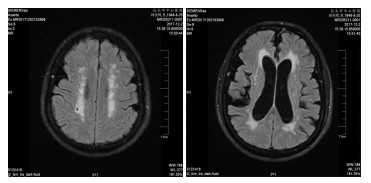
Efficacy of neuroacid combined with flunarizine hydrochloride capsules in the treatment of cognitive impairment caused by leukoaraiosis
-
摘要:
目的探讨分析神经酸联合盐酸氟桂利嗪胶囊对脑白质疏松所致认知功能障碍的疗效。 方法选取86例脑白质疏松所致认知功能障碍患者并将其按照随机数表分为常规组和联合组,43例/组。常规组采用单纯盐酸氟桂利嗪胶囊治疗,联合组给予神经酸联合盐酸氟桂利嗪胶囊治疗。对比2组基线资料,治疗前后认知功能变化,临床疗效,不良反应发生率。 结果联合组基线资料与常规组均相近,差异无统计学意义(P>0.05);治疗前联合组与常规组视空间与执行、注意、命名、语言、抽象、延迟记忆、定向维度蒙特利尔认知评估量表(MoCA)评分与总分相近(P>0.05),治疗后联合组注意、语言、抽象、延迟记忆方面的MoCA评分与总分均高于治疗前(P < 0.05);联合组在注意、抽象、以及MoCA总分方面临床疗效分布与常规组对比差异有统计学意义(86.05% vs 58.14%,P < 0.05);联合组不良反应发生率(11.63%)与常规组(6.98%)相近(P>0.05),且患者均可耐受。 结论对脑白质疏松所致认知功能障碍患者给予神经酸联合盐酸氟桂利嗪胶囊治疗可改善其认知功能,增强疗效,且安全可靠。 Abstract:ObjectiveTo explore and analyze the effect of neuroacid combined with Flunarizine Hydrochloride Capsule on cognitive impairment caused by leukoaraiosis. MethodsEighty-six patients with cognitive impairment caused by leukoaraiosis were selected and randomly divided into routine group and combined group, 43 cases in each group.The routine group was treated with flunarizine hydrochloride capsule alone.The combined group was treated with nerve acid and Flunarizine Hydrochloride capsules.The baseline data of the two groups were compared. The changes of cognitive function, clinical efficacy before and after treatment and incidence of adverse reactions were compared. ResultsThe baseline data of the combined group were similar to those of the routine group (P>0.05). Before treatment, the scores of visual space and execution, attention, naming, language, abstraction, delayed memory and orientation dimension Montreal Cognitive Assessment Scale (MoCA) were similar to those of the routine group (P>0.05), but after treatment, the scores of MoCA in the combined group were higher than those before treatment (P < 0.05), and after treatment, the above dimensions of MoCA in the combined group were higher than those before treatment (P < 0.05). The scores and total scores were higher than those of the routine group (P < 0.05). The clinical efficacy distribution of the combined group was significantly different from that of the routine group (P < 0.05). The total effective rate of the former group was 86.05%, which was significantly higher than that of the latter group (58.14%) (P < 0.05). The incidence of adverse reactions in the combined group was 11.63%, which was similar to 6.98% in the routine group (P>0.05), and the patients were tolerable. ConclusionNeuric acid combined with flunarizine hydrochloride capsules can improve the cognitive function and enhance the curative effect of patients with cognitive impairment caused by leukoaraiosis, which is safe and reliable. -
表 1 2组患者的基线资料对比
Table 1. Comparison of baseline data between the two groups [n=43, n(%)]
指标 联合组 常规组 t/Z/χ2 P 性别 0.187 0.665 男 24 (55.81) 22 (51.16) 女 19 (44.19) 21 (48.84) 年龄(岁, Mean±SD) 66.29±10.18 67.27±10.22 0.445 0.657 脑白质疏松分级 0.244 0.621 1级 9 (20.93) 9 (20.93) 2级 11 (25.58) 13 (30.23) 3级 13 (30.23) 12 (27.91) 4级 10 (23.26) 9 (20.93) 受教育年限(年) 0.205 0.651 < 12 16 (37.21) 14 (32.56) ≥12 27 (62.79) 29 (67.44) 表 2 治疗前后认知功能变化对比
Table 2. Comparison of cognitive function before and after treatment (Score, n=43, Mean±SD)
指标 联合组 t P 常规组 t P 治疗前 治疗后 治疗前 治疗后 视空间与执行 2.05±0.41 3.05±0.44 5.955 0.087 2.00±0.38 2.51±0.40 0.587 0.559 注意 1.98±0.32 3.16±0.42 6.703 0.007 2.00±0.35 2.56±0.41 0.277 0.783 命名 2.02±0.39 3.19±0.50 0.825 0.331 1.98±0.40 2.53±0.39 0.470 0.640 语言 2.00±0.35 3.00±0.46 5.171 0.000 1.95±0.36 2.47±0.49 4.653 0.016 抽象 1.98±0.37 3.07±0.52 5.950 0.040 1.95±0.35 2.44±0.46 0.386 0.700 延迟记忆 2.00±0.36 2.93±0.44 3.726 0.000 1.91±0.37 2.56±0.48 1.143 0.036 定向 1.98±0.39 2.95±0.46 3.764 0.055 2.00±0.40 2.56±0.50 0.235 0.815 总分 14.37±2.15 21.72±3.80 5.349 0.000 14.12±2.17 17.95±2.63 0.537 0.593 表 3 临床疗效对比
Table 3. Clinical efficacy comparison [n=43, n(%)]
组别 显效 有效 无效 总有效率 联合组 14(32.56) 23(53.49) 6(13.95) 37(86.05) 常规组 6(13.95) 19(44.19) 18(41.86) 25(58.14) Z/χ2 9.602 8.323 P 0.001 0.004 -
[1] 黄斌, 秦怀洲. 脑小血管病引发脑白质疏松与患者认知功能障碍的关系[J]. 河北医学, 2018, 24(1): 174-6. doi: 10.3969/j.issn.1006-6233.2018.01.046 [2] 冯丽, 叶娜, 王金芳, 等. 脑白质疏松患者病变部位与认知功能的相关性[J]. 中华行为医学与脑科学杂志, 2018, 27(1): 26-30. [3] Biyik Z, Guney I. Relationship between uric acid, proteinuria, and atherogenic index of plasma in renal transplant patients[J]. Transplant Proc, 2018, 50(10): 3376-80. doi: 10.1016/j.transproceed.2018.05.021 [4] 苏爱梅, 赵燕, 杨立, 等. 盐酸多奈哌齐片联合神经酸治疗脑白质疏松症伴认知障碍的临床疗效[J]. 实用心脑肺血管病杂志, 2017, 25 (S1): 84-5. https://www.cnki.com.cn/Article/CJFDTOTAL-SYXL2017S1033.htm [5] 冯涛, 王拥军. 脑白质疏松的影像学评测量表[J]. 中国卒中杂志, 2009, 4(3): 226-30. doi: 10.3969/j.issn.1673-5765.2009.03.010 [6] Yuan JL, Wang SK, Guo XJ, et al. Disconnections of corticosubcortical pathways related to cognitive impairment in patients with leukoaraiosis: a preliminary diffusion tensor imaging study[J]. Eur Neurol, 2017, 78(1/2): 41-7. http://europepmc.org/abstract/MED/28618415 [7] Wang S, Yuan J, Guo X, et al. Correlation between prefrontal-striatal pathway impairment and cognitive impairment in patients with leukoaraiosis[J]. Medicine (Madr), 2017, 96(17): e6703. [8] Zhang Z, Ren WW, Shao B, et al. Leukoaraiosis is associated with worse short-term functional and cognitive recovery after minor stroke[J]. Neurol Med Chir (Tokyo), 2017, 57(3): 136-43. doi: 10.2176/nmc.oa.2016-0188 [9] Feng L, Jiang H, Li YX, et al. Effects of citicoline therapy on the network connectivity of the corpus callosum in patients with leukoaraiosis[J]. Medicine (Baltimore), 2017, 96(4): e5931. doi: 10.1097/MD.0000000000005931 [10] 张强, 高政, 邢芸芸, 等. 预防性应用盐酸氟桂利嗪对高血糖SD大鼠局部脑缺血再灌注模型bcl-2表达的影响[J]. 医学与哲学: 临床决策论坛版, 2010, 31(2): 42-4. https://www.cnki.com.cn/Article/CJFDTOTAL-YXZL201002019.htm [11] Kueider AM, An Y, Tanaka T, et al. Sex-dependent associations of serum uric acid with brain function during aging[J]. J Alzheimers Dis, 2017, 60(2): 699-706. doi: 10.3233/JAD-170287 [12] Pu ZP, Xu WJ, Lin Y, et al. Oxidative stress markers and metal ions are correlated with cognitive function in Alzheimer's disease[J]. Am JAlzheimers Dis Other Demen, 2017, 32(6): 353-9. doi: 10.1177/1533317517709549 [13] Singh R, Kumar P, Mishra DN, et al. Effect of gender, age, diet and smoking status on the circadian rhythm of serum uric acid of healthy indians of different age groups[J]. Indian J Clin Biochem, 2019, 34 (2): 164-71. doi: 10.1007/s12291-017-0724-8 [14] 战静, 徐平. α7烟碱型乙酰胆碱受体在认知功能障碍及神经保护中的作用[J]. 实用医学杂志, 2019, 35(4): 662-5. https://www.cnki.com.cn/Article/CJFDTOTAL-SYYZ201904037.htm [15] Ma H, Wang X, Guo XY, et al. Distinct uric acid trajectories are associated with different risks of incident hypertension in middleaged adults[J]. Mayo Clin Proc, 2019, 94(4): 611-9. doi: 10.1016/j.mayocp.2018.08.042 [16] Jan MI, Khan RA, Sultan A, et al. Analysis of NT-proBNP and uric acid due to left ventricle hypertrophy in the patients of aortic valve disease[J]. Pak J Med Sci, 2018, 35(1): 183-188. http://www.researchgate.net/publication/329873336_Analysis_of_NT-proBNP_and_uric_acid_due_to_left_ventricle_hypertrophy_in_the_patients_of_aortic_valve_disease [17] 方依卡, 潘速跃, 赵德强, 等. 卒中患者脑白质疏松的危险因素[J]. 国际脑血管病杂志, 2011, 19(1): 58-62. https://www.cnki.com.cn/Article/CJFDTOTAL-NXGB201409001.htm [18] 郭大志, 齐亚南, 潘树义. 高压氧对轻度认知障碍的脑白质疏松症患者的疗效和安全性研究[J]. 重庆医学, 2020, 49(16): 2637-41. https://www.cnki.com.cn/Article/CJFDTOTAL-CQYX202016006.htm -






 下载:
下载: