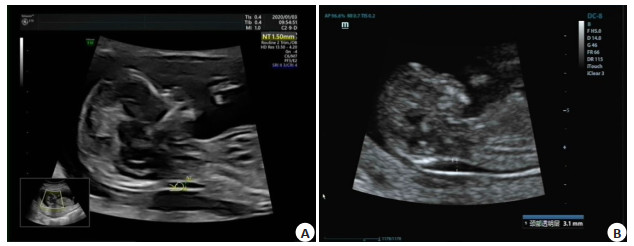
Thickness of different neck transparent layers can be used as a predictor of outcome of fetal poor perinatal
-
摘要:
目的探索不同颈项透明层厚度(NT)与胎儿不良围产结局的关系。 方法回顾性分析2017年3月~2019年3月于我院分娩的496例孕妇临床资料,筛选其中胎儿NT值异常的98例孕妇(单纯NT值增厚56例,妊娠不良结局42例)为研究对象,依据妊娠结局分为单纯胎儿NT值增厚组56例与妊娠不良结局组42例,对两组NT值、年龄、血清Freeβ-hCG异常率、NIPT染色体异常率进行对比;依据胎儿NT值异常增厚程度分为Ⅰ组:2.50~3.00 mm的,Ⅱ组:3.01~4.00 mm,Ⅲ组:4.01~5.00 mm,Ⅳ组: > 5.00 mm,对不良妊娠结局以及染色体异常发生率进行对比;利用Logistic回归分析法对胎儿围产结局、染色体异常的相关因素进行检验。 结果本次研究共发现56例单纯NT值增厚患者,42例妊娠不良结局患者,妊娠不良结局发生率为42.86%;妊娠不良结局组NT值、年龄均大于单纯NT增厚组,妊娠不良结局组血清人绒毛膜促性腺激素游离β亚基(Freeβ-hCG)异常率、NIPT染色体异常率高于单纯NT增厚组(P < 0.05)。各不同胎儿NT值分组孕周、初产妇、BMI、长期吸烟史、糖尿病、高血压数据对比差异不具有统计学意义(P > 0.05)。Ⅰ、Ⅱ组正常胎儿占比高于Ⅲ、Ⅳ组,染色体异常发生率则较低(P < 0.05)。Logistic回归显示,NT值过度增加、年龄偏大、Freeβ-hCG异常及NIPT染色体异常是影响胎儿妊娠结局的危险因素(P < 0.05,OR > 1);此外,NT值过度增加、年龄偏大是影响染色体异常的危险因素(P < 0.05,OR > 1),而Freeβ-hCG异常和染色体异常也有显著的关联影响关系(P < 0.05)。 结论胎儿NT值能够作为胎儿围产期妊娠不良结局的预测指标,且胎儿NT值增加会提高胎儿发生妊娠不良结局的风险及胎儿染色体异常的发生率。 Abstract:ObjectiveTo explore the relationship between the thickness of different cervical transparent layers (NT) and the outcome of fetal poor perinatal outcomes. MethodsThe clinical data of 496 pregnant women who were delivered in our hospital from March 2017 to March 2019 were retrospectively analyzed. Niety-eight pregnant women with abnormal fetal NT value were divided into 56 cases of pure fetal NT value thickening group and 42 cases of poor pregnancy outcome group according to pregnancy outcome. The NT value, age, serum Freeβ-hCG abnormal rate and NIPT chromosome abnormal rate were compared between the two groups. The value of abnormal thickening was divided into 4 groups of 2.50-3.00 mm group (group Ⅰ), 3.01-4.00 mm group (group Ⅱ), 4.01-5.00 mm group (group Ⅲ) and 5.00 mm group (group Ⅳ). The rates were compared. Logistic regression analysis was used to test the related factors of fetal perinatal outcomes and chromosomal abnormalities. ResultsA total of 56 patients with purely thickened NT values and 42 patients with poor pregnancy outcomes were found. The incidence of poor pregnancy outcomes was 42.86%. The NT value and age of the patients with poor pregnancy outcomes were significantly larger than those of the purely thickened NT patients. The abnormal rate of serum human chorionic gonadotropin free β-subunit (Freeβ-hCG) and the abnormal rate of NIPT chromosomes were significantly higher in the group than in the NT thickening group. The proportion of normal fetus in group Ⅰ was significantly higher than that in group Ⅱ, group Ⅲ and group Ⅳ. The incidence of fetal pregnancy in group Ⅲ was 100.00%, and the incidence of chromosomal abnormality was 71.43%, which was significantly higher than group Ⅰ and Ⅱ. The incidence of chromosomal abnormalities in the incidence of fetal pregnancy in group and group Ⅳ was significantly different (P < 0.05). ConclusionFetal NT value can be used as a predictor of fetal perinatal pregnancy outcome. The increase of fetal NT value will increase the risk of fetal adverse pregnancy outcome. The highest incidence of fetal chromosomal abnormalities between NT and 4.10-5.00 mm. -
Key words:
- neck transparent layer thickness /
- adverse outcome /
- perinatal period /
- correlation
-
表 1 单纯NT增厚组和妊娠不良结局组超声参数与异常情况对比
Table 1. Comparison of ultrasound parameters and abnormalities in the NT thickening group and the adverse pregnancy outcome group
组别 NT值(mm, Mean±SD) 年龄(岁, Mean±SD) 结构异常[n (%)] Freeβ-hCG异常[n(%)] NIPT染色体异常[n(%)] 单纯NT增厚组(n=56) 2.86±0.15 27.29±3.12 - 1 (1.79) 1 (1.79) 妊娠不良结局组(n=42) 5.61±0.79 32.59±4.57 36 (85.71) 6 (14.29) 10 (23.81) t/χ2 22.261 6.470 - 3.926 9.577 P 0.000 0.000 - 0.048 0.002 NIPT: Non-invasive Prenatal Testing. 表 2 不同胎儿NT值分组胎儿临床特征对比
Table 2. Comparison of clinical characteristics of fetuses with different fetal NT values
组别 孕周(周, Mean±SD) 初产妇[n (%)] BMI (kg/m2, Mean±SD) 长期吸烟史[n (%)] 糖尿病[n (%)] 高血压[n (%)] Ⅰ组(n=51) 39.57±5.64 7 (13.73) 24.75±3.29 13 (25.49) 8 (15.69) 3 (5.88) Ⅱ组(n=22) 40.15±7.15 3 (13.64) 23.98±2.15 5 (22.73) 3 (13.64) 1 (4.55) Ⅲ组(n=7) 38.16±6.30 1 (14.29) 25.10±3.47 2 (28.57) 1 (14.29) 0 (0.00) Ⅳ组(n=18) 37.59±5.10 2 (11.11) 24.87±2.88 4 (22.22) 3 (16.67) 1 (5.56) χ2/F 0.337 0.091 0.553 0.178 0.084 0.462 P 0.799 0.993 0.647 0.981 0.994 0.927 BMI: Body Mass Index. 表 3 不同胎儿NT值分组胎儿妊娠结局及染色体异常情况对比
Table 3. Comparison of fetal pregnancy outcomes and chromosomal abnormalities in different fetal NT groups[n(%)]
组别 正常胎儿 妊娠不良结局胎儿 NIPT染色体异常 Ⅰ组(n=51) 40 (78.43) 11 (21.57) 1 (1.96) Ⅱ组(n=22) 15 (68.18) 7 (31.82) 3 (13.64) Ⅲ组(n=7) 0 (0.00) 7 (100.00) 5 (71.43) Ⅳ组(n=18) 1 (5.56) 17 (94.44) 1 (5.56) χ2 39.426 33.126 P 0.000 0.000 表 4 胎儿妊娠结局的影响因素的Logistic回归结果
Table 4. Logistic regression results of influencing factors of fetal pregnancy outcome
因素 赋值说明 回归系数 标准误差 Wald卡方 P OR OR 95%置信区间 NT值 1=≥3.5mm,0= < 3.5 mm 1.816 0.490 13.762 0.000 6.147 2.355~16.045 年龄 1=≥29岁,0= < 29岁 0.757 0.339 4.995 0.025 2.132 1.098~4.141 Freeβ-hCG异常 1=异常,0=否 0.420 0.178 5.566 0.018 1.522 1.074~2.158 NIPT结果 1=染色体异常,0=否 1.217 0.351 12.034 0.000 3.377 1.698~6.717 表 5 染色体异常的影响因素之Logistic回归结果
Table 5. Logistic regression results of factors affecting chromosomal abnormalities
因素 赋值说明 回归系数 标准误差 Wald卡方 P OR OR 95%置信区间 NT值 1=≥,0= < 1.293 0.369 12.267 0.000 3.642 1.767~7.507 年龄 1= ≥,0= < 0.423 0.211 4.042 0.044 1.527 1.011~2.307 Freeβ-hCG异常 1= ≥,0= < 0.979 0.411 5.673 0.017 2.661 1.189~5.954 -
[1] 王清, 王欣.妊娠早期水囊状淋巴管瘤胎儿的结局分析及其与颈部透明层增厚的关系[J].中华妇产科杂志, 2018, 53(10): 665-70. http://d.old.wanfangdata.com.cn/Periodical/zhfck201810003 [2] 周伟娜, 李春擎, 高磊, 等.超声下颈项透明层异常对胎儿染色体的筛查效果[J].中国医药导刊, 2017, 19(1): 49-50. http://d.old.wanfangdata.com.cn/Periodical/zgyydk201701025 [3] Koert E, Harrison C, Bunting L, et al. Causal explanations for lack of pregnancy applying the common sense model of illness representation to the fertility context[J]. Psychol Health, 2018, 33 (10): 1284-301. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=10.1080/08870446.2018.1494831 [4] Lopes van Balen VA, van Gansewinkel TAG, de Haas S, et al. Physiological adaptation of endothelial function to pregnancy: systematic review and meta-analysis[J]. Ultrasound Obstet Gynecol, 2017, 50(6): 697-708. http://cn.bing.com/academic/profile?id=de48d88ca089715a4f275cbf21b66112&encoded=0&v=paper_preview&mkt=zh-cn [5] 唐永红, 党彩玲, 阳春芳.妊娠早期单胎NT≥2.5 mm孕妇侵入性产前诊断及预后分析[J].四川医学, 2019, 40(6): 580-3. http://d.old.wanfangdata.com.cn/Periodical/scyx201906008 [6] 蒋瑜, 杨太珠, 罗红128例颈项透明层厚度异常染色体正常胎儿妊娠结局分析[J].中国超声医学杂志, 2017, 33(5): 447-9. http://d.old.wanfangdata.com.cn/Periodical/zgcsyxzz201705023 [7] 徐玲玲, 余颀, 毛倩倩, 等. 128例颈项透明层增厚胎儿染色体核型及妊娠结局分析[J].中国妇幼保健, 2019, 34(4): 858-60. http://d.old.wanfangdata.com.cn/Periodical/zgfybj201904044 [8] 袁小波, 朱文兵.探讨颈项透明层厚度与胎儿染色体异常及妊娠结局的关系[J].中国妇幼保健, 2019, 34(13): 3115-7. http://d.old.wanfangdata.com.cn/Periodical/zgfybj201913067 [9] Yu YX, Li MC, Pu LY, et al. Sleep was associated with depression and anxiety status during pregnancy: a prospective longitudinal study[J]. Arch Womens Ment Health, 2017, 20(5): 695-701. http://cn.bing.com/academic/profile?id=3426f966ccde29e79ac4edad99a2703a&encoded=0&v=paper_preview&mkt=zh-cn [10] Baumfeld Y, Herskovitz R, Niv ZB, et al. Placenta associated pregnancy complications in pregnancies complicated with placenta previa[J]. Taiwan J Obstet Gynecol, 2017, 56(3): 331-5. http://cn.bing.com/academic/profile?id=baa473e266807f32548e778c93ad45a1&encoded=0&v=paper_preview&mkt=zh-cn [11] 王齐媛.彩色多普勒超声对异常双胎妊娠及妊娠结局的诊断价值[J].中国妇幼保健, 2016, 31(7): 1543-4. http://d.old.wanfangdata.com.cn/Periodical/zgfybj201607073 [12] 郑烨, 勇强, 张蕾, 等.胎儿颈项透明层测值与妊娠不良结局的相关性分析[J].中国超声医学杂志, 2019, 35(1): 43-5. http://d.old.wanfangdata.com.cn/Periodical/zgcsyxzz201901015 [13] 侯莉, 张冬梅, 叶才为, 等.超声检测早孕期颈项透明层增厚的临床价值[J].临床超声医学杂志, 2017, 19(9): 637-9. http://d.old.wanfangdata.com.cn/Periodical/lccsyxzz201709025 [14] Barisic T, Mandic V, Barac I. Associations of body mass index and gestational weight gain with term pregnancy outcomes[J]. Mater Sociomed, 2017, 29(1): 52-7. http://d.old.wanfangdata.com.cn/OAPaper/oai_doaj-articles_5f5844477694865dad6cca9e84e902d8 [15] Jain D. Rh isoimmunized pregnancy managed noninvasively: a report of two cases[J]. Int J Appl Basic Med Res, 2017, 7(1): 73-6. http://cn.bing.com/academic/profile?id=6d05192d12424434d1300bf26ff8e110&encoded=0&v=paper_preview&mkt=zh-cn [16] 何顺安, 肖燕, 魏玲, 等.胎儿颈项透明层厚度对筛查胎儿异常的临床价值[J].中国实验诊断学, 2017, 21(3): 458-60. http://d.old.wanfangdata.com.cn/Periodical/zgsyzdx201703026 [17] 倪梦瑶, 李洁, 朱湘玉, 等.染色体微阵列分析在颈项透明层增厚胎儿产前诊断中的应用[J].中华医学遗传学杂志, 2019(10): 970-4. http://d.old.wanfangdata.com.cn/Periodical/zhyxycx201910006 [18] 燕凤, 徐慧, 李春艳, 等. NT增厚胎儿的染色体异常率及妊娠结局分析[J].中国妇幼健康研究, 2019, 30(12): 1557-60. http://d.old.wanfangdata.com.cn/Periodical/gwyx-fybj201912015 [19] 陶华娟, 王春霞, 李晓东, 等.胎儿超声软指标异常与不良妊娠结局的临床价值研究[J].中国产前诊断杂志:电子版, 2018, 10(3): 18-20. http://d.old.wanfangdata.com.cn/Periodical/zgcqzdzz201803006 [20] 邝彩红.早孕期胎儿颈项透明层增厚与不良妊娠结局关系的研究[J].中国实用医药, 2019, 14(11): 46-7. http://d.old.wanfangdata.com.cn/Periodical/zgsyyy201911025 -







 下载:
下载: