-
摘要:
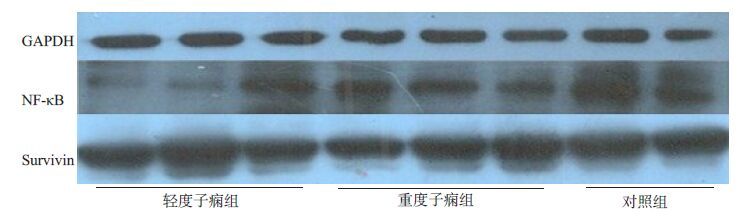
目的通过检测不同程度的妊娠高血压孕妇与正常妊娠孕妇胎盘组织中hTERT及NF-κB、survivin的表达,探索妊娠高血压的发病机制 方法选取2013~2014年的在我院分娩的孕妇为研究对象,共计90例,其中正常孕妇30例,足月轻度子痫前期孕妇30例,足月重度子痫前期孕妇30例,采用定量实时RT-PCR的方法检测胎盘中hTERT mRNA的水平,采用Westernblot对NF-κB、survivin表达量的细胞进行定量分析。 结果与正常孕妇的胎盘组织相比,hTERTmRNA在足月重度子痫前期和足月轻度子痫前期的胎盘组织的表达均显著上升,差异有统计学意义(P<0.05);与正常孕妇的胎盘组织相比,NF-κB、survivin在重度子痫前期胎盘的表达显著降低,而轻度子痫前期孕妇的胎盘组织Survivin的表达显著降低,差异有统计学意义(P<0.05);在重度子痫前期胎盘组织中,hTERTmRNA与NF-κB和Survivin的表达呈负相关系数分别为R1=-0.793,R2=-0.827,P<0.05。 结论对于轻度子痫和重度子痫的病人,hTERTmRNA表达均显著上升、NF-κB和Survivin 的表达均不同程度的下降,推测hTERT及NF-κB和survivin的表达与妊娠高血压的发病过程有密切关系。 -
表 1 孕妇一般资料(n=30)
组别 年龄 分娩孕周(d) BMI 正常孕妇组 27.3±3.2 278.6±7.5 26.3±2.1 足月轻度子痫组 28.7±2.7 269.4±6.7 27.3±1.7 足月重度子痫组 28.5±2.9 272.1±6.3 28.1±2.3 表 2 三组孕妇hTERT mRNA、NF-κB和survivin的表达量(n=30)
组别 hTERT mRNA表达量 NF-κB表达量 Survivin的表达量 正常孕妇组 37.65±10.54 109.37±17.73 302.34±54.23 足月轻度子痫组 43.23±9.87* 78.33±13.54* 253.54±37.41* 足月重度子痫组 56.91±12.20* 66.70±12.11* 199.53±29.37** *代表与正常孕妇相比,差异有统计学意义;*代表与足月轻度子痫组相比差异有统计学意义. -
[1] Levine RJ, Thadhani R, Qian C, et al. Urinary placental growth factor and risk of preeclampsia[J]. JAMA, 2005, 293(1): 77-85. doi: 10.1001/jama.293.1.77 [2] Duckitt K, Harrington D. Risk factors for pre-eclampsia at antenatal booking: systematic review of controlled studies[J]. Br Med J, 2005, 330: 565. doi: 10.1136/bmj.38380.674340.E0 [3] Dekker GA, Sibai BM. Etiologyand pathogenesis of preeclampsia: current concepts[J]. Am J Obstet Gynecol, 1998(179): 1359-1375. [4] Harley CB, Futcher AB, Greider CW. Telomeres shorten during ageing of human fibroblasts[J]. Nature, 1990, 345(6274): 458-60. doi: 10.1038/345458a0 [5] Aviv A. Chronology versus biology: telomeres, essential hypertension, and vascular aging[J]. Hypertension, 2002, 40(3): 229-32. doi: 10.1161/01.HYP.0000027280.91984.1B [6] Samani NJ, Boultby R, Butler R, et al. Telomere shortening in athero-sclerosis[J]. Lancet, 2001(358): 472-473. [7] Nakayama J, Tahara H, Tahara E, et al. Telomerase activation by hTRT in human normal fibroblasts and hepatocellular carcinomas [J]. Nat Genet, 1998, 18(1): 65-8. doi: 10.1038/ng0198-65 [8] Takakura M, Kyo S, Kanaya T, et al. Expression of human telomerase subunits and correlation with telomerase activity in cervical Cancer[J]. Cancer Res, 1998, 58(7): 1558-61. [9] Didonato JA, Mercurio F, Karin M. NF-κB and the Link between inflammation and Cancer[J]. Immunol Rev, 2012, 246(1): 379-400. doi: 10.1111/j.1600-065X.2012.01099.x [10] Altieri DC. Survivin in apoptosis control and cell cycle regulation in Cancer[J]. Prog Cell Cycle Res, 2003, 5(5): 447-52. https://www.ncbi.nlm.nih.gov/pubmed/14593739 [11] Molvi SN, Mir S, Rana VS, et al. Role of antihypertensive therapy in mild to moderate pregnancy-induced hypertension: a prospective randomized study comparing labetalol with alpha methyldopa[J]. Arch Gynecol Obstet, 2012, 285(6): 1553-62. doi: 10.1007/s00404-011-2205-2 [12] Chang S, Khoo CM, Naylor ML, et al. Telomere-based crisis: functional differences between telomerase activation and ALT in tumor progression[J]. Genes Dev, 2003, 17(1): 88-100. doi: 10.1101/gad.1029903 [13] Marzioni D, Capparuccia L, Todros T, et al. Growth factors and their receptors: fundamental molecules for human placental development [J]. Ital J Anat Embryol, 2005, 110(2 Suppl 1): 183-7. http://d.scholar.cnki.net/detail/SJPD2059_U/SJPD12102401128777 [14] Chen RJ, Chu CT, Huang SC, et al. Telomerase activity in gestational trophoblastic disease and placental tissue from early and late human pregnancies[J]. Hum Reprod, 2002, 17(2): 463-8. doi: 10.1093/humrep/17.2.463 [15] Lehner R, Bobak J, Kim NW, et al. Localization of telomerase hTERT protein and survivin in placenta: relation to placental development and hydatidiform mole[J]. Obstet Gynecol, 2001, 97 (6): 965-70. [16] Caniggia I, Grisaru-Gravnosky S, Kuliszewsky M, et al. Inhibition of TGF-beta 3 restores the invasive capability of extravillous trophoblastsin preeclamptic pregnancies[J]. J Clin Invest, 1999, 103: 1641-50. doi: 10.1172/JCI6380 [17] Rajakumar A, Conrad KP. Expression, ontogeny, and regulation of hypoxia-inducible tran-scription factors in the human placenta[J]. Biol Reprod, 2000, 63: 559-69. doi: 10.1095/biolreprod63.2.559 [18] Rajakumar A, Conrad KP. Expression, ontogeny, and regulation of hypoxia-inducible transcription factors in the human placenta[J]. Biol Reprod, 2000, 63(2): 559-69. doi: 10.1095/biolreprod63.2.559 [19] Sharp AN, Heazell AE, Crocker IP, et al. Placental apoptosis in health and disease[J]. Am J Reprod Immunol, 2010, 64(3): 159-69. doi: 10.1111/j.1600-0897.2010.00837.x [20] Fitzpatrick AL, Kronmal RA, Gardner JP, et al. Leukocyte telomere length and cardiovascular disease in the cardiovascular health study [J]. Am J Epidemiol, 2007, 165(1): 14-21. [21] Valdes AM, Andrew T, Gardner JP, et al. Obesity, cigarette smoking, and telomere length in women[J]. Lancet, 2005, 366 (9486): 662-4. doi: 10.1016/S0140-6736(05)66630-5 -







 下载:
下载: