Value of transvaginal sonography combined with MRI in the diagnosis of residual myometrial thickness in cesarean scar pregnancy
-
摘要:
目的分析经阴道彩色多普勒超声(TVS)检查联合MRI诊断剖宫产切口瘢痕妊娠残余子宫肌层厚度的价值。 方法连续收集2019年1月~2020年6月本院收治的80例超声检查剖宫产切口瘢痕妊娠(CSP)疑似切口处残余子宫肌层小于3 mm患者的临床资料,80例患者均要求终止妊娠,所有患者入院后均完善阴道超声检查和MRI检查,并与手术、病理学检查结果进行对比,分析两种诊断方法的影像学特点,探讨其临床诊断价值。 结果经手术、病理学证实80例疑似CSP切口处残余子宫肌层小于3 mm患者有71例,阴道超声联合MRI诊断阳性72例,阴性8例,诊断准确率为96.25%,特异度77.78%,灵敏度98.59%,阳性预测值为97.22%,阴性预测值87.50%,Kappa值0.803;阴道超声观察到卵黄囊结构40例、胚芽结构25例,原始心管搏动15例,MRI在对孕囊内部结构观察方面远不如超声,其优势在于孕囊周边的比邻结构的观察。 结论阴道超声检查与MRI对CSP切口处残余子宫肌层厚度的诊断准确率均较高,两者联合大大提高了诊断准确率,超声在切口肌层血流信号观察、阻力指数、孕囊内卵黄囊、胚芽及胎心搏动诊断方面有优势,实时、价廉,可重复性强,MRI能够更好的评估切口处剩余肌层的厚度以及与周围组织的关系,二者联合检测可更好的评估切口处残余子宫肌层的厚度,为患者和手术医生选择手术方式提供更有力的依据。 Abstract:ObjectiveTo analyze the value of transvaginal sonography (TVS) combined with MRI in the diagnosis of residual myometrial thickness in cesarean scar pregnancy (CSP). MethodsEighty CSP cases with residual myometrium less than 3 mm were collected from January 2019 to June 2020. All patients were requested for termination of pregnancy and received TVS and MRI after admission. Besides, the examination results were compared with surgical and pathological findings. Imaging features of the two diagnostic methods were analyzed, and their clinical diagnostic value was discussed. ResultsIn this study, surgery and pathology confirmed 71 cases with residual myometrial thickness smaller than 3mm at the incision of CSP. TVS combined with MRI diagnostic results were positive in 72 cases and negative in 8 cases, and the diagnostic accuracy, specificity, sensitivity, positive predictive value, negative predictive value and Kappa value were 96.25%, 77.78%, 98.59%, 97.22%, 87.50%, and 0.803, respectively. TVS found 40 cases with yolk sac structure, 25 cases with germ structure, 15 cases with pulsating primitive heart tube. MRI was far inferior to ultrasound in observing internal structure of the gestational sac but it was better than ultrasound in observing adjacent structure around the gestational sac. ConclusionBoth TVS and MRI have high accurac in the diagnosis of residual myometrial thickness of CSP, and combination of these two methods greatly improves the diagnostic accuracy. Ultrasound has more advantages in observing blood flow signals at incision muscular layer, resistance index, yolk sac inside the pregnancy sac, blastema and fetal heartbeat, which is also real-time, cheap and highly repeatable. MRI can be used to better assess the thickness of residual muscle layer at the incision and its relationship with surrounding tissues. The joint detection of these two methods can better display the residual myometrial thickness at the incision, thereby providing a strong basis for patients and surgeons to choose the operation method. -
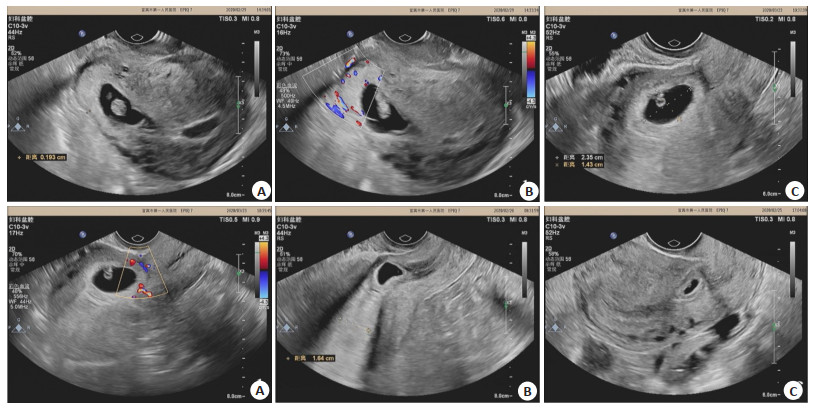
图 1 阴道超声妊娠诊断的切口妊娠图片
A, B为同一患者:A:经阴道超声诊断的切口妊娠(2D图); B:经阴道超声诊断的孕60余天的切口妊娠,胎盘已可见,完全植入切口内,向膀胱方向凸出,残余子宫肌层菲薄(小于3 mm), Ⅲ型; C, D为同一患者:C:经阴道超声检查的切口妊娠, 妊娠囊大部分位于宫腔, Ⅱ型; D:经阴道超声检查切口妊娠彩色多普勒血流图, 切口处肌层菲薄, 切口处肌层血流较丰富, 切口肌层小于3 mm, Ⅱ型; E:经阴道超声检查的切口妊娠, 孕囊凸入切口内, 向膀胱方向凸出, 切口处肌层小于3 mm, Ⅲ型; F:经阴道超声检查的停经40 d的切口妊娠, 孕囊凸入切口内, 切口处肌层小于3 mm,Ⅱ型.
Figure 1. Images of incision pregnancy diagnosed by vaginal ultrasound.
表 1 MRI诊断与手术、病理学结果比较(n)
Table 1. Comparison of diagnostic results between MRI and surgical pathology
诊断方法 手术、病理学 合计 阳性 阴性 阴道超声联合MRI检杳 阳性 70 2 72 阴性 1 7 8 合计 71 9 80 -
[1] Glenn TL, Bembry J, Findley AD, et al.Cesarean scar ectopic pregnancy:current management strategies[J].Obstet Gynecol Surv, 2018, 73(5):293-302. [2] Vikhareva O, Rickle GS, Lavesson T, et al.Hysterotomy level at Cesarean section and occurrence of large scar defects:a randomized single-blind trial[J].Ultrasound Obstet Gynecol, 2019, 53(4):438-42. [3] 叶青剑, 邓佩霞, 沈晓婷, 等.剖宫产切口瘢痕妊娠分析[J].中山大学学报:医学科学版, 2017, 38(4):596-600. [4] Setubal A, Alves J, Osório F, et al.Treatment for uterine isthmocele, A pouchlike defect at the site of a cesarean section scar[J].J Minim Invasive Gynecol, 2018, 25(1):38-46. [5] Tulandi T, Cohen A.Emerging manifestations of cesarean scar defect in reproductive-aged women[J].J Minim Invasive Gynecol, 2016, 23(6):893-902. [6] 符声玉, 龙璨.经阴道彩超诊断剖宫产瘢痕部位妊娠的临床意义[J].中国现代医学杂志, 2019, 29(24):123-6. [7] Corrado G, Durante A, Genchi V, et al.Prevalence of previously undiagnosed abdominal aortic aneurysms in the area of Como:the ComoCuore"looking for AAA"ultrasonography screening[J].Int J Cardiovasc Imaging, 2016, 32(8):1213-7. [8] 刘炳光, 曹满瑞, 张玉霞, 等.不同类型剖宫产切口妊娠MRI特征及比较[J].放射学实践, 2017, 32(3):275-8. [9] 王亚, 郑晓林, 王强, 等.瘢痕妊娠MRI表现及对临床分型的价值[J].临床放射学杂志, 2019, 38(8):1463-7. [10] Gonzalez N, Tulandi T.Cesarean scar pregnancy:a systematic review[J].J Minim Invasive Gynecol, 2017, 24(5):731-8. [11] Donnez O, Donnez J, Orellana R, et al.Gynecological and obstetrical outcomes after laparoscopic repair of a cesarean scar defect in a series of 38 women[J].Obstet Gynecol Surv, 2017, 72(5):283-4. [12] Keung JJ, Spies JB, Caridi TM.Uterine artery embolization:a review of current concepts[J].Best Pract Res Clin Obstet Gynaecol, 2018, 46:66-73. [13] Elshani B, Arifi H, Daci A.Microperforated hymen presenting spontaneous pregnancy with cesarean delivery and hymenotomy surgery:a case report[J].Open Access Maced J Med Sci, 2018, 6(3):528-30. [14] 雷岩, 魏冉, 宋彬.剖宫产子宫瘢痕妊娠MRI及超声诊断对照分析[J].中国医学计算机成像杂志, 2017, 23(2):151-5. [15] 杨婷, 吴婷婷, 唐纳, 等.经阴道超声在子宫切口妊娠诊断和治疗中的应用[J].上海交通大学学报:医学版, 2017, 37(10):1398-401. [16] 陈丽, 李小晶, 李蕾, 等.经阴道超声和MRI对剖宫产术后早期子宫瘢痕妊娠的诊断价值比较[J].实用放射学杂志, 2016, 32(4):566-9. [17] 徐优文, 郭银珍.剖宫产切口瘢痕妊娠的MRI、超声表现及诊断价值[J].中国CT和MRI杂志, 2016, 14(6):101-3. [18] 郭艳嫦, 严燕琼, 雷伟玲, 等.经阴道彩色多普勒超声对Ⅰ型及Ⅱ型子宫瘢痕妊娠的诊断价值[J].分子影像学杂志, 2019, 42(3):306-9. [19] Cheng XY, Cheng L, Li WJ, et al.The effect of surgery on subsequent pregnancy outcomes among patients with cesarean scar diverticulum[J].Int J Gynaecol Obstet, 2018, 141(2):212-6. [20] 许国琰.超声诊断子宫下段全层厚度对瘢痕子宫再妊娠患者分娩结局的影响[J].中国实验诊断学, 2019, 23(7):1169-71. -






 下载:
下载: