Prediction value of CT-based radiomics in lymph node metastasis of T1 lung adenocarcinoma
-
摘要:
目的 分析CT影像组学对T1期肺腺癌淋巴结转移状态的预测价值。 方法 回顾性选择2016年6月~2019年5月我院收治的肺腺癌患者140例,以术中送检的病理组织标本检查结果为金标准,分为金标准阳性组67例与金标准阴性组73例。分别采用术前增强CT、术前CT影像组学评估两组淋巴结转移发生情况。利用Delong检验评估CT影像组学与增强CT在两组中预测对淋巴结转移的价值。 结果 CT影像组学法对阳性淋巴结转移的预测比率为86.57%(58/67),高于增强CT法的64.18%(43/67)(P < 0.05);CT影像组学法对阴性淋巴结转移的预测比率为100.00%(73/73),高于增强CT法的93.15%(68/73)(P < 0.05);CT影像组学法预测到的金标准阳性组中发生淋巴结转移患者的风险评分值明显高于未发生淋巴结转移患者(P < 0.05);金标准阳性组中CT影像组学对患者淋巴结转移预测的曲线下面积高于增强CT(P < 0.05),金标准阴性组中CT影像组学对患者淋巴结转移预测的曲线下面积高于增强CT(P < 0.05)。 结论 与增强CT相比,CT影像组学在术前预测肺腺癌淋巴结转移阳性预测值和阴性预测值更高,具有更高的诊断价值。 Abstract:Objective To investigate the predictive value of CT-based radiomics in lymph node metastasis in stage T1 lung adenocarcinoma. Methods A total of 140 patients with lung adenocarcinoma admitted to our hospital from June 2016 to May 2019 were retrospectively selected. With the results of pathological tissue samples in intraoperative examination as the gold standard, they were divided into the gold standard positive group (n=67) and the gold standard negative group (n=73). Preoperative enhanced CT and preoperative CT imaging were used to evaluate lymph node metastasis in the two groups. Delong test was used to evaluate the value of CT imaging and enhanced CT in predicting lymph node metastasis in both groups. Results In the two groups, the prediction ratioof positive lymph node metastasis by CT radiomics was 86.57% (58/67), which was higher than that by enhanced CT method [64.18% (43/67)] (P < 0.05). The prediction ratioof negative lymph node metastasis by CT radiomics was 100.00% (73/73), which was higher than that by enhanced CT [93.15% (68/73)] (P < 0.05). In the gold standard positive group, the risk score of patients with lymph node metastasis was significantly higher than that of patients without lymph node metastasisvia CT radiomics (P < 0.05). In the gold standard positive group, the AUC area of CTradiomics in prediction of lymph node metastasiswas significantly higher than that of enhanced CT (P < 0.05), and so was in the gold standard negative group (P < 0.05). Conclusions Compared with enhanced CT, CT radiomics has a higher positive predictive value and negative predictive value for predicting lymph node metastasis of lung adenocarcinoma before surgery with high diagnostic value. -
Key words:
- CT radiomics /
- lung adenocarcinoma /
- lymph node metastasis /
- predictive value
-
表 1 两组临床资料比较
Table 1. Comparison of clinical data of two groups (n)
组别 有吸烟史 CEA水平(阴性/阳性) 术后肿瘤病理类型 肿瘤直径(cm, Mean±SD) 原位腺癌 黏液腺癌 腺泡型癌 浸润型癌 金标准阳性组(n=67) 53 6/61 34 27 3 3 3.35±0.82 金标准阴性组(n=73) 25 71/2 46 24 2 1 2.13±0.31 t/χ2 8.792 9.254 4.659 11.450 P 0.048 < 0.001 0.601 < 0.001 表 2 不同方法两组预测术前淋巴结转移结果比较
Table 2. Comparison of different methods in predicting preoperative lymph node metastasis between the two groups [n(%)]
组别及预测方法 发生淋巴结转移 未发生淋巴结转移 金标准阳性组(n=67) 增强CT 43(64.18) 24(35.82) CT影像组学 58(86.57) 9(13.43) χ2 3.814 P 0.026 金标准阴性组(n=73) 增强CT 5(6.85) 68(93.15) CT影像组学 0(0) 73(100.00) χ2 23.176 P < 0.001 表 3 增强CT与CT影像组学在两组患者术前淋巴结转移中的预测价值
Table 3. Predictive value of enhanced CT and CT radiomics in preoperative lymph node metastasis in two groups of patients
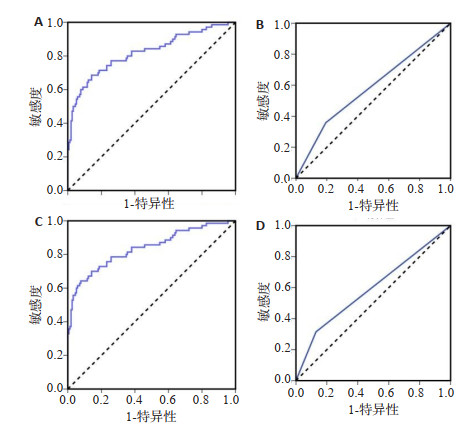
组别 曲线下面积 Youden P 敏感度(%) 特异性(%) 阴性预测值(%) 阳性预测值(%) 金标准阳性组 CT影像组学 0.820 0.544 < 0.001 68.6 85.8 73.2 82.9 增强CT 0.583 0.165 0.035 35.8 80.7 55.7 65.0 金标准阴性组 CT影像组学 0.837 0.565 < 0.001 64.3 92.3 72.1 89.3 增强CT 0.593 0.175 0.097 31.5 87.0 55.9 70.8 -
[1] 刘洋, 寻航, 李修奎, 等. 不同病理类型肺癌的双源CT参数特征及诊断鉴别价值[J]. 中国CT和MRI杂志, 2018, 16(2): 77-80. doi: 10.3969/j.issn.1672-5131.2018.02.023 [2] Kim CR, Kim B, Ning MS, et al. Cost analysis of PET/CT versus CT as surveillance for stage Ⅲ non-small-cell lung cancer after definitive radiation therapy[J]. Clin Lung Cancer, 2018, 19(4): e517- 28. doi: 10.1016/j.cllc.2018.03.012 [3] 史张, 李晶, 边云, 等. 影像组学在临床精确诊疗中的研究进展[J]. 中华放射学杂志, 2018, 52(10): 801-4. doi: 10.3760/cma.j.issn.1005-1201.2018.10.019 [4] 杨志炜, 郭天, 谢海滨, 等. 影像组学在脑胶质瘤分级中的应用研究[J]. 磁共振成像, 2018, 9(6): 439-45. https://www.cnki.com.cn/Article/CJFDTOTAL-CGZC201806010.htm [5] Lambin P, Rios-Velazquez E, Leijenaar R, et al. Radiomics: Extracting more information from medical images using advanced feature analysis[J]. Eur J Cancer, 2012, 48(4): 441-6. doi: 10.1016/j.ejca.2011.11.036 [6] Gillies RJ, Kinahan PE, Hricak H. Radiomics: images are more than pictures, they are data[J]. Radiology, 2016, 278(2): 563-77. doi: 10.1148/radiol.2015151169 [7] Avanzo M, Wei LS, Stancanello J, et al. Machine and deep learning methods for radiomics[J]. Med Phys, 2020, 47(5): e185-202. [8] Yang F, Ford JC, Dogan N, et al. Magnetic resonance imaging (MRI)- based radiomics for prostate cancer radiotherapy[J]. Transl Androl Urol, 2018, 7(3): 445-58. doi: 10.21037/tau.2018.06.05 [9] 李武超, 陈琦, 蒋仪, 等. 基于CT影像组学术前预测胃癌淋巴血管侵犯[J]. 中国医学影像技术, 2019, 35(7): 1057-60. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYXX201907031.htm [10] Li XM, Dong XP, Lian J, et al. Knockoff filter-based feature selection for discrimination of non-small cell lung cancer in CT image[J]. IET Image Process, 2019, 13(3): 543-8. doi: 10.1049/iet-ipr.2018.6053 [11] 徐茂林, 李芳, 刘玉林, 等. 肺腺癌乳腺转移超声及MRI表现1例[J]. 中国临床医学影像杂志, 2019, 30(3): 227-8. https://www.cnki.com.cn/Article/CJFDTOTAL-LYYX201903028.htm [12] 吉蘅山, 张龙江, 朱虹. 肺癌PET-CT影像组学研究进展[J]. 中华放射学杂志, 2019, 53(2): 154-7. doi: 10.3760/cma.j.issn.1005-1201.2019.02.017 [13] 洪敏萍, 王云华, 顾吾立, 等. 肺内淋巴结伴周围炎症与胸膜下微浸润性肺腺癌的CT鉴别分析[J]. 中国临床医学影像杂志, 2020, 31(9): 637-40. https://www.cnki.com.cn/Article/CJFDTOTAL-LYYX202009010.htm [14] 肖磊, 顾潜彪, 张堃, 等. CT影像组学标签预测肺腺癌表皮生长因子受体基因敏感突变[J]. 中国介入影像与治疗学, 2019, 16(4): 220-4. https://www.cnki.com.cn/Article/CJFDTOTAL-JRYX201904011.htm [15] Sotoudeh H, Sadaatpour Z, Rezaei A, et al. The role of machine learning and radiomics for treatment response prediction in idiopathic normal pressure hydrocephalus[J]. Cureus, 2021, 13(10): e18497 [16] Forghani R. Precision digital oncology: emerging role of radiomicsbased biomarkers and artificial intelligence for advanced imaging and characterization of brain tumors[J]. Radiol Imaging Cancer, 2020, 2(4): e190047. doi: 10.1148/rycan.2020190047 [17] Ou J, Wu L, Li R, et al. CT radiomics features to predict lymph node metastasis in advanced esophageal squamous cell carcinoma and to discriminate between regional and non-regional lymph node metastasis: a case control study[J]. Quant Imaging Med Surg, 2021, 11(2): 628-40. doi: 10.21037/qims-20-241 [18] Wu QX, Wang S, Li L, et al. Radiomics Analysis of Computed Tomography helps predict poor prognostic outcome in COVID-19 [J]. Theranostics, 2020, 10(16): 7231-44. doi: 10.7150/thno.46428 [19] 岳军艳, 窦文广, 梁长华, 等. 实性肺腺癌和鳞癌的性别、年龄及CT征象分析[J]. 实用放射学杂志, 2019, 35(2): 208-11. doi: 10.3969/j.issn.1002-1671.2019.02.009 [20] 宋文娟, 平学军, 石惠, 等. 周围型肺癌能谱CT定量分析与免疫组化指标的相关性分析[J]. 实用放射学杂志, 2018, 34(10): 1517-20, 1525. doi: 10.3969/j.issn.1002-1671.2018.10.009 [21] 谭剑, 杨星萍, 田仁江, 等. 肺腺癌中T细胞免疫球蛋白黏蛋白分子3与干扰素γ表达及其临床意义[J]. 中华生物医学工程杂志, 2020, 26 (3): 231-6. doi: 10.3760/cma.j.cn115668-20200126-00009 [22] 史张, 刘崎. 影像组学技术方法的研究及挑战[J]. 放射学实践, 2018, 33(6): 633-6. https://www.cnki.com.cn/Article/CJFDTOTAL-FSXS201806028.htm [23] 林斌, 王韬, 沈可人, 等. 肺黏膜相关淋巴组织淋巴瘤与肺腺癌鉴别的影像组学研究[J]. 中华放射学杂志, 2018, 52(10): 766-9. doi: 10.3760/cma.j.issn.1005-1201.2018.10.009 [24] 吴光耀. 影像组学在肺癌的应用及研究进展[J]. 实用放射学杂志, 2018, 34(10): 1635-7, 1642. doi: 10.3969/j.issn.1002-1671.2018.10.039 -







 下载:
下载: