Value of DCE-MRI and DWI in predicting sentinel lymph node metastasis of breast cancer
-
摘要:
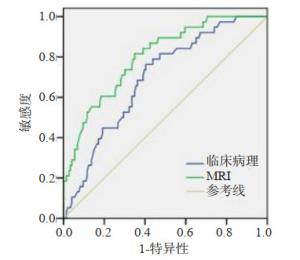
目的回顾性分析磁共振动态对比增强成像(DCE-MRI)及扩散加权成像(DWI)预测乳腺癌前哨淋巴结(SLN)转移的价值。 方法收集我院乳腺癌患者216例,包括SLN转移39例,无SLN转移177例。比较转移组、未转移组间影像特征及临床病理特征的差异,通过多元Logistic回归分析SLN转移的危险性因素,利用受试者工作曲线分析比较影像和临床病理特征对SLN的预测效能。 结果两组患者影像、临床病理特征比较,患者年龄、病灶大小、内部强化方式、瘤周/肿瘤表观扩散系数(ADC)比值具有统计学意义(P=0.003、0.001、0.020、0.001)。经Logistic回归分析,肿瘤大小、边缘增强和不均匀强化、瘤周/肿瘤ADC值比与SLN转移独立相关(OR=1.15, P < 0.001;OR=15.54, P=0.007;OR=5.24, P=0.006;OR=70.62, P < 0.001);临床病理资料中年龄、CD31与SLN转移独立相关(OR=0.96, P=0.012;OR=2.90, P=0.049)。MRI特征预测效能显著高于临床病理变量(P=0.048)。 结论术前DCE-MRI病灶大小、内部增强模式和瘤周/肿瘤ADC比可能有助于预测乳腺癌患者的SLN转移。 Abstract:ObjectiveTo retrospectively analyze the value of magnetic resonance dynamic contrast enhancement (DCE-MRI) and diffusion-weighted imaging (DWI) in predicting sentinel lymph node (SLN) metastasis in breast cancer. MethodsA total of 216 breast cancer patients in our hospital were collected, including 39 cases with SLN metastasis and 177 cases without SLN metastasis. The difference of image features and clinicopathological features were compared between metastatic and nonmetastatic groups. The risk factors of SLN metastasis were analyzed by multiple logistic regression. And by receiver operating characteristic (ROC), the predictive power of imaging and clinicopathological features were compared on SLN. ResultsThe imaging and clinicopathological characteristics of the two groups were statistically significant. The age, lesion size, internal enhancement method, and the ratio of peritumoral/tumor apparent diffusion coefficient (apparent diffusion coefficient, ADC) were statistically significant (P=0.003, 0.001, 0.020, 0.001). Logistic regression analysis showed that tumor size, edge enhancement and uneven enhancement, peritumoral/tumor ADC value ratio were independently related to SLN metastasis (OR= 1.15, P < 0.001; OR=15.54, P=0.007; OR=5.24, P=0.006; OR=70.62, P < 0.001); age, CD31 and SLN metastasis were independently related in the clinicopathological data (OR=0.96, P=0.012; OR=2.90, P=0.049). The predictive power of MRI features was significantly higher than clinicopathological variables (P=0.048). ConclusionThe preoperative DCE-MRI lesion size, internal enhancement pattern, and peritumoral/tumor ADC ratio may help predict SLN metastasis in breast cancer patients. -
表 1 SLN转移组与无SLN转移组临床病理变量比较(n)
Table 1. Comparison of clinicopathological variables between SLN metastasis group and non-SLN metastasis group
临床病理性质 转移(n=39) 无转移(n=177) P 年龄(岁, Mean±SD) 50.5.3±11.2 57.2±12.6 0.003 组织学分级 0.547 Ⅰ/Ⅱ 16 82 Ⅲ 23 95 脉管癌拴 0.213 有 12 38 无 27 139 雌激素受体 0.759 阳性 30 132 阴性 9 45 孕激素受体 0.158 阳性 24 129 阴性 15 48 HER-2表达 0.862 阳性 12 57 阴性 27 120 Ki-67表达 0.676 阳性 21 70 阴性 28 107 p53表达 0.946 阳性 6 28 阴性 33 149 CD31表达 0.023 阳性 17 45 阴性 22 132 分子亚型 0.087 Luminal A 14 65 Luminal B 13 78 HER-2阳性 7 16 三阴性 5 18 表 2 SLN转移组与无SLN转移组DCE-MRI及DWI影像特征比较(n)
Table 2. Comparison of the characteristics of DCE-MRI and DWI between SLN metastasis group and non-SLN metastasis group
影像特征 转移(n=39) 无转移(n=177) P 大小(mm, Mean±SD) 19.3±5.2 14.2±4.6 0.001 背景实质增强 0.687 轻中度 21 89 明显 18 88 内部增强 0.020 均匀 5 58 不均匀 30 111 边缘强化 4 8 相邻血管标记 0.749 有 15 73 无 24 104 全乳血管分布 0.256 无增多 20 116 轻度增多 13 41 显著增多 6 20 最初强化特征 0.751 快速 31 132 中等 7 37 慢速 1 8 增强曲线类型 0.465 流人型 4 23 平台型 14 78 流出遨 21 76 DWl (Mean±SD) 肿瘤ADC(10-3mm2/s) 0.942±0168 0.967±0.142 0.275 瘤周ADC (10-3mm2/s) 1.618±0.115 1.610±0.120 0.785 瘤周/肿瘤ADC 1.610±0.066 1.540±0.082 0.001 表 3 肿瘤影像及临床病理性质logistic回归分析
Table 3. Logistic regression analysis of tumor imaging and clinicopathological features
项目 单因素分析 多因素分析 OR值(95%CI) p OR值 p MRI 肿瘤大小 1.15(1.12, 1.16) < 0.001 1.15(1.09, 1.24) < 0.001 瘤周/肿瘤ADC 32.58 (4.86, 223.75) < 0.001 70.62 < 0.001 内部增强 0.028 0.006 均匀 1 1 不均匀 2.54 (0.98, 7.13) 0.048 5.24(1.56, 16.32) 0.006 边缘强化 9.08(1.48, 48.28) 0.012 15.54(2.12, 113.72) 0.007 临床病理 年龄 0.92 (0.86, 0.96) 0.002 0.96 (0.92, 0.99) 0.012 CD31 阳性 2.28 (0.97, 5.58) 0.058 2.90(1.04, 8.92) 0.049 阴性 1 1 -
[1] 苟军, 胥化虎, 杨桂松, 等. MRI在乳腺癌腋窝前哨淋巴结转移的诊断价值[J].放射学实践, 2018, 33(6): 574-8. http://www.cnki.com.cn/Article/CJFDTotal-FSXS201806009.htm [2] 李培, 陈嘉健, 吴炅.乳腺癌前哨淋巴结的研究热点与评价[J].中国癌症杂志, 2020, 30(3): 161-5. http://www.cnki.com.cn/Article/CJFDTotal-ZGAZ200505003.htm [3] 牛瑞洁, 韩宝三.乳腺癌前哨淋巴结的定位及诊断的影像研究进展[J].国际医学放射学杂志, 2016, 39(6): 637-40. http://www.cqvip.com/QK/92692X/201606/670787710.html [4] Mori N, Mugikura S, Takasawa C, et al. Peritumoral apparent diffusion coefficients for prediction of lymphovascular invasion in clinically node-negative invasive breast cancer[J]. Eur Radiol, 2016, 26(2): 331-9. doi: 10.1007/s00330-015-3847-4 [5] 谢运娟, 廖伶艺, 高强.弥散张量成像在脑卒中患者运动功能预后评估中的研究进展[J].中国康复理论与实践, 2019, 25(5): 546-9. http://www.cqvip.com/QK/98413X/20195/7002014536.html [6] 熊瑜琦, 蒋莉莉, 康宁. DWI与多普勒超声及CT对甲状腺癌颈部淋巴结转移癌的临床诊断效果分析[J].实用癌症杂志, 2018, 33(12): 1983-6. doi: 10.3969/j.issn.1001-5930.2018.12.020 [7] Morris EA, Comstock CE, Lee CH, et al. ACR BI-RADS magnetic resonance imaging//ACR BI-RADS atlas, breast imaging reporting and data system[M]. Reston: American College of Radiology, 2013. [8] Mennella S, Garlaschi A, Paparo F, et al. Magnetic resonance imaging of breast cancer: factors affecting the accuracy of preoperative lesion sizing[J].Acta Radiol, 2015, 56(3): 260-8. doi: 10.1177/0284185114524089 [9] Dong YH, Feng QJ, Yang W, et al. Preoperative prediction of sentinel lymph node metastasis in breast cancer based on radiomics of T2- weighted fat-suppression and diffusion-weighted MRI[J]. Eur Radiol, 2018, 28(2): 582-91. doi: 10.1007/s00330-017-5005-7 [10] Cululi B, Veiten M, Rodier JF, et al. Preoperative assessment of axillary lymph-node involvement in small breast cancers. Analysis of 893 cases[J]. Eur J Cancer, 1998, 34: S46. https://www.sciencedirect.com/science/article/pii/S1526820911703238 [11] 张晖, 单春辉, 王勇.磁共振动态对比增强及扩散加权成像技术在诊断和预估乳腺癌复发中的价值[J].磁共振成像, 2017, 8(11): 827-33. doi: 10.12015/issn.1674-8034.2017.11.006 [12] Chang YW, Kwon KH, Choi DL, et al. Magnetic resonance imaging of breast cancer and correlation with prognostic factors[J]. Acta Radiol, 2009, 50(9): 990-8. doi: 10.3109/02841850903225180 [13] van den Eynden GG, Colpaert CG, Couvelard A, et al. A fibrotic focus is a prognostic factor and a surrogate marker for hypoxia and (lymph)angiogenesis in breast cancer: review of the literature and proposal on the criteria of evaluation[J]. Histopathology, 2007, 51 (4): 440-51. doi: 10.1111/j.1365-2559.2007.02761.x [14] 杨红玲, 杨清.高频超声联合磁共振可提高对乳腺癌早期诊断的价值[J].分子影像学杂志, 2020, 43(3): 520-4. doi: 10.12122/j.issn.1674-4500.2020.03.32 [15] Gladwish A, Milosevic M, Fyles A, et al. Association of apparent diffusion coefficient with disease recurrence in patients with locally advanced cervical cancer treated with radical chemotherapy and radiation therapy[J]. Radiology, 2016, 279(1): 158-66. doi: 10.1148/radiol.2015150400 [16] Liu CL, Ding J, Spuhler K, et al. Preoperative prediction of sentinel lymph node metastasis in breast cancer by radiomic signatures from dynamic contrast-enhanced MRI[J]. J Magn Reson Imaging, 2019, 49(1): 131-40. doi: 10.1002/jmri.26224 [17] Capdet J, Martel P, Charitansky H, et al. Factors predicting the sentinel node metastases in T1 breast cancer tumor: an analysis of 1416 cases[J]. Eur J Surg Oncol, 2009, 35(12): 1245-9. doi: 10.1016/j.ejso.2009.06.002 [18] Lee JA, Bae JW, Woo SU, et al. D2-40, podoplanin, and CD31 as a prognostic predictor in invasive ductal carcinomas of the breast[J]. J Breast Cancer, 2011, 14(2): 104. doi: 10.4048/jbc.2011.14.2.104 [19] 苏春燕, 杨智, 付兵, 等.乳腺癌多模态MRI表现与前哨淋巴结是否转移的临床研究价值[J].实用放射学杂志, 2020, 36(4): 579-82. doi: 10.3969/j.issn.1002-1671.2020.04.018 -






 下载:
下载: