Clinical value of ultrasonic fetal membrane thickness combined with serum IL-6 and CRP in predicting premature delivery in the second and third trimesters of pregnancy
-
摘要:
目的 探讨孕中晚期超声胎膜厚度检测联合血清白介素-6(IL-6)、C反应蛋白(CRP)预测早产发生的临床价值。 方法 收集2019年1月1日~2020年12月31日于我院建档进行产检和分娩的599例孕妇作为研究对象,根据分娩时间将孕妇分为早产组(n=86)和足月组(n=513),分析两组孕妇孕中、晚期血清IL-6、CRP及超声胎膜厚度,采用ROC曲线分析上述3项指标对孕妇早产的预测价值,并比较两组孕妇通过各指标诊断的阳性率。 结果 在孕23~25周和孕32~34周,早产组孕妇血清IL-6、CRP水平高于足月组(P < 0.05),胎膜厚度低于足月组(P < 0.05);ROC曲线分析结果显示,超声胎膜厚度联合血清IL-6、CRP预测早产的ROC曲线下面积高于3项指标单独预测的ROC曲线下面积(P < 0.05);且联合预测的准确度、敏感度和特异性均较高。早产组孕妇血清IL-6、CRP和胎膜厚度单项诊断和联合诊断早产的阳性率均高于足月组(P < 0.05)。 结论 与足月生产孕妇比较,早产孕妇中晚期的血清IL-6、CRP水平明显更高,胎膜厚度更高,联合检测血清IL-6、CRP和胎膜厚度对于预测孕妇早产具有较高的应用价值。 Abstract:Objective To explore the clinical value of ultrasonic fetal membrane thickness combined with serum interleukin-6 (IL-6) and C-reactive protein (CRP) in predicting premature delivery in the second and third trimesters of pregnancy. Methods A total of 599 pregnant women undergoing prenatal examination and delivery in the hospital were enrolled as the research objects from January 1st, 2019 to December 31st, 2020. According to different delivery time, they were divided into premature delivery group (n=86) and full-term group (n=513). The serum IL-6, CRP and ultrasonic fetal membrane thickness in both groups were analyzed in the second and third trimesters of pregnancy. The predictive value of the above three indexes for premature delivery was analyzed by ROC curves. The positive rates of different indexes were compared between the two groups. Results Within 23-25 and 32-34 gestational weeks, levels of serum IL-6 and CRP in premature delivery group were significantly higher than those in full-term group (P < 0.05), while thickness of fetal membranes was thinner than that in fullterm group (P < 0.05). The ROC curves analysis showed that the area under the ROC curve of ultrasonic fetal membrane thickness combined with serum IL-6 and CRP for predicting premature delivery was greater than that of single index (P < 0.05). The accuracy, sensitivity and specificity of combined prediction were higher. The positive rates of premature delivery by single diagnosis and combined diagnosis in premature delivery group were higher than those in full-term group (P < 0.05). Conclusion Compared with full-term pregnant women, levels of serum IL-6 and CRP are significantly higher, and thickness of fetal membranes is thicker in pregnant women with premature deliver in the second and third trimesters. The combined detection of serum IL-6, CRP and fetal membrane thickness has higher predictive value for premature delivery. -
表 1 两组孕妇孕中晚期血清IL-6、CRP水平及胎膜厚度比较
Table 1. Comparison of serum IL- 6, CRP levels and fetal membrane thickness between the two groups during middle and late pregnancy (Mean±SD)
组别 IL-6(μg/L) CRP(mg/L) 胎膜厚度(mm) 孕23~25周 孕32~34周 孕23~25周 孕32~34周 孕23~25周 孕32~34周 早产组(n=86) 6.45±2.19 8.52±2.68a 11.36±2.37 14.49±3.15a 1.21±0.27 1.24±0.24 足月组(n=513) 3.67±1.04 4.05±1.33 4.69±1.34 4.85±1.25 1.46±0.25 1.43±0.26 t 18.800 24.072 37.423 49.864 8.482 6.339 P < 0.001 < 0.001 < 0.001 < 0.001 < 0.001 < 0.001 aP < 0.05 vs孕23~25周. IL-6: 白介素-6; CRP: C反应蛋白. 表 2 ROC曲线各项指标对早产的曲线下面积值
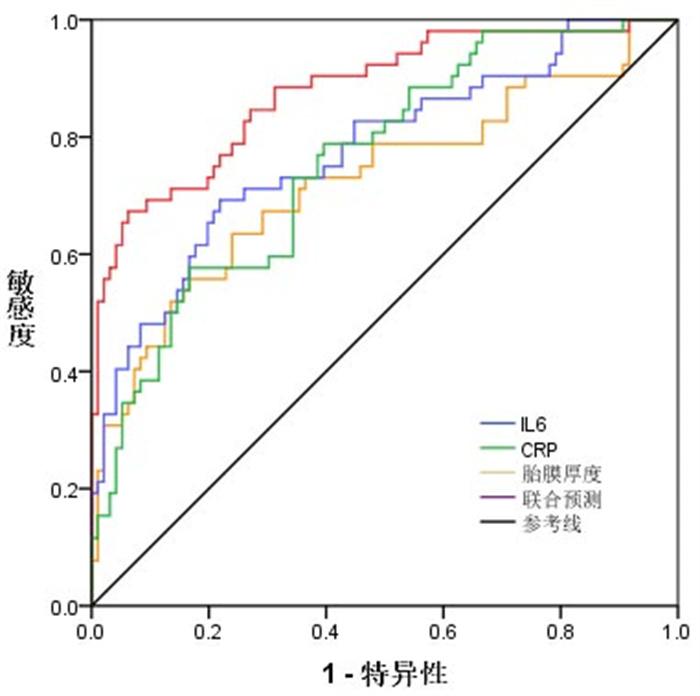
Table 2. AUC values of ROC curve for each indicator about premature delivery
指标 曲线下面积 SE P 截断值 95% CI IL-6 0.776 0.041 < 0.001 > 5.823 μg/L 0.695~0.857 CRP 0.758 0.040 < 0.001 > 10.122 mg/L 0.679~0.837 胎膜厚度 0.725 0.047 < 0.001 < 1.309 mm 0.633~0.817 联合预测 0.878 0.031 < 0.001 0.818~0.938 表 3 各项指标预测早产的准确度、敏感度和特异性
Table 3. Accuracy, sensitivity, and specificity of various indicators for predicting preterm birth (%)
指标 准确度 敏感度 特异性 IL-6 74.96 69.12 77.96 CRP 77.96 57.60 83.14 胎膜厚度 71.95 63.44 75.96 联合预测 87.98 67.28 93.66 表 4 两组孕妇血清IL-6、CRP水平及胎膜厚度的单项、联合诊断阳性率比较
Table 4. The positive rates of serum IL-6, CRP levels and membrane thickness were compared between the two groups by single and combined diagnosis [n(%)]
组别 IL-6 CRP 胎膜厚度 IL-6+CRP+胎膜厚度 早产组(n=86) 62(72.09) 71(82.56) 65(75.58) 76(88.37) 足月组(n=513) 296(57.70) 302(58.87) 299(58.28) 314(61.20) χ2 6.345 17.592 9.243 23.992 P 0.012 < 0.001 0.002 < 0.001 -
[1] Salas A, Gastón B, Barrenetxea J, et al. Predictive value of hyperglycosylated human chorionic gonadotropin for pregnancy outcomes in threatened abortion in first-trimester viable pregnancies [J]. An Sist Sanit Navar, 2021, 44(1): 23-31. doi: 10.23938/ASSN.0933 [2] 丁晓颖, 蔡燕, 杨慧琳, 等. 孕中期宫颈阴道分泌物中IL-6、TNF-α和CRH的水平与早产的关系[J]. 中国妇幼健康研究, 2018, 29(11): 1414-8. doi: 10.3969/j.issn.1673-5293.2018.11.012 [3] Liang L, Rasmussen MLH, Piening B, et al. Metabolic dynamics and prediction of gestational age and time to delivery in pregnant women [J]. Cell, 2020, 181(7): 1680-92. e15. doi: 10.1016/j.cell.2020.05.002 [4] 杨仪心, 叶小凤, 劳力, 等. CRP、PCT、IL-6检测在妊娠晚期GBS感染患者妊娠结局预测中的价值[J]. 中国性科学, 2020, 29(1): 91-4. https://www.cnki.com.cn/Article/CJFDTOTAL-XKXZ202001028.htm [5] 苗菁菁, 喻红霞, 邵文嘉, 等. 宫颈长度及胎膜厚度预测双胎妊娠早产的价值研究[J]. 中国全科医学, 2021, 24(33): 4240-5. doi: 10.12114/j.issn.1007-9572.2021.02.045 [6] 吴红莲, 陈艳, 黄志华, 等. 胎膜早破孕妇血清白细胞介素-6和C-反应蛋白的变化情况与胎膜早破感染的关系[J]. 中华医院感染学杂志, 2018, 28(7): 1086-8, 1096. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHYY201807034.htm [7] 吴旸, 周欣. 妊娠中期羊水中相关炎症介质预测早产的研究进展[J]. 国际妇产科学杂志, 2019, 46(6): 627-31. doi: 10.3969/j.issn.1674-1870.2019.06.007 [8] 廖化波, 魏利, 程相红, 等. 血清MMP-2、IL-8、β-hCG对胎膜早破妊娠患者合并羊膜腔感染的诊断[J]. 中华医院感染学杂志, 2020, 30 (9): 1393-7. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHYY202009026.htm [9] 中国抗癌协会妇科肿瘤专业委员会. 妊娠滋养细胞疾病诊断与治疗指南(2021年版[) J]. 中国癌症杂志, 2021, 31(6): 520-32. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGAZ202106010.htm [10] 胡彦, 李岚, 刘彤, 等. 白细胞介素-6、肿瘤坏死因子-α、基质金属蛋白酶-8与胎膜早破早产及宫内感染的关系[J]. 中国妇幼保健, 2018, 33(7): 1463-5. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFYB201807007.htm [11] 向涛. 炎性因子检测在胎膜早破宫内感染中的价值探讨[J]. 上海医药, 2018, 39(5): 44-5, 63. doi: 10.3969/j.issn.1006-1533.2018.05.013 [12] 邢秋景, 李文丽, 徐发林. 妊娠期李斯特菌感染的临床特征及结局分析[J]. 河南医学研究, 2020, 29(8): 1372-4. doi: 10.3969/j.issn.1004-437X.2020.08.009 [13] 黄亚军, 孙佳, 赵艳丽. β-HCG、PCT、CRP、hs-CRP在胎膜早破中预测宫内感染的意义[J]. 中国医师杂志, 2020, 22(7): 1091-3. doi: 10.3760/cma.j.cn431274-20190428-00501 [14] 王慧, 高洁, 王菲. 早产胎膜早破孕妇血清中IL-6、TNF-α、sICAM- 1的水平及临床意义[J]. 贵州医药, 2019, 43(7): 1080-1. doi: 10.3969/j.issn.1000-744X.2019.07.027 [15] 赵雪琼, 贺艺, 艾鑫, 等. 产妇宫内感染影响因素及其与新生儿脑损伤的关系[J]. 中华医院感染学杂志, 2021, 31(18): 2816-20. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHYY202118022.htm [16] 李洁. 血清β-HCG hs-CRP IL-6联合检测对胎膜早破合并宫内感染的诊断价值分析[J]. 河北医学, 2019, 25(2): 182-6. doi: 10.3969/j.issn.1006-6233.2019.02.002 [17] 李小叶, 李德忠, 刘叶君. 白细胞介素及胎儿纤维连接蛋白水平对早产的预测价值[J]中国医师杂志, 2022, 24(1): 101-4. doi: 10.3760/cma.j.cn431274-20210104-00006 [18] 侯静, 樊珍. 早产儿脑损伤与脐带血中血清炎性因子的水平及产妇宫内感染的关系[J]. 当代医药论丛, 2022, 20(3): 51-3. [19] 欧婉婷, 雷克竞. PCT、IL-6、LBP预测胎膜早破早产儿宫内感染准确度比较[J]. 现代仪器与医疗, 2019, 25(3): 27-30. https://www.cnki.com.cn/Article/CJFDTOTAL-XDYI201903008.htm [20] 郭婕, 花少栋. 胎儿炎症反应综合征与新生儿脑部疾病[J]. 中国小儿急救医学, 2015, 22(7): 498-501. doi: 10.3760/cma.j.issn.1673-4912.2015.07.013 [21] 吴莉莉, 吕燕, 沈悦. 超声评估心肌做功指数和血流频谱对胎儿生长受限及妊娠结局的预测价值[J]. 中国临床研究, 2021, 34(8): 1039- 44. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGCK202108007.htm [22] 黎新艳, 庞彩英, 黄欢, 等. 早中孕期超声测量正常胎盘厚度Z-评分的研究[J]. 中国超声医学杂志, 2019, 35(11): 1015-8. doi: 10.3969/j.issn.1002-0101.2019.11.017 [23] 林雅茵, 林新祝, 李雅丹, 等. 脐血降钙素原、白细胞介素-6和C反应蛋白对新生儿宫内细菌感染的诊断价值[J]. 中国新生儿科杂志, 2014, 29(2): 98-101. https://www.cnki.com.cn/Article/CJFDTOTAL-HNYX202117032.htm [24] 严东琴, 谭琴, 林晓岚. PAPP-A联合HCG在先兆流产患者中的检测水平及与妊娠不良结局的相关性[J]. 中国临床研究, 2020, 33(2): 186-8, 193. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGCK202002012.htm [25] 杨春燕, 杨玉军, 李宝云, 等. 超敏C-反应蛋白与白蛋白比值对早产儿早发型感染的诊断价值[J]. 中华危重病急救医学, 2016(2): 173-7. doi: 10.3760/cma.j.issn.2095-4352.2016.02.017 -







 下载:
下载: