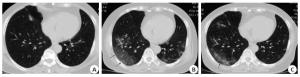
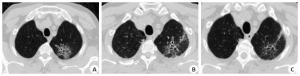
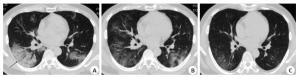
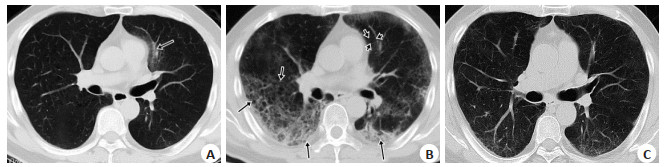
Chest CT findings of COVID-19 in different stages and the changes in lung lesions with positive for nucleic acid test after discharge
-
摘要:
目的探讨COVID-19在不同时期的胸部CT表现及出院后核酸复阳肺内病灶变化特点。 方法回顾性分析54例COVID-19患者的临床资料及影像学表现,通过3次以上胸部CT检查动态观察病灶变化,对比住院期间及出院后核酸检测复阳患者的胸部CT改变。 结果78%的病例近14 d去过武汉市或湖北省,22%的病例无去武汉市或湖北省史;普通型51例(94%),重型3例(6%);单叶单灶2例(3.7%),单叶多灶3例(5.6%),多叶多灶例49例(90.7%);沿胸膜下分布为主46例,沿血管束分布为主6例,沿肺叶分布2例;磨玻璃(GGO)54例,GGO伴局灶实变28例,GGO伴细网格征34例,GGO伴晕征23例,含气囊腔征3例,蜂窝征1例;血管束增粗14例,支气管增粗或扩张18例;1例伴双侧少量胸腔积液。早期表现单发或多发斑片磨玻璃灶;进展期病灶数量增多、范围增大、密度增高、局部实变或大片实变;重症期双肺多发或弥漫磨玻璃密度背景下节段或肺叶实变;转归期病灶缩小、密度不均匀减低,大部分病灶完全消失,少量形成纤维条索;6例(11.5%)在转归期出现“此消彼长”表现。47例(87%)在7~ 14 d病灶开始吸收,7例(13%)病灶开始吸收时间在14 d后。46例符合临床出院标准时,出院前胸部CT仍见多发磨玻璃病灶;9例出院后7~15 d出现核酸检测复阳,2例核酸复阳出现在15 d后,但其肺内病灶较上一次CT(出院前)吸收减少,未见新增病灶。 结论COVID-19不同时期影像学表现不同,其转归过程有一定的特征及规律,正确认识及掌握其影像学变化对其早期诊断、排查及疗效评估有重要价值。 Abstract:ObjectiveTo investigate the absorptive characteristics and the CT imaging features of COVID-19 in different stages and the changes in lung lesions with positive for nucleic acid test after discharge. MethodsThe CT imaging and clinical manifestations of 54 patients with COVID-19 were restrospectively analyzed. Through more than 3 times of chest CT examination to dynamically observe the changes of lesions, the changes of chest CT in patients with positive of nucleic acid test after discharge were compared with the last chest CT examination during hospitalization. Results42 patients (78%) come from Wuhan or Hubei to Huizhou in recent 14 days and 22% of the cases had no history of going to Wuhan or Hubei Province. Among them, 51 common type case (94%), 3 critical type case (6%) were divided by clinical symptoms and CT findings. Single lesion was located in the single pulmonary lobe in 2 cases; multiple lesions were located in the single pulmonary lobe in 3 cases; multiple lesions were located in the multiple pulmonary lobe in 49 cases; most lesions were located on the subpleural area in 46 cases; 6 cases were extended along the bronchovascular bundle; 2 cases were distributed along the pulmonary lobe. Ground glass opacities (GGO) were found in 54 patients; Consolidation was found in 28 cases; Interlobular septal thickening was appeared in GGO in 34 cases; Halo sign with GGO was found in 23 cases; Air sacs was occurred in the lesions of GGO or consolidation in 3 cases, and honeycomb sign was appeared in 1 case. Vascular bundle thickening in 14 cases, Bronchial thickening or dilatation in 18 cases, bilateral small amount of pleural effusion in 1 case. In early stage, patchy GGO was found on the subpleural area in 54 patients. In advanced stage, the number, density and range of lesions were more, denser and larger than those in the early stage. Segment or lobe consolidation in the background of diffuse or multiple ground glass opacities with double lungs in critical stage. In absorption stage, the lesions were significantly smaller and lighter in density, most of which disappeared, and a small amount of fibrosis were formed. The lesions in 47 cases began to be absorbed within 7-14 days, and the lesions in 7 cases began to be absorbed after 14 days. Positive for nucleic acid test occurred in 9 patients during 7-15 days after discharge, and 2 patients were occurred after 15 days, but the lesions were reduced compared with the previous CT (before discharge), and no new lesion was found. When 46 patients met the clinical discharge criteria, multiple ground glass lesions were still found on chest CT before discharge. ConclusionThe imaging manifestations of COVID-19 are different in different periods, and its evolution process has certain characteristics and rules. It is of great clinical value to correctly understand evolution process of COVID-19 for the early diagnosis, screening and efficacy evaluation. -
Key words:
- COVID-19 /
- different stages /
- chest CT findings /
- discharge /
- nucleic acid /
- positive
-
-
[1] 丁义, 黄增发, 赵胜超, 等.新型冠状病毒肺炎(COVID-19)临床及影像学特征分析[J].放射学实践, 2020, 35(3): 281-5. [2] 郑颖彦, 马昕, 王慧英, 等.新型冠状病毒肺炎的CT征象[J/OL].上海医学: 1-10[2020-04-29]. http://kns.cnki.net/kcms/detail/31.1366.r.20200209.1042.002.html. [3] 陈志勇, 程正银, 张旭辉, 等.新型冠状病毒肺炎的临床表现及CT影像学特点[J].放射学实践, 2020, 35(3): 286-90. [4] 李小虎, 王海涛, 朱娟, 等.输入性新型冠状病毒肺炎治愈患者肺内病变的影像学动态观察[J].中华放射学杂志, 2020, 54(5): 435-9. [5] 史河水, 韩小雨, 樊艳青, 等.新型冠状病毒(2019-nCoV)感染的肺炎临床特征及影像学表现[J/OL].临床放射学杂志, 2020. doi: 10.13437/j.cnki.jcr.20200206.002. [6] 刘发明, 丁惠玲, 龚晓明, 等.新型冠状病毒肺炎(COVID-19)的胸部CT表现与临床特点[J].放射学实践, 2020, 35(3): 266-8. [7] 赵双全, 周永生, 殷亮, 等. COVID-19的临床特征和CT表现[J].分子影像学杂志, 2020, 43(1): 59-63. doi: 10.12122/j.issn.1674-4500.2020.01.13 [8] 国家卫生健康委员会.新型冠状病毒肺炎诊疗方案(试行第七版修正版)[EB/OL].[2020-03-04]. http://www.nhc.gov.cn/yzygj/s7652m/202003/a31191442e29474b98bfed5579d5af95.shtml. [9] 中国研究型医院学会感染与炎症放射学专业委员会, 中国医师协会放射医师分会感染影像专业委员会, 中华医学会放射学分会传染病学组中国性病艾滋病防治协会感染(传染病)影像工作委员会, 等.新型冠状病毒肺炎影像诊断指南(2020年第二版简版) [J].首都医科大学学报, 2020, 41(2): 168-73. [10] 管汉雄, 熊颖, 申楠茜, 等.新型冠状病毒肺炎(COVID-19)临床影像学特征[J].放射学实践, 2020, 35(2):125-30. [11] 钟飞扬, 张寒菲, 王彬宸, 等.新型冠状病毒肺炎的CT影像学表现[J/OL].武汉大学学报: 医学版, 2020, 41(3): 345-8. [12] 刘长华, 余晓洁, 杨先春, 等.胸部CT特征预测普通型新型冠状病毒肺炎患者转归的价值[J].放射学实践, 2020, 35(5): 587-91. [13] 吕志彬, 关春爽, 闫铄, 等. CT在预测新型冠状病毒肺炎临床分型转变中的价值[J/OL].中华放射学杂志, 2020. doi: 10.3760/cma.j.issn.1005-1201.2020.0020. [14] Pan F, Ye T, Sun P, et al. Time course of lung changes on chest CT during recovery from 2019 novel coronavirus (COVID-19) pneumonia[J]. Radiology, 2020: 200370. [15] 柏玉涵, 杨健, 彭红芬, 等.初诊普通型新型冠状病毒肺炎的肺部高分辨率CT表现与动态观察[J/OL].实用医学杂志: 1-5[2020-05-07]. http://kns.cnki.net/kcms/detail/44.1193.r.20200414.1619.003.html. [16] 程庆红, 盛茂, 赵子健, 等. COVID-19患者胸部CT变化规律及转归[J].分子影像学杂志, 2020, 43(2): 274-7. doi: 10.12122/j.issn.1674-4500.2020.02.19 [17] 郭佑民, 陈欣, 牛刚.新型冠状病毒肺炎影像学诊断[M].西安:西安交通大学出版社, 2020. [18] Luo W, Yu H, Gou J, et al. Clinical Pathology of Critical Patient with Novel Coronavirus pneumonia (COVID-19)[J/OL]. Preprints, 2020. doi: 10.13140/RG.2.2.22934.29762 [19] 刘茜, 王荣帅, 屈国强, 等.新型冠状病毒肺炎死亡尸体系统解剖大体观察报告[J].法医学杂志, 2020, 36(2): 1-3. [20] Kong W, Agarwal PP. Chest Imaging Appearance of COVID-19 Infection[J]. Radiol Cardiothorac Imaging, 2020, 2(1): e200028. -






 下载:
下载: