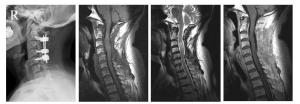
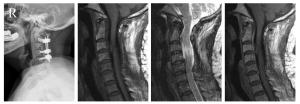
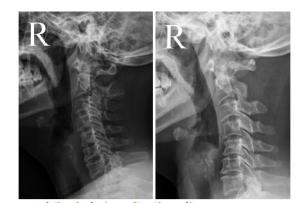
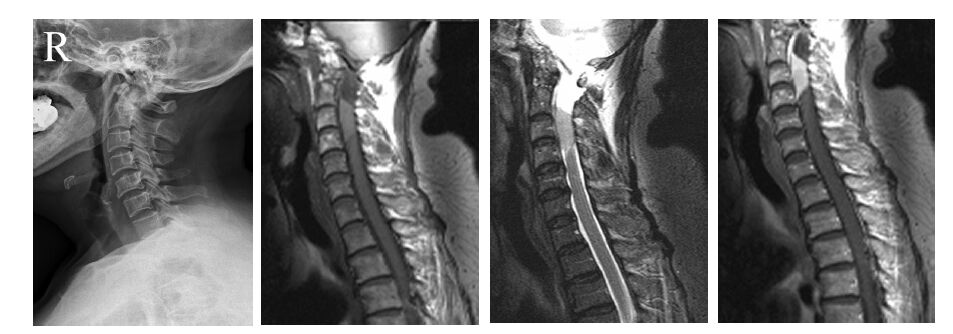
Surgical treatment of 27 cervical intraspinal tumor
-
摘要:
目的探讨颈椎椎管内肿瘤的外科治疗方法及内固定对其临床疗效的影响。 方法回顾分析27例我院脊柱骨科与神经外科2011年1月~2014年12月收治的颈椎椎管内肿瘤临床资料,13例行肿瘤切除及内固定手术(内固定组),14行单纯肿瘤切除手术(无内固定组)。两组患者性别、年龄及病程比较,差异均无统计学意义(P>0.05)。分别于术前和术后随访时按日本骨科协会(JOA)颈椎疗效评定标准17分评分法对患者进行疗效评估,并复查颈椎X线平片及颈椎MRI,了解手术对颈椎椎管内肿瘤的治疗效果及内固定对其的影响。 结果所有患者均行外科手术切除肿瘤,术后1~56个月随访,平均29.7个月,除2例复发外,其余患者术后根性痛、感觉障碍、运动障碍及反射异常较术前明显改善,JOA评分由术前11.7分升高至末次随访时14.9分(P < 0.05)。两组患者术前及末次随访时JOA评分改善率比较差异均无统计学意义(P>0.05)。未行内固定治疗的患者术后有出现鹅颈畸形的现象。 结论无论是否行内固定,颈椎椎管内肿瘤手术治疗可以取得较好的临床效果。 Abstract:ObjectiveTo investigate the surgical treatment of cervical intraspinal tumor and the influence of instrumentation. MethodsA total of 27 patients with cervical intraspinal tumor surgically treated from January 2011 to December 2014 were retrospectively analyzed. Patients were divided into the internal fixation group (13 cases) and the simple tumor resection group (14 cases). No significant differences were found in gender, age, disease duration between 2 groups (P>0.05). JOA score was analyzed before and after operation, the cervical spine radiographs and MR images were recorded. ResultsAll tumors in the 27 patients were primarily removed. The follow-up time ranged from 1 to 56 months with an average of 29.7 months. Radicular pain, sensory disturbances, movement disorders and altered reflexes were significantly improved, JOA score increased from 11.7 points preoperatively to 14.9 points at the end of the follow-up (P < 0.05). No significant difference was found in JOA score improvement rate between 2groups (P>0.05). In the simple tumor resection group, 2 cases appeared recurvation deformity in cervical spine. ConclusionSurgical treatment can achieve good clinical efficacy in the treatment of cervical intraspinal tumor with or without fixation. -
Key words:
- cervical spine /
- intraspinal tumor /
- JOA score /
- surgical treatment
-
表 1 两组患者手术情况及JOA评分比较
组别 n 手术时间(min) 出血量(mL) JOA评分 改善率(%) 术前 术后3个月 末次随访 内固定组 13 294.9±90.8# 442.3±309.5* 12.2±3.6* 14.4±2.4* 14.9±3.3* 66.7±38.9* 无内固定组 14 219.7±76.8 323.6±287.0 11.3±4.1 13.6±3.0 14.9±2.7 70.6±27.4 #P<0.05 vs 无内固定组; *P>0.05 vs 无内固定组. -
[1] 谢京城, 王振宇, 马长城, 等. 660例椎管内肿瘤的手术治疗[J]. 中国微创外科杂志, 2009, 9(10): 940-5. http://www.cnki.com.cn/Article/CJFDTOTAL-ZWWK200910033.htm [2] 杨树源, 洪国良. 椎管内肿瘤402例报告[J]. 中华神经外科杂志, 2000,16(3): 162-5. http://www.cnki.com.cn/Article/CJFDTOTAL-ZHSW200003014.htm [3] Fujiwara A, Kobayashi N, Saiki K, et al. Association of the Japanese orthopaedic association score with the oswestry disability index, Roland-Morris disability questionnaire, and short-form 36[J].Spine, 2003, 28(14): 1601-7. http://cn.bing.com/academic/profile?id=9c164b29208dea0149326f0546db4c67&encoded=0&v=paper_preview&mkt=zh-cn [4] Hamamoto Y, Kataoka M, Senba T, et al. Vertebral metastases with high risk of symptomatic malignant spinal cord compression[J]. Jpn J Clin Oncol, 2009, 39(7): 431-4. doi: 10.1093/jjco/hyp039 [5] Mechtler LL, Nandigam K. Spinal cord tumors new views and future directions[J]. Neurol Clin, 2013, 31(1): 241-5. doi: 10.1016/j.ncl.2012.09.011 [6] 赵建华, 刘鹏. 骨科与神经外科交界的专科:脊柱脊髓外科-现状与进展[J]. 局解手术学杂志, 2014, 06(6): 575-7. http://www.cnki.com.cn/Article/CJFDTOTAL-JJXZ201406001.htm [7] 菅凤增, 方铁. 美国神经脊柱外科高速发展带给我们的启示[J]. 中华神经外科疾病研究杂志, 2015, 14(1): 1-3. http://www.cnki.com.cn/Article/CJFDTOTAL-SJWK201501001.htm [8] 王跃龙, 黄思庆. 不同术式切除椎管内肿瘤对脊柱稳定性的影响[J].中华神经外科杂志, 2013, 29(3): 313-5. http://cn.bing.com/academic/search?q=%e4%b8%ad%e5%8d%8e%e7%a5%9e%e7%bb%8f%e5%a4%96%e7%a7%91%e6%9d%82%e5%bf%97&FORM=AJOUR [9] Katsumi Y, Honma T, Nakamura T. Analysis of cervical instability resulting from laminectomies for removal of spinal cord tumor[J].Spine, 1989, 14(11): 1171-6. doi: 10.1097/00007632-198911000-00007 [10] Sciubba DM, Chaichana KL, Woodworth GF, et al. Factors associated with cervical instability requiring fusion after cervical laminectomy for intradural tumor resection[J]. J Neurosurg Spine, 2008, 8(5): 413-9. doi: 10.3171/SPI/2008/8/5/413 [11] 林国中, 王振宇, 谢京城, 等. 颈椎椎板切除术后稳定性研究[J]. 北京医学, 2010, 32(5): 336-40. http://www.cnki.com.cn/Article/CJFDTOTAL-BJYX201005003.htm [12] Cusick JF, Yoganandan N, Pintar F, et al. Biomechanics of cervical spine facetectomy and fixation techniques[J]. Spine, 1988, 7(13):808-12. http://cn.bing.com/academic/profile?id=150196578b4b162255ed3dc4e96a2026&encoded=0&v=paper_preview&mkt=zh-cn [13] 郭功亮, 齐兵, 曲阳, 等. 关节突关节切除范围对下颈椎稳定性影响的生物力学研究[J]. 生物医学工程研究, 2010, 29(4): 259-62, 267. http://www.cnki.com.cn/Article/CJFDTOTAL-SDSG201004013.htm [14] Geng XP, Wang X, Meng T, et al. The influence of posterior approach cervical intraspinal tumor resection on the stability of cervical vertebra[J]. J Biol Reg Homeos Ag, 2015, 2(11): 389-94. http://cn.bing.com/academic/profile?id=e30ad71d3a5d0c1577475b35110141fb&encoded=0&v=paper_preview&mkt=zh-cn [15] Merboth MK, Barnason S. Managing pain:the fifth vital sign[J].Nurs Clin North Am, 2000, 2(8): 375-83. http://cn.bing.com/academic/profile?id=b7e1ff21c4af4edf1ae3a92725ff2986&encoded=0&v=paper_preview&mkt=zh-cn [16] Halvorsen CM, Ronning P, Hald JA, et al. The long-term outcome after resection of intraspinal nerve sheath tumors: report of 131 consecutive cases[J]. Neurosurgery, 2015, 77(4): 585-92. doi: 10.1227/NEU.0000000000000890 [17] 于佶, 徐启武, 闻金坤. 椎管内肿瘤术后复发的原因及治疗[J]. 中国脊柱脊髓杂志, 2001, 11(1): 26-8. http://www.cnki.com.cn/Article/CJFDTOTAL-ZJZS200101009.htm -






 下载:
下载: