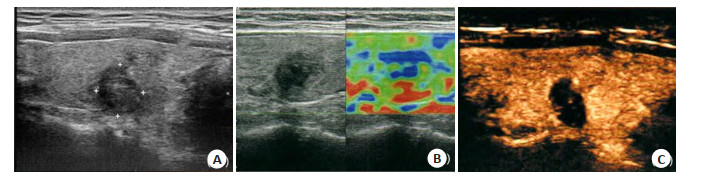
Application of contrast-enhanced ultrasound combined with elastography in blood perfusion analysis and benign and malignant evaluation of breast nodules
-
摘要:
目的探究超声造影和弹性成像在乳腺结节血流灌注分析及结节良恶性评估中的应用价值。 方法回顾性分析2017年1月~2020年6月在本院收治的102例乳腺结节患者的临床资料,所有患者均接受病理、常规超声、超声造影及超声弹性成像检查,根据病理检查 结果将患者分为良性组和恶性组。分析不同良恶性程度乳腺结节的血流灌注情况,比较超声造影和弹性成像对良恶性乳腺结节的诊断效能。 结果102例乳腺结节患者,经手术病理检查共检出良性结节69例(良性组),恶性结节33例(恶性组),恶性组的结节最大径大于良性组(P < 0.05)。恶性组的峰值强度(PI)明显小于良性组(P < 0.05),两组患者的达峰时间(TP)和平均度越时间(MTT)差异无统计学意义(P>0.05);恶性组组中,不同区域的PI比较,结节旁组织>结节边缘>结节中心(P < 0.05),不同区域的TP和MTT差异无统计学意义(P>0.05);良性组中,不同区域的PI、TP和MTT差异均无统计学意义(P>0.05)。恶性组的0~2分比例明显低于良性组,3~4分比例明显高于良性组(P < 0.05)。超声造影诊断良恶性乳腺结节的敏感度、特异性和准确率分别为83.78%、84.62%和84.31%;超声弹性成像诊断良恶性乳腺结节的敏感度、特异性和准确率分别为74.42%、89.83%和83.33%;联合诊断的敏感度、特异性和准确率分别为91.43%、94.03%和93.14%,且联合诊断的准确率均高于超声造影和超声弹性成像(P < 0.05)。 结论超声造影和弹性成像在诊断乳腺结节中具有良好的应用价值,超声造影定量参数的差异可在一定程度上反映结节的微血管分布特征,超声造影联合弹性成像可提高良恶性乳腺结节的诊断准确率。 Abstract:ObjectiveTo explore the application value of contrast-enhanced ultrasound combined with elastography in blood perfusion analysis and benign and malignant evaluation of breast nodules. MethodsThe study retrospectively analyzed clinical data of 102 patients with breast nodules treated in the hospital between January 2017 and June 2020. All patients were subjected to pathological examination, conventional ultrasound, contrast- enhanced ultrasound and ultrasound elastography. According to the pathological results, patients were divided into benign group and malignant group. Blood perfusion of the two groups was compared, and the diagnostic efficiencies of contrast-enhanced ultrasound and elastography for benign and malignant breast nodules were analyzed. ResultsIn the 102 patients with breast nodules, 69 cases with benign nodules (benign group) and 33 cases with malignant nodules (malignant group) were detected by surgical pathology. The maximum diameter of nodules in the malignant group was larger than that in the benign group (P < 0.05). The peak intensity (PI) of the malignant group was significantly lower than that of the benign group (P < 0.05), but no significant differences were found in time to peak (TP) and mean transit time (MTT) (P>0.05). In the malignant group, comparison of PI in different regions showed tissue around the nodule >nodule margin > nodule center (P < 0.05), but no significant differences were found in TP and MTT in different regions (P>0.05). In the benign group, no significant differences were found in PI, TP and MTT in different regions (P> 0.05). The ratio of 0-2 points was significantly lower and the ratio of 3-4 points was significantly higher in the malignant group than in the benign group (P < 0.05). The sensitivity, specificity and accuracy of contrast- enhanced ultrasound in diagnosing benign and malignant breast nodules were 83.78%, 84.62% and 84.31%, which of ultrasound elastography were 74.42%, 89.83 and 83.33%. The sensitivity, specificity and accuracy of combined diagnosis were 91.43%, 94.03%, and 93.14%, respectively. The accuracy of combined diagnosis was higher than that of contrast-enhanced ultrasound or ultrasound elastography alone (P < 0.05). ConclusionBoth contrast-enhanced ultrasound and ultrasound elastography can be used to diagnose breast nodules. The differences in quantitative parameters of contrast-enhanced ultrasound can reflect microvessel distribution characteristics of the nodule to a certain extent. Contrast-enhanced ultrasound combined with elastography can improve the diagnostic accuracy for benign and malignant breast nodules -
表 1 不同良恶性结节超声造影定量参数比较
Table 1. Comparison of contrast-enhanced ultrasound quantitative parameters between benign and malignant nodules (Mean±SD)
组别 PI(%) TP(s) MTT(s) 恶性组(n=33) 18.63±5.41 31.67±8.33 48.62±12.38 良性组(n=69) 22.46±6.84 30.52±7.94 50.21±11.76 t 3.064 0.662 0.617 P 0.003 0.510 0.539 表 2 不同区域超声造影定量参数比较
Table 2. Comparison of contrast-enhanced ultrasound quantitative parameters between different regions (Mean±SD)
区域 恶性组(n=33) 良性组(n=69) PI(%) TP(s) MTT(s) PI(%) TP(s) MTT(s) 结节中心 14.27±4.16*# 30.18±6.32 47.61±8.36 21.84±6.75 30.21±7.28 50.15±9.63 结节边缘 21.33±5.38* 29.33±7.06 48.22±9.13 20.93±5.57 31.18±6.43 49.38±9.17 结节旁组织 25.64±6.71 31.06±5.28 48.72±10.27 22.35±5.24 30.83±5.17 50.94±8.12 F 35.738 0.630 0.118 1.029 0.413 0.519 P < 0.001 0.535 0.889 0.359 0.663 0.593 *P < 0.05 vs结节旁组织; #P < 0.05 vs结节边缘. 表 3 不同良恶性结节的超声弹性评分比较
Table 3. Comparison of ultrasonic elastography scores between benign and malignant nodules [n (%)]
组别 0分 1分 2分 3分 4分 恶性组(n=33) 0(0.00) 3(9.09) 4(12.12) 15(45.45) 11(33.33) 良性组(n=69) 4(5.80) 18(26.09) 36(52.17) 7(10.14) 4(5.80) t 38.591 P < 0.001 表 4 超声造影、超声弹性成像检查与病理检查结果比较
Table 4. Comparison of the results of contrast- enhanced ultrasound, ultrasound elastography and pathological examination (n)
检查方法 病理结果 良性 恶性 超声造影 良性 31 10 恶性 6 55 超声弹性成像 良性 32 6 恶性 11 53 联合检测 良性 32 4 恶性 3 63 -
[1] 李阳, 赵松, 冀亮, 等. 超声引导下微波消融与传统开放手术治疗乳腺多发良性结节的比较[J]. 中国微创外科杂志, 2018, 18(10): 911-4, 919. doi: 10.3969/j.issn.1009-6604.2018.10.014 [2] Desai S, Aramin H, Gupta G, et al. Steatocystoma multiplex presenting as breast nodules: a case report and literature review[J]. Am J Clin Pathol, 2018, 150(1): S35. http://academic.oup.com/ajcp/article/150/suppl_1/S35/5103003 [3] Quan J, Hong YR, Zhang X, et al. The clinical role of contrast enhanced ultrasound in differential diagnosis of BI-RADS 4 breast disease[J]. Clin Hemorheol Microcirc, 2019, 72(3): 293-303. doi: 10.3233/CH-180495 [4] 王佳讯, 陈毓菁, 梁展鹏, 等. 超声造影结合细针穿刺活检诊断甲状腺结节[J]. 分子影像学杂志, 2017, 40(4): 397-400. doi: 10.3969/j.issn.1674-4500.2017.04.04 [5] 陈颖, 李红. 弹性超声成像技术与常规超声在乳腺结节诊断中的比较[J]. 中国地方病防治杂志, 2017, 32(3): 346, 348. https://www.cnki.com.cn/Article/CJFDTOTAL-DYBF201703064.htm [6] American College of Radiology. Breast imaging reporting and datasystem (BI-RADS)[M]. Reston: American College of Radiology, 2003. [7] 贾红飞, 牛宁宁, 张学娜. 超声弹性成像技术联合血清uPA检测对甲状腺结节良恶性鉴别诊断的价值分析[J]. 中华地方病学杂志, 2020, 39(7): 516-20. doi: 10.3760/cma.j.cn231583-20200320-00052 [8] Liu QH, Cheng J, Li JJ, et al. The diagnostic accuracy of contrastenhanced ultrasound for the differentiation of benign and malignant thyroid nodules: a PRISMA compliant meta-analysis[J]. Medicine, 2018, 97(49): e13325. doi: 10.1097/MD.0000000000013325 [9] 罗慧, 施杨, 肖晓君, 等. 超声弹性成像对伴后方回声衰减乳腺结节的鉴别诊断价值[J]. 中华超声影像学杂志, 2020, 29(8): 695-9. doi: 10.3760/cma.j.cn131148-20200227-00117 [10] 陈晓琴, 乔学研, 益磋, 等. 诊断超声激励微泡增强乳腺癌血流灌注的研究[J]. 临床超声医学杂志, 2018, 20(2): 82-5. doi: 10.3969/j.issn.1008-6978.2018.02.004 [11] Lehotska V, Rauova K, Vanovcanova L. Pitfalls of contrast enhanced ultrasound (CEUS) in determination of breast tumor biological dignity[J]. Neoplasma, 2018, 65(1): 124-31. doi: 10.4149/neo_2018_170116N43 [12] 张金堂, 黄品同, 骆洁丽. 超声造影与弹性成像联合评分法对TIRADS4类甲状腺结节良恶性的诊断价值[J]. 中华超声影像学杂志, 2017(8): 677-81. doi: 10.3760/cma.j.issn.1004-4477.2017.08.008 [13] Chen F, Liu J, Wan P, et al. Immunohistochemical index prediction of breast tumor based on multi-dimension features in contrastenhanced ultrasound[J]. Med Biol Eng Comput, 2020, 58(6): 1285- 95. doi: 10.1007/s11517-020-02164-2 [14] Zhao LX, Liu H, Wei Q, et al. Contrast-enhanced ultrasonography features of breast malignancies with different sizes: correlation with prognostic factors[J]. Biomed Res Int, 2015, 2015: 613831. http://pubmedcentralcanada.ca/pmcc/articles/PMC4735976/ [15] 吴昌财, 朱凌源, 陈文艳, 等. 超声造影定量分析对甲状腺实性结节血流灌注异质性的评价[J]. 中华医学杂志, 2015, 95(43): 3519-22. doi: 10.3760/cma.j.issn.0376-2491.2015.43.009 [16] Kapetas P, Clauser P, Woitek R, et al. Quantitative multiparametric breast ultrasound: application of contrast- enhanced ultrasound and elastography leads to an improved differentiation of benign and malignant lesions[J]. Investig Radiol, 2019, 54(5): 257-64. doi: 10.1097/RLI.0000000000000543 [17] Zhao J, Zhang J, Zhu QL, et al. The value of contrast- enhanced ultrasound for sentinel lymph node identification and characterisation in pre-operative breast cancer patients: a prospective study[J]. Eur Radiol, 2018, 28(4): 1654-61. doi: 10.1007/s00330-017-5089-0 [18] 刘文, 杨景桂, 刘仁来, 等. 弹性成像对超声引导乳腺肿块穿刺活检指导价值[J]. 分子影像学杂志, 2019, 42(2): 204-6. doi: 10.12122/j.issn.1674-4500.2019.02.14 [19] Zhao QL, Xia XN, Zhang Y, et al. Elastosonography and twodimensional ultrasonography in diagnosis of axillary lymph node metastasis in breast cancer[J]. Clin Radiol, 2018, 73(3): 312-8. doi: 10.1016/j.crad.2017.09.013 [20] 任艳, 刘晓晖. 超声弹性成像联合二维超声评分法对乳腺癌腋窝淋巴结转移状态的诊断价值[J]. 实用临床医药杂志, 2019, 23(2): 4-7. -






 下载:
下载: