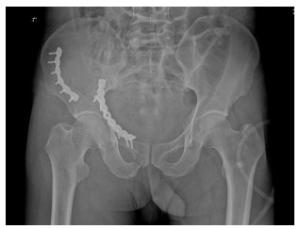
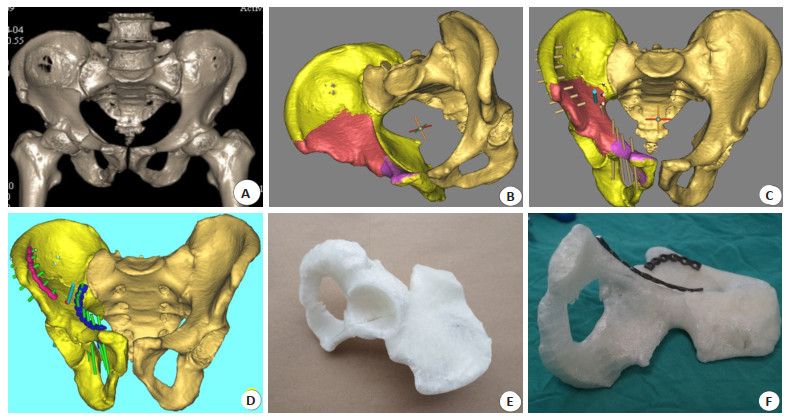
Comparation of the treatment of pelvic fractures with 3D printing and pararectus abdominis approach
-
摘要:
目的探讨腹直肌旁切口结合3D打印技术在骨盆骨折治疗中的应用效果。 方法回顾性研究收集由研究者于2013年9月~2015年6月主刀完成的骨盆骨折患者50例为研究对象。将患者分成对照组和观察组,对照组术前常规X线、CT三维重建检查采用腹直肌旁切口完成手术;观察组在X线、CT三维重建检查基础上采用3D打印技术术前模拟手术结合腹直肌旁切口完成手术。观察平均手术时间、术中失血量和平均切口长度。通过Matta和Majeed评分评估治疗效果,通过影像学方法评估内固定和术后骨盆骨折恢复情况。 结果采用3D打印技术术前模拟手术结合腹直肌旁切口治疗骨盆骨折,患者切口长度缩短,术中出血量减少,手术时间缩短(P < 0.05);用Matta标准评价骨折复位情况优良率96%。采用Majeed评分标准功能评定优良率为94%。术后影像评估内固定与术前模拟内固定基本一致。 结论采用3D打印技术术前模拟手术结合腹直肌旁切口结合治疗骨盆骨折具有创伤小、切口小、失血量低、术后疼痛轻、康复快、骨折复位满意度高。使患者早日重返工作岗位,提高康复效果,降低医疗成本,为社会节约了血源,值得广泛推广。 Abstract:ObjectiveTo determine the effect of pararectus abdominis approach combined with 3D printing in the treatment of pelvic fracture. MethodsFifty patients with pelvic fracture undergoing operation performed by the researchers from September 2013 to June 2015 were selected as the study objects. In the control group, routine X-ray, CT plain scan and threedimensional reconstruction were performed before operation; In the observation group, virtual fracture reduction, internal fixation design, simulated internal fixation and steel plate pre- bending were used on the basis of X-ray, CT plain scan and three-dimensional reconstruction. Then we used the steel plate and screw which had been pre bent and implanted into the body during the simulated internal fixation under the minimally invasive pararectus abdominis approach. Both groups were treated with the incision beside the replicator. The average operation time, intraoperative blood loss and incision length were observed. In both groups, pelvic fractures were treated by a pararectus abdominis approach. The average operation time, intraoperative blood loss and incision length were observed. The therapeutic effect was evaluated by Matta and majeed scores, and the recovery of internal fixation and postoperative pelvic fracture was evaluated by imaging methods. ResultsCompared with the group of pararectus abdominis approach, the length of incision was significantly shortened, the amount of bleeding was significantly reduced and the time of operation were significantly shortened (P < 0.05); The excellent rate of fracture reduction was 96% by the evaluation with Matta standard. The excellent rate of fracture reduction was 96% by the evaluation with Majeed standard. The postoperative image evaluation of internal fixation is basically the same as that of preoperative simulated internal fixation. ConclusionCompared with the traditional operation, the pararectus abdominis approach combined with 3D printing technology in the treatment of pelvic fracture has the advantages of small trauma, small incision, low blood loss, light postoperative pain, fast recovery and high satisfaction of fracture reduction. It can make the patients return to work as soon as possible, improve the rehabilitation effect, reduce the medical cost and save the blood source for the society, which is worth popularizing widely. -
Key words:
- 3D printing /
- pararectus abdominis approach /
- pelvic fracture /
- internal fixation
-
表 1 两组患者切口长度、手术时间及出血量的比较
Table 1. Comparison of incision length, operation time and bleeding amount (Mean±SD)
项目 常规手术腹直肌旁切口(n=27) 3D结合腹直肌旁切口(n=23) t P 切口长度(cm) 9.56±1.98 6.33±0.90 7.597 0.000 手术时间(min) 170.00±69.02 80.65±20.85 6.393 0.000 出血量(mL) 8 94.44±473.80 389.13±191.12 4.788 0.000 -
[1] Pelleray C. Protrusion of the femoral vessels into the obturator foramen associated with fracture of the pelvis. Surgical treatment[J]. J Chir, 1976, 112(5): 161-4. [2] Vallier HA, Cureton BA, Patterson BM. Factors affecting revenue from the management of pelvis and acetabulum fractures[J]. J Orthop Trauma, 2013, 27(5): 267-74. doi: 10.1097/BOT.0b013e318269b2c3 [3] 吴超, 邓佳燕, 谭伦, 等. 3D打印技术辅助不稳定性骨盆骨折手术疗效分析[J].中国修复重建外科杂志, 2019, 33(4): 455-61. [4] 殷勇. 3D打印骨折模型在复杂骨盆骨折手术治疗中的远期效果分析[J].广西医科大学学报, 2019, 36(2): 305-7. [5] 李攀, 李让贤, 夏兴平, 等. 3D打印技术在复杂Pilon骨折治疗中的应用[J].实用骨科杂志, 2016, 22(10): 939-41, 942. [6] 马腾, 魏代好, 秦悦, 等.常规影像学结合3D打印技术在复杂胫骨平台骨折治疗中的应用[J].宁夏医科大学学报, 2017, 39(12): 1452- 4, 1506. [7] 钟浩博, 刘伟乐, 孙春汉, 等. 3D打印技术在肘关节恐怖三联征治疗中的应用效果评估[J].分子影像学杂志, 2020, 43(1): 162-6. doi: 10.12122/j.issn.1674-4500.2020.01.34 [8] 曾参军, 谭新宇, 黄华军, 等.基于3D打印的腹直肌旁切口治疗骨盆骨折的临床疗效[J].南方医科大学学报, 2016, 36(2): 220-5. doi: 10.3969/j.issn.1673-4254.2016.02.13 [9] Matta JM, Dickson KF, Markovich GD. Surgical treatment of pelvic nonunions and malunions[J]. Clin Orthop Relat Res, 1996(329): 199-206. [10] Majeed SA. Grading the outcome of pelvic fractures[J]. J Bone Jo Surg-Br Vol, 1989, 71(2): 304-6. [11] Ormond JK, Fairey PW. Urethral rupture at apex of the prostate; complication of fracture of the pelvis[J]. J Am Med Assoc, 1952, 149 (1): 15-8. doi: 10.1001/jama.1952.02930180017004 [12] Wardle B, Eslick GD, Sunner P. Internal versus external fixation of the anterior component in unstable fractures of the pelvic ring: pooled results from a systematic review[J]. Eur J Trauma Emerg Surg, 2016, 42(5): 635-43. doi: 10.1007/s00068-015-0554-4 [13] 林钢.数字化结合3D打印技术辅助复杂骨盆骨折的手术设计[J].中国临床解剖学杂志, 2016, 34(3): 293-7. [14] 章莹, 李宝丰, 王新宇, 等.术前3D打印技术模拟复杂骨盆骨折手术提高疗效的可行性研究[J].中华创伤骨科杂志, 2015(1): 29-33. doi: 10.3760/cma.j.issn.1671-7600.2015.01.008 [15] 高文杰. 3D打印技术用于骨盆骨折的疗效探究[J].甘肃科技, 2020, 36(4): 121-3. doi: 10.3969/j.issn.1000-0952.2020.04.040 [16] 张国栋, 林海滨, 陈宣煌, 等.基于多平面三维测量的髋臼骨折数字化内固定植入方案[J].中华临床医师杂志(电子版), 2012, 6(8): 2010-5. doi: 10.3877/cma.j.issn.1674-0785.2012.08.009 [17] 孟国林, 刘建, 胡蕴玉, 等.快速成型模型在制定胫骨平台复杂骨折手术方案中的指导作用[J].中华创伤骨科杂志, 2011(12): 1135-8. doi: 10.3760/cma.j.issn.1671-7600.2011.12.009 -






 下载:
下载: