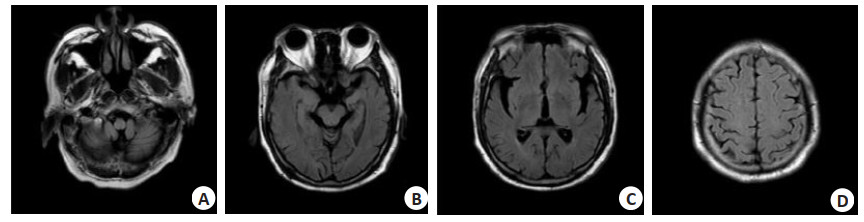
Correlation of carotid artery color Doppler ultrasound examination indexes, white matter lesions and cognitive function changes
-
摘要:
目的 探讨双侧颈动脉内膜-中层厚度、斑块的数量和狭窄程度与脑白质病变(WML)及认知功能改变的相关性。 方法 纳入2020年1月~2021年1月就诊于连云港市第一人民医院神经内科的146例患者作为研究对象,其中73例WML患者作为WML组,73例非WML患者作为非WML组,采取前瞻性观察性队列研究方法,对患者进行认知功能评分、颈部血管彩超、头颅MRI的WML程度评分,分析颈动脉病变各指标与WML程度量表评分、认知功能量表评分的关联性,探索颈动脉病变与WML和认知功能障碍的关系。 结果 WML组患者颈动脉内膜-中层厚度、斑块的数量总分和狭窄程度总分高于非WML组(1.97± 0.83 mm vs 0.87±0.12 mm,6±3.28分vs 4±1.96分,4.83±1.17分vs 2.89±1.05分,P < 0.05);WML组患者MoCA量表评分高于非WML组(18±6.82分vs 10±5.67分,P < 0.01)。对WML组患者颈动脉彩超指标与WML程度评分的相关性分析发现,WML组患者颈动脉内膜-中层厚度(r=0.828,P=0.020)、狭窄程度(r=0.897,P=0.010)和WML程度评分相关;而斑块的数量和WML程度评分之间无相关关系(P > 0.05)。对WML组患者颈动脉彩超指标与MoCA评分的相关性分析发现,WML组患者颈动脉内膜-中层厚度(r=-0.793,P=0.020)、狭窄程度(r=-0.873,P=0.010)和MoCA量表评分相关,而斑块的数量和MoCA评分不相关(P > 0.05)。WML组患者MoCA量表评分与WML程度评分呈负相关(r=-0.837,P < 0.01)。 结论 颈部血管彩超的颈动脉内膜-中层厚度以及血管狭窄程度与WML程度、认知功能障碍相关,WML程度与认知功能障碍程度呈负相关,颈动脉彩超对于临床诊断和预测WML和认知功能障碍具有一定的指导作用。 Abstract:Objective To investigate the correlation between the intima-media thickness of the bilateral carotid arteries, the number of plaques and the degree of stenosis, white matter lesions (WHL) and cognitive function changes. Methods A total of 146 patients in our hospital from January 2020 to January 2021 were selected. Among the patients, 73 patients with WHL were treated as WHL group, and 73 non-WHL patients were treated as non-WHL group. For patients with WHL, a prospective observational cohort study method was performed. Cognitive function scores, cervical vascular color Doppler ultrasound, and head MRI WHL were scored for each case, and various indicators of carotid artery lesions and WHL scales were analyzed. The correlation between score and cognitive function scale score, to explore the relationship between carotid artery disease and WHL and cognitive dysfunction. Results The intima-media thickness, total number of plaque points and total stenosis degree points in WML group were higher than those in non-WML group (1.97±0.83 mm vs 0.87±0.12 mm, 6±3.28 vs 4±1.96, 4.83±1.17 vs 2.89±1.05, P < 0.05). The MoCA score of WML group was significantly higher than that of non-WML group (18±6.82 vs 10±5.67, P < 0.01). The correlation analysis of carotid artery color doppler ultrasound index and WML degree score showed that carotid intima-media thickness (r=0.828, P=0.020), stenosis degree (r=0.897, P=0.010) and WML degree score were correlated. The number of plaques and the WML degree showed no correlation (P > 0.05). The correlation analysis of carotid artery color doppler ultrasound index and MoCA score in the WML group showed that intima-media thickness (r=-0.793, P=0.020), stenosis degree (r=-0.873, P=0.010) and MoCA scale score were correlated in the WML group. There was no correlation between plaque number and MoCA score (P > 0.05). The correlation analysis of the MoCA scale score and the WHL degree score of the WHL group showed that the MoCA scale score and the WHL degree score of the WHL group were negatively correlated (r=-0.837, P < 0.01). Conclusion The carotid intima-media thickness and the degree of vascular stenosis of cervical vascular color Doppler ultrasound are related to the degree of WHL and cognitive dysfunction. The degree of WHL is negatively correlated with the degree of cognitive dysfunction. Carotid artery color Doppler ultrasound is useful for clinical diagnosis. And predict WML and cognitive dysfunction has a certain guiding role. -
表 1 两组颈动脉内膜-中层厚度、斑块的数量和狭窄程度及MoCA量表评分比较
Table 1. Comparison of carotid intima-media thickness, plaque number and degree of stenosis and MoCA score between two groups (n=73, Mean±SD)
组别 颈动脉内膜-中层厚度(mm) 斑块的数量总分 狭窄程度总分 MoCA量表评分 WML组 1.97±0.83 6±3.28 4.83±1.17 18±6.82 非WML组 0.87±0.12 4±1.96 2.89±1.05 10±5.67 t 8.70 15.34 10.58 7.89 P 0.010 0.040 0.020 < 0.01 WML: 脑白质病变. 表 2 WML患者颈动脉彩超指标与WML程度的相关性
Table 2. Correlation between carotid artery color Doppler ultrasound and white matter damage in WML patients
项目 r P 颈动脉内膜-中层厚度 0.828 0.020 斑块的数量 0.162 0.203 颈动脉狭窄程度 0.897 0.010 表 3 WML患者颈动脉彩超指标与MoCA评分的相关性
Table 3. Correlation between carotid artery color Doppler ultrasound and MoCA score in WML patients
项目 r P 颈动脉内膜-中层厚度 -0.793 0.020 斑块的数量 0.089 0.360 颈动脉狭窄程度 -0.873 0.010 -
[1] Nakao S, Yamamoto T, Kimura S, et al. Brain white matter lesions and postoperative cognitive dysfunction: a review[J]. J Anesth, 2019, 33(2): 336-40. doi: 10.1007/s00540-019-02613-9 [2] Srikanth V, Sinclair AJ, Hill-Briggs F, et al. Type 2 diabetes and cognitive dysfunction-towards effective management of both comorbidities[J]. Lancet Diabetes Endocrinol, 2020, 8(6): 535-45. doi: 10.1016/S2213-8587(20)30118-2 [3] Vista FP 4th, Ngo MT, Cho SB, et al. Carotid artery plaque identification and display system (MRI-CAPIDS) using opensource tools[J]. Diagnostics (Basel), 2020, 10(12): 1111. doi: 10.3390/diagnostics10121111 [4] Murray CSG, Nahar T, Kalashyan H, et al. Ultrasound assessment of carotid arteries: current concepts, methodologies, diagnostic criteria, and technological advancements[J]. Echocardiography, 2018, 35 (12): 2079-91. doi: 10.1111/echo.14197 [5] Song S, Heo R, Lee SE, et al. Comparing the feasibility and accuracy of three-dimensional ultrasound to two-dimensional ultrasound and computed tomography angiography in the assessment of carotid atherosclerosis[J]. Echocardiography, 2019, 36(12): 2241-50. doi: 10.1111/echo.14543 [6] Liu DM, Liu Y, Hu XH, et al. Alterations of white matter integrity associated with cognitive deficits in patients with glioma[J]. Brain Behav, 2020, 10(7): e01639. [7] Hajjar I, Okafor M, McDaniel D, et al. Effects of candesartan vs lisinopril on neurocognitive function in older adults with executive mild cognitive impairment: a randomized clinical trial[J]. JAMA Netw Open, 2020, 3(8): e2012252. doi: 10.1001/jamanetworkopen.2020.12252 [8] Wardlaw JM, Smith C, Dichgans M. Small vessel disease: mechanisms and clinical implications[J]. Lancet Neurol, 2019, 18 (7): 684-96. doi: 10.1016/S1474-4422(19)30079-1 [9] 刘晓丽, 符大勇, 周建国. 脑白质疏松患者微出血与认知功能障碍的相关性研究[J]. 中国实用神经疾病杂志, 2019, 22(15): 1637-42. https://www.cnki.com.cn/Article/CJFDTOTAL-HNSJ201915003.htm [10] Iordanishvili E, Schall M, Loução R, et al. Quantitative MRI of cerebral white matter hyperintensities: a new approach towards understanding the underlying pathology[J]. NeuroImage, 2019, 202: 116077. doi: 10.1016/j.neuroimage.2019.116077 [11] Nicoletti A, Luca A, Baschi R, et al. Vascular risk factors, white matter lesions and cognitive impairment in Parkinson's disease: the PACOS longitudinal study[J]. J Neurol, 2021, 268(2): 549-58. doi: 10.1007/s00415-020-10189-8 [12] Yuan YJ, Li NF, Liu Y, et al. Positive association between plasma aldosterone concentration and white matter lesions in patients with hypertension[J]. Front Endocrinol (Lausanne), 2021, 12: 753074. doi: 10.3389/fendo.2021.753074 [13] 沈友进, 王丹, 万婷玉, 等. 脑白质病变、颈动脉狭窄与非痴呆型血管性认知功能障碍患者预后的关系[J]. 中国现代医学杂志, 2020, 30 (7): 117-20. doi: 10.3969/j.issn.1005-8982.2020.07.024 [14] 邬午龙, 宋则周, 张艳明, 等. Logistic回归模型评估颈动脉斑块新生血管的超声造影分级预测重度脑白质病变的价值[J]. 中国超声医学杂志, 2018, 34(1): 1-5. doi: 10.3969/j.issn.1002-0101.2018.01.001 [15] 周芬莉, 吴军, 江锦赵, 等. 脑白质病变与颅内动脉硬化的相关性研究[J]. 罕少疾病杂志, 2009, 16(3): 1-3, 6. doi: 10.3969/j.issn.1009-3257.2009.03.001 [16] Porcu M, Sanfilippo R, Montisci R, et al. White- matter hyperintensities in patients with carotid artery Stenosis: an exploratory connectometry study[J]. Neuroradiol J, 2020, 33(6): 486-93. doi: 10.1177/1971400920959323 [17] Liu ZD, Zhao YX, Wang XD, et al. Low carotid artery wall shear stress is independently associated with brain white-matter hyperintensities and cognitive impairment in older patients[J]. Atherosclerosis, 2016, 247: 78-86. doi: 10.1016/j.atherosclerosis.2016.02.003 [18] Wang YX, Jiang C, Huang H, et al. Correlation of cerebral white matter lesions with carotid intraplaque neovascularization assessed by contrast- enhanced ultrasound[J]. J Stroke Cerebrovasc Dis, 2020, 29(8): 104928. doi: 10.1016/j.jstrokecerebrovasdis.2020.104928 [19] Berman SE, Wang X, Mitchell CC, et al. The relationship between carotid artery plaque stability and white matter ischemic injury[J]. Neuroimage Clin, 2015, 9: 216-22. doi: 10.1016/j.nicl.2015.08.011 [20] Guliaev SM, Urbanova EZ. Cognitive impairments and microvascular endothelial dysfunction in unilateral occlusion of the carotid artery[J]. Angiol Sosud Khir, 2019, 25(3): 17. doi: 10.33529/ANGI02019313 [21] Gaudet JG, Meyers PM, McKinsey JF, et al. Incidence of moderate to severe cognitive dysfunction in patients treated with carotid artery stenting[J]. Neurosurgery, 2009, 65(2): 325-30. doi: 10.1227/01.NEU.0000349920.69637.78 [22] Huang P, He XY, Xu M. Effects of carotid artery stent and carotid endarterectomy on cognitive function in patients with carotid Stenosis[J]. Biomed Res Int, 2020, 2020: 6634537. https://www.ncbi.nlm.nih.gov/pubmed/24550944 [23] 冯丽, 叶娜, 贾伟丽, 等. 脑白质病变评价量表在认知功能障碍中的作用[J]. 中国医刊, 2018, 53(7): 730-4. doi: 10.3969/j.issn.1008-1070.2018.07.009 [24] 司丽丽, 赵德涛, 相波, 等. 脑白质病变伴颈动脉狭窄患者认知功能障碍的相关危险因素分析[J]. 科学技术创新, 2018(13): 1-5. doi: 10.3969/j.issn.1673-1328.2018.13.002 [25] Xiang Y, Chen SG, Lin HB, et al. Cognitive function and white matter lesions in medication-overuse headache[J]. J Pain Res, 2021, 14: 1845-53. doi: 10.2147/JPR.S310064 -







 下载:
下载: