MRI texture feature on breast cancer vascular invasion assessment and missing histological information imputation
-
摘要:
目的 探讨MRI纹理特征评估浸润性乳腺癌脉管浸润的价值,及其对缺失的乳腺癌分子分型和细胞角蛋白5/6基因表达信息的填充。 方法 将114例接受MRI检查并经病理确诊为乳腺癌的患者分为训练组(n=51)、内部验证组(n=30)、外部验证组(n=33)。根据临床病理特征与MRI征象观察脉管浸润独立危险因素,构建MRI征象模型和纹理特征模型,评估2种模型的诊断效能估。采取交叉验证支持向量机递归特征消除法进行纹理特征选择,结合乳腺癌患者病理信息,建立非负矩阵分解(NMF)模型与协同过滤模型,采取受试者工作特征曲线进行模型填充性能评价。 结果 3组患者瘤周胸肌前水肿、淋巴结转移状态差异具有统计学意义(P < 0.05),是影响脉管浸润的独立危险因素。纹理特征模型诊断乳腺癌脉管浸润的曲线下面积高于MRI征象模型(P < 0.05)。在缺失率为20%~40%时,NMF法的曲线下面积高于协同过滤法(P < 0.05);在特征数为140时,NMF模型的曲线下面积高于协同过滤模型(P < 0.05)。使用影像组学特征NMF模型的曲线下面积高于不使用影像组学特征NMF模型(P < 0.05)。 结论 MRI纹理特征可在术前有效预测乳腺癌脉管浸润,填充缺失的分子分型以及细胞角蛋白5/6基因表达信息。 Abstract:Objective To explore the value of MRI texture features in evaluating the vascular infiltration of invasive breast cancer, as well as the missing molecular typing and cytokeratin 5/6 gene expression information imputation. Methods A total of 114 patients with breast cancer diagnosed by MRI and pathology were divided into training group (n=51), internal validation group (n=30) and external validation group (n=33). According to the clinicopathological features and MRI texture features, the independent risk factors of vascular infiltration were observed, the MRI sign model and texture feature model were constructed and their diagnostic efficacy was compared. Non-negative matrix decomposition (NMF) and collaborative filtering imputation models were established with the texture features selected by cross-validation support vector machine recursive feature elimination, and pathological information of breast cancer patients. The receiver operating characteristic curve was used to evaluate their imputation performance. Results There were statistically significant differences in peritumor prethoracic edema and lymph node metastasis status, which were independent risk factors for vascular invasion (P < 0.05). The area under the curve (AUC) of the texture feature model in diagnosis of breast cancer vascular invasion was higher than that of MRI model (P < 0.05). When the loss rate was 20%- 40%, the AUC of NMF was higher than that of collaborative filtering (P < 0.05). When the feature number was 140, the AUC of NMF was higher than that of collaborative filtering (P < 0.05). The AUC of NMF with image omics was higher than that of NMF without image omics (P < 0.05). Conclusion MRI texture features can effectively predict breast cancer vascular invasion before surgery, and fill in missing molecular typing and cytokeratin 5/6 gene expression information. -
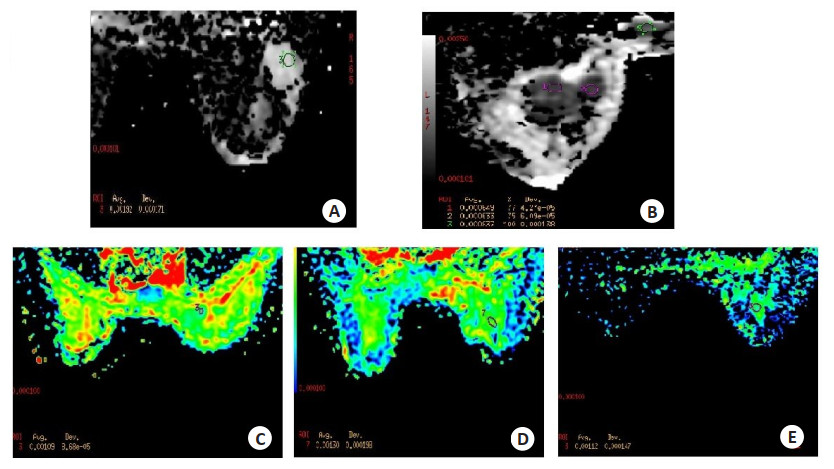
图 1 不同乳腺癌病理类型T2WI信号下的ADC值表现
A: 女性, 54岁, 诊断为右乳粘液癌, ADC值较高, 约1.92×10-3 mm2/s; B: 女性, 57岁, 诊断为左乳浸润性导管癌, ADC值低, 约0.63~0.83×103 mm2/s; C: 女性, 33岁, 诊断为右乳浸润性导管癌合并高级别导管内癌, ADC值低, 约1.09×103 mm2/s; D: 女性, 52岁, 诊断为右乳浸润性微乳头状癌, ADC值稍低, 约1.30×103 mm2/s; E: 女性, 54岁, 诊断为高级别导管原位癌并伴局部微浸润, ADC值低, 约1.12×103 mm2/s.
Figure 1. ADC value under T2WI signal of different pathological types of breast cancer.
表 1 3组患者MRI特征比较
Table 1. Comparison of MRI features of three groups [n(%)]
指标 训练组(n=51) 内部验证组(n=30) 外部验证组(n=33) 脉管浸润阳性(n=25) 脉管浸润阴性(n=26) P 脉管浸润阳性(n=12) 脉管浸润阴性(n=18) P 脉管浸润阳性(n=13) 脉管浸润阴性(n=20) P 年龄(岁, Mean±SD) 51.24±5.25 49.34±5.42 0.226 51.54±5.19 49.07±5.75 0.128 51.05±5.22 49.82±5.56 0.746 肿瘤直径(cm, Mean±SD) 2.74±0.62 2.56±0.64 0.330 2.66±0.61 2.51±0.58 0.388 2.58±0.64 2.49±0.57 0.282 淋巴结转移 0.005 0.035 0.027 是 16 6 8 5 9 6 否 9 20 4 13 4 14 瘤周胸肌前水肿 0.034 0.025 0.037 是 17 11 9 6 10 8 否 8 15 3 12 3 12 强化方式 0.265 0.765 0.435 均匀 11 16 6 10 6 12 非均匀 14 10 6 8 7 8 病灶类型 0.446 0.367 0.829 肿块 10 12 4 9 6 10 0.746 非肿块 15 14 8 9 7 10 0.282 表 2 MRI征象模型、纹理特征模型诊断效能分析
Table 2. Analysis of diagnostic efficacy of MRI sign model and texture feature model
模型 训练组 内部验证组 外部验证组 AUC 95% CI AUC 95% CI AUC 95% CI MRI征象模型 0.774 0.626~0.923 0.769 0.589~0.948 0.773 0.598~0.945 纹理特征模型 0.846 0.726~0.967 0.847 0.682~0.995 0.852 0.722~0.951 Z 3.125 3.835 2.886 P < 0.001 < 0.001 < 0.001 AUC: 曲线下面积. 表 3 不同缺失率病理信息填充结果
Table 3. Filling results of pathological information with different deletion rates
缺失率(%) NMF法 CF法 P AUC 95% CI AUC 95% CI 10 0.764 0.625~0.892 0.728 0.565~0.844 0.058 15 0.754 0.612~0.887 0.702 0.642~0.825 0.062 20 0.745 0.625~0.844 0.672 0.605~0.764 0.034 25 0.732 0.608~0.815 0.624 0.518~0.723 0.006 30 0.713 0.628~0.802 0.635 0.534~0.735 0.038 35 0.695 0.602~0.785 0.594 0.504~0.683 0.008 40 0.672 0.596~0.724 0.571 0.502~0.664 0.014 NMF: 非负矩阵分解; CF: 协同过滤. 表 4 不同特征数病理信息填充结果分析
Table 4. Analysis of filling results of pathological information with different characteristic numbers
特征数 NMF法 CF法 P AUC 95% CI AUC 95% CI 40 0.755 0.645~0.862 0.722 0.615~0.834 0.054 60 0.764 0.652~0.867 0.712 0.602~0.826 0.066 80 0.776 0.665~0.854 0.738 0.645~0.814 0.074 100 0.744 0.638~0.855 0.708 0.618~0.827 0.106 120 0.763 0.648~0.882 0.705 0.614~0.831 0.056 140 0.790 0.682~0.905 0.712 0.604~0.823 0.038 160 0.772 0.665~0.884 0.711 0.592~0.837 0.066 180 0.742 0.623~0.862 0.702 0.585~0.814 0.056 200 0.778 0.658~0.891 0.715 0.605~0.828 0.071 表 5 使用和不使用影像特征的填充结果
Table 5. Filling results with and without image feature
缺失率(%) 使用影像组学特征NMF模型 不使用影像组学特征NMF模型 P AUC 95% CI AUC 95% CI 10 0.764 0.625~0.892 0.678 0.535~0.814 0.018 15 0.754 0.612~0.887 0.662 0.634~0.792 0.022 20 0.745 0.625~0.844 0.634 0.585~0.771 0.008 25 0.732 0.608~0.815 0.609 0.508~0.713 0.012 30 0.713 0.628~0.802 0.595 0.494~0.705 0.010 35 0.695 0.602~0.785 0.584 0.486~0.673 0.015 40 0.672 0.596~0.724 0.562 0.472~0.638 0.020 -
[1] 陶咏, 李晓兵, 李跃华, 等. 不同影像学检查对乳腺癌患者术前肿瘤大小准确度的临床研究[J]. 中国医学计算机成像杂志, 2019, 25(3): 252-5. doi: 10.3969/j.issn.1006-5741.2019.03.008 [2] 张静, 甘旭, 陈微微. 术前影像学指标预测乳腺癌模型的构建与评价[J]. 中华肿瘤防治杂志, 2020, 27(20): 1664-8. https://www.cnki.com.cn/Article/CJFDTOTAL-QLZL202020011.htm [3] 刘青, 张英, 周馨, 等. 2009-2018年北京地区单中心乳腺癌临床流行病学及病理特征回顾性分析[J]. 肿瘤, 2020, 40(6): 431-9. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLL202006006.htm [4] 杨丽洁, 杨铁成, 石丽稳, 等. 基于生物信息学分析筛选三阴性乳腺癌相关的预后标志物[J]. 中华实验外科杂志, 2020, 37(8): 1505-8. doi: 10.3760/cma.j.cn421213-20200224-01073 [5] 张晓宁, 孔祥真, 罗传文, 等. 用于样本聚类和网络分析的整合鲁棒结构化NMF模型[J]. 应用科学学报, 2020, 38(5): 825-42. doi: 10.3969/j.issn.0255-8297.2020.05.012 [6] Pan JJ, Gillis N. Generalized separable nonnegative matrix factorization[J]. IEEE Trans Pattern Anal Mach Intell, 2021, 43(5): 1546-61. doi: 10.1109/TPAMI.2019.2956046 [7] 陈洁文, 李姣, 马微妹, 等. 早期浸润性乳腺癌腋窝淋巴结转移与术前MRI及临床病理特征的相关性分析[J]. 中国临床医学影像杂志, 2020, 31(9): 618-23, 654. https://www.cnki.com.cn/Article/CJFDTOTAL-LYYX202009005.htm [8] Sukumar J, Gast K, Quiroga D, et al. Triple-negative breast cancer: promising prognostic biomarkers currently in development[J]. Expert RevAnticancer Ther, 2021, 21(2): 135-48. doi: 10.1080/14737140.2021.1840984 [9] 于晓军, 陈永升, 王春艳, 等. MRI表现及ADC直方图对预测乳腺浸润性导管癌脉管浸润的价值[J]. 临床放射学杂志, 2020, 39(2): 294-8. https://www.cnki.com.cn/Article/CJFDTOTAL-LCFS202002017.htm [10] 牟方胜, 陈莉, 陈垚, 等. 乳腺癌的MRI间接征象与淋巴结转移相关性[J]. 放射学实践, 2019, 34(6): 635-9. https://www.cnki.com.cn/Article/CJFDTOTAL-FSXS201906008.htm [11] Uematsu T. Focal breast edema associated with malignancy on T2- weighted images of breast MRI: peritumoral edema, prepectoral edema, and subcutaneous edema[J]. Breast Cancer, 2015, 22(1): 66- 70. doi: 10.1007/s12282-014-0572-9 [12] 刘壮盛, 李昌林, 衣利磊, 等. MRI纹理特征分析预测浸润性乳腺癌脉管浸润[J]. 中国医学影像技术, 2020, 36(11): 1637-42. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYXX202011011.htm [13] 薛珂, 丁莹莹, 李振辉, 等. 利用磁共振成像动态增强纹理特征预测不同分子亚型乳腺癌[J]. 实用放射学杂志, 2020, 36(8): 1235-9. doi: 10.3969/j.issn.1002-1671.2020.08.015 [14] 姚家炳. 乳腺癌患者脉管癌栓与临床病理特征及预后关系的研究[D]. 郑州: 郑州大学, 2018. [15] 刘恒, 王钢乐, 董懿, 等. 原发性浸润性乳腺癌患者发生脉管浸润的相关危险因素分析[J]. 癌症进展, 2019, 17(15): 1821-3. https://www.cnki.com.cn/Article/CJFDTOTAL-AZJZ201915024.htm [16] 李艳生, 刘园, 张毅. 基于感知掩蔽的重构非负矩阵分解单通道语音增强算法[J]. 计算机应用, 2019, 39(3): 894-8. https://www.cnki.com.cn/Article/CJFDTOTAL-JSJY201903046.htm [17] 何亚琼, 朱晓军. 深度协同过滤算法实现药物-靶标关系预测[J]. 计算机工程与设计, 2020, 41(8): 2195-200. https://www.cnki.com.cn/Article/CJFDTOTAL-SJSJ202008017.htm [18] 胡金月, 孙永强. 脉管癌栓与激素受体阳性乳腺癌患者临床病理特征及预后的关系[J]. 临床医学研究与实践, 2019, 4(35): 33-5. https://www.cnki.com.cn/Article/CJFDTOTAL-YLYS201935014.htm [19] 付振宇, 范明, 厉力华. 基于DCE-MRI影像组学非负矩阵分解的乳腺癌病理信息缺失填充研究[J]. 中国生物医学工程学报, 2021, 40 (4): 401-9. doi: 10.3969/j.issn.0258-8021.2021.04.03 [20] 吴佩琪, 刘再毅, 梁长虹. 基于MRI的影像组学特征在鉴别乳腺浸润性导管癌病理分级中的价值[J]. 医学研究生学报, 2018, 31(9): 938- 42. https://www.cnki.com.cn/Article/CJFDTOTAL-JLYB201809009.htm [21] 范丽娟, 王嘉, 高雪, 等. 脉管癌栓中间质细胞/癌细胞、巨噬细胞/癌细胞比值与pT1~4N1~3M0期乳腺癌患者临床病理特征及预后的关系[J]. 中华乳腺病杂志: 电子版, 2020, 14(1): 23-31. doi: 10.3877/cma.j.issn.1674-0807.2020.01.008 [22] Han M, Qi YN, Cui XX, et al. Texture analysis of computed tomography images in the lung of patients with breast cancer[J]. J ComputAssist Tomogr, 2021, 45(6): 837-42. doi: 10.1097/RCT.0000000000001198 [23] Song SE, Seo BK, Cho KR, et al. Prediction of inflammatory breast cancer survival outcomes using computed tomography-based texture analysis[J]. Front Bioeng Biotechnol, 2021, 9: 695305. doi: 10.3389/fbioe.2021.695305 [24] Song LR, Li CL, Yin JD. Texture analysis using semiquantitative kinetic parameter maps from DCE-MRI: preoperative prediction of HER2 status in breast cancer[J]. Front Oncol, 2021, 11: 675160. doi: 10.3389/fonc.2021.675160 -







 下载:
下载: