Application of transcranial Doppler ultrasound in cerebral hemodynamic monitoring and prognosis evaluation in patients with extracorporeal membrane pulmonary oxygenation
-
摘要:
目的 探讨经颅多普勒超声在体外膜肺氧合患者脑血流动力学监测及预后评估中的应用价值。 方法 回顾性分析2015年5月20日~2020年1月3日在本院87例进行体外膜肺氧合治疗患者的临床资料,比较患者治疗前后脑血流动力学指标[收缩峰值血流速度(Vs)、舒张期峰值流速(Vd)、平均血流速度(Vm)、搏动指数(PI)]和心功能指标[左心射血分数(LVEF)、左心室流出道血流速度时间积分(VTI)、平均动脉压(MAP)]。随访1年,统计患者的预后状态。依据其不同的预后状态分为预后良好组(n= 56)和预后不良组(n=31),比较两组性别、年龄、疾病分类、肾功能不全、肝功能异常、多器官衰竭、体外膜肺氧合流量、正性肌力药物评分(IS)、Vs、Vd、Vm、PI、LVEF、MAP水平。 结果 治疗前与治疗后Vs、Vd、Vm、PI值差异无统计学意义(P>0.05);体外膜肺氧合患者治疗后LVEF、MAP、VTI升高(P < 0.05);单因素分析结果显示,两组肾功能不全、多器官功能衰竭率及Vs、Vd、Vm、PI、LVEF、VTI、MAP值的差异有统计学意义(P < 0.05),两组性别、年龄、疾病分类、体外膜肺氧合流量及IS评分的差异无统计学意义(P>0.05);Logistics回归分析结果显示,肾功能不全、Vs、Vd、Vm、PI、MAP是影响体外膜肺氧合患者预后不良的独立危险因素(P < 0.05)。 结论 脑血流动力学指标(Vs、Vd、Vm、PI)与体外膜肺氧合患者预后有密切联系,临床需加强联合各指标检测,尽早评估体外膜肺氧合患者预后状态。 Abstract:Objective To investigate the application value of transcranial Doppler ultrasonography in cerebral hemodynamic monitoring and prognosis evaluation of patients with extracorporeal membrane oxygenation. Methods The clinical data of 87 patients who underwent extracorporeal membrane oxygenation in our hospital from May 20 th, 2015 to January 3 rd, 2020 were retrospectively analyzed. The indexes of cerebral hemodynamics[peak systolic blood flow velocity (Vs), peak diastolic flow velocity (Vd), mean blood flow velocity (Vm), pulsatility index (PI)] and cardiac function indicators [left ventricular ejection fraction (LVEF), left ventricular outflow tract blood flow velocity time integral (VTI), mean arterial pressure (MAP)] were compared before and after treatment. After 1 year of follow-up, the prognosis status of 87 patients was counted. According to their different prognostic status, they were divided into good prognosis group (n=56) and poor prognosis group (n=31). The gender, age, disease classification, renal insufficiency, abnormal liver function, multiple organ failure, extracorporeal membrane oxygenation flow, inotrope score, Vs, Vd, Vm, PI, LVEF, MAP levels were compared between two groups. Results There was no significant difference in Vs, Vd, Vm and PI values before and after treatment (P>0.05). After extracorporeal membrane oxygenation treatment, LVEF, MAP and VTI increased, and the difference was statistically significant (P < 0.05). Univariate analysis showed that there were statistically significant differences in the rates of renal insufficiency, multiple organ failure, and Vs, Vd, Vm, PI, LVEF, VTI and MAP values between the two groups (P < 0.05). There was no significant difference in gender, age, disease classification, extracorporeal membrane oxygenation flow and inotrope score between the two groups (P>0.05). Vs, Vd, Vm, PI and MAP were independent risk factors for poor prognosis in patients with extracorporeal membrane oxygenation (P < 0.05). Conclusion Cerebral hemodynamic indexes (Vs, Vd, Vm, PI) are closely related to the prognosis of patients with extracorporeal membrane oxygenation. It is necessary to strengthen the detection of various indicators in clinical practice to assess the prognosis of patients with extracorporeal membrane oxygenation as soon as possible. -
表 1 治疗前后脑血流动力学指标
Table 1. Cerebral hemodynamic indexes before and after treatment (n=87, Mean±SD)
时间 Vs(cm/s) Vd(cm/s) Vm(cm/s) PI 治疗前 45.25±7.89 29.49±5.19 32.46±7.15 0.41±0.12 治疗后 69.17±8.16 31.31±6.10 43.03±6.88 0.67±0.19 t 0.756 0.231 0.404 1.014 P 0.451 0.818 0.687 0.312 Vs: 收缩期峰值血流速度; Vd: 舒张期峰值血流速度; Vm: 平均血流速度; PI: 搏动指数. 表 2 治疗前后心功能及平均动脉压比较
Table 2. Comparison of cardiac function and mean arterial pressure before and after treatment (n=87, Mean±SD)
时间 LVEF(%) VTI(cm) MAP(mmHg) 治疗前 28.25±5.25 7.74±2.10 65.74±6.14 治疗后 49.48±6.24 13.71±3.45 71.33±8.48 t 12.845 11.463 9.571 P < 0.001 < 0.001 0.047 LVEF: 左室射血分数; VTI: 左室流出道速度时间积分; MAP: 平均动脉压. 表 3 影响体外膜肺氧合患者预后不良的单因素分析
Table 3. Univariate analysis of poor prognosis in patients with extracorporeal membrane oxygenation [n(%), Mean±SD]
因素 预后良好组(n=31) 预后不良组(n=56) χ2/t P 性别 0.748 0.387 男 17(54.84) 36(64.29) 女 14(45.16) 20(35.71) 年龄(岁) 52.67±6.16 52.19±5.51 0.373 0.710 疾病分类 0.013 0.910 心衰 17(54.84) 30(53.57) 心源性休克 14(45.16) 26(46.43) 肾功能不全 35.883 < 0.001 是 5(8.93) 22(70.97) 否 51(91.07) 9(29.03) 肝功能异常 2.338 0.126 是 10(32.26) 10(17.86) 否 21(67.74) 46(82.14) 多器官功能衰竭 是 12(38.71) 29(94.64) 33.042 < 0.001 否 19(61.29) 27(5.36) 体外膜肺氧合流量(L) 3.30±0.53 3.27±0.46 0.192 0.848 IS 5.23±0.79 5.11±0.70 0.731 0.467 Vs(cm/s) 42.21±7.62 48.36±8.46 3.361 0.001 Vd(cm/s) 14.82±4.31 18.69±5.54 3.364 0.001 Vm(cm/s) 44.79±6.77 48.27±6.94 2.259 0.003 PI 1.07±0.27 0.82±0.15 5.564 < 0.001 LVEF(%) 42.23±6.98 37.96±5.83 3.047 0.003 VTI(cm) 15.33±3.77 12.81±3.27 3.258 0.002 MAP(mmHg) 46.39±10.40 41.64±8.97 2.234 0.028 IS: 正性肌力药物评分. 表 4 影响体外膜肺氧合患者预后不良的Logistics回归分析
Table 4. Logistic regression analysis of poor prognosis in patients with extracorporeal membrane oxygenation
因素 β SE Wald χ2 P HR OR 95% Cl 下限 上限 肾功能不全 3.216 0.613 27.498 < 0.001 24.933 7.494 82.956 多器官功能衰竭 -0.928 0.512 3.280 0.070 0.070 0.395 1.079 Vs(cm/s) -0.083 0.029 8.362 0.004 0.921 0.870 0.974 Vd(cm/s) -0.186 0.055 11.432 0.001 0.830 0.745 0.925 Vm(cm/s) 0.103 0.043 5.772 0.016 1.109 1.019 1.206 PI 6.664 1.592 17.523 < 0.001 783.521 34.595 17 745.516 LVEF(%) -0.043 0.028 2.420 0.120 0.958 0.907 1.011 VTI(cm) -0.017 0.031 0.294 0.588 0.983 0.926 1.045 MAP(mmHg) 0.258 0.072 12.916 < 0.001 1.295 1.125 1.491 表 5 脑血流动力学指标对体外膜肺氧合患者预后不良的预测价值分析
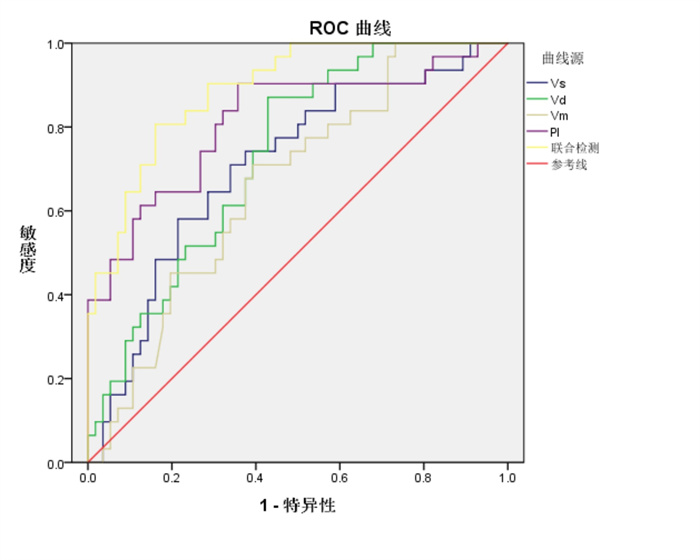
Table 5. Predictive value of cerebral hemodynamic indexes for poor prognosis in patients with extracorporeal membrane oxygenation
测因子 最佳临界值 敏感度 特异性 P AUC 95%CI 下限 上限 Vs 0.551 0.825 0.643 < 0.001 0.707 0.594 0.821 Vd 0.632 0.776 0.708 0.011 0.732 0.629 0.836 Vm 0.758 0.642 0.856 < 0.001 0.664 0.550 0.779 PI 0.434 0.804 0.723 < 0.001 0.814 0.714 0.914 联合检测 1.000 0.954 0.857 < 0.001 0.891 0.828 0.957 -
[1] 王晓存, 王红, 侯晓彤. 心脏手术患者体外膜肺氧合撤机后系统性炎症反应状况分析[J]. 心肺血管病杂志, 2020, 39(3): 291-5. doi: 10.3969/j.issn.1007-5062.2020.03.017 [2] 石秀茹, 郭远, 郑凯兰, 等. 1例危重型新型冠状病毒肺炎患者并发消化道出血应用体外膜肺氧合治疗的护理[J]. 中华护理杂志, 2020, 55 (S1): 675-7. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHHL2020S1279.htm [3] 唐绪荣, 聂谦, 赵珏, 等. 体外膜肺氧合联合主动脉内球囊反搏治疗急性心肌梗死合并心源性休克1例[J]. 中南医学科学杂志, 2020, 48 (3): 333-6. https://www.cnki.com.cn/Article/CJFDTOTAL-HYYY202003028.htm [4] Reimer A, Vogl H, Schmid S, et al. Klinische pharmakokinetik der antiinfektiva Bei extrakorporaler membranoxygenierung[J]. Der Anaesthesist, 2019, 68(12): 821-6. doi: 10.1007/s00101-019-00702-8 [5] Ramanathan K, Tan CS, Rycus P, et al. Extracorporeal membrane oxygenation in pregnancy: an analysis of the extracorporeal life support organization registry[J]. Crit Care Med, 2020, 48(5): 696- 703. doi: 10.1097/CCM.0000000000004269 [6] 边志杰, 刘傲飞, 刘云娥, 等. 前后循环颅内动脉重度狭窄或闭塞患者认知功能损害的比较[J]. 中华行为医学与脑科学杂志, 2020, 29(6): 506-10. doi: 10.3760/cma.j.cn371468-20191202-00867 [7] 陈妙莲, 钟涛, 谢林辉, 等. 彩色多普勒超声辅助下调整体外膜肺氧合参数对呼吸衰竭患者预后具有改善作用[J]. 分子影像学杂志, 2018, 41(3): 291-6. doi: 10.3969/j.issn.1674-4500.2018.03.02 [8] 韩凤君, 吴世新. 基层医院诊断舒张功能不全心衰的参考标准[J]. 临床荟萃, 1993, 8(S4): 854. https://www.cnki.com.cn/Article/CJFDTOTAL-LCFC1993Z4074.htm [9] 张松. 心源性休克诊治进展及指南解读[J]. 医学研究杂志, 2017, 46 (10): 1-3, 17. https://www.cnki.com.cn/Article/CJFDTOTAL-YXYZ201710003.htm [10] Zhang F, Liang Y, Chen XX, et al. Echocardiographic evaluation of left ventricular end diastolic pressure in patients with diastolic heart failure: a comparative study with real-time catheterization[J]. Medicine, 2020, 99(49): e22683. doi: 10.1097/MD.0000000000022683 [11] Chaves R, Rabello Filho R, Timenetsky KT, et al. Extracorporeal membrane oxygenation: a literature review[J]. Rev Bras Ter Intensiva, 2019, 31(3): 410-24. [12] 王淑芹, 张春艳, 孙兵, 等. 体外膜肺氧合支持心肺衰竭危重患者院际转运的应用研究进展[J]. 中国护理管理, 2019, 19(7): 1069-73. doi: 10.3969/j.issn.1672-1756.2019.07.023 [13] 邵程程, 王粮山, 王红, 等. 成人心脏术后心源性休克患者接受体外膜肺氧合辅助的临床结果荟萃分析[J]. 中国体外循环杂志, 2019, 17 (1): 4-7, 25. https://www.cnki.com.cn/Article/CJFDTOTAL-TWXH201901002.htm [14] 焦志欣, 李海欣, 杨丽萍, 等. 彩色多普勒超声成像与经颅多普勒超声成像联合检查对颈部血管狭窄的诊断价值[J]. 中国临床医生杂志, 2019, 47(2): 193-5. doi: 10.3969/j.issn.2095-8552.2019.02.020 [15] 郑家涛, 徐新禹. 颈动脉支架置入术对颈内动脉狭窄患者脑血管反应性及认知功能的影响[J]. 川北医学院学报, 2020, 35(6): 1037-9, 1050. doi: 10.3969/j.issn.1005-3697.2020.06.023 [16] 王巍, 马琳, 孙玉伟. 经颅多普勒超声与CTA在缺血性脑血管病诊断中的应用[J]. 中国超声医学杂志, 2019, 35(6): 481-4. doi: 10.3969/j.issn.1002-0101.2019.06.001 [17] Dar IA, Khan IR, Maddox RK, et al. Towards detection of brain injury using multimodal non-invasive neuromonitoring in adults undergoing extracorporeal membrane oxygenation[J]. Biomed Opt Express, 2020, 11(11): 6551-69. doi: 10.1364/BOE.401641 [18] 李剑平, 叶萍, 季勇, 等. 经颅多普勒超声联合血流速度检测在颈内动脉支架置入术后高灌注损伤中的应用[J]. 临床和实验医学杂志, 2021, 20(17): 1895-8. doi: 10.3969/j.issn.1671-4695.2021.17.030 [19] 鲍黎明, 刘新宾, 赵忠, 等. 体外膜肺氧合技术在心肺复苏中的应用体会[J]. 心肺血管病杂志, 2020, 39(8): 963-5. doi: 10.3969/j.issn.1007-5062.2020.08.017 [20] Bhagavan D, Padovano WM, Kovács SJ. Alternative diastolic function models of ventricular longitudinal filling velocity are mathematically identical[J]. Am J Physiol Heart Circ Physiol, 2020, 318(5): H1059-67. doi: 10.1152/ajpheart.00681.2019 [21] Simpson TF, Tyler JM, Thomas RC, et al. Mitral annular peak systolic and diastolic velocities are characteristic of healthy hearts: a Doppler tissue imaging study[J]. Echocardiography, 2019, 36(3): 433-8. doi: 10.1111/echo.14247 [22] 朱军, 李振鹏, 方开峰. 经颅彩色多普勒超声检查及血清胰岛素样生长因子-1、神经元特异性烯醇化酶检测在脑梗死病情评估中的应用价值[J]. 中国医师进修杂志, 2021, 44(4): 367-71. doi: 10.3760/cma.j.cn115455-20201001-01333 [23] 曾景, 林月雄, 金廷荣, 等. 基于脑功能监测指标构建预测心搏骤停行心肺复苏后自主循环恢复患者神经功能预后不良的多因素Logistic回归模型[J]. 实用心脑肺血管病杂志, 2021, 29(12): 28-34, 46. doi: 10.12114/j.issn.1008-5971.2021.00.257 -







 下载:
下载: