Diagnostic value of high field intensity MRI and multi-slice CT in occult fracture of knee joint
-
摘要:
目的 研究高场强MRI与多层螺旋CT(MSCT)对膝关节隐匿性骨折的检出情况及其诊断价值。 方法 以2019年1月~ 2022年1月我院收治的疑似膝关节隐匿性骨折患者90例为研究对象,所有患者均进行关节镜、高场强MRI及MSCT检查,以关节镜检查结果作为金标准,比较高场强MRI、MSCT对膝关节隐匿性骨折的检查结果与关节镜检出情况、诊断价值及对骨折塌陷程度、水平错位程度显示情况。 结果 90例疑似膝关节隐匿性骨折患者经关节镜检查确诊56例,高场强MRI检出率为92.86%,高于MSCT(78.57%,P < 0.05)。高场强MRI诊断膝关节隐匿性骨折的敏感度、特异性、阳性预测值、阴性预测值、准确度及曲线下面积(92.86%、94.12%、96.30%、88.89%、93.33%、0.935)均高于MSCT(78.57%、67.65%、80.00%、65.71%、74.44%、0.731,P < 0.05)。高场强MRI对骨折塌陷程度、水平错位程度显示率(64.44%、73.33%)均高于MSCT(43.33%、47.78%,P < 0.05)。 结论 与MSCT相比,高场强MRI对膝关节隐匿性骨折的检出率和诊断价值更高,对折塌陷程度、水平错位程度显示情况更好,可为膝关节隐匿性骨折的临床诊断提供可靠信息。 Abstract:Objective To investigate the diagnostic value of high field intensity MRI and multi-slice CT (MSCT) for occult fracture of knee joint. Methods A total of 90 patients with suspected occulted fracture of knee joint admitted to our hospital from January 2019 to January 2022 were studied. All patients underwent arthroscopy, high field intensity MRI and MSCT examination. With arthroscopy as the gold standard, compare the examination results of high field intensity MRI and MSCT on occult fracture of knee joint with the arthroscopic detection, diagnostic value, fracture collapse degree and horizontal dislocation degree. Results Among 90 suspected occult fracture of knee joint, 56 cases were diagnosed by arthroscopy. The detection rate of high field intensity MRI was higher than that of MSCT (92.86% vs 78.57%, P < 0.05). The sensitivity, specificity, positive predictive value, negative predictive value, accuracy and area under curve (92.86%, 94.12%, 96.30%, 88.89%, 93.33%, 0.935) of high field intensity MRI in the diagnosis of latent fracture of knee joint were higher than those of MSCT (78.57%, 67.65%, 80.00%, 65.71%, 74.44%, 0.731, P < 0.05). High field intensity MRI showed higher rates of fracture collapse degree and horizontal dislocation degree (64.44%, 73.33%) than MSCT (43.33%, 47.78%, P < 0.05). Conclusion Compared with MSCT, high-field MRI had a higher detection rate and diagnostic value for occult fracture of knee joint, and had a better indication of the degree of collapse and horizontal dislocation, which could provide reliable information for the clinical diagnosis of occult fracture of knee joint. -
表 1 高场强MRI、MSCT对膝关节隐匿性骨折的检查结果与关节镜检出情况对比
Table 1. Comparison between the examination results of occult fracture of knee joint by high field intensity MRI and MSCT and arthroscopy(n)
检查方法 关节镜 总计 膝关节隐匿性骨折 膝关节非隐匿性骨折 高场强MRI 膝关节隐匿性骨折 52 2 54 膝关节非隐匿性骨折 4 32 36 总计 56 34 90 MSCT 膝关节隐匿性骨折 44 11 55 膝关节非隐匿性骨折 12 23 35 总计 56 34 90 MSCT: 多层螺旋CT. 表 2 高场强MRI、MSCT对膝关节隐匿性骨折的诊断价值比较
Table 2. Comparison of the diagnostic value of high field intensity MRI and MSCT in occult fracture of knee joint
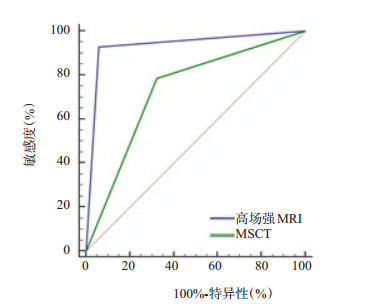
检查方法 敏感度(%) 特异性(%) 阳性预测值(%) 阴性预测值(%) 准确度(%) 曲线下面积 95% CI 高场强MRI 92.86(52/56) 94.12(32/34) 96.30(52/54) 88.89(32/36) 93.33(84/90) 0.935 0.863~0.976 MSCT 78.57(44/56) 67.65(23/34) 80.00(44/55) 65.71(23/35) 74.44(67/90) 0.731 0.627~0.819 χ2 4.667 6.087 5.425 4.213 11.879 4.522 - P 0.031 0.014 0.020 0.040 0.001 <0.001 - 表 3 高场强MRI、MSCT对骨折塌陷程度、水平错位程度显示情况比较
Table 3. Comparison of high field intensity MRI and MSCT on fracture collapse degree and horizontal dislocation degree [n=90, n(%)]
检查方法 骨折塌陷程度 水平错位程度 0级 Ⅰ级 Ⅱ级 Ⅲ级 显示率 0级 Ⅰ级 Ⅱ级 Ⅲ级 显示率 高场强MRI 32(35.56) 28(31.11) 22(24.44) 8(8.89) 58(64.44) 24(26.67) 32(35.56) 24(26.67) 10(11.11) 66(73.33) MSCT 51(56.67) 17(18.89) 16(17.78) 6(6.67) 39(43.33) 47(52.22) 22(24.44) 18(20) 3(3.33) 43(47.78) χ2 8.071 12.304 P 0.004 <0.001 -
[1] Shu ZH, Lei J, Ding CQ. Diagnostic value comparison between multislice spiral computerized tomography and magnetic resonance imaging under artificial intelligence algorithm in diagnosing occult fractures of the knee joint[J]. Contrast Media Mol Imaging, 2022, 2022: 3282409. [2] Fukui K, Kaneuji A, Hirata H, et al. Bilateral spontaneous simultaneous femoral neck occult fracture in a middle-aged man due to osteoporosis and vitamin D deficiency osteomalacia: a case report and literature review[J]. Int J Surg Case Rep, 2019, 60: 358-62. doi: 10.1016/j.ijscr.2019.06.058 [3] 蒲学佳, 胡元明, 吕涵青, 等. 双能量CT虚拟去钙技术对膝关节隐匿性骨折的诊断价值[J]. 影像诊断与介入放射学, 2020, 29(1): 22-6. doi: 10.3969/j.issn.1005-8001.2020.01.004 [4] 叶清岚, 李晶, 候金丹, 等. 多层螺旋CT与MRI在膝关节隐匿性骨折伴半月板及韧带损伤中的诊断比较[J]. 中国骨伤, 2022, 35(10): 967-70. doi: 10.12200/j.issn.1003-0034.2022.10.011 [5] 肖格林, 张海涛, 黄鸣宇. MSCT 3D技术在踝关节骨折Lauge-Hansen分型中的应用[J]. 中国CT和MRI杂志, 2018, 16(7): 147-9. doi: 10.3969/j.issn.1672-5131.2018.07.044 [6] 胥少汀, 葛宝丰, 徐印坎. 实用骨科学[M]. 4版. 北京: 人民军医出版社, 2012: 93-96. [7] 李颖, 刘云飞, 李艳茹, 等. 膝关节隐匿性骨折诊断中高场强MRI与MSCT应用价值比较[J]. 中国CT和MRI杂志, 2022, 20(4): 177-9. doi: 10.3969/j.issn.1672-5131.2022.04.057 [8] Park YC, Um KS, Hong SP, et al. Preoperative "Computed tomography capsular sign"for the detection of occult ipsilateral femoral neck fractures associated with femoral shaft fractures[J]. Injury, 2020, 51(4): 1051-6. doi: 10.1016/j.injury.2020.02.067 [9] Park YC, Song HK, Yang KH. Prevention of unplanned surgery due to delayed diagnosis of occult ipsilateral femoral neck fractures associated with femoral shaft fractures: a study of the CT capsular sign with lipohemarthrosis[J]. J Bone Joint Surg Am, 2021, 103 (15): 1431-7. doi: 10.2106/JBJS.20.02033 [10] 何源亮, 李旭, 熊雄. CT和MRI应用于骨关节隐匿性骨折中的临床价值分析[J]. 中国CT和MRI杂志, 2021, 19(8): 172-4. doi: 10.3969/j.issn.1672-5131.2021.08.056 [11] 朱亚敏, 殷向辉, 朱昕怡, 等. CT与MRI扫描三维重建在四肢骨关节隐匿性骨折诊断中的应用[J]. 现代生物医学进展, 2020, 20(22): 4344-7, 4278. https://www.cnki.com.cn/Article/CJFDTOTAL-SWCX202022032.htm [12] 李渡江, 陈伟, 董研. 分析多层螺旋CT在中老年复杂性膝关节骨折临床诊断中的效果及对骨折分型的临床诊断效果[J]. 中国CT和MRI杂志, 2021, 19(3): 165-7. doi: 10.3969/j.issn.1672-5131.2021.03.055 [13] 任海娟, 魏剑波, 刘颖, 等. MSCT联合MRI在马拉松运动员膝关节损伤诊断中的应用[J]. 影像科学与光化学, 2022, 40(4): 971-5. https://www.cnki.com.cn/Article/CJFDTOTAL-GKGH202204053.htm [14] 张军胜, 赵波. 多层螺旋CT对膝关节损伤后胫骨平台隐匿性骨折早期诊断的效果及价值[J]. 解放军医药杂志, 2018, 30(8): 96-9. https://www.cnki.com.cn/Article/CJFDTOTAL-HBGF201808025.htm [15] 吴发财, 杨东辉, 陈琦, 等. 不同影像学方法诊断踝关节隐匿性骨折的准确率比较[J]. 中国CT和MRI杂志, 2019, 17(2): 140-2. https://www.cnki.com.cn/Article/CJFDTOTAL-CTMR201902043.htm [16] 蔡金玉, 钟海燕, 杨璐丹, 等. 多层螺旋CT三维重建技术在隐匿性微小骨折诊断中的应用[J]. 蚌埠医学院学报, 2018, 43(11): 1493-5. https://www.cnki.com.cn/Article/CJFDTOTAL-BANG201811031.htm [17] 李文敏. 应用MRI脂肪抑制技术对膝关节隐匿性骨折诊断价值探讨[J]. 中国CT和MRI杂志, 2020, 18(12): 167-9. https://www.cnki.com.cn/Article/CJFDTOTAL-CTMR202012053.htm [18] 陈勇, 韩金花, 刘青云, 等. MRI、MSCT后处理技术对隐匿性骨折的诊断价值分析[J]. 中国CT和MRI杂志, 2021, 19(2): 162-4. https://www.cnki.com.cn/Article/CJFDTOTAL-CTMR202102055.htm [19] 张静雅, 刘宁, 刘爽, 等. 隐匿性胫骨平台骨折MRI、CT检查的影像学表现及其诊断价值对比的回顾性研究[J]. 现代生物医学进展, 2021, 21(6): 1085-8. https://www.cnki.com.cn/Article/CJFDTOTAL-SWCX202106020.htm [20] Kwong A, Aldridge ES, Jayawardana R, et al. Length of stay outcomes in patients receiving ketamine sedation versus Bier's block anaesthesia for procedural closed fracture reduction: a retrospective audit of paediatric emergency department patients[J]. Emerg Med Australas, 2022, 34(1): 73-7. [21] 孙秋原, 李骥, 牛亚峰. 外伤性膝关节隐性骨折的核磁共振成像表现及其诊断价值分析[J]. 影像科学与光化学, 2020, 38(1): 138-43. https://www.cnki.com.cn/Article/CJFDTOTAL-GKGH202001020.htm -







 下载:
下载: