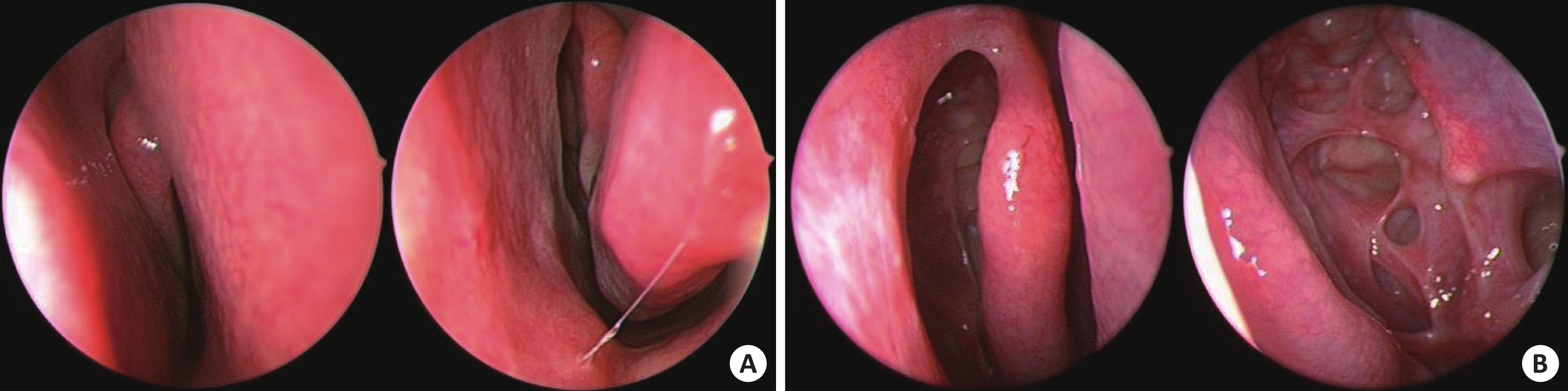
Effect of nasal dilation on the subjective and objective symptoms of sleep in patients with OSAHS
-
摘要:
目的 探讨鼻腔扩容术对阻塞型睡眠呼吸暂停低通气综合征(OSAHS)患者睡眠主客观症状的影响,为鼻腔扩容术在OSAHS中应用提供临床依据。 方法 选择56例于我院耳鼻咽喉科行鼻腔扩容术的OSAHS患者为研究对象,比较患者手术前后的多导睡眠监测结果与鼻堵量表、嗜睡量表及鼾声量表评分。 结果 鼻腔扩容术后OSAHS患者睡眠呼吸暂停低通气指数较术前降低(12.3±4.0 vs 6.3±1.7,P<0.05),平均血氧饱和度(80.6%±11.3% vs 88.1%±14.4%)以及最低血氧饱和度(71.2%±10.7%vs 79.8%±13.5%)均增加(P<0.05);鼾声量表评分(5.7±1.6分 vs 3.2±0.7分)、鼻堵量表评分(8.9±2.0分 vs 2.8±0.7分)及嗜睡量表量表评分(12.1±2.7分 vs 5.6±1.5分)较术前下降(P<0.05)。 结论 鼻腔扩容术在缓解OSAHS患者阻塞性睡眠呼吸暂停的严重程度及改善OSAHS患者睡眠打鼾、鼻堵及白天嗜睡症状方面效果明显,对OSAHS患者的治疗有重要临床意义。 -
关键词:
- 睡眠呼吸暂停低通气综合征 /
- 鼻腔扩容术 /
- 睡眠主客观症状
Abstract:Objective To explore the effect of nasal dilation on the subjective and objective symptoms of sleep in patients with obstructive sleep apnea hypopnea syndrome (OSAHS), and provide clinical basis for the application of nasal cavity expansion in patients with OSAHS. Methods Fifty-six cases adult patients with OSAHS were chosen as objects. The nasal resistance, the results of multiple sleep monitoring (PSG), the snore outcome survey (SOS), the visual analogue scale (VAS) and the epworth sleepy survey (ESS) were compared before and after nasal surgery expansion. Results After nasal dilation, the nasal resistance and apnea hypopnea index (AHI) of OSAHS patients were decreased significantly (P<0.05).The average oxygen saturation and the lowest oxygen saturation were increased significantly (P<0.05). Scores of SOS scale, VAS scale and ESS scale which reflecting the sleep subjective symptoms were decreased significantly (P<0.05). Conclusion Nasal dilation has a curative effect on reducing nasal resistance and alleviating the severity of obstructive sleep apnea in OSAHS patients.It improves sleep subjective symptoms such as sleep snoring nasal blockage and daytime sleepiness. It is significant in the treatment of patients with OSAHS. -
表 1 患者一般资料(
$\bar x \pm s$ )分组 例数 年龄(岁) 术前BMI(kg/m2) 术后BMI(kg/m2) 男性 39 46.7±11.9 29.72±2.97 28.41±3.02* 女性 17 51.3±7.6 28.68±2.87 28.39±3.14* 全部 56 48.1±11.2 29.40±2.94 28.40±3.07* *P>0.05vs术前BMI. 表 2 手术前后患者PSG监测结果比较(
$\bar x \pm s$ )监测时间 最低血氧饱和度(%) 平均血氧饱和度(%) AHI指数(次/h) 术前 71.2±10.7 80.6±11.3 12.3±4.0 术后6月 79.8±13.5 88.1±14.4 6.3±1.7 t –3.736 –3.006 10.331 P <0.05 <0.05 <0.05 表 3 手术前后患者睡眠主观症状的比较(
$\bar x \pm s$ ,分)监测时间 嗜睡量表 鼻堵量表 打鼾量表 术前 12.1±2.7 8.9±2.0 5.7±1.6 术后6月 5.6±1.5 2.8±0.7 3.2±0.7 t 15.748 21.543 10.712 P <0.05 <0.05 <0.05 -
[1] Stone KL, Blackwell TL, Ancoli IS, et al. Sleep disordered breathing and risk of stroke in older Community-Dwelling men[J]. Sleep, 2016, 39(3): 531-40. doi: 10.5665/sleep.5520 [2] 中华医学会呼吸病学分会睡眠呼吸障碍学组. 阻塞性睡眠呼吸暂停低通气综合征诊治指南(2011年修订版)[J]. 中华结核和呼吸杂志, 2012, 35(1): 9-12. http://cpfd.cnki.com.cn/Article/CPFDTOTAL-OGSF201508002009.htm [3] Koo D, Nam H. Association between obstructive sleep apnea syndrome and cerebral microbleeds in patients with ischemic stroke[J]. Sleep Med, 2015, 16(5): S361-4. [4] Roest AM, Carney RM, Stein PK, et al. Obstructive sleep apnea/hypopnea syndrome and poor response to sertraline in patients with coronary heart disease[J]. J Clin Psychiatry, 2012, 73(1): 31-6. doi: 10.4088/JCP.10m06455 [5] Pérez-Rico C, Gutiérrez-Díaz E, Mencía-Gutiérrez E, et al. Obstructive sleep apnea-hypopnea syndrome (OSAHS) and glaucomatous optic neuropathy[J]. Graefes Arch Clin Exp Ophthalmol, 2014, 252(9): 1345-57. doi: 10.1007/s00417-014-2669-4 [6] 张庆翔, 刘宏刚, 王云丽, 等. 鼻腔扩容术治疗轻中度阻塞性睡眠呼吸暂停低通气综合征的疗效分析[J]. 中国中西医结合耳鼻咽喉科杂志, 2015, 23(2): 115-7. http://www.cnki.com.cn/Article/CJFDTOTAL-XYJH201502011.htm [7] 彭莉莉, 李进让, 孙建军, 等. Epworth嗜睡量表简体中文版信度和效度评价[J]. 中华耳鼻咽喉头颈外科杂志, 2011, 46(1): 44-9. http://cdmd.cnki.com.cn/Article/CDMD-12121-1016266530.htm [8] 王学艳, 任华丽, 石海云, 等. 变应性鼻炎症状评分及视觉模拟量表适用性比较[J]. 中国耳鼻咽喉头颈外科, 2012, 19(11): 609-11. http://www.cnki.com.cn/Article/CJFDTOTAL-EBYT201211010.htm [9] 吴瑞珊, 王佳蓉, 陈翊民. 鼻外科手术联合上气道射频消融术用于阻塞性睡眠呼吸暂停低通气综合征伴慢性鼻塞患者治疗的疗效分析[J]. 重庆医科大学学报, 2015, 13(1): 112-5. http://www.cnki.com.cn/Article/CJFDTOTAL-ZQYK201501025.htm [10] Lacedonia D, Carpagnano GE, Sabato R, et al. Characterization of obstructive sleep apnea-hypopnea syndrome (OSA) population by means of cluster analysis[J]. J Sleep Res, 2016, 25(6): 724-30. doi: 10.1111/jsr.12429 [11] 张 庆, 王京娜, 何权瀛, 等. 阻塞性睡眠呼吸暂停低通气综合征对心血管系统的影响[J]. 医学与哲学, 2013, 34(10): 7-9. http://www.cnki.com.cn/Article/CJFDTOTAL-JLYX201610006.htm [12] 赵化庭, 戴海龙, 光雪峰. 阻塞性睡眠呼吸暂停低通气综合征与高血压关系的研究进展[J]. 中国心血管病研究, 2015, 13(1): 5-7. http://www.cnki.com.cn/Article/CJFDTOTAL-DDYI201021011.htm [13] 侯微微, 刘 双, 张 蔚. 阻塞性睡眠呼吸暂停低通气综合征对肺血栓栓塞症的影响[J]. 中国医药, 2014, 9(10): 1567-8. doi: 10.3760/cma.j.issn.1673-4777.2014.10.048 [14] 陈 婷. 阻塞性睡眠呼吸暂停低通气综合征并Ⅱ型呼吸衰竭6例分析[J]. 临床合理用药杂志, 2014, 20(7): 134-5. http://www.cnki.com.cn/Article/CJFDTOTAL-ZGSQ201002069.htm [15] Yaggi HK, Strohl KP. Adult obstructive sleep apnea/hypopnea syndrome: definitions, risk factors, and pathogenesis[J]. Clin Chest Med, 2010, 31(2): 179-86. doi: 10.1016/j.ccm.2010.02.011 [16] 周 敬, 鲁沈源, 励雯静, 等. 148例鼾症及阻塞性睡眠呼吸暂停低通气综合征危险因素的分析[J]. 复旦学报: 医学版, 2010, 37(2): 207-10. http://www.cnki.com.cn/Article/CJFDTOTAL-SHYK201002019.htm [17] Moret BV, Alvarez-Estévez D, Fernández-Leal A, et al. Intelligent approach for analysis of respiratory signals and Oxygen saturation in the sleep apnea/hypopnea syndrome[J]. Open Med Inform J, 2014, 8(12): 1-19. [18] 惠培林, 谢宇平, 马 薇, 等. 鼻腔扩容术作为基础术式在治疗OSAHS中的临床价值分析[J]. 临床耳鼻咽喉头颈外科杂志, 2015, 17(21): 1860-3. http://www.cnki.com.cn/Article/CJFDTOTAL-LCEH201521005.htm [19] Li HY, Wang PC, Chen YP, et al. Critical appraisal and meta-analysis of nasal surgery for obstructive sleep apnea[J]. Am J Rhinol Allergy, 2011, 25(1): 45-9. doi: 10.2500/ajra.2011.25.3558 [20] 彭易坤, 胡德峰, 吴欣华, 等. 阻塞性睡眠呼吸暂停低通气综合征患者双侧鼻腔扩容术前后鼻腔通气程度主客观的变化[J]. 武汉大学学报: 医学版, 2015, 36(6): 952-5. http://www.cnki.com.cn/Article/CJFDTOTAL-HBYK201506026.htm -







 下载:
下载: