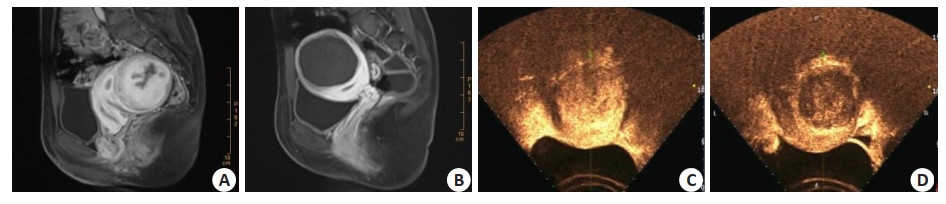
Application of enhanced MRI and contrast-enhanced ultrasound in the evaluation of HIFU uterine fibroids before and after treatment
-
摘要:
目的比较增强MRI与超声造影在高强度聚焦超声(HIFU)治疗子宫肌瘤疗效观察中的应用价值。 方法 选取2019年2月~2020年2月我院收治102例行HIFU治疗的子宫肌瘤患者,患者治疗前后均进行超声造影和增强MRI检查,比较两种检测方法在疗效评价中的作用。 结果两种检测方法治疗前后肌瘤均径、肌瘤体积比较差异无统计学意义(P>0.05),其中增强MRI可明显显示肌瘤的大小和边界,而超声造影对子宫肌瘤的边界图像显示相对不足,且增强MRI图像质量评分、消融率高于超声造影, 差异有统计学意义(P<0.05);增强MRI和超声造影对消融区、残余灶均能有效显示,两者评价HIFU治疗子宫肌瘤总有效率比 较差异无统计学意义(P>0.05)。 结论增强MRI在子宫肌瘤定性诊断方面优于超声造影,而超声造影检查更具有可重复性、灵活性,两者均为HIFU治疗前后的必要检查。 Abstract:ObjectiveTo compare the application value of enhanced MRI and contrast-enhanced ultrasound in efficacy observation of high-intensity focused ultrasound (HIFU) for uterine fibroids. MethodsBetween February 2019 and February 2020, 102 patients with uterine fibroids underwent HIFU treatment in our hospital were selected for contrast- enhanced ultrasound and enhanced MRI pre- and postoperatively. The effects of the two detection methods in the evaluation of efficacy were compared. ResultsThere was no significant difference in the average diameter and volume of fibroids before and after treatment by the two detection methods (P>0.05). The enhanced MRI could clearly show the size and boundary of fibroids, while contrast- enhanced ultrasound showed relatively insufficient automatic fibroids. The image quality score and the ablation rate of Enhanced MRI were higher than those of contrast-enhanced ultrasound (P < 0.05). Enhanced MRI and contrastenhanced ultrasound were effective in presenting ablation areas and residual lesions. There was no significant difference in the total effective rate of HIFU for uterine fibroids between the two (P>0.05). ConclusionEnhanced MRI is superior to contrastenhanced ultrasound in the qualitative diagnosis of uterine fibroids, while contrast-enhanced ultrasound examination is more repeatable and flexible. Both are necessary examinations before and after HIFU treatment.c -
Key words:
- enhanced MRI /
- contrast-enhanced ultrasound /
- uterine fibroids /
- efficacy evaluation
-
表 1 两种检测方法图像质量和消融率比较
Table 1. Comparison of image quality and ablation rate by detection methods (n=153, Mean±SD)
检查 图像质量评分 消融率(%) 增强MRI 3.8±0.4 80.4±10.5 超声造影 2.7±0.5 72.6±11.8 t 21.249 6.108 P 0.000 0.000 表 2 两组残余灶检查情况比较
Table 2. Comparison of residual focus inspection between the two groups (n=153)
检查 消融区 残余灶 + - + - 增强MRI 153 0 151 2 超声造影 153 0 150 3 表 3 治疗前后子宫肌瘤体积变化
Table 3. Volume changes of uterine fibroids before and after treatment (n=153, Mean±SD)
检查 肌瘤均径(cm) 肌瘤体积(cm3) 治疗前 治疗后 治疗前 治疗后 增强MRI 54.9±6.4 13.6±1.5 113.6±27.4 85.6±10.5 超声造影 53.7±6.8 13.9±1.2 110.5±29.2 83.9±11.3 t 1.590 1.932 0.958 1.363 P 0.113 0.054 0.339 0.174 表 4 两种方法评价HIFU疗效比较
Table 4. Comparison of the efficacy of HIFU by two methods [n(%), n=153]
检查方式 显效 有效 无效 总有效 增强MRI 84(54.90) 41(26.80) 28(18.30) 125(81.70) 超声造影 82(53.59) 44(28.76) 27(17.65) 126(83.35) χ2 - 0.148 P - 0.929 -
[1] 耿丽娜. 术前超声鉴别子宫肌瘤可靠性的研究[J]. 湖南师范大学学报: 医学版, 2018, 15(1): 165-9. doi: 10.3969/j.issn.1673-016X.2018.01.054 [2] 边芳, 张黎莎, 刘伟丽. 80例子宫内膜间质肉瘤患者DWI检查图像分析及相关生物学行为评价[J]. 中华生物医学工程杂志, 2019, 25 (3): 376-80. http://d.wanfangdata.com.cn/periodical/xdlcyxswgcxzz201903036 [3] Zeccolini G, del Biondo D, Cicero C, et al. Comparison of ContrastEnhanced Ultrasound Scan (CEUS) and MRI in the follow-up of cryoablation for small renal tumors. Experience on 25 cases[J]. Urol J, 2014, 81(23_suppl): S1-8. doi: 10.5301/RU.2014.11986 [4] 洪晓纯, 王忠, 曾淑芬, 等. 磁共振平扫在子宫肌瘤海扶刀治疗后近期疗效评估及与增强扫描的比较[J]. 广东医学, 2020, 41(5): 501-5. https://www.cnki.com.cn/Article/CJFDTOTAL-GAYX202005016.htm [5] Johnson BE, Crawford J, Downey RJ, et al. Small cell lung cancer clinical practice guidelines in oncology[J]. J Natl Compr Canc Netw, 2006, 4(6): 602-22. doi: 10.6004/jnccn.2006.0050 [6] 李爱丽, 穆清林, 苏琳. 超声造影与MRI对胰腺囊性病变的诊断价值比较[J]. 中国CT和MRI杂志, 2018, 16(7): 103-5, 2. doi: 10.3969/j.issn.1672-5131.2018.07.031 [7] Yu L, Zhang HF, Jiang DW, et al. Comparison of imaging features and diagnostic values of MRI, CT and contrast-enhanced ultrasonography in the diagnosis of cervical carcinoma staging[J]. Eur Rev Med Pharmacol Sci, 2018, 22(15): 4784-91. http://www.ncbi.nlm.nih.gov/pubmed/30070310 [8] 杨丽新, 徐士丞, 陈莹, 等. 超声造影评估子宫肌层肿瘤的形态学特征[J]. 解剖学研究, 2018, 40(6): 514-6. https://www.cnki.com.cn/Article/CJFDTOTAL-GDJP201806015.htm [9] Lin J, Baohua HU, Lan F, et al. Contrast-enhanced ultrasound and MRI factors influencing therapeutic effects of high intensity focused ultrasound in treatment of hysteromyoma[J]. Oncoradiology, 2018, 9 (15): 264-7. http://www.zhangqiaokeyan.com/academic-journal-cn_shanghai-medical-imaging_thesis/0201225451081.html [10] 胡红, 许芙蓉, 但汉丽, 等. 超声造影评价高强度聚焦超声消融治疗子宫肌瘤疗效的价值[J]. 川北医学院学报, 2019, 34(3): 363-6, 374. doi: 10.3969/j.issn.1005-3697.2019.03.11 [11] Zhou LL, Tang LM, Yang T, et al. Comparison of contrast-enhanced ultrasound with MRI in the diagnosis of complex cystic renal masses: a meta-analysis[J]. Acta Radiol Stock Swed, 2018, 59(10): 1254-63. http://smartsearch.nstl.gov.cn/paper_detail.html?id=84d6c139897c1116f198726652ea6a6a [12] 苏萍, 许永华, 王伊, 等. 增强MRI和超声造影评估高强度聚焦超声治疗子宫肌瘤的比较研究[J]. 介入放射学杂志, 2019, 28(2): 138-42. doi: 10.3969/j.issn.1008-794X.2019.02.008 [13] Zhou LL, Tang LM, Yang T, et al. Comparison of contrast-enhanced ultrasound with MRI in the diagnosis of complex cystic renal masses: a meta-analysis[J]. Acta Radiol Stock Swed, 2018, 59(10): 1254-63. http://smartsearch.nstl.gov.cn/paper_detail.html?id=84d6c139897c1116f198726652ea6a6a [14] 寸江平, 赵卫, 范宏杰, 等. MRI在高强度聚焦超声消融子宫肌瘤中的应用进展[J]. 中国医学影像技术, 2019, 35(6): 946-9. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYXX201906054.htm [15] Sawatzki M, Hechelhammer L, Semela D, et al. Comparison of the diagnostic accuracy of contrast-enhanced ultrasound (CEUS) within 5 minutes and CT/MRI for diagnosing vital tumor tissue after RFA/ TACE in HCC and liver metastasis in a tertiary Swiss GI center[J]. Eur J Ultrasound, 2018, 39(10): 124-9. doi: 10.1055/s-0038-1670435 [16] 刘政, 田锦, 张惠, 等. 利用超声造影评估高强度聚焦超声和子宫动脉栓塞治疗子宫肌瘤疗效差异[J]. 实用妇产科杂志, 2019, 35(8): 633-8. https://www.cnki.com.cn/Article/CJFDTOTAL-SFCZ201908022.htm [17] 金琳, 王迎春, 封岚, 等. 超微血流成像技术评估高强度聚焦超声治疗子宫肌瘤疗效的应用价值[J]. 中华超声影像学杂志, 2018, 27(4): 334-7. doi: 10.3760/cma.j.issn.1004-4477.2018.04.015 [18] Sanampudi S, Gabriel G, Hoffman M, et al. Impending fibroid expulsion on MRI after uterine fibroid embolization[J]. Radiol Case Rep, 2019, 14(6): 673-7. doi: 10.1016/j.radcr.2019.03.011 [19] 彭红艳, 余松远, 贺飞, 等. 超声造影在经皮微波消融治疗子宫肌瘤疗效观察中的应用价值[J]. 医学影像学杂志, 2018, 28(9): 1506-9. https://www.cnki.com.cn/Article/CJFDTOTAL-XYXZ201809026.htm [20] 王英姿, 马建平. CEUS和MRI评价高强度聚焦超声治疗子宫肌瘤的效果对比[J]. 中国CT和MRI杂志, 2020, 18(4): 114-6. doi: 10.3969/j.issn.1672-5131.2020.04.034 [21] Torkzaban M, Machado P, Gupta I, et al. Contrast-enhanced ultrasound for monitoring non-surgical treatments of uterine fibroids: a systematic review[J]. Ultrasound Med Biol, 2021, 47(1): 3-18. doi: 10.1016/j.ultrasmedbio.2020.09.016 [22] 魏庆, 陈锦云, 刘一诺, 等. 子宫肌瘤超声消融后早期子宫浆肌层损伤的MRI评价[J]. 第三军医大学学报, 2019, 41(12): 1161-6. https://www.cnki.com.cn/Article/CJFDTOTAL-DSDX201912011.htm [23] 范宏杰, 赵卫, 谢璇丞, 等. 对比增强MRI在预测HIFU消融子宫肌瘤效果中的价值[J]. 中国医学计算机成像杂志, 2018, 24(6): 500-4. doi: 10.3969/j.issn.1006-5741.2018.06.011 [24] Small Layne A, Pedroso J. Comparison of MRI fibroid volume and post-myomectomy specimen volume[J]. J Minim Invasive Gynecol, 2018, 25(7): S97. http://www.researchgate.net/publication/328670972_Comparison_of_MRI_Fibroid_Volume_and_Post-Myomectomy_Specimen_Volume [25] 张璐, 朱辉, 周崑, 等. 超声造影剂对超声消融单发子宫肌瘤增效作用的临床观察[J]. 重庆医科大学学报, 2019, 44(1): 34-8. https://www.cnki.com.cn/Article/CJFDTOTAL-ZQYK201901008.htm -







 下载:
下载: