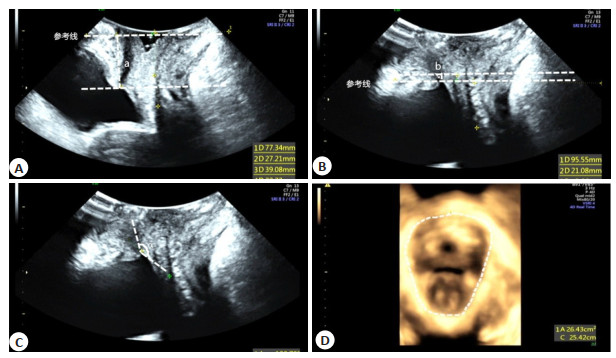
Transperineal color Doppler ultrasound parameters of women with postpartum stress urinary incontinence and effect of pelvic floor biofeedback electrical stimulation
-
摘要:
目的 采用经会阴彩色多谱勒超声评估女性产后压力性尿失禁(SUI)患者盆底生物电反馈刺激治疗的盆底超声参数特征及效果。 方法 选择2019年1月~2021年10月本院收治的120例产后SUI女性作为研究对象,按随机数字表法分为治疗组与对照组,60例/组。对照组予常规健康教育和产后保健,治疗组予盆底生物电反馈刺激治疗。于治疗前及治疗后3月对两组患者进行1 h尿垫试验、盆底超声参数测量和生活质量问卷评估,比较两组治疗有效率、治疗前后膀胱残余尿量、漏尿次数及漏尿量。 结果 治疗组总有效率较对照组更高(95.00% vs 81.67%,P < 0.05);治疗后,两组膀胱颈移动度、膀胱最低点位置、膀胱后角、肛提肌裂孔面积、膀胱残余尿量、漏尿次数、漏尿量、国际尿失禁咨询委员会尿失禁问卷简表(ICIQ-SF)及尿失禁影响问卷简表(IIQ-7)评分较治疗前降低,肛提肌厚度升高(P < 0.05);治疗组治疗后膀胱颈移动度、膀胱最低点位置、膀胱后角、肛提肌裂孔面积、膀胱残余尿量、漏尿次数、漏尿量、ICIQ-SF及IIQ-7评分低于对照组,肛提肌厚度高于对照组(P < 0.05)。 结论 女性产后SUI患者采用盆底生物电反馈刺激治疗可提升疗效,改善患者盆底功能,减轻SUI症状;采用经会阴彩色多谱勒超声检查能为SUI患者盆底功能损伤和康复提供客观评价指标。 Abstract:Objective To evaluate the transperineal color Doppler ultrasound parameters of women with postpartum stress urinary incontinence (SUI), and the effect of pelvic floor biofeedback electrical stimulation. Methods A total of 120 women with postpartum SUI admitted to the hospital from January 2019 to October 2021 were selected. They were divided into treatment group and control group by random number table method, with 60 cases in each group. The control group was treated with routine health education and postpartum health care. The treatment group was treated with biofeedback electrical stimulation. 1-hour pad test was conducted, pelvic floor ultrasound parameters were measured, and quality of life was evaluated before treatment and after 3 months of treatment. The treatment response rate, residual urine volume before and after treatment, frequency and volume of urine leakage were compared between the two groups. Results The total response rate of treatment group was higher than control group (95.00% vs 81.67%, P < 0.05). After treatment, the bladder neck descent, bladder lowest descent, retrovesical angle, levator hiatus area, residual urine volume, frequency and volume of urine leakage, the International Consultation Incontinence Questionnaire Short-Form (ICIQ-SF) scores and the Incontinence Impact Questionnaire (IIQ-7) scores were reduced, while levator thickness was increased in the two groups (P < 0.05). After treatment, bladder neck descent, bladder lowest descent, retrovesical angle, levator hiatus area, residual urine volume, frequency and volume of urine leakage, the ICIQ-SF scores and IIQ-7 scores of treatment group were smaller/lower than those of the control group, and levator thickness was larger than that of the control group (P < 0.05). Conclusion Applying pelvic floor biofeedback electrical stimulation to women with postpartum SUI can improve the curative effect and pelvic floor function, relieve symptoms of SUI. Transperineal color Doppler ultrasonography can provide objective evaluation indicators for pelvic floor function damage and rehabilitation in SUI patients. -
表 1 两组患者一般资料比较
Table 1. Comparison of general data between the two groups (n=60, Mean±SD)
组别 年龄(岁) BMl(kg/m2) 分娩孕周(周) 第二产程延长[n(%)] 受教育时间(年) 治疗组 31.10±5.29 22.34±3.27 39.12±1.56 23(38.33) 12.35±3.19 对照组 30.97±5.14 21.49±3.50 38.58±2.00 25(41.67) 12.74±3.51 t/χ2 0.137 1.375 1.649 0.139 0.392 P 0.892 0.172 0.102 0.709 0.696 表 2 两组患者的疗效比较
Table 2. Comparison of curative effect between the two groups [n=60, n(%)]
组别 治愈 好转 无效 总有效 治疗组 32(53.33) 25(41.67) 3(5.00) 57(95.00) 对照组 22(36.67) 27(45.00) 11(18.33) 49(81.67) χ2 5.175 P 0.023 表 3 两组治疗前后盆底超声参数比较
Table 3. Comparison of pelvic floor ultrasound parameters between the two groups before and after treatment (n=60, Mean±SD)
时间 组别 BND(mm) BLD(mm) RVA(°) T(mm) LHA(cm2) 治疗前 治疗组 33.85±5.17 27.35±7.10 144.35±12.30 10.75±2.21 29.26±4.61 对照组 34.19±5.32 27.69±6.88 145.53±12.36 10.23±2.00 30.53±4.13 t 0.355 0.266 0.524 1.351 1.525 P 0.723 0.790 0.601 0.179 0.130 治疗后 治疗组 27.96±4.07* 21.23±5.68* 124.59±10.12* 15.41±4.43* 21.63±4.35* 对照组 33.57±4.98* 25.24±6.17* 132.42±11.54* 13.24±3.70* 25.59±4.41* t 6.756 3.704 3.952 2.912 4.952 P < 0.001 < 0.001 < 0.001 0.004 < 0.001 *P < 0.05 vs同组治疗前. BND: 膀胱颈移动度; BLD: 膀胱最低点位置; RVA: 膀胱后角; T: 肛提肌厚度; LHA: 肛提肌裂孔面积. 表 4 两组治疗前后膀胱残余尿量、漏尿次数及漏尿量比较
Table 4. Comparison of residual urine volume, urinary leakage frequency and leakage volume between the two groups before and after treatment (n=60, Mean±SD)
时间 组别 膀胱残余尿量(mL) 漏尿次数(d) 漏尿量(mL) 治疗前 治疗组 69.58±20.14 5.75±1.23 10.95±2.69 对照组 68.71±21.25 6.09±1.10 10.53±2.71 t 0.230 1.596 0.852 P 0.818 0.113 0.396 治疗后 治疗组 16.31±5.07* 0.98±0.31* 1.07±0.26* 对照组 28.19±6.65* 1.67±0.59* 1.79±0.43* t 11.004 8.019 11.099 P < 0.001 < 0.001 < 0.001 *P < 0.05 vs同组治疗前. 表 5 两组治疗前后ICIQ-SF、IIQ-7评分比较
Table 5. Comparison of ICIQ- SF scores and IIQ- 7 scores between the two groups before and after treatment (point, n=60, Mean±SD)
时间 组别 ICIQ-SF评分 IIQ-7评分 治疗前 治疗组 12.56±2.60 10.67±2.38 对照组 12.70±2.49 10.29±2.46 t 0.301 0.860 P 0.764 0.392 治疗后 治疗组 3.09±0.81* 1.78±0.56* 对照组 4.27±1.12* 2.43±0.60* t 6.613 6.135 P < 0.001 < 0.001 *P < 0.05 vs同组治疗前. ICIQ-SF: 国际尿失禁咨询委员会尿失禁问卷简表; IIQ-7: 尿失禁影响问卷简表. -
[1] Preda A, Moreira S. Stress urinary incontinence and female sexual dysfunction: the role of pelvic floor rehabilitation[J]. Acta Med Portuguesa, 2019, 32(11): 721-6. doi: 10.20344/amp.12012 [2] Wang K, Xu XL, Jia GM, et al. Risk factors for postpartum stress urinary incontinence: a systematic review and meta-analysis[J]. Reprod Sci, 2020, 27(12): 2129-45. doi: 10.1007/s43032-020-00254-y [3] 刘成成, 金永红, 左冬梅, 等. 三维盆底超声可动态观察初产妇早期盆底结构及功能的变化[J]. 分子影像学杂志, 2021, 44(5): 733-8. doi: 10.12122/j.issn.1674-4500.2021.05.01 [4] Nunes EFC, Sampaio LMM, Biasotto-Gonzalez DA, et al. Biofeedback for pelvic floor muscle training in women with stress urinary incontinence: a systematic review with meta-analysis[J]. Physiotherapy, 2019, 105(1): 10-23. doi: 10.1016/j.physio.2018.07.012 [5] 李霞, 庞稼燕. 肌电刺激联合生物反馈盆底肌训练治疗女性轻中度压力性尿失禁的临床观察[J]. 中国临床研究, 2015, 28(1): 80-1. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGCK201501031.htm [6] Liu D, Adams M, Burdette EC, et al. Dual-sectored transurethral ultrasound for thermal treatment of stress urinary incontinence: in silico studies in 3D anatomical models[J]. Med Biol Eng Comput, 2020, 58(6): 1325-40. doi: 10.1007/s11517-020-02152-6 [7] 中华医学会妇产科学分会妇科盆底学组. 女性压力性尿失禁诊断和治疗指南(试行[) J]. 中华妇产科杂志, 2011, 46(10): 796-8. doi: 10.3760/cma.j.issn.0529-567x.2011.10.023 [8] 蔡文智, 张焱, 陈玲, 等. 电刺激联合生物反馈治疗初产妇和经产妇压力性尿失禁的疗效观察[J]. 中国康复医学杂志, 2020, 35(2): 141- 5, 150. doi: 10.3969/j.issn.1001-1242.2020.02.003 [9] Lin YH, Chang SD, Hsieh WC, et al. Persistent stress urinary incontinence during pregnancy and one year after delivery; its prevalence, risk factors and impact on quality of life in Taiwanese women: an observational cohort study[J]. Taiwan J Obstet Gynecol, 2018, 57(3): 340-5. doi: 10.1016/j.tjog.2018.04.003 [10] 王元毅, 轩留明, 王勤章. 中国女性压力性尿失禁危险因素的Meta分析[J]. 中国临床研究, 2021, 34(7): 865-71. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGCK202107001.htm [11] 杨明丽, 王青, 于晓杰, 等. 5143例产后早期妇女的盆底功能状况及其影响因素分析[J]. 中华妇产科杂志, 2019, 54(8): 522-6. doi: 10.3760/cma.j.issn.0529-567x.2019.08.004 [12] Shobeiri SA, Kerkhof MH, Minassian VA, et al. IUGA committee opinion: laser- based vaginal devices for treatment of stress urinary incontinence, genitourinary syndrome of menopause, and vaginal laxity[J]. Int Urogynecol J, 2019, 30(3): 371-6. doi: 10.1007/s00192-018-3830-0 [13] 刘良乐, 戴鸣海, 叶秀芝, 等. 盆底电生物反馈法治疗中老年颈部脊髓损伤患者术后排尿困难的疗效研究[J]. 中国全科医学, 2019, 22 (11): 1359-63. https://www.cnki.com.cn/Article/CJFDTOTAL-QKYX201911030.htm [14] 卢惠苹, 卢萍丹, 陈昕, 等. 盆底肌生物反馈刺激治疗脊髓损伤排尿功能障碍的疗效[J]. 中国临床研究, 2020, 33(1): 80-3, 87. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGCK202001019.htm [15] Zhong FL, Miao WB, Yu ZX, et al. Clinical effect of electrical stimulation biofeedback therapy combined with pelvic floor functional exercise on postpartum pelvic organ prolapse[J]. Am J Transl Res, 2021, 13(6): 6629-37. [16] 蒋惠瑜, 黄亚莲. 盆底肌功能锻炼联合肌电刺激对产后盆底功能障碍患者功能恢复及生活质量的影响[J]. 山东医药, 2018, 58(17): 75-7. https://www.cnki.com.cn/Article/CJFDTOTAL-SDYY201817024.htm [17] 尹蕊, 胡兵. 超声和临床诊断女性压力性尿失禁进展[J]. 中国医学影像技术, 2019, 35(8): 1260-3. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYXX201908049.htm [18] 郑兰英, 吴羽, 辜莉, 等. 经会阴盆底超声智能识别及自动测量软件量化评价膀胱后壁脱垂的初步研究[J]. 中国超声医学杂志, 2019, 35 (6): 547-50. doi: 10.3969/j.issn.1002-0101.2019.06.022 [19] 李文婷, 李淑萍, 王英红. 经会阴超声动态观察孕期及分娩后早期盆底结构的变化[J]. 重庆医学, 2019, 48(10): 1674-6, 1682. doi: 10.3969/j.issn.1671-8348.2019.10.013 [20] Aalaie B, Tavana B, Rezasoltani Z, et al. Biofeedback versus electrical stimulation for sexual dysfunction: a randomized clinical trial[J]. Int Urogynecol J, 2021, 32(5): 1195-203. doi: 10.1007/s00192-020-04373-7 [21] Moore IS, James ML, Brockwell E, et al. Multidisciplinary, biopsychosocial factors contributing to return to running and running related stress urinary incontinence in postpartum women[J]. Br J Sports Med, 2021, 55(22): 1286-92. [22] 周勋琦, 邓乙首, 李丹, 等. 基于电诊断评估的产后压力性尿失禁综合康复治疗临床疗效观察[J]. 中国康复医学杂志, 2021, 36(5): 553-8. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGKF202105009.htm -







 下载:
下载: