Evaluation value of calcitonin original and blood coagulation function for the prognosis of patients with sepsis
-
摘要:
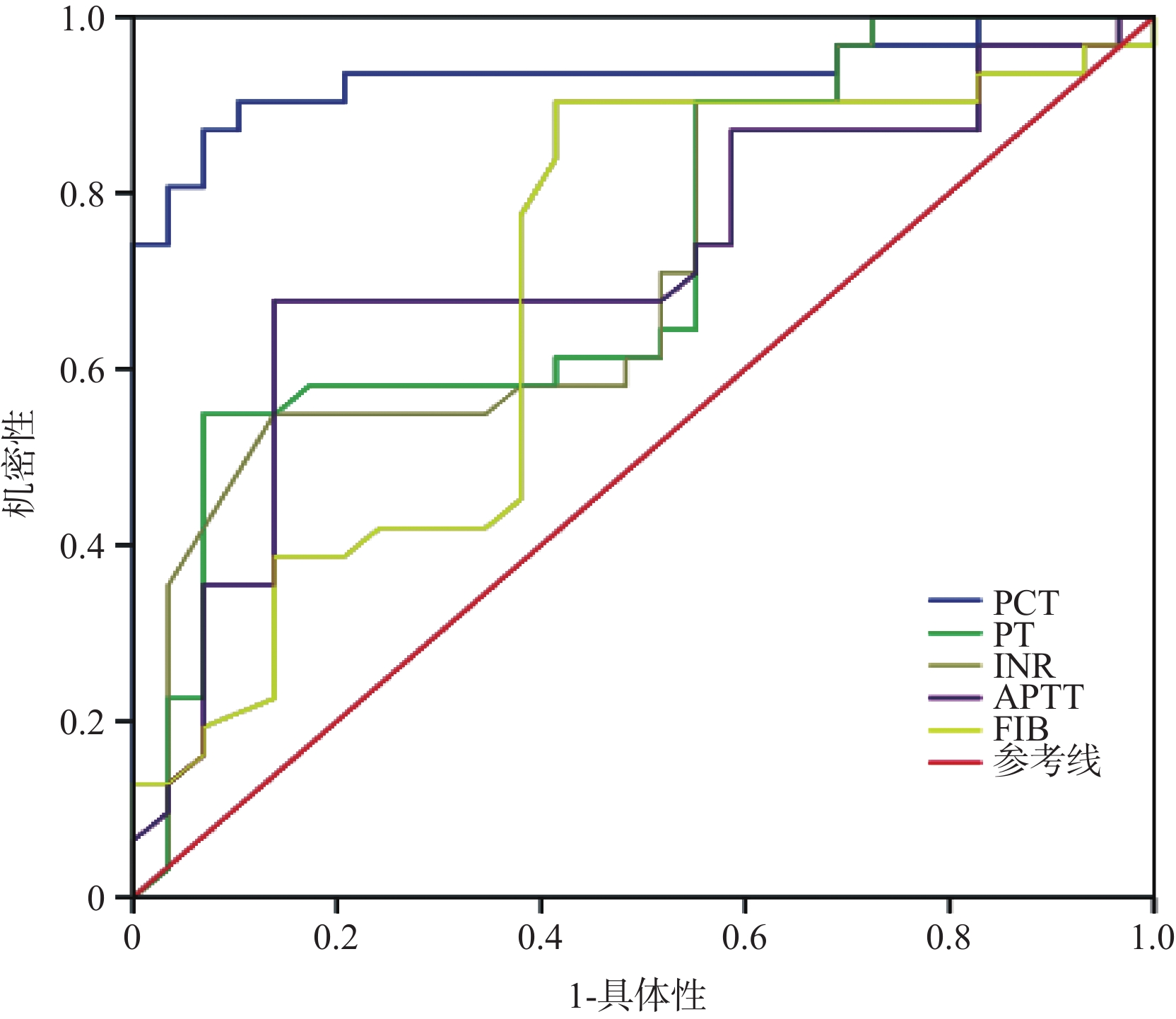
目的 探讨脓毒血症患者的凝血功能状况变化及降钙素原变化趋势与预后的相关性。 方法 选取本院2015年1月~2016年6月入住急诊ICU的脓毒血症患者作为研究对象,按照预后分为死亡组和存活组。分别检测两组患者血浆凝血酶原时间、活化部分凝血活酶时间、凝血酶时间、纤维蛋白原和血清降钙素原水平。 结果 死亡组的PCT和凝血功能水平均高于存活组(P<0.05),ROC曲线显示血清降钙素原最佳截断点为34.24时,曲线下面积(AUG)为93.4,敏感度87.1%,特异度93.1%;血浆凝血酶原时间最佳截断点为14.75时,AUG为72.5,敏感度54.8%,特异度93.1%;国际标准化比值最佳截断点为1.31时,AUG为72,敏感度48.4%,特异度89.7%;活化部分凝血活酶时间最佳截断点为39.20时,AUG为71.7,敏感度67.7%,特异度86.2%;Fbg最佳截断点为3.31时,AUG为90.3,敏感度58.6%,特异度93.1%。 结论 降钙素原和凝血功能与脓毒血症病情密切相关,可作为监测病情及预后的重要指标。 Abstract:Objective To investigate the blood coagulation function in patients with sepsis and the correlation of procalcitonin change trend with prognosis. Methods The patients with sepsis in emergency ICU of our hospital in January 2015-June 2016 were choosed as research object. Patients were divided into death group and alive group according to prognosis. Plasma prothrombin time (PT), activated partial clotting enzyme live time (APTT), thrombin time (TT), fibrinogen (FIB) and serum calcitonin (PCT) level of 2 groups were detected. Results The difference of 2 groups was significantly(P<0.05). ROC curve showed the best cut-off point of PCT was 34.24, with the area under the curve (AUG) of 93.4, sensitivity of 87.1%, specific degree of 93.1%; best cut-off point of PT was 14.75, with AUG of 72.5, sensitivity of 54.8%, the specific degree of 93.1%; best cut-off point of INR was 1.305, with AUG of 72, sensitivity of 48.4%, the specific degree of 89.7%; best cut-off point of APTT was 39.2, with AUG of 71.7, sensitivity of 67.7%, the specific degree of 86.2%; best cut-off point of Fbg was 3.315, with AUG of 90.3, sensitivity of 58.6% and specific degree of 93.1%. Conclusion Procalcitonin and blood coagulation function are closely related to the severity of sepsis. They can be used as an important index of disease monitoring and prognosis. -
Key words:
- procalcitonin /
- blood coagulation function /
- sepsis /
- prognosis
-
表 1 脓毒血症两组不同预后指标的比较(
$\, \overline{{x}}{{±}}{{s}}$ )分组 PCT(ng/mL) PT(s) INR APTT(s) TT(s) Fbg(g/L) 死亡组 76.9±27.3 18.2±14.2 1.5±1.3 45.5±15.8 14.7±5.8 3.4±1.3 存活组 15.7±10.7 10.9±12.5 0.9±1.1 34.0±12.2 13.9±6.1 4.06±5.8 P 0.000 0.003 0.003 0.004 0.069 0.012 PCT: 血清降钙素原; PT: 血浆凝血酶原时间; INR: 国际标准化比值; APTT: 活化部分凝血活酶时间; TT: 凝血酶时间; Fbg: 空腹血糖. 表 2 受试者ROC曲线在脓毒血症预测价值的比较(%)
分组 PCT(ng/mL) PT(s) INR APTT(s) TT(s) Fbg(g/L) 死亡组 76.9±27.3 18.2±14.2 1.5±1.3 45.5±15.8 14.7±5.8 3.4±1.3 存活组 15.7±10.7 10.9±12.5 0.9±1.1 34.0±12.2 13.9±6.1 4.06±5.8 P 0.000 0.003 0.003 0.004 0.069 0.012 PCT: 血清降钙素原; PT: 血浆凝血酶原时间; INR: 国际标准化比值; APTT: 活化部分凝血活酶时间; TT: 凝血酶时间; Fbg: 空腹血糖. -
[1] Salomao R, Brunialti MK, Rapozo MM, et al. Bacterial sensing, cell signaling, and modulation of the immune response during sepsis[J]. Shock, 2012, 38(3): 227-42. doi: 10.1097/SHK.0b013e318262c4b0 [2] Venkataraman R, Kellum JA. Sepsis: update in the management[J]. Adv Chronic Kidney Dis, 2013, 20(1): 6-13. doi: 10.1053/j.ackd.2012.10.013 [3] Lindvig KP, Henriksen DP, Nielsen SL, et al. How do bacteraemic patients present to the emergency department and what is the diagnostic validity of the clinical parameters; temperature, C-reactive protein and systemic inflammatory response syndrome?[J]. Scand J Trauma Resusc Emerg Med, 2014, 22(5): 39-42. [4] Wacker C, Prkno A, Brunkhorst FM, et al. Procalcitonin as a diagnostic marker for sepsis: a systematic review and meta-analysis[J]. Lancet Infect Dis, 2013, 13(5): 426-35. doi: 10.1016/S1473-3099(12)70323-7 [5] 田 虹, 王洪霞. 老年脓毒血症患者凝血功能紊乱及预后的关系[J]. 中国急救医学, 2014,45(11): 966-9. doi: 10.3969/j.issn.1002-1949.2014.11.03 [6] 陈 伟, 胡志华, 杨远征. 乌司他丁辅助高容量血液滤过对严重脓毒血症血清细胞黏附分子-1、胆碱酯酶和凝血功能的影响[J]. 中国现代医学杂志, 2016, 26(11): 54-8. doi: 10.3969/j.issn.1005-8982.2016.11.011 [7] Hofbauer B, Saluja AK, Bhatia M, et al. Effect of recombinant platelet-activating factor acetylhydrolase on two models of experimental acute pancreatitis[J]. Gastroenterology, 1998, 115(5): 1238-47. doi: 10.1016/S0016-5085(98)70096-4 [8] Glickman SW, Cairns CB, Otero RM, et al. Disease progression in hemodynamically stable patients presenting to the emergency department with sepsis[J]. Acad Emerg Med, 2010, 17(4): 383-90. doi: 10.1111/acem.2010.17.issue-4 [9] Charchaflieh J, Wei J, Labaze G, et al. The role of complement system in septic shock[J]. Clin Dev Immunol, 2012,13(2): 407324-6. [10] Liu B, Chen YX, Yin Q, et al. Diagnostic value and prognostic evaluation of Presepsin for sepsis in an emergency department[J]. Crit Care, 2013, 17(5): R244-7. doi: 10.1186/cc13070 [11] Lubberts E. IL-17/Th17 targeting: on the road to prevent chronic destructive arthritis[J]. Cytokine, 2008, 41(2): 84-91. doi: 10.1016/j.cyto.2007.09.014 [12] Ma HL, Liang S, Li J, et al. IL-22 is required for Th17 cell-mediated pathology in a mouse model of psoriasis-like skin inflammation[J]. J Clin Invest, 2008, 118(2): 597-607. [13] 武万良, 李风侠, 向 磊. 脓毒血症患儿的凝血功能监测[J]. 临床儿科杂志, 2010, 28(1): 24-5, 33. http://d.wanfangdata.com.cn/Periodical/lcekzz201001007 [14] Bloos F. Clinical diagnosis of sepsis and the combined use of biomarkers and culture- and non-culture-based assays[J]. Methods Mol Biol, 2015, 1237(8): 247-60. [15] Talebi-Taher M, Babazadeh S, Barati M, et al. Serum inflammatory markers in the elderly: are they useful in differentiating sepsis from SIRS[J]?. Acta Med Iran, 2014, 52(6): 438-42. [16] Boskabadi H, Maamouri G, Tavakol Afshari J, et al. Evaluation of serum interleukins-6, 8 and 10 levels as diagnostic markers of neonatal infection and possibility of mortality[J]. Iran J Basic Med Sci, 2013, 16(12): 1232-7. [17] Hegazy MA, Omar AS, Samir N, et al. Amalgamation of procalcitonin, C-reactive protein, and sequential organ failure scoring system in predicting sepsis survival[J]. Anesthesia, essays and researches, 2015, 8(3): 296-301. [18] 郑 超, 乔陈财, 陈 奕, 等. 菌血症患者细菌感染程度与血清PCT, hs-CRP水平变化研究[J]. 重庆医科大学学报, 2017, 42(2): 240-3. [19] 周 凯, 胡迎春. 脓毒血症患者血清降钙素原的变化及其预后意义[J]. 中国老年学杂志, 2016, 36(8): 1944-5. http://d.wanfangdata.com.cn/Periodical/zglnxzz201608072 [20] 杨志瑜, 夏 岳, 戚国庆, 等. 脓毒血症患者血清降钙素原与心肌肌钙蛋白I动态变化及临床意义[J]. 中华医院感染学杂志, 2016, 26(10): 2248-50. [21] 马 颖, 季 萍, 张朝霞, 等. 降钙素原与超敏C-反应蛋白和N端前体脑钠肽对脓毒症预后的评估价值[J]. 中华医院感染学杂志, 2016, 26(10): 2245-7. -






 下载:
下载: