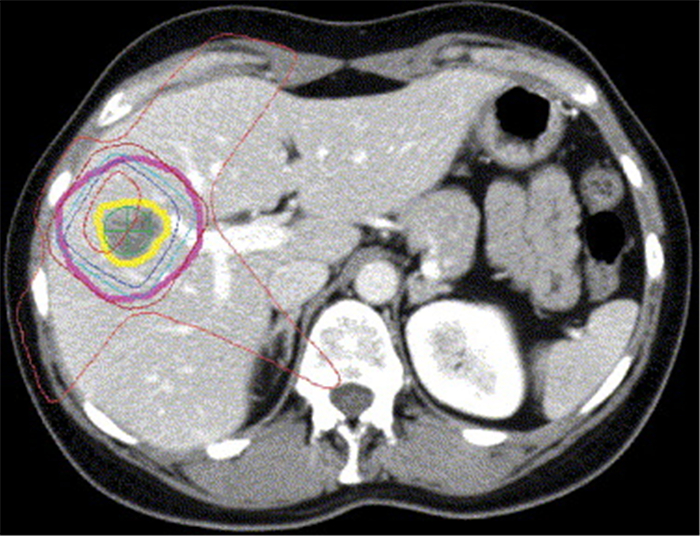
Prospective comparison of CT and MRI in delineation of hepatocellular carcinoma using deformable image registration
-
摘要:
目的 通过比较MRI与CT对肝癌肿瘤的诊断情况,进而进行高精度放疗计划。 方法 选择2020年7月~2022年7月收治的26例不可切除的肝转移(n=8)、肝细胞癌(n=10)和胆管癌(n=8)患者作为研究对象,患者在放疗计划时进行了具有诊断质量的MRI扫描和三期CT扫描,并确定了肝内解剖参考点。在最能显示肿瘤的CT和MRI系列中,勾画了肝脏和肿瘤体积,确定了肝内解剖参考点。采用形变配准对CT和MRI的肝脏进行配准。 结果 5例肝癌CT病灶数量与MRI有差异,MRI病灶多3例,CT病灶多2例。肝脏变形配准后,CT肿瘤表面与MRI肿瘤表面平均距离的人群中位数为3.7(2.2~21.3)mm。肿瘤表面积相差5 mm的中位百分比为26%(38%~86%)。转移瘤的中位符合率为81%(77%~86%),肝细胞癌的一致性为78%(44%~86%),胆管癌的一致性为69%(25%~85%)。 结论 MRI诊断的肝癌肿瘤体积与CT诊断的肝癌肿瘤体积存在显著差异,且在原发性肝癌中更为常见。 Abstract:Objective To compare MRI and CT in the diagnosis of hepatocellular carcinoma tumors and to conduct high-precision radiotherapy planning. Methods Twenty-six patients with unresectable liver metastases (n=8), hepatocellular carcinoma (n=10) and cholangiocarcinoma (n=8) from July 2020 to July 2022 were selected. All patients underwent MRI and three-phase CT scans of diagnostic quality at the time of radiotherapy planning, and intrahepatic anatomical reference points were identified. In the CT and MRI series that best visualized the tumor, liver and tumor volume were delineated and intrahepatic anatomical reference points were identified. Deformable registration was used to register CT and MRI livers. Results The number of CT lesions was different from that of MRI in 5 cases of liver cancer. MRI lesions were more in 3 cases and CT lesions were more in 2 cases. After liver deformation registration, the average distance between CT tumor surface and MRI tumor surface in the population was 3.7(2.2-21.3) mm. The median percentage of tumor surface area difference of 5 mm was 26%(38%-86%). The median coincidence rate was 81%(77%-86%)for metastases, 78%(44%-86%) for hepatocellularcarcinoma, and 69%(25%-85%) for cholangiocarcinoma. Conclusion The tumor volume of hepatocellular carcinoma diagnosed by MRI is significantly different from that diagnosed by CT, and it is more common in primary hepatocellular carcinoma. -
表 1 CT和MRI上显性GTV体积的差异
Table 1. Difference in dominant GTV volume between CT and MRI
类型 CT-GTV与MRI-GTV的中位比值及范围 病例数(n) 病变数量差异(n) CT-GTV≥1.2 MRI-GTV MRI-GTV≥1.2 CT-GTV 肝癌 1.01(0.29~1.47) 4/10 1/10 5/10 胆管癌 1.07(0.21~3.98) 3/8 1/8 No 肝转移 0.94(0.80~1.50) 2/8 1/8 No 单发灶 1.13(0.28~1.45) 5/11 1/11 N/A 混合肿瘤 0.95(0.21~3.98) 4/15 2/15 5/15 总和 1.02(0.21~3.98) 9/26 3/26 5/26 GTV: 肿瘤体积. 表 2 26例患者的变形配准
Table 2. Deformation registration of 26 patients
类型 几何分辨视图CT体积(cc) CV锥体配准 CV变形配准 肝癌 211(12~1483) 75%(38%~86%) 78%(44%~88%) 胆管癌 146(3~538) 65%(15%~81%) 69%(25%~85%) 肝转移 191(9~516) 73%(55%~86%) 81%(77%~86%) 单发灶 130(9~232) 63%(38%~86%) 77%(44%~86%) 混合肿瘤 283(3~1483) 75%(15%~86%) 79%(22%~86%) 总和 169(3~1483) 74%(15%~86%) 78%(25%~88%) %CV: 一致性百分比. 以中位数(范围)表示. 表 3 几何分辨CT-GTV和MRI-GTV之间的表面积在空间位置上百分比的总体中值
Table 3. Overall median of the percentage of surface area between geometrically resolved CT-GTV and MRI-GTV at spatial locations
类型 百分比表面积 > 3 mm > 5 mm > 10 mm > 15 mm 肝癌 60%(28%~78%) 45%(38%~86%) 13%(0%~31%) 7%(0%~25%) 胆管癌 58%(40%~93%) 26%(38%~86%) 5%(0%~66%) 2%(0%~56%) 肝转移 40%(28%~75%) 19%(38%~86%) 1%(0%~31%) 0%(0%~15%) 单发灶 48%(28%~76%) 22%(38%~86%) 2%(0%~31%) 0%(0%~25%) 混合肿瘤 58%(28%~93%) 28%(38%~86%) 16%(0%~66%) 2%(0%~56%) 总和 55%(28%~93%) 26%(38%~86%) 5%(0%~66%) 0%(0%~56%) 以中位数(范围)表示. -
[1] 程洪涛, 郭晨阳, 耿翔, 等. 肝动脉造影CT引导下经皮穿刺射频消融治疗富血管肝细胞癌的临床研究[J]. 中华放射学杂志, 2022, 56(7): 800-4. doi: 10.3760/cma.j.cn112149-20210726-00701 [2] Kim SY, An J, Lim YS, et al. MRI with liver-specific contrast for surveillance of patients with cirrhosis at high risk of hepatocellular carcinoma[J]. JAMA Oncol, 2017, 3(4): 456-63. doi: 10.1001/jamaoncol.2016.3147 [3] 王远平, 郑露露, 张光亮. MRI与4DCT联合指导勾画原发性肝癌患者放疗靶区初步研究[J]. 实用肝脏病杂志, 2022, 25(4): 567-70. doi: 10.3969/j.issn.1672-5069.2022.04.028 [4] 叶鹏飞, 胡博, 田恩照. 64层螺旋CT与磁共振成像对乙型肝炎肝硬化背景小肝癌病灶的诊断效果[J]. 实用医学影像杂志, 2022, 23(3): 277-9. https://www.cnki.com.cn/Article/CJFDTOTAL-SYXY202203019.htm [5] Roberts LR, Sirlin CB, Zaiem F, et al. Imaging for the diagnosis of hepatocellular carcinoma: a systematic review and meta-analysis[J]. Hepatology, 2018, 67(1): 401-21. doi: 10.1002/hep.29487 [6] 黄淑芳, 李长清, 罗是是. 普美显增强MRI与CT对原发性肝癌诊断的价值研究[J]. 中国医学装备, 2022, 19(6): 43-8. https://www.cnki.com.cn/Article/CJFDTOTAL-YXZB202206010.htm [7] 廖云鸿, 张克文. 普美显增强MRI联合GE-64排螺旋CT放射诊断肝癌及肝脏局灶性结节增生的临床价值分析[J]. 现代医用影像学, 2022, 31(5): 858-61. doi: 10.3969/j.issn.1006-7035.2022.05.016 [8] Alabousi M, McInnes MD, Salameh JP, et al. MRI vs. CT for the detection of liver metastases in patients with pancreatic carcinoma: a comparative diagnostic test accuracy systematic review and meta-analysis[J]. J Magn Reson Imaging, 2021, 53(1): 38-48. doi: 10.1002/jmri.27056 [9] Hecht EM, Zins M, Tamm EP. Editorial for "MRI vs. CT for the detection of liver metastases in patients with pancreatic carcinoma: a comparative diagnostic test accuracy systematic review and meta-analysis"[J]. J Magn Reson Imaging, 2021, 53(1): 49-50. doi: 10.1002/jmri.27072 [10] 伍秋艳, 刘娟, 杨崇双, 等. 影像学检查在诊断小肝癌中的应用价值[J]. 中华消化外科杂志, 2022, 21(4): 543-50. [11] Zech CJ, Korpraphong P, Huppertz A, et al. Randomized multicentre trial of gadoxetic acid-enhanced MRI versus conventional MRI or CT in the staging of colorectal cancer liver metastases[J]. Br J Surg, 2014, 101(6): 613-21. doi: 10.1002/bjs.9465 [12] Semaan S, Vietti Violi N, Lewis S, et al. Hepatocellular carcinoma detection in liver cirrhosis: diagnostic performance of contrast-enhanced CT vs. MRI with extracellular contrast vs. gadoxetic acid[J]. Eur Radiol, 2020, 30(2): 1020-30. doi: 10.1007/s00330-019-06458-4 [13] 李园苑, 王露颖, 沈莹. CT和MRI对原发性肝癌患者介入及分子靶向治疗效果评价[J]. 医学影像学杂志, 2022, 32(3): 535-8. https://www.cnki.com.cn/Article/CJFDTOTAL-XYXZ202203043.htm [14] 姜永继, 邱冬, 郑萍, 等. 多层螺旋CT扫描评估肝癌介入治疗临床效果及应用意义[J]. 中国CT和MRI杂志, 2022, 20(4): 93-5. https://www.cnki.com.cn/Article/CJFDTOTAL-CTMR202204054.htm [15] Kim C, Kim SY, Kim MJ, et al. Clinical impact of preoperative liver MRI in the evaluation of synchronous liver metastasis of colon cancer[J]. Eur Radiol, 2018, 28(10): 4234-42. [16] 刘迪斯, 陈洁文, 洪静静, 等. MRI联合多层螺旋CT检查用于原发性肝癌介入治疗患者疗效评定的价值[J]. 分子影像学杂志, 2022, 45(2): 210-3. doi: 10.12122/j.issn.1674-4500.2022.02.09 [17] Basha MAA, AlAzzazy MZ, Ahmed AF, et al. Does a combined CT and MRI protocol enhance the diagnostic efficacy of LI-RADS in the categorization of hepatic observations? A prospective comparative study[J]. Eur Radiol, 2018, 28(6): 2592-603. [18] 赵姝娟. 磁共振动态增强联合磁共振弥散加权成像对肝占位性病变的诊断价值探讨[J]. 中国实用医药, 2022, 17(4): 76-8. https://www.cnki.com.cn/Article/CJFDTOTAL-ZSSA202204028.htm [19] Kim YY, Choi JY, Sirlin CB, et al. Pitfalls and problems to be solved in the diagnostic CT/MRI Liver Imaging Reporting and Data System(LI-RADS)[J]. Eur Radiol, 2019, 29(3): 1124-32. [20] Voroney JP, Brock KK, Eccles C, et al. Prospective comparison of computed tomography and magnetic resonance imaging for liver cancer delineation using deformable image registration[J]. Int J Radiat Oncol Biol Phys, 2006, 66(3): 780-91. [21] Xu H, Gong GZ, Wei H, et al. Feasibility and potential benefits of defining the internal gross tumor volume of hepatocellular carcinoma using contrast-enhanced 4D CT images obtained by deformable registration[J]. Radiat Oncol, 2014, 9: 221. [22] Wang H, Krishnan S, Wang XC, et al. Improving soft-tissue contrast in four-dimensional computed tomography images of liver cancer patients using a deformable image registration method[J]. Int J Radiat Oncol, 2008, 72(1): 201-9. -







 下载:
下载: