Curative effect and imaging effect of PLF on patients with lumbar spondylolisthesis
-
摘要:
目的探讨后外侧植骨融合术(PLF)在治疗腰椎滑脱症患者中的临床效果。 方法回顾性研究我院骨科收治的118例腰椎滑脱症患者,其中58例患者采用PLF联合椎弓根螺钉内固定手术治疗(PLF组)、60例患者采用后路椎间植骨融合术(PLIF)联合椎弓根螺钉内固定手术治疗(PLIF组);统计分析两组的手术时间、手术出血量以及采用X线、CT等手段测量植骨融合率、并发症率、手术前后日本骨科协会评估治疗(JOA评分)、椎间隙高度、椎体滑脱率等。 结果PLF组和PLIF组患者的手术时间、手术出血量差异无统计学意义(P>0.05);PLF组的植骨融合率低于PLIF组患者(84.48% vs 96.67% P < 0.05);术前PLF组和PLIF组患者的JOA评分、椎间隙高度、椎体滑脱率差异无统计学意义(P>0.05);术后1年PLF组的JOA评分低于PLIF组患者的96.67%(P < 0.05),PLF组患者的椎体滑脱率高于PLIF组(P < 0.05);术后1月、术后1年,PLF组的椎间隙高度均低于PLIF组(P < 0.05);PLF组的手术并发症率(6.90%)与PLIF组患者(3.33%)的差异无统计学意义(P>0.05)。 结论腰椎滑脱症患者采用PLF与PLIF治疗效果均较好,PLIF手术较PLF手术更有利于维持术后腰椎功能恢复、维持椎间隙高度、减少术后椎体滑脱的发生率。 Abstract:ObjectiveTo explore the clinical effect of posterolateral bone graft fusion (PLF) in the treatment of patients with lumbar spondylolisthesis. MethodsA retrospective study of 118 patients with lumbar spondylolisthesis was conducted in our hospital's Orthopedics Department. Among them, 58 patients were treated with PLF combined with pedicle screw internal fixation (PLF group), and 60 patients were treated with posterior interbody fusion (PLIF) along with pedicle screw internal fixation surgery (PLIF group). Operation time, surgical bleeding volume, bone graft fusion rate using X lines, CT, complications rate, JOA score before and after the operation, intervertebral space height, vertebral body slippage rate, ect. were statistically analyzed in two groups. ResultsThere was no statistically significant difference in operation time, the amount of bleeding, JOA score intervertebral space height, and vertebral spondylolisthesis rate between the PLF group and the PLIF group (P>0.05); the bone graft fusion rate in the PLF group was 84.48% lower than the 96.67% in the PLIF group (P < 0.05); The surgical complication rate had no significant different with 6.90% of PLF group and 3.33% of PLIF group.1 year after operation, JOA score in PLF group was lower than 96.67% in PLIF group (P < 0.05), the vertebral spondylolisthesis rate of patients in PLF group was higher than that of PLIF group (P < 0.05); the height of intervertebral space in PLF group was lower than that of PLIF group 1 month and 1 year after surgery (P < 0.05). ConclusionPLF and PLIF are both good treatment for lumbar spondylolisthesis. PLIF surgery is more beneficial to maintain postoperative lumbar spine function recovery, intervertebral space height, and reduce the incidence of postoperative vertebral spondylolisthesis. -
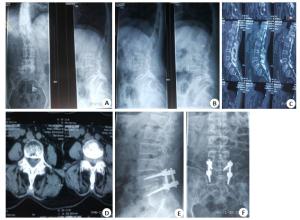
图 1 患者男,61岁,腰椎滑脱腰椎间盘突出症,完善影像学检查后确定为腰5椎体Ⅱ度滑脱
A:术前X线正侧位; B:过伸过屈位X线; C: CT冠状位扫描; D: CT平扫患者采用PLIF联合椎弓根螺钉内固定手术治疗; E~F:术后1月X线复查结果.
Figure 1. A 61-year-old male with lumbar spondylolisthesis of the lumbar intervertebral disc. After complete imaging examination, it was determined that the lumbar 5 vertebral body spondylolisthesis
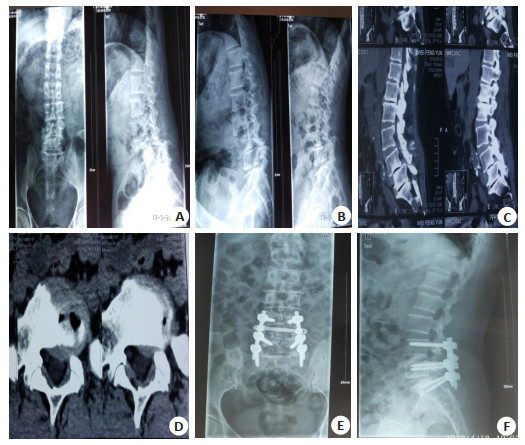
图 2 患者女,73岁,腰椎滑脱入院,完善影像学检查后确定为腰5椎体Ⅰ度滑脱
A:术前X线正侧位; B:过伸过屈位X线; C: CT冠状位扫描; D: CT平扫患者采用PLF联合椎弓根螺钉内固定手术治疗; E~F:术后1月X线复查结果.
Figure 2. A female patient was 73 years old and was admitted to the hospital with lumbar spondylolisthesis. After complete imaging examination, it was determined that the lumbar 5 vertebral body was spondylolisthesis.
表 1 两组患者手术相关指标比较
Table 1. Comparison of surgery-related indexes between the two groups
组别 手术时间(min, Mean±SD) 手术出血量(mL, Mean±SD) 植骨融合率[n(%)] PLF组(n=58) 180.6±15.8 676.8±89.4 49(84.48) PLIF组(n=60) 183.2±18.6 688.1±95.2 58(96.67) t/χ2 -0.817 -0.664 5.179 P 0.416 0.508 0.023 表 2 两组患者手术前后的JOA评分、椎间隙高度、椎体滑脱率比较
Table 2. Comparison of JOA score, intervertebral space height, and vertebral spondylolisthesis before and after operation in two groups (Mean±SD)
指标 术前 术后1月 术后1年 JOA评分(分) PLF组(n=58) 16.33±2.75 21.76±3.20 24.37±2.85 PLIF组(n=60) 15.97±2.60 22.61±2.94 25.78±2.67 t 0.731 -1.503 -2.774 P 0.466 0.135 0.006 椎间隙高度(mm) PLF组(n=58) 6.83±1.50 10.82±2.41 10.78±2.67 PLIF组(n=60) 6.60±1.48 14.11±2.79 13.85±2.60 t 0.838 -6.845 -6.328 P 0.404 0.000 0.000 椎体滑脱率(%) PLF组(n=58) 34.72±5.04 14.69±2.80 16.00±2.77 PLIF组(n=60) 34.26±4.98 13.88±2.69 14.21±2.51 t 0.499 1.603 3.681 P 0.619 0.112 0.000 表 3 两组患者手术并发症率率比较
Table 3. Comparison of the rate of surgical complications between the two groups (n)
组别 切口感染 下肢深静脉血栓 泌尿系统感染 并发症率[n(%)] PLF组(n=58) 1 1 2 4(6.90) PLIF组(n=60) 0 1 1 2(3.33) χ2 - - - 0.776 P - - - 0.378 -
[1] 冯学烽, 邹伟民, 庞祖才, 等. 3D打印技术在腰椎滑脱症椎弓根螺钉置入术中的应用[J].临床骨科杂志, 2018, 21(1): 17-9. http://www.cnki.com.cn/Article/CJFDTotal-LCGK201801007.htm [2] 王成伟, 鲁世保, 孔超, 等.单节段退变性腰椎滑脱与腰椎间盘突出症患者椎旁肌横截面积的比较研究[J].中华外科杂志, 2018, 56(4): 303-4. http://oldmed.wanfangdata.com.cn/Paper/Detail/PeriodicalPaper_zhwk201804013 [3] 农家隆.椎弓根螺钉复位内固定后单纯植骨融合与椎间融合器融合治疗腰椎滑脱症的疗效比较[J].中外医疗, 2018, 37(8): 39-41, 44. http://www.cqvip.com/QK/88753X/20188/7000649143.html [4] 刘鹏辉, 郑燕平, 阎峻, 等.退变性腰椎滑脱患者多裂肌萎缩与滑脱程度相关性研究[J].中华骨科杂志, 2020, (2): 82-7. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=zhgkzz98202002003 [5] 曾忠友, 张建乔, 严卫锋, 等.双侧肌间隙入路通道下椎弓根钉棒复位融合固定治疗腰椎滑脱症[J].中华骨科杂志, 2018(20):1220-9. [6] Zhang HP, Miao Q, Hao DJ, et al. Direction-changeable cage reduces X-ray exposure in treating isthmic lumbar spondylolisthesis: a retrospective study[J].Am J Transl Res, 2019, 11(2): 1066-72. http://www.ncbi.nlm.nih.gov/pubmed/30899406 [7] 张玉民, 王献印, 张欲燃.后路经椎弓根钉棒系统复位固定+椎体间融合及后外侧融合治疗腰椎滑脱症[J].中国医药指南, 2011, 9(7): 84-5. http://d.wanfangdata.com.cn/Periodical/zgyyzn201107054 [8] Spoor JKH, Dallenga AHG, Gadjradj PS, et al. A novel noninstrumented surgical approach for foramen reconstruction for isthmic spondylolisthesis in patients with radiculopathy: preliminary clinical and radiographic outcomes[J]. Neurosurg Focus, 2018, 44(1): E7. http://www.ncbi.nlm.nih.gov/pubmed/29290136 [9] 戎飞龙, 尹若峰, 冯蒙蒙, 等.退变性腰椎滑脱症和腰椎管狭窄症与椎体周围肌容量的相关性: CT和MRI影像资料分析[J].中国组织工程研究, 2019, 23(24): 74-9. http://www.cqvip.com/QK/80481C/201924/7002014002.html [10] Jazini E, Gum JL, Glassman SD, et al. Cost-effectiveness of circumferential fusion for lumbar spondylolisthesis: propensitymatched comparison of transforaminal lumbar interbody fusion with anterior-posterior fusion[J]. Spine J, 2018, 18(11): 1969-73. http://europepmc.org/abstract/MED/29705337 [11] Tschugg A, Kavakebi P, Hartmann S, et al. Clinical and radiological effect of medialized cortical bone trajectory for lumbar pedicle screw fixation in patients with degenerative lumbar spondylolisthesis: study protocol for a randomized controlled trial (mPACT) [J]. Trials, 2018, 19(1): 129. doi: 10.1186/s13063-018-2504-z [12] Cyriac M, Kyhos J, Iweala U, et al. Anterior lumbar interbody fusion with cement augmentation without posterior fixation to treat isthmic spondylolisthesis in an osteopenic patient-A surgical technique[J]. Int J Spine Surg, 2018, 12(3): 322-7. doi: 10.14444/5037 [13] 陈景涛.后路减压椎弓根螺钉内固定复位联合椎间融合器植骨融合术治疗腰椎滑脱症的体会[J].河南外科学杂志, 2019, 25(3): 129-30. http://d.old.wanfangdata.com.cn/Periodical/hnwkxzz201903072 [14] Meissner-Haecker A, Urrutia J. Does adding interbody fusion to posterolateral fusion increase success in the surgical management of degenerative lumbar spondylolisthesis[J]? Medwave, 2018, 18(1): e7147. http://www.ncbi.nlm.nih.gov/pubmed/29385121 [15] Urquhart JC, Alnaghmoosh N, Gurr KR, et al. Posterolateral versus posterior interbody fusion in lumbar degenerative spondylolisthesis [J]. Clin Spine Surg, 2018, 31(9): E446-52. http://journals.lww.com/jspinaldisorders/Abstract/2018/11000/Posterolateral_Versus_Posterior_Interbody_Fusion.12.aspx [16] Sleem A, Marzouk A. Transforaminal lumbar interbody fusion with local bone graft alone for single-level isthmic spondylolisthesis[J]. Int J Spine Surg, 2018, 12(1): 70-5. http://www.ncbi.nlm.nih.gov/pubmed/30280086 [17] Karki S, Zhang SD, Wang XH, et al. Comparison of clinical outcomes of cortical bone trajectory and traditional pedicle screw fixation in posterior lumbar interbody fusion[J]. Open J Orthop, 2019, 9(3): 31-47. http://www.researchgate.net/publication/331402060_Comparison_of_Clinical_Outcomes_of_Cortical_Bone_Trajectory_and_Traditional_Pedicle_Screw_Fixation_in_Posterior_Lumbar_Interbody_Fusion [18] Cho JH, Hwang CJ, Kim H, et al. Effect of osteoporosis on the clinical and radiological outcomes following one-level posterior lumbar interbody fusion[J]. J Orthop Sci, 2018, 23(6): 870-7. http://www.ncbi.nlm.nih.gov/pubmed/30431006 [19] Sakaura H, Miwa T, Yamashita T, et al. Cortical bone trajectory screw fixation versus traditional pedicle screw fixation for 2- level posterior lumbar interbody fusion: comparison of surgical outcomes for 2-level degenerative lumbar spondylolisthesis[J]. J Neurosurg Spine, 2018, 28(1): 57-62. http://www.ncbi.nlm.nih.gov/pubmed/29125430 [20] 卢文灿, 段春光, 陶惠人, 等.腰椎后路椎间融合术后融合器脱出的处理策略[J].中华骨与关节外科杂志, 2019, 12(5): 356-61. -






 下载:
下载: