Relationship between TSH level and prognosis of patients with thyrotropin-secreting pituitary adenoma
-
摘要:
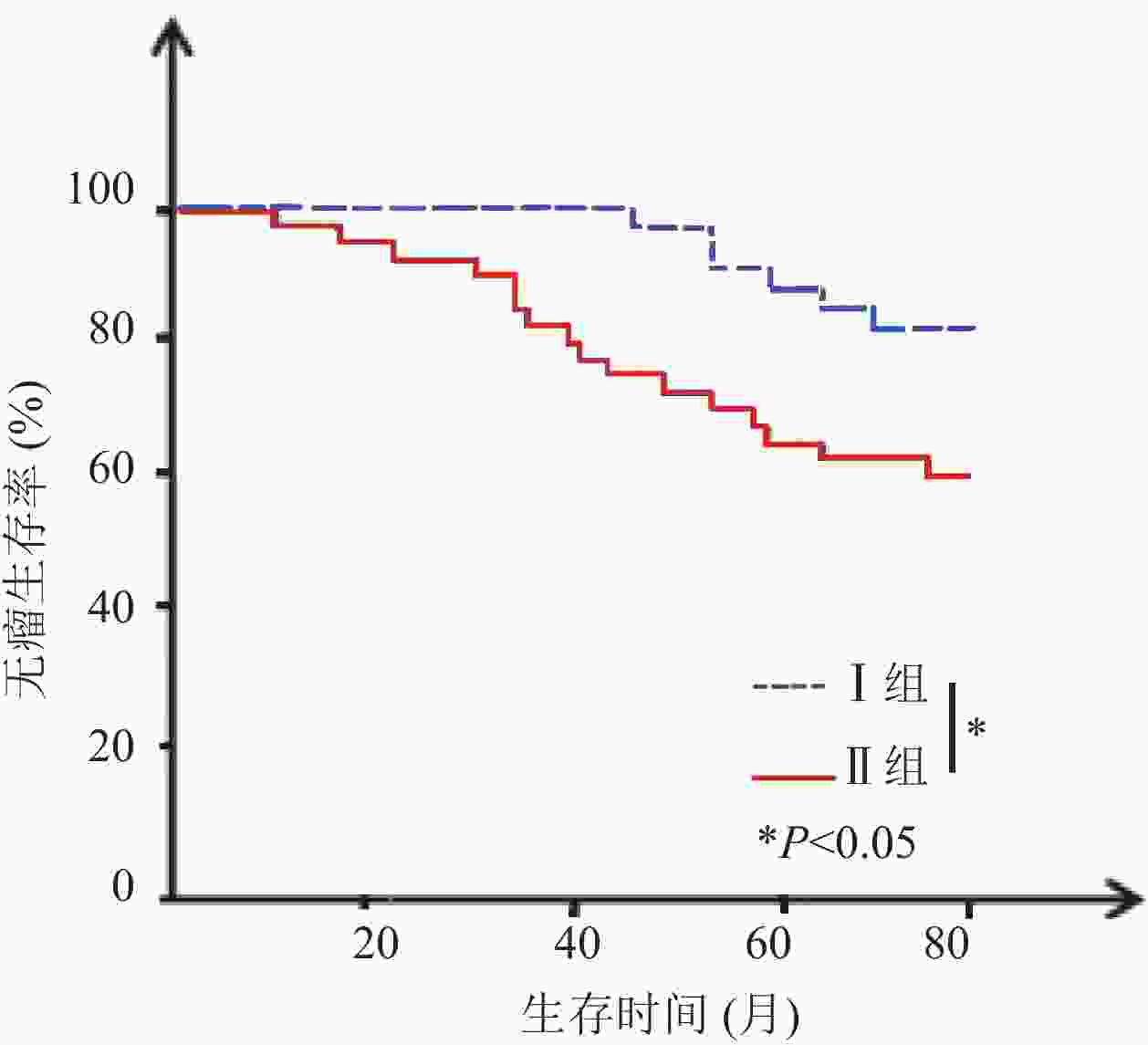
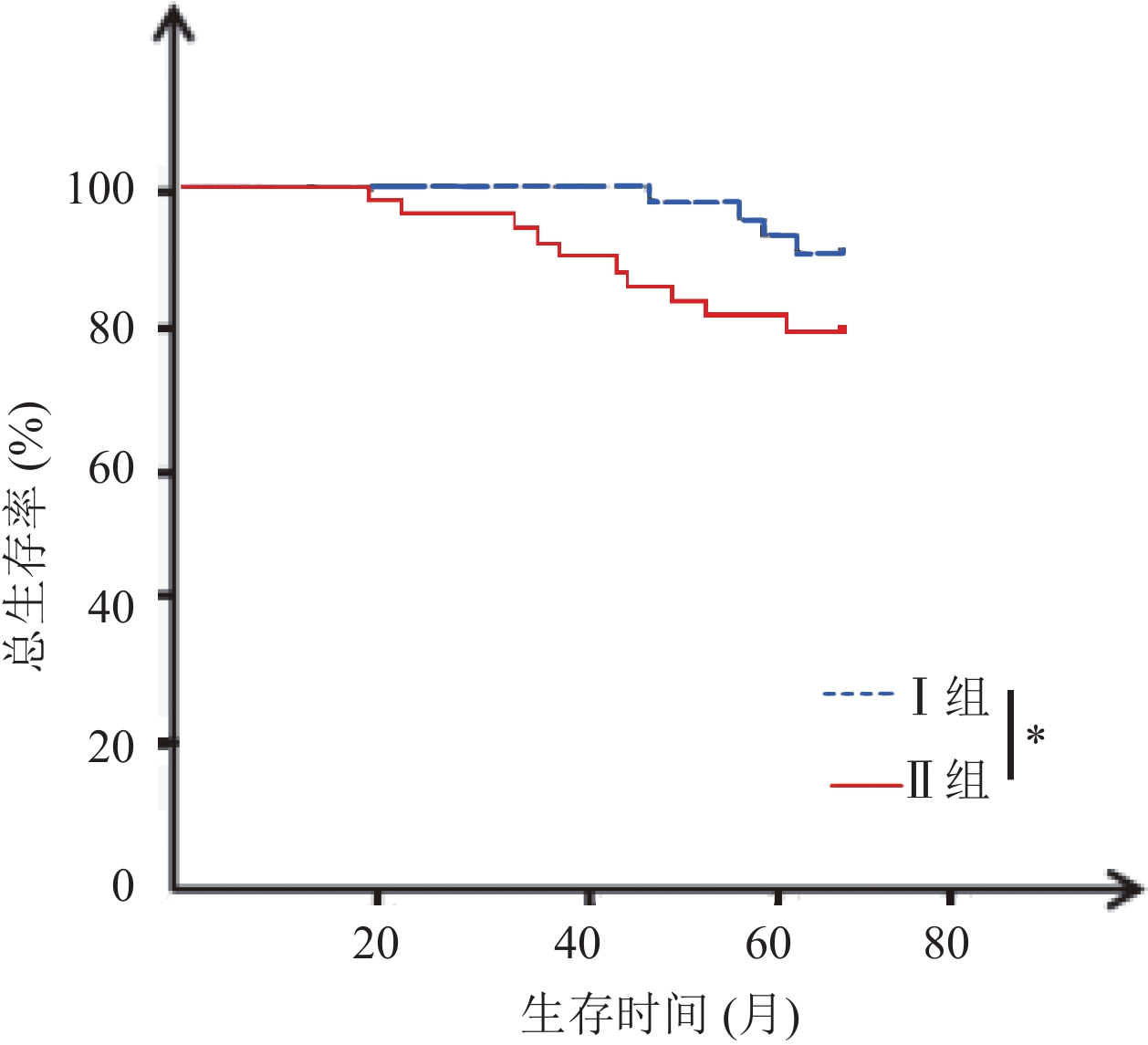
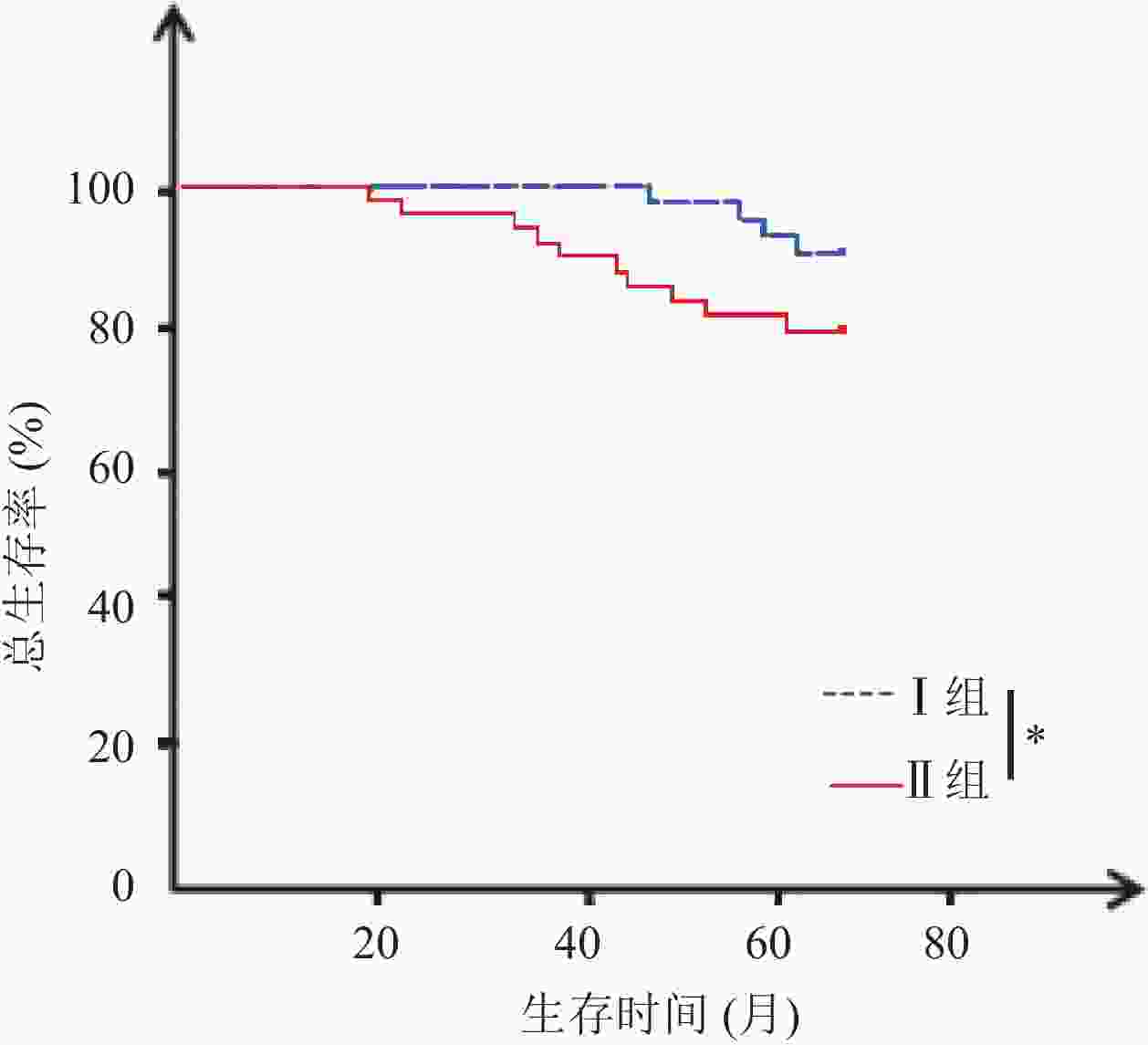
目的 分析促甲状腺激素(TSH)水平与垂体促甲状腺素腺瘤患者预后的关系。 方法 回顾性收集53例垂体促甲状腺素腺瘤患者的临床资料,各项检查后均进行常规治疗,治疗前1周内检测血清TSH水平,并根据TSH水平分为I组(n=20,TSH<2.5 mU/L)、Ⅱ组(n=33,TSH≥2.5 mU/L)。两组均进行至少5年期的随访(或至死亡终期),记录其无瘤生存和总生存情况。 结果 两组性别、年龄、肿瘤直径比较无统计学意义(P>0.05),但Ⅱ组淋巴结转移率高于I组(36.36% vs 10.00%,P<0.05),TNM分期中Ⅲ~Ⅳ期占比高于I组(57.58% vs 25.00%,P<0.05),且Ⅱ组治疗前三碘甲腺原氨酸、甲状腺素水平均高于I组,差异均有统计学意义(P<0.05)。截至2017年2月,Ⅱ组5年无瘤生存率和总生存率分别为48.48%、63.64%,低于I组80.00%、90.00%,差异有统计学意义(P<0.05)。Cox回归风险模型危险因素分析发现淋巴结转移、TNM分期及三碘甲腺原氨酸、甲状腺素、TSH水平为影响垂体促甲状腺素腺瘤患者治疗后5年生存率的独立影响因素(P<0.05)。 结论 高TSH水平与垂体促甲状腺素腺瘤患者预后不良有关,临床应积极采取对症措施调控患者TSH水平。 Abstract:Objective To explore the relationship between thyroid stimulating hormone (TSH) level and the prognosis of patients with thyrotropin-secreting pituitary adenoma. Methods The clinical data of 53 patients with thyrotropin-secreting pituitary adenoma were retrospectively analyzed. Patients were performed with routine treatment after examination. One week before treatment, serum TSH level was detected.According to TSH level, the patients were divided into group I (n=20, TSH level <2.5 mU/L) and group II (n=33, TSH level ≥ 2.5 mU/L). The two groups were followed up for at least 5 years (or till death). The tumor-free survival and total survival were recorded. Results There were no significant differences of gender, age and tumor size between the two groups (P>0.05). Rate of lymph node metastasis was significantly higher in group II than group I (36.36% vs 10.00%, P<0.05). Among all TNM stages, the proportion of stage III~IVwas significantly higher in group II than group I (57.58% vs 25.00%, P<0.05). Before treatment, levels of triiodothyronine (T3) and thyroxine (T4) were significantly higher in group II than group I (P<0.05). Till February 2017, the 5-year disease-free survival rate and overall survival rate of group II were significantly lower than those of group I (48.48% and 63.64% vs 80.00% and 90.00%, P<0.05). Cox regression risk model showed that lymph node metastasis, TNM stage, levels of T3, T4 and TSH were independent factors influencing the 5-year survival rate of patients with thyrotropin-secreting pituitary adenoma (P<0.05). Conclusion High TSH levels are associated with poor prognosis of patients with thyrotropin-secreting pituitary adenoma. Clinical measures should be taken to control the TSH level of patients. -
表 1 两组患者的临床一般资料与病理资料比较(n,
$\bar x \pm s$ )组别 女性(n,%) 年龄(岁) 肿瘤直径(cm) 淋巴结转移(n,%) TNM分期(I~Ⅱ/Ⅲ~Ⅳ期) I组(n=20) 14(70.00) 49.66±11.34 2.00±0.20 2(10.00) 15(75.00)/5(25.00) Ⅱ组(n=33) 22(66.67) 51.79±10.82 2.06±0.28 12(36.36) 14(42.42)/19(57.58) χ2/t 0.06 0.68 0.84 4.45 5.33 P 0.801 0.498 0.407 0.035 0.021 表 2 两组治疗前T3、T4水平比较(
$\bar x \pm s$ ,pmol/L)组别 T3 T4 I组(n=20) 2.26±0.72 7.41±1.42 Ⅱ组(n=33) 2.68±0.50 8.42±1.55 t 2.29 2.42 P 0.026 0.019 表 3 垂体促甲状腺素腺瘤患者预后的Cox回归分析
影响因素 Exp(B) 95%CI P 性别(女,男) 1.312 0.569~2.331 0.992 年龄(≥55岁和<55岁) 1.602 0.145~2.147 0.135 肿瘤直径(≥2 cm和<2 cm) 2.550 1.223~4.387 0.074 淋巴结转移(是,否) 3.164 2.012~6.321 0.001 TNM分期(I~Ⅱ期,Ⅲ~Ⅳ期) 3.027 1.226~5.430 0.019 T3(≥2.5 pmol/L和<2.5 pmol/L) 3.271 1.096~6.210 0.001 T4(≥7.2 pmol/L和<7.2 pmol/L) 3.450 3.471~6.996 0.001 TSH(≥2.5 mU/L和<2.5 mU/L) 4.270 1.174~7.393 0.000 -
[1] 国垂体腺瘤协作组. 中国垂体腺瘤外科治疗专家共识[J]. 中华医学杂志, 2015, 95(5): 1324-9. http://www.cnki.com.cn/Article/CJFDTOTAL-QKYL201703002.htm [2] 岳志远, 张韶君. 垂体促甲状腺素腺瘤的研究进展[J]. 中国现代医生, 2016, 54(33): 165-8. http://www.cnki.com.cn/Article/CJFDTOTAL-ZDYS201633050.htm [3] 姜晓华, 蔡 洁, 王卫庆, 等. 垂体促甲状腺素瘤的临床特点与诊治分析[J]. 中华内分泌代谢杂志, 2012, 28(9): 729-33. http://cpfd.cnki.com.cn/Article/CPFDTOTAL-ZHYX201208002234.htm [4] 杜立平. 促甲状腺激素TSH受体基因突变同侵袭性垂体瘤的相关性研究[J]. 国际检验医学杂志, 2013, 34(8): 921-2. http://www.cnki.com.cn/Article/CJFDTOTAL-GWSQ201308006.htm [5] 姜 艳, 顾 锋, 朱惠娟, 等. 分泌促甲状腺素及生长激素的垂体混合瘤临床特点及诊疗分析[J]. 中国实用内科杂志, 2016, 36(7): 567-9. http://www.cnki.com.cn/Article/CJFDTOTAL-SYNK201607011.htm [6] 王璐璐. 内分泌激素水平监测对生长激素型垂体腺瘤患者手术远期疗效的研究[J]. 中国医药指南, 2017, 15(9): 132-3. http://www.cnki.com.cn/Article/CJFDTOTAL-YYXK201709110.htm [7] 唐 鲲, 时立新, 严 征. 甲状腺结节良恶性与术前血清促甲状腺素间的关系研究(附1553例报告)[J]. 贵州医药, 2015, 39(7): 619-20. http://www.cnki.com.cn/Article/CJFDTOTAL-GZYI201507018.htm [8] 赵苇苇, 杨叶虹, 叶红英, 等. 垂体促甲状腺素分泌瘤20例临床分析[J]. 中华内科杂志, 2014, 53(1): 19-22. http://cpfd.cnki.com.cn/Article/CPFDTOTAL-ZHYX201308001A4E.htm [9] 张国军, 吕 虹, 马瑞敏, 等. 多激素平行测定法的建立及其在垂体腺瘤筛查中的初步研究[J]. 中华临床医师杂志:电子版, 2013, 9(7): 2918-22. http://www.cnki.com.cn/Article/CJFDTOTAL-ZLYD201307043.htm [10] 陈东栋, 黄擎擎, 吴建东, 等. 垂体促甲状腺激素腺瘤的诊断和治疗[J]. 中华神经外科疾病研究杂志, 2015, 14(5): 441-3. http://www.cnki.com.cn/Article/CJFDTOTAL-SJWK201505017.htm [11] 李洁茹, 白 斌, 曹 娟, 等. 老年急性缺血性脑卒中患者下丘脑腺垂体激素水平与预后相关性分析[J]. 山西医药杂志, 2014, 43(14): 1611-4. http://www.cnki.com.cn/Article/CJFDTOTAL-SXYY201414001.htm [12] 马飞国, 王红军. 甲状腺乳头状癌颈侧区淋巴结转移与血清促甲状腺激素的相关关系研究[J]. 中华普外科手术学杂志电子版, 2015, 9(6): 59-60. http://www.cnki.com.cn/Article/CJFDTOTAL-ZHPW201506024.htm [13] Rinaldi S, Plummer M, Biessy C, et al. Thyroid-stimulating hormone, thyroglobulin, and thyroid hormones and risk of differentiated thyroid carcinoma: the EPIC study[J]. J Natl Cancer Inst, 2014, 106(6): 97-100. [14] 曾剑锋, 杨跃超, 郭 红, 等. 新疆昌吉回族自治州结节性甲状腺肿术后血清促甲状腺素水平与复发关系的研究[J]. 重庆医科大学学报, 2013, 38(5): 554-7. http://www.cnki.com.cn/Article/CJFDTOTAL-ZQYK201305023.htm [15] 叶文春, 方向明, 王玉容, 等. 亚临床甲状腺功能减退症患者促甲状腺素水平与血脂的关系研究[J]. 华西医学, 2015, 30(5): 846-9. doi: 10.7507/1002-0179.20150244 [16] 滕晓春, 金 婷, 王冉冉, 等. 一例TRβ基因P453 T突变所致的甲状腺激素抵抗综合征合并垂体TSH微腺瘤的病例报告[J]. 中华内分泌代谢杂志, 2016, 32(1): 19-23. [17] 凌 南, 李向东, 惠国桢, 等. 垂体促甲状腺素腺瘤的诊断和处理[J]. 江苏医药, 2012, 38(16): 1896-8. http://www.cnki.com.cn/Article/CJFDTOTAL-YIYA201216014.htm [18] Kuzu F, Bayraktaroğlu T, Zor F, et al. A thyrotropin-secreting macroadenoma with positive growth hormone and prolactin immunostaining: A case report and literature review[J]. Niger J Clin Pract, 2015, 18(5): 693-7. doi: 10.4103/1119-3077.158983 [19] 杨莹莹, 刘 浩, 胡 嫒, 等. 甲状腺素检测在垂体促甲状腺激素腺瘤术后随访中的意义[J]. 中华医学杂志, 2016, 96(47): 3825-8. doi: 10.3760/cma.j.issn.0376-2491.2016.47.012 [20] 李 杰, 张 博, 白 杨, 等. 血清甲状腺球蛋白及促甲状腺素在分化型甲状腺癌预后判断中的意义[J]. 临床外科杂志, 2016, 24(3): 193-6. http://www.cnki.com.cn/Article/CJFDTOTAL-LCWK201603017.htm [21] 岳增文, 刘进忠, 朱宝玉, 等. 转酮醇酶样蛋白1在舌鳞状细胞癌中的表达及意义[J]. 口腔疾病防治, 2016, 24(3): 150-3. -






 下载:
下载: