Diagnostic efficacy of transvaginal ultrasound combined with contrast enhanced ultrasound for first-trimester caesarean scar ectopic pregnancy
-
摘要:
目的 探究阴道超声联合超声造影测定子宫瘢痕厚度对瘢痕妊娠的诊断价值。 方法 选取我院2019年12月~2021年12月收治的92例疑似瘢痕妊娠患者为研究对象,采用阴道超声与超声造影对患者进行孕早期子宫瘢痕厚度测定,比较两种检查方式相关图像表现结果与病理检查结果,采用ROC曲线判断其厚度对瘢痕妊娠的诊断效能。 结果 阴道超声测量结果为7.03± 0.17 mm,超声造影结果为7.25±0.14 mm,病理检查结果为7.42±0.15 mm,超声造影检查的厚度高于经阴道超声(P < 0.05),两种方式检查结果均低于病理检查结果(P < 0.05)。对两种检查方式的图像进行比较,阴道超声检查诊断为92例患者均无法排除瘢痕妊娠,其中83例患者明确观察到妊娠物着床于瘢痕处,确诊为瘢痕妊娠,另9例患者无法确定其着床位置,无法排除瘢痕妊娠。进行超声造影后发现,有86例患者诊断为瘢痕妊娠,其中孕囊型57例,包块型29例,6例组织物植入肌层。病理检查结果显示,瘢痕妊娠88例,非瘢痕处峡部妊娠2例,妊娠着床位置过低2例。经阴道超声诊断准确度为92.39%,敏感度为94.31%,特异性为50.00%,超声造影诊断准确度、敏感度以及特异性分别为96.74%、97.73%、75.00%。经ROC曲线分析可得,阴道超声和超声造影诊断瘢痕妊娠的曲线下面积分别为0.722、0.864,超声造影诊断整体效能高于经阴道超声。 结论 与经阴道超声相比,超声造影对子宫瘢痕厚度测量更加接近病理检查结果,能更为清晰地观察妊娠物着床部位,显示其与子宫肌层的关系,对瘢痕妊娠的诊断准确性、敏感度和特异性更高。 Abstract:Objective To analyze the diagnostic efficacy of transvaginal ultrasound combined with contrast enhanced ultrasound for first-trimester caesarean scar ectopic pregnancy. Methods Ninety-two women with suspected scar pregnancy in our hospital from December 2019 to December 2021 were enrolled. The lower uterine segment thickness was measured using transvaginal ultrasound combined with contrast enhanced ultrasound. The imaging findings and the pathological results were compared between two examinations were compared. ROC curve was used to evaluate the diagnostic efficacy of lower uterine segment thickness on scar pregnancy. Results The mean lower uterine segment thickness was 7.03 ± 0.17 mm measured by transvaginal ultrasound, 7.25±0.14 mm by contrast enhanced ultrasound and 7.42±0.15 mm by pathological examination. The scar thickness in contrast enhanced ultrasound was significantly thicker than that in transvaginal ultrasound (P < 0.05). Comparison of the two types of images showed that 83 of the 92 patients diagnosed by transvaginal ultrasound had clearly observed the implantation of embryos at the scar and were diagnosed as scar pregnancy, while the implantation position of the other 9 patients could not be determined and scar pregnancy could not be ruled out. Contrast enhanced ultrasound showed that 86 patients were diagnosed with scar pregnancy, including 57 cases of cyst type, 29 cases of mass type, and 6 cases of myometrial trophoblastic tissue implantation. Pathological examination results showed that 88 cases of scar pregnancy, 2 cases of isthmic pregnancy, 2 cases of low embryo implantation site. Transvaginal ultrasound had a diagnostic accuracy of 92.39%, sensitivity of 94.31% and specificity of 50.00%, while contrast-enhanced ultrasound had a diagnostic accuracy of 96.74%, sensitivity of 97.73% as well as specificity of 75.00%, respectively. The AUCs of transvaginal ultrasound and contrast-enhanced ultrasound for the diagnosis of scar pregnancy were 0.722 and 0.864. The overall diagnostic efficacy of contrast enhanced ultrasound was significantly better than that of transvaginal ultrasound. Conclusion Taking pathological findings as golden standard, contrast- enhanced ultrasound has a better uterine scar thickness measurement compared with transvaginal ultrasound, which can clearly observe embryo implantation site and the relationship with the myometrium, achieves better diagnostic accuracy, sensitivity and specificity for scar pregnancy. -
表 1 不同检查方式瘢痕诊断与病理结果对比
Table 1. Comparison of scar diagnosis and pathological results of different examination methods (n)
检杳方式 检查结果 金标准 合计 瘢痕妊娠 非瘢痕妊娠 经阴道超声 瘢痕妊娠 83 2 85 非瘢痕妊娠 5 2 7 超声造影 瘢痕妊娠 86 1 87 非瘢痕妊娠 2 3 5 合计 88 4 92 表 2 不同检查方式对瘢痕妊娠的诊断效能
Table 2. Diagnostic efficacy of different examination methods for scar pregnancy (%)
检杳方式 准确率 特异性 敏感度 阴道超声 92.39 50.00(2/4) 94.3(83/88) 超声造影 96.74 75.00(3/4) 97.73(86/88) 表 3 不同检查方式瘢痕诊断及联合诊断瘢痕妊娠的ROC曲线分析
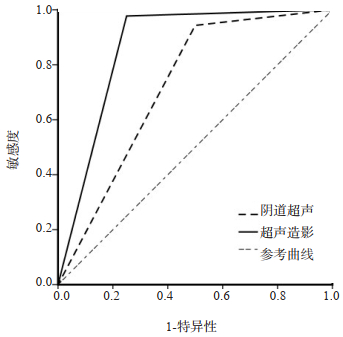
Table 3. ROC curve analysis of scar diagnosis and combined diagnosis of scar pregnancy by different examination methods
指标 AUC 95% CI P 敏感度(%) 特异性(%) 阴道超声 0.722 0.409~1.000 0.135 94.31 50.00 超声造影 0.864 0.608~1.000 0.014 97.73 75.00 -
[1] 黄波涛, 区俊兴, 原仲晖, 等. 对比MRI动态增强和超声在早期剖宫产瘢痕妊娠中的应用价值[J]. 临床放射学杂志, 2018, 37(5): 781-5. https://www.cnki.com.cn/Article/CJFDTOTAL-LCFS201805017.htm [2] Calì G, Timor-Tritsch IE, Palacios-Jaraquemada J, et al. Outcome of Cesarean scar pregnancy managed expectantly: systematic review and meta-analysis[J]. Ultrasound Obstet Gynecol, 2018, 51 (2): 169-75. doi: 10.1002/uog.17568 [3] 叶天和, 潘峰, 周国锋, 等. 预防性子宫动脉化疗栓塞术序贯超声导引下清宫术治疗瘢痕妊娠的临床观察[J]. 介入放射学杂志, 2018, 27 (2): 128-32. doi: 10.3969/j.issn.1008-794X.2018.02.008 [4] 宁浩杰, 韦德湛, 谢宏基, 等. 经阴道三维超声对剖宫产瘢痕部位妊娠的早期预测价值[J]. 中国现代医学杂志, 2020, 30(11): 69-73. doi: 10.3969/j.issn.1005-8982.2020.11.015 [5] 石辛景, 康志平, 邢龙颜, 等. 经阴道多普勒彩色超声联合血清人绒毛膜促性腺激素对子宫瘢痕妊娠的诊断价值分析[J]. 影像科学与光化学, 2020, 38(2): 280-5. https://www.cnki.com.cn/Article/CJFDTOTAL-GKGH202002019.htm [6] 李康宁, 姜玉新, 刘真真, 等. 宫腔超声造影对剖宫产瘢痕妊娠治疗后的远期随访评估[J]. 中国医学影像技术, 2016, 32(3): 411-5. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYXX201603032.htm [7] 肖汀, 黄伟俊, 张四友, 等. 经阴道超声与超声造影联合临床因素评估剖宫产术后瘢痕妊娠治疗方式的研究[J]. 中华超声影像学杂志, 2022, 31(3): 231-5. [8] Morlando M, Buca D, Timor-Tritsch I, et al. Reproductive outcome after cesarean scar pregnancy: a systematic review and metaanalysis[J]. Acta Obstet Gynecol Scand, 2020, 99(10): 1278-89. doi: 10.1111/aogs.13918 [9] Kim SY, Yoon SR, Kim MJ, et al. Cesarean scar pregnancy; Diagnosis and management between 2003 and 2015 in a single center[J]. Taiwan J Obstet Gynecol, 2018, 57(5): 688-91. doi: 10.1016/j.tjog.2018.08.013 [10] 王超, 姚颖, 李蓉, 等. 剖宫产瘢痕妊娠的流行病学研究: 现状与展望[J]. 中国妇产科临床杂志, 2021, 22(4): 444-5. https://www.cnki.com.cn/Article/CJFDTOTAL-FKLC202104037.htm [11] 刘亚静, 石辛景, 陈莉茹, 等. MRI、超声测量瘢痕妊娠的瘢痕厚度与病理测量结果的相关性[J]. 放射学实践, 2020, 35(9): 1161-5. https://www.cnki.com.cn/Article/CJFDTOTAL-FSXS202009025.htm [12] 卓娜, 汪娟. 经阴道三维超声联合超声造影对瘢痕妊娠的诊断价值[J]. 临床与病理杂志, 2020, 40(9): 2302-6. https://www.cnki.com.cn/Article/CJFDTOTAL-WYSB202009013.htm [13] 陈小梅. 妊娠期子宫瘢痕情况与剖宫产术后再次妊娠孕妇发生子宫破裂的相关性[J]. 甘肃医药, 2021, 40(4): 340-2. https://www.cnki.com.cn/Article/CJFDTOTAL-GSYY202104018.htm [14] Pędraszewski P, Wlaźlak E, Panek W, et al. Cesarean scar pregnancya new challenge for obstetricians[J]. J Ultrason, 2018, 18 (72): 56-62. [15] Harb HM, Knight M, Bottomley C, et al. Caesarean scar pregnancy in the UK: a national cohort study[J]. BJOG, 2018, 125(13): 1663-70. [16] 刘洁, 崔稳丽, 柴义青. 三维彩超在评估剖宫产后子宫瘢痕部位妊娠中的应用[J]. 中国临床医学影像杂志, 2018, 29(2): 118-20. https://www.cnki.com.cn/Article/CJFDTOTAL-LYYX201802013.htm [17] 樊宇英, 王伦志, 唐磊, 等. 阴道超声联合MRI诊断剖宫产切口瘢痕妊娠残余子宫肌层厚度的价值[J]. 分子影像学杂志, 2020, 43(4): 672-5. doi: 10.12122/j.issn.1674-4500.2020.04.26 [18] 胡晶晶, 罗振凌. 对比经阴道超声与MRI检查对剖宫产术后瘢痕妊娠的诊断价值研究[J]. 中国CT和MRI杂志, 2022, 20(3): 111-2, 125. https://www.cnki.com.cn/Article/CJFDTOTAL-CTMR202203028.htm [19] 吕群星. 阴道超声联合超声造影在剖宫产后疤痕妊娠中的应用分析[J]. 现代医用影像学, 2020, 29(5): 921-3. https://www.cnki.com.cn/Article/CJFDTOTAL-XDYY202005041.htm [20] 马斌, 王艺璇, 冉婕, 等. 超声鉴别诊断瘢痕妊娠与宫腔下段非瘢痕妊娠[J]. 中国医学影像技术, 2018, 34(5): 729-33. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYXX201805029.htm [21] Timor-Tritsch IE, Monteagudo A, Calì G, et al. Cesarean scar pregnancy: diagnosis and pathogenesis[J]. Obstet Gynecol Clin N Am, 2019, 46(4): 797-811. [22] Liu DM, Gu XN, Liu F, et al. Contrast-enhanced ultrasound in uterine artery embolization treatment of cesarean scar pregnancy [J]. J Int Med Res, 2020, 48(12): 030006052098021. [23] 田媛媛, 赵萍, 刘鸽, 等. 经阴道二维联合三维超声对剖宫产后子宫瘢痕妊娠的诊断价值[J]. 中国超声医学杂志, 2021, 37(9): 1043-6. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGCY202109027.htm [24] 乐小莉, 范俊儿. 彩色多普勒超声联合超声造影早期诊断不同类型剖宫产瘢痕部位妊娠的临床价值[J]. 中国妇幼保健, 2018, 33(8): 1874-6. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFYB201808065.htm [25] 朱莉, 李丽雅, 吕国荣. 超声造影在瘢痕妊娠诊疗中的应用[J]. 中国超声医学杂志, 2019, 35(9): 837-9. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGCY201909022.htm [26] 郭艳嫦, 严燕琼, 雷伟玲, 等. 经阴道彩色多普勒超声对Ⅰ型及Ⅱ型子宫瘢痕妊娠的诊断价值[J]. 分子影像学杂志, 2019, 42(3): 306-9. doi: 10.12122/j.issn.1674-4500.2019.03.06 -







 下载:
下载: