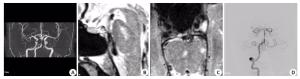
Contrast analysis of high resolution vascular wall magnetic resonance imaging and DSA in evaluating cerebral artery stenosis
-
摘要:
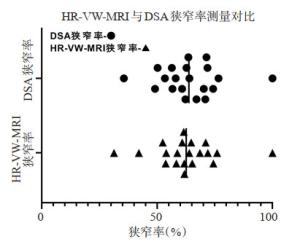
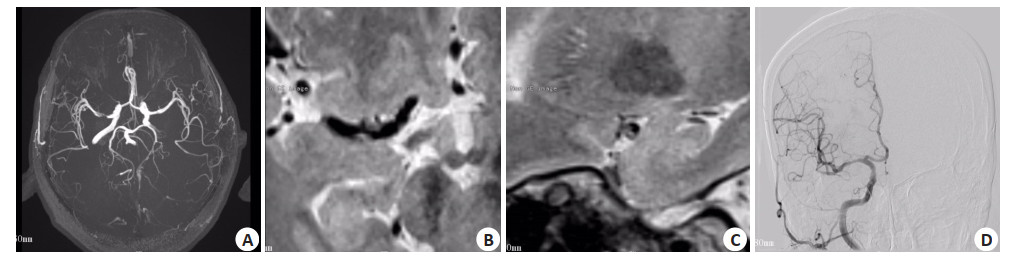
目的探讨高分辨率血管壁磁共振成像(HR-VW-MRI)评估脑血管狭窄与数字减影血管造影(DSA)金标准对照的临床诊断价值。 方法收集本院2016年1月~2019年12月入院25例近期发生缺血性脑病患者,行CT血管造影、磁共振血管成像检查证实存在脑血管狭窄,在1周内行DSA检查及HR-VW-MRI,分别测量、计算狭窄段脑动脉DSA与HR-VW-MRI狭窄率,对责任区血管进行高分辨率磁共振血管壁重建、T1WI增强,根据线性回归分析,Pearson相关性分析评价HR-VW-MRI测量脑血管狭窄率与DSA狭窄率的相关性,并探寻脑动脉狭窄原因。 结果25例患者共有20例完成HR-VW-MRI和DSA数据测量。HRVW-MRI狭窄率为62.66±13.79,DSA狭窄率为63.78±13.10,Pearson相关性分析显示两组检查方式呈正相关(P < 0.05),线性回归分析显示两组方式检查相关性良好(R2=0.880,P < 0.05),HR-VW-MRI发现脑动脉狭窄段责任斑块。 结论HR-VW-MRI检查在测量脑血管狭窄方面与DSA具有良好的相关性,因具有无创性,良好的组织结构分辨率,能通过三维角度更好的显示脑血管壁结构及管腔大小,分析病因,做出诊断,在替代DSA检查方面具有一定的优势。 -
关键词:
- 高分辨率血管壁磁共振成像 /
- 数字减影血管造影 /
- 脑动脉狭窄 /
- 斑块
Abstract:ObjectiveTo explore the clinical diagnostic value of HR-VW-MRI in evaluating cerebrovascular stenosis compared with DSA. MethodsA total of 25 patients with recent ischemic encephalopathy admitted to our hospital from January 2016 to December 2019 were collected and confirmed with CTA and MRA examinations. Within one week, DSA examination and HRVW-MRI were performed to measure and calculate the stenosis rates of DSA and HR-VW-MRI in the stenosis segment. Highresolution magnetic resonance vascular wall reconstruction and T1WI enhancement were performed on the vessels in the responsible area. Linear regression analysis and Pearson correlation analysis were used to evaluate the correlation between cerebral vascular stenosis rate measured by HR-VW-MRI and DSA stenosis rate, and to explore the causes of cerebral artery stenosis. ResultsA total of 20 of the 25 patients completed HR-VW-MRI and DSA data measurement. The mean stenosis rate of HR-VW-MRI was 62.66±13.79, and that of DSA was 63.78±13.10. According to Pearson correlation analysis (P < 0.05), there was positive correlation between the two groups. The linear regression analysis showed that the r-squared value was 0.880, and the P < 0.05, and the correlation between the two groups was good. HR-VW-MRI found the responsible plaque of cerebral artery stenosis. ConclusionHR-VW-MRI has a good correlation with DSA in the measurement of cerebrovascular stenosis. Because of its non-invasive and good resolution of tissue structure, it can better display the structure of cerebrovascular wall and the size of vascular cavity from a three-dimensional Angle, analyze the etiology and make diagnosis, which has certain advantages in replacing DSA. -
表 1 HR-VW-MRI狭窄率和DSA狭窄率相关性分析
Table 1. Correlation analysis between HR-VW-MRI stenosis rate and DSA stenosis rate
项目 HR-VW-MRI狭窄率 DSA狭窄率 Pearson相关 HR-VW-MRI狭窄率 1.000 0.938 DSA狭窄率 0.938 1.000 显著性(单尾) HR-VW-MRI狭窄率 0.000 DSA狭窄率 0.000 -
[1] 王伊龙.专题综述:动脉管壁成像的临床应用[J].中国卒中杂志, 2017, 12(6): 506. http://www.cnki.com.cn/article/cjfdtotal-zuzh201706009.htm [2] 段青顺. CTA、MRA与DSA诊断在脑血管狭窄疾病诊断中的应用[J].黑龙江医学, 2019, 43(3): 249-50. http://www.cnki.com.cn/Article/CJFDTotal-HLYX201903027.htm [3] 张丹凤, 陈慧铀, 张卫东, 等.高分辨率磁共振大脑中动脉粥样硬化斑块的分布及信号特点与脑梗死的关系[J].磁共振成像, 2017, 8 (1): 4-7. http://www.cnki.com.cn/Article/CJFDTotal-CGZC201701004.htm [4] Corrado S, Branden C, Andrew K, et al. Vessel wall magnetic resonance imaging in intracranial aneurysms: Principles and emerging clinical applications[J]. Interv Neuroradiol, 2019, 26(2): 159101991989129. http://www.researchgate.net/publication/337868092_Vessel_wall_magnetic_resonance_imaging_in_intracranial_aneurysms_Principles_and_emerging_clinical_applications [5] Lindenholz A, van der Schaaf IC, van der Kolk AG, et al. MRI vessel wall imaging after intra-arterial treatment for acute ischemic stroke [J].Am J Neuroradiol, 2020, 41(4): 624-31. https://pubmed.ncbi.nlm.nih.gov/32139427/ [6] Watase H, Shen M, Sui BB, et al. Differences in atheroma between caucasian and asian subjects with anterior stroke: a vessel wall MRI study[J]. Stroke Vasc Neurol, 2020, 8: 000370. https://svn.bmj.com/content/early/2020/08/13/svn-2020-000370 [7] Matouk CC, Cord BJ, Yeung J, et al. High-resolution vessel wall magnetic resonance imaging in intracranial aneurysms and brain arteriovenous malformations[J]. Top Magn Reson Imaging, 2016, 25 (2): 49-55. http://www.ncbi.nlm.nih.gov/pubmed/27049241 [8] 周斌, 孙祎, 曹烨, 等.三维血管壁MRI与DSA评价大脑中动脉粥样硬化性狭窄对比研究[J].介入放射学杂志, 2019, 28(11): 1024-8. http://d.old.wanfangdata.com.cn/Periodical_zhqkyszz201906011.aspx [9] Samuels OB, Joseph GJ, Lynn MJ, et al. A standardized method for measuring intracranial arterial stenosis[J]. Am J Neuroradiol, 2000, 21(4): 643-6. http://europepmc.org/abstract/MED/10782772 [10] Eiden S, Beck C, Venhoff N, et al. High-resolution contrastenhanced vessel wall imaging in patients with suspected cerebral vasculitis: Prospective comparison of whole-brain 3D T1 SPACE versus 2D T1 black blood MRI at 3 Tesla[J]. PloS one, 2019, 14(3): e0213514. http://www.ncbi.nlm.nih.gov/pubmed/30849127 [11] Saito A, Fujimura M, Endo H, et al. Diagnostic value of contrastenhanced magnetic resonance vessel wall imaging on the onset type of vertebral artery dissection[J]. Cerebrovasc dis, 2019, 48(3- 6): 124-31. https://www.ncbi.nlm.nih.gov/pubmed/31770765 [12] 石增强, 贾琳, 贾文霄, 等. HRMR-VWI在椎-基底动脉病变诊断中的应用价值[J].医学影像学杂志, 2020, 30(2): 173-7. http://www.cqvip.com/main/zcps.aspx?c=1&id=7101015958 [13] Kern KC, Liebeskind DS. Vessel wall imaging of cerebrovascular disorders[J]. Curr Treat Options Cardio Med, 2019, 21(11): 65. http://www.researchgate.net/publication/337246215_Vessel_Wall_Imaging_of_Cerebrovascular_Disorders [14] Mossa-Basha M, Alexander M, Gaddikeri S, et al. Vessel wall imaging for intracranial vascular disease evaluation[J]. J Neurointerv Surg, 2016, 8(11): 1154-9. http://jnis.bmj.com/content/8/11/1154 [15] Laviña B. Brain vascular imaging techniques[J]. Int J Mol Sci, 2016, 18(1): 70. http://diva-portal.org/smash/record.jsf?pid=diva2:1291597 [16] Zhao XH, Li R, Hippe DS, et al. Chinese Atherosclerosis Risk Evaluation (CARE Ⅱ) study: a novel cross-sectional, multicentre study of the prevalence of high-risk atherosclerotic carotid plaque in Chinese patients with ischaemic cerebrovascular events: design and rationale[J]. BMJ, 2017, 2(1): 15-20. http://pubmedcentralcanada.ca/pmcc/articles/PMC5435211/ [17] Hashimoto Y, Matsushige T, Shimonaga K, et al. Vessel wall imaging predicts the presence of atherosclerotic lesions in unruptured intracranial aneurysms[J]. World Neurosurg, 2019, 132: e775-e782. http://www.sciencedirect.com/science/article/pii/S1878875019321710 [18] Jia S, Zhang L, Ren LJ, et al. Joint intracranial and carotid vessel wall imaging in 5 minutes using compressed sensing accelerated DANTE-SPACE[J]. Eur Radiol, 2020, 30(1): 119-27. doi: 10.1007/s00330-019-06366-7 [19] Harteveld AA, Denswil NP, van Hecke W, et al. Ex vivo vessel wall thickness measurements of the human circle of Willis using 7T MRI [J].Atherosclerosis, 2018, 273: 106-14. http://europepmc.org/abstract/MED/29715587 [20] Zwartbol MHT, van der Kolk AG, Ghaznawi R, et al. Intracranial vessel wall lesions on 7T MRI (magnetic resonance imaging)[J]. Stroke, 2019, 50(1): 88-94. http://www.researchgate.net/publication/329757231_Intracranial_Vessel_Wall_Lesions_on_7T_MRI_Magnetic_Resonance_Imaging_Occurrence_and_Vascular_Risk_Factors_The_SMART-MR_Study [21] Yu YN, Liu MW, Villablanca JP, et al. Middle cerebral artery plaque hyperintensity on T2-weighted vessel wall imaging is associated with ischemic stroke[J]. AJNR Am J Neuroradiol, 2019, 40(11): 1886-92. http://www.ajnr.org/content/early/2019/10/17/ajnr.A6260 [22] Alexander MD, de Havenon A, Kim SE, et al. Assessment of quantitative methods for enhancement measurement on vessel wall magnetic resonance imaging evaluation of intracranial atherosclerosis[J]. Neuroradiology, 2019, 61(6): 643-50. doi: 10.1007/s00234-019-02167-3 [23] 张梁, 周志斌.高分辨率磁共振血管壁成像在颅内动脉粥样硬化性疾病中的应用[J].分子影像学杂志, 2020, 43(1): 45-8. doi: 10.12122/j.issn.1674-4500.2020.01.10 [24] 慧娟, 郭秀海.基于高分辨率磁共振的颅内动脉粥样硬化性狭窄的研究进展[J].中国脑血管病杂志, 2019, 16(11): 607-12. http://www.cqvip.com/QK/87378X/201911/7100324016.html [25] Kathuveetil A, Sylaja PN, Senthilvelan S, et al. Vessel wall thickening and enhancement in high-resolution intracranial vessel wall imaging: a predictor of future ischemic events in moyamoya disease[J].AJNRAm J Neuroradiol, 2020, 41(1): 100-5. https://www.ncbi.nlm.nih.gov/pubmed/31896569 -






 下载:
下载: