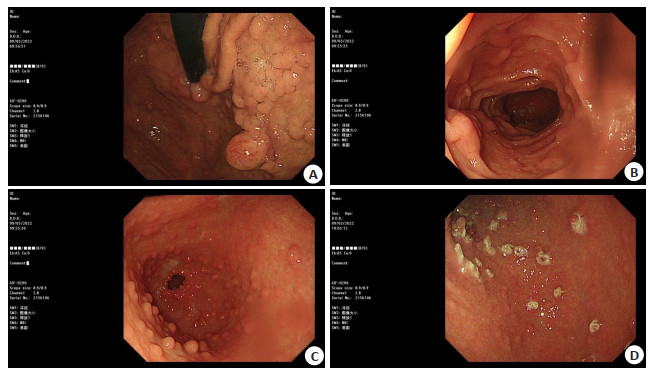
Difference between endoscopic clamp biopsy and pathological diagnosis of gastric polyp
-
摘要:
目的 分析内镜下钳夹活检诊断胃息肉的病变性质,探究其与内镜下胃息肉切除术后标本的病理诊断结果的差异。 方法 回顾性选取2021年2月~2022年2月于本院消化内科行内镜下钳夹活检诊断及内镜下胃息肉切除术的145例患者的临床资料,分析内镜下钳夹活检诊断胃息肉的病变性质,并对比其与内镜下胃息肉切除术病理检查结果的一致性,评价影响内镜下钳夹活检诊断与病理诊断胃息肉差异的影响因素。 结果 145例患者中单发息肉124例(85.52%),多发息肉21例(14.48%)。共检出171枚息肉,内镜下钳夹活检诊断与电切术后病理学诊断结果一致的共119枚(69.59%),不一致的共52枚(30.41%)。两种诊断的病理学诊断结果的Kappa值为0.182,差异有统计学意义(P < 0.05)。Logistic多因素分析结果显示,患者年龄≥60岁、息肉大小≥2.0 cm是影响内镜下钳夹活检与电切术后病理学诊断间组织学差异的独立影响因素。 结论 内镜下钳夹活检诊断胃息肉病变性质及与病理诊断胃息肉结果存在不一致性,尤其对于年龄≥60岁、息肉大小≥2.0 cm的患者的差异更大,在临床诊断中应格外注意此类患者的胃息肉与癌变病灶并存现象。 Abstract:Objective To analyze the pathological characteristics of gastric polyps diagnosed by endoscopic forceps biopsy, and explore the difference between the pathological diagnosis of gastric polyp specimens diagnosed by endoscopic forceps biopsy and the pathological diagnosis of gastric polyp specimens. Methods Clinical data of 145 patients who underwent endoscopic forceps biopsy diagnosis and endoscopic gastric polypectomy in the department of Gastroenterology of our hospital from February 2021 to February 2022 were retrospectively selected. We analyzed the pathological characteristics of gastric polyps diagnosed by endoscopic forceps biopsy, and compared the consistency with the pathological results of endoscopic gastric polypectomy. The influencing factors affecting the difference between endoscopic clamp biopsy and pathological diagnosis of gastric polyp were evaluated. Results A total of 124 cases (85.52%) had single polyp and 21 cases (14.48%) had multiple polyp in 145 patients. A total of 171 polyps were detected, 119 polyps were consistent with the pathological diagnosis after endoscopic clamp biopsy, accounting for 69.59%, and 52 polyps were inconsistent, accounting for 30.41%. The pathological diagnosis result Kappa value of the two diagnoses was 0.182, the difference was statistically significant (P < 0.05). Logistic multivariate analysis showed that age≥60 years and polyp size≥2.0 cm were independent influencing factors influencing the histological difference between endoscopic clamp biopsy and electrosurgical diagnosis. Conclusion There is inconsistency between the nature of gastric polyp diagnosed by endoscopic clamp biopsy and the results of pathological diagnosis, especially for patients with age≥60 years and polyp size≥2.0 cm. Special attention should be paid to the coexistence of gastric polyps and cancerous lesions in such patients in clinical diagnosis. -
表 1 胃息肉内镜下特征
Table 1. Endoscopic features of gastric polyps
特征 数量(n) 占比(%) 单发息肉 124 85.52 多发息肉 21 14.48 息肉部位 胃体 61 35.67 胃窦 68 39.77 胃底 32 18.71 贲门 10 5.85 息肉大小(cm) 0.5~0.9 106 61.99 1.0~1.9 51 29.82 ≥2.0 14 8.19 山田分型 Ⅰ型 21 12.28 Ⅱ型 77 45.03 Ⅲ型 58 33.92 Ⅳ型 15 8.77 表 2 内镜下钳夹活检诊断与病理学诊断结果的一致性检验
Table 2. Consistency test of endoscopic clamp biopsy diagnosis and pathological diagnosis (n)
内镜下钳夹活检诊断 电切术后病理学诊断 炎性息肉 增生性息肉 腺瘤性息肉 胃底腺息肉 非典型增生 息肉癌变 总计[n(%)] 炎性息肉 8 15 3 2 3 0 31(18.13) 增生性息肉 4 83 10 3 5 2 107(62.57) 腺瘤性息肉 0 0 12 1 1 0 14(8.19) 胃底腺息肉 0 0 1 3 0 0 4(2.34) 非典型增生 0 2 0 0 13 0 15(8.77) 总计[n(%)] 12(7.02) 100(58.48) 26(15.20) 9(5.26) 22(12.86) 2(1.17) 171(100.00) 表 3 内镜下钳夹活检与电切术后病理学诊断间组织学差异的单因素分析
Table 3. Univariate analysis of histological differences between endoscopic clamp biopsy and postoperative pathological diagnosis
项目 一致(n) 不一致(n) 差异率(%) χ2 P 性别 0.518 0.472 男 39 20 33.90 女 80 32 28.57 年龄(岁) 10.332 0.001 < 60 93 28 23.14 ≥60 26 24 48.00 息肉部位 2.739 0.434 胃体 47 14 24.14 胃窦 45 23 33.82 胃底 20 12 37.50 贲门 7 3 30.00 息肉大小(cm) 8.145 0.015 0.5~0.9 78 28 26.42 1.0~1.9 36 15 29.41 ≥2.0 5 9 64.28 山田分型 0.133 0.104 Ⅰ型 14 7 33.33 Ⅱ型 49 28 36.36 Ⅲ型 42 16 27.59 Ⅳ型 14 1 6.67 表 4 内镜下钳夹活检与电切术后病理学诊断间组织学差异的多因素分析
Table 4. Multi-factor analysis of histological differences between endoscopic clamp biopsy and postoperative pathological diagnosis
相关因素 β SE P OR 95% CI 年龄≥60岁 1.344 0.668 0.021 7.255 4.711~14.321 息肉大小≥2.0 cm 1.643 0.752 0.003 9.526 5.390~22.709 -
[1] Goddard AF, Badreldin R, Pritchard DM, et al. The management of gastric polyps[J]. Gut, 2010, 59(9): 1270-6. doi: 10.1136/gut.2009.182089 [2] Cao HL, Wang BM, Zhang ZH, et al. Distribution trends of gastric polyps: an endoscopy database analysis of 24 121 northern Chinese patients[J]. J Gastroenterol Hepatol, 2012, 27(7): 1175-80. doi: 10.1111/j.1440-1746.2012.07116.x [3] 杨振, 吴战军. 不同病理类型胃息肉患者Hp感染情况及胃、结直肠息肉之间的相关性[J]. 山东医药, 2015, 55(37): 55-7. doi: 10.3969/j.issn.1002-266X.2015.37.021 [4] 贾剑南, 唐艳萍, 康丽丽, 等. 胃息肉的特点及其与Hp感染的相关性研究[J]. 中国中西医结合消化杂志, 2020, 28(9): 651-5, 667. doi: 10.3969/j.issn.1671-038X.2020.09.02 [5] Yoon WJ, Lee DH, Jung YJ, et al. Histologic characteristics of gastric polyps in Korea: emphasis on discrepancy between endoscopic forceps biopsy and endoscopic mucosal resection specimen[J]. World J Gastroenterol, 2006, 12(25): 4029-32. doi: 10.3748/wjg.v12.i25.4029 [6] Draganov PV, Chang MN, Alkhasawneh A, et al. Randomized, controlled trial of standard, large-capacity versus jumbo biopsy forceps for polypectomy of small, sessile, colorectal polyps[J]. Gastrointest Endosc, 2012, 75(1): 118-26. doi: 10.1016/j.gie.2011.08.019 [7] Isomoto H, Nakao K. Endoscopic procedures developed in Japan[J]. Ann Transl Med, 2014, 2(3): 11. [8] Song JY, Kim HH, Lee HW, et al. Four endoscopic predictors of carcinoma as a final diagnosis after endoscopic resection of forceps biopsy-proven gastric adenomas[J]. Korean J Helicobacter Up Gastrointest Res, 2013, 13(1): 36. doi: 10.7704/kjhugr.2013.13.1.36 [9] 洪捷敏, 林琪, 李昌水, 等. 胃无蒂息肉内镜活检与黏膜切除标本病理差异的研究[J]. 现代实用医学, 2012, 24(5): 572-4. doi: 10.3969/j.issn.1671-0800.2012.05.051 [10] 刘彤华. 诊断病理学[M]. 2版. 北京: 人民卫生出版社, 2006: 52-53. [11] Gerada J, Fenech V, Attard J, et al. Endoscopic mucosal resection for early gastric cancer arising in a small adenomatous polyp[J]. Austin J Gastroenterol, 2015, 2(3): 1042. [12] Jung JT. Gastric polyps and protruding type gastric cancer[J]. Clin Endosc, 2013, 46(3): 243-7. doi: 10.5946/ce.2013.46.3.243 [13] Kim JH, Kim YJ, An J, et al. Endoscopic features suggesting gastric cancer in biopsy-proven gastric adenoma with high-grade neoplasia [J]. World J Gastroenterol, 2014, 20(34): 12233-40. doi: 10.3748/wjg.v20.i34.12233 [14] Mori H, Nishiyama N, Kobara H, et al. The use of a detachable multiple polyp catcher to facilitate accurate location and pathological diagnosis of resected polyps in the proximal colon[J]. Gastrointest Endosc, 2016, 83(1): 262-3. doi: 10.1016/j.gie.2015.08.008 [15] 贺利影, 吴学勇, 吴伟. 胃息肉内镜下钳夹活检与电切术后组织病理诊断结果的差异[J]. 解放军预防医学杂志, 2019, 37(9): 188-9, 195 https://www.cnki.com.cn/Article/CJFDTOTAL-JYYX201909075.htm [16] 陈珊杰, 陈云云. 胃息肉内镜下钳夹活检术与内镜切除术后病理诊断的比较[J]. 中国临床研究, 2015, 28(5): 613-5. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGCK201505023.htm [17] Markowski AR, Guzinska-Ustymowicz K. Gastric hyperplastic polyp with focal cancer[J]. Gastroenterol Rep: Oxf, 2014, 4(2): 158-61. [18] 张晓艳, 吴学勇, 吴伟. 胃息肉193例临床病理及内镜治疗分析[J]. 陕西医学杂志, 2016, 45(9): 1264-5. doi: 10.3969/j.issn.1000-7377.2016.09.079 [19] 叶玲, 张桂英. 胃息肉钳夹活检术与切除术后的病理诊断比较[J]. 实用医学杂志, 2009, 25(19): 3276-8. doi: 10.3969/j.issn.1006-5725.2009.19.040 [20] 余艳秋, 王建宁, 彭春艳, 等. 胃黏膜上皮内瘤变内镜切除术后病理与术前活检病理的差异比较及原因分析[J]. 中华消化内镜杂志, 2018, 35(12): 880-4. doi: 10.3760/cma.j.issn.1007-5232.2018.12.004 -







 下载:
下载: