Clinical value of progesterone and β-HCG levels combined with subchorionic hemorrhage predicting early pregnancy outcome in threatened abortion patients
-
摘要:
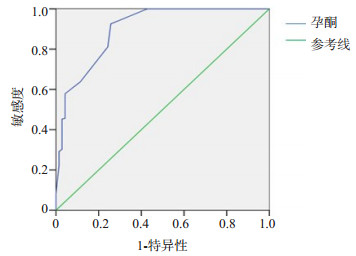
目的探讨超声绒毛膜下血肿(SCH)联合血清孕酮、β-绒毛膜促性腺激素(β-HCG)预测早孕期结局的临床价值。 方法选取2020年6~12月因先兆流产来我院检查的324例患者,行超声检查及血清孕酮、β-HCG检测,随访至孕14周,观察其妊娠结局,其中治疗后继续妊娠者为先兆流产组(n=254),发展为难免流产者为流产组(P < 070)。比较组间的孕酮、β-HCG水平以及SCH阳性率差异性,采用受试者工作特征(ROC)曲线分析孕酮与β-绒毛膜促性腺激素对流产的预测价值。 结果流产组血清孕酮、β-HCG水平明显低于先兆流产组,流产组患者SCH阳性率明显高于先兆流产组,差异均具有统计学意义(P < 0.05)。血清孕酮的ROC曲线下面积为0.90(95%CI:0.85~0.94),当cut-off值为18.5时,其预测流产的敏感度和特异性分别为92.5%和74.3%。血清β-HCG的ROC曲线下面积为0.89(95%CI:0.84~0.94),当cut-off值为6926时,其预测流产的敏感度和特异性分别为78.6%和92.9%。血清孕酮、β-HCG及SCH阳性联合检测预测先兆流产结局的敏感度、特异性、阳性预测值和阴性预测值分别为70.8%、98.3%、97.1%和80.8%。 结论超声SCH和血清孕酮、β-HCG水平对预测先兆流产患者早期妊娠结局具有一定的价值,三者联合检测可提高预测的特异性和阳性预测值。 -
关键词:
- 超声 /
- 绒毛膜下血肿 /
- 血清孕酮 /
- β-人绒毛膜促性腺激素 /
- 先兆流产
Abstract:ObjectiveTo explore the clinical value of subchorionic hemorrhage(SCH)combined with progesterone and β-HCG for predicting early pregnancy outcome in threatened abortion patients. MethodsA total of 324 patients who came to our hospital due to threatened abortion from June 2020 to December 2020 were selected for serum progesterone, β-HCG and ultrasound examination. They were followed up for 14 weeks of gestation to observe the pregnancy outcome. The patients who continued pregnancy after treatment were defined threatened abortion group, and those who developed inevitable abortion were defined abortion group. The differences of progesterone, β-hCG and the positive rate of SCH between two groups were compared. The prediction value of progesterone and β-hCG for abortion were analyzed by receiver operating characteristic (ROC) curve. ResultsThe 254 cases were in threatened abortion group and 70 cases were in abortion group. The levels of serum progesterone and β-hCG in abortion group were significantly lower than those in threatened abortion group, and the positive rate of SCH in abortion group was significantly higher than those in threatened abortion group (P < 0.05). The area under ROC curve of serum progesterone was 0.90 (95% CI: 0.85-0.94). When cut off value was 18.5, the sensitivity and specificity of predicting abortion were 92.5% and 74.3%, respectively. The area under ROC curve of serum β-hCG was 0.89 (95% CI: 0.84-0.94). When cut off value was 6926, the sensitivity and specificity of predicting abortion were 78.6% and 92.9%, respectively. The sensitivity, specificity, positive predictive value and negative predictive value of serum progesterone, β-hCG and SCH were 70.8%, 98.3%, 97.1% and 80.8% respectively. ConclusionsThe SCH, Serum progesterone and β-HCG level have certain value for predicting the early pregnancy outcome in threatened abortion patients. The combined detection of the three indicators can improve the specificity and positive predictive value. -
Key words:
- ultrasound /
- subchorionic hemorrhage /
- serum progesterone /
- β-HCG /
- threatened abortion
-
表 1 组之间孕酮、β-HCG及SCH结果的比较
Table 1. Comparison of the results of progesterone, β-HCG and SCH among the three groups
组别 孕酮(ng/mL, Mean±SD) β-HCG(U/L, Mean±SD) SCH阳性[n(%)] 先兆流产组(n=254) 23. 99±3. 15 8606.00±1864.00 103(40.6) 流产组(n=70) 17. 21±3. 29 6031.64±1028.00 59(84.3) P < 0.05 < 0.05 < 0.05 β-HCG:β-人绒毛膜促性腺激素,SCH:绒毛膜下血肿. 表 2 各指标对难免流产预测价值的比较
Table 2. Comparison of the predictive value of each index for inevitable abortion(%)
检测指标 敏感度 特异性 阳性预测值 阴性预测值 孕酮 92.5 74.3 76.1 79.0 β-HCG 78.6 90.9 76.9 85.7 SCH 88.3 61.7 65.2 88.1 联合检测 80.8 98.3*#△ 97.1*#△ 85.8 *P < 0.05 vs孕酮;#P < 0.05 vs β-HCG;△P < 0.05 vs SCH. -
[1] 华克勤, 丰有吉. 实用妇产科学[M]. 3版. 北京: 人民卫生出版社, 2013: 96. [2] 刘德广, 马红丽, 王宇, 等. 先兆流产治疗的研究进展[J]. 中国医药导报, 2019, 16(5): 30-3. https://www.cnki.com.cn/Article/CJFDTOTAL-YYCY201905008.htm [3] Carp H. A systematic review of dydrogesterone for the treatment of threatened miscarriage[J]. Gynecol Endocrinol, 2012, 28(12): 983-90. doi: 10.3109/09513590.2012.702875 [4] Johns J, Muttukrishna S, Lygnos M, et al. Maternal serum hormone concentrations for prediction of adverse outcome in threatened miscarriage[J]. Reprod Biomed Online, 2007, 15(4): 413-21. doi: 10.1016/S1472-6483(10)60367-7 [5] Kasap B, Özel Türkçü Ü, Akbaba E, et al. The predictive role of sTWEAK levels in pregnant women with first-trimester vaginal bleeding[J]. J Matern Fetal Neonatal Med, 2018, 31(13): 1715-9. doi: 10.1080/14767058.2017.1326097 [6] Kim YJ, Shin JH, Hur JY, et al. Predictive value of serum progesterone level on β-hCG check day in women with previous repeated miscarriages after in vitro fertilization[J]. PLoS One, 2017, 12(7): e0181229. doi: 10.1371/journal.pone.0181229 [7] 王玮, 谢一红, 杨石慧, 等. 血清CA125水平对妊娠早期自然流产的预测价值[J]. 中华生殖与避孕杂志, 2019, 39(4): 286-91. [8] 白璐, 吴利英, 杨红, 等. 早期先兆流产患者不同孕龄血清雌二醇水平波动对妊娠结局的影响[J]. 临床和实验医学杂志, 2021, 20(2): 194-6. doi: 10.3969/j.issn.1671-4695.2021.02.023 [9] Yalçin İ, Taşkin S, Pabuçcu EG, et al. The value of placental protein 13, β-human chorionic gonadotropin and progesterone in the prediction of miscarriages in threatened miscarriage patients[J]. J Obstet Gynaecol, 2015, 35(3): 283-6. doi: 10.3109/01443615.2014.948822 [10] 周荣向, 杨军, 林春扬, 等. 血清孕酮联合甲胎蛋白检测诊断早期先兆流产的价值[J]. 中国妇幼保健, 2017, 32(19): 4772-4. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFYB201719061.htm [11] 吴碧云, 毛文礼, 张美婵, 等. 血清雌二醇、β-绒毛膜促性腺激素及孕酮水平检测在早期先兆流产结局预测中的应用价值[J]. 中国当代医药, 2021, 28(6): 149-52. doi: 10.3969/j.issn.1674-4721.2021.06.044 [12] 严东琴, 谭琴, 林晓岚. PAPP-A联合HCG在先兆流产患者中的检测水平及与妊娠不良结局的相关性[J]. 中国临床研究, 2020, 33(2): 186-8, 193. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGCK202002012.htm [13] 温明晓. 血清P、PRL联合β-HCG对孕6周~12周先兆流产保胎结局预测价值分析[J]. 中国性科学, 2020, 29(4): 52-7. https://www.cnki.com.cn/Article/CJFDTOTAL-XKXZ202004018.htm [14] Pillai RN, Konje JC, Tincello DG, et al. Role of serum biomarkers in the prediction of outcome in women with threatened miscarriage: a systematic review and diagnostic accuracy meta-analysis[J]. Hum Reprod Update, 2016, 22(2): 228-39. http://humupd.oxfordjournals.org/cgi/content/abstract/dmv054v1 [15] Pedersen JF, Mantoni M. Prevalence and significance of subchorionic hemorrhage in threatened abortion: a sonographic study[J]. AJR Am J Roentgenol, 1990, 154(3): 535-7. doi: 10.2214/ajr.154.3.2106217 [16] 岳洁, 刘晓华, 卢钺, 等. 早孕期绒毛膜下血肿的位置与大小对妊娠结局的影响[J]. 中国妇幼保健, 2015, 30(34): 5983-4. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFYB201534018.htm [17] Zhou J, Wu M, Wang B, et al. The effect of first trimester subchorionic hematoma on pregnancy outcomes in patients underwent IVF/ICSI treatment[J]. J Matern Fetal Neonatal Med, 2017, 30(4): 406-10. doi: 10.1080/14767058.2016.1174682 [18] 李清, 朱瑾, 华克勤. 绒毛膜下血肿孕妇妊娠结局的荟萃分析[J]. 中华医学杂志, 2016, 3(17): 1383-5. doi: 10.3760/cma.j.issn.0376-2491.2016.17.017 [19] 张宇迪, 于松, 卢丹, 等. 妊娠早期绒毛膜下血肿对妊娠结局的影响[J]. 临床与病理杂志, 2016, 36(5): 601-5. https://www.cnki.com.cn/Article/CJFDTOTAL-WYSB201605014.htm [20] 陈秀娟, 曾学燚, 梁小勤, 等. 早孕期绒毛膜隆起的超声表现及临床意义[J]. 临床超声医学杂志, 2019, 21(8): 623-5. doi: 10.3969/j.issn.1008-6978.2019.08.022 [21] 王晓莉, 常小霞, 蔡雯, 等. 早期妊娠合并子宫内血肿的临床意义[J]. 中国妇幼健康研究, 2019, 30(7): 859-62. doi: 10.3969/j.issn.1673-5293.2019.07.020 [22] 丁艳婷. 绒毛膜下血肿的研究进展[J]. 现代妇产科进展, 2019, 28 (10): 791-3. https://www.cnki.com.cn/Article/CJFDTOTAL-XDFC201910016.htm [23] 张静. 妊娠早期合并绒毛膜隆起的超声特点及妊娠结局分析[J]. 中国妇幼保健, 2021, 36(2): 285-7. [24] 刘晓华, 岳洁, 卢钺, 等. 先兆流产合并绒毛膜下血肿孕妇孕早期激素水平与妊娠结局的相关性分析[J]. 海南医学院学报, 2016, 22(4): 361-3. https://www.cnki.com.cn/Article/CJFDTOTAL-HNYY201604014.htm [25] Yan Y, Chen Z, Yang Y, et al. Efficacy of progesterone on threatened miscarriage: an updated meta-analysis of randomized trials[J]. Arch Gynecol Obstet, 2021, 303(1): 27-36. doi: 10.1007/s00404-020-05808-8 [26] Li L, Zhang Y, Tan H, et al. Effect of progestogen for women with threatened miscarriage: a systematic review and meta-analysis[J]. BJOG, 2020, 127(9): 1055-63. doi: 10.1111/1471-0528.16261 -







 下载:
下载: