, 98(1): e2. doi: 10.2106/JBJS.N.01330 [21] 李绍光, 刘智, 孙天胜, 等. 老年髋部骨折术后1年死亡率及危险因素分析[J]. 北京医学, 2015, 37(11): 1031-5. https://www.cnki.com.cn/Article/CJFDTOTAL-BJYX201511005.htm [22] 赵建文, 王晓伟, 孙天胜, 等. 老年髋部骨折术后1年死亡风险及危险因素分析[J]. 实用骨科杂志, 2020, 26(5): 399-403. https://www.cnki.com.cn/Article/CJFDTOTAL-SGKZ202005005.htm [23] Chung AS, Hustedt JW, Walker R, et al. Increasing severity of malnutrition is associated with poorer 30-day outcomes in patients undergoing hip fracture surgery[J]. J Orthop Trauma, 2018, 32(4): 155-60. doi: 10.1097/BOT.0000000000001081 -






 下载:
下载: