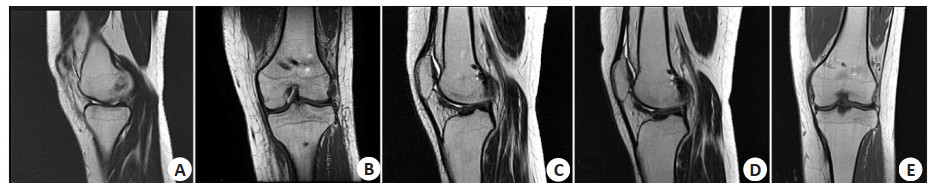
Application of MRI in the preoperative guidance and evaluation ofsurgical effects ofanterior cruciate ligament reconstruction combined with partial synovectomy
-
摘要:
目的探讨MRI在前交叉韧带(ACL)重建术联合滑膜部分切除术前指导及手术效果评估中的应用价值。 方法选择2017年1月~2019年1月我院收治的80例ACL损伤患者作为观察组,接受ACL重建术和滑膜部分切除术治疗;另外选择无损伤的MRI检查者40例作为对照组。观察组手术前后、对照组均进行MRI检查,记录两组的ACL角、PCL夹角、PCL指数、Blumensaat角、胫骨前移指标。观察组患者术后1年来院接受MRI检查,进行前抽屉实验、Lachman实验、轴移实验,用Lysholm评分、Tegner评分评估膝关节功能,计算ACL移植物MRI评分。 结果观察组术后ACL角较术前升高,PCL指数、Blumensaat角、胫骨前移较术前降低(P < 0.05),与对照组差异无统计学意义(P < 0.05),术后PCL夹角较术前升高,高于对照组(P < 0.05)。80例患者中,前抽屉实验、Lachman实验、轴移实验3项检查 结果均为阴性者70例(87.50%),1项或以上为阳性者10例(12.50%)。移植物的完整性和信号依据Rak’s法分级:1级73例(92.25%),2级7例(8.75%)。Lysholm膝关节评分88.63±6.51分,Tegner膝关节运动评分8.02±1.56分,较术前升高(P < 0.05),ACL移植物MRI评分72.13±10.02分。Pearson相关性分析 结果显示,ACL移植物MRI评分与Lysholm膝关节评分、Tegner膝关节运动评分呈正相关(r=0.675、0.742,P < 0.05)。 结论ACL重建术联合滑膜部分切除术对ACL损伤患者有较好的治疗效果,可恢复膝关节功能和稳定性,MRI是术前指导、术后手术效果评估的有力工具。 Abstract:ObjectiveTo explore the application value of MRI in the preoperative guidance and evaluation of surgical effect sofanterior cruciate ligament (ACL) reconstruction combined with partial synovectomy. MethodsEighty patients with ACL injury admitted to our hospital from January 2017 to January 2019 were selected. The patients received ACL reconstruction and partial synovectomy. We selected 40 uninjured people with MRI examination as control group. MRI examination was performed in observation group before and after surgery and in control group. The ACL angle, PCL included angle, PCL index, Blumensaat angle, and tibial anterior movement index were recorded in the two groups. Observation group received MRI examination, anterior drawer test, Lachman test, and axis shift test in the hospital during one year after surgery. Lysholm score and Tegner score were used to evaluate the knee joint function, and the MRI score of ACL graft was calculated. ResultsThe ACL angle in observation group was higher than that before surgery while the PCL index, Blumensaat angle. The tibial anterior movement were lower than those before surgery (P < 0.05). There were no significant differences compared with those in control group (P>0.05). The PCL included angle after surgery was higher than that before surgery, and higher than that in control group (P < 0.05). Among the 80 patients, 70 cases (87.50%) were negative for the anterior drawer test, Lachman test and axis shift test, and 10 cases (12.50%) were positive for 1 testor or more. The integrity and signal of the graft were graded according to Rak's method, showing 73 cases (92.25%) of grade 1 and 7 cases (8.75%)of grade 2. Lysholm knee joint score with 88.63±6.51 points and Tegner knee joint motor score with 8.02±1.56 point, which were higher than those before surgery (P < 0.05). The MRI score of ACL graft was 72.13±10.02 points. Pearson correlation analysis results showed that MRI score of ACL graft was significantly positively correlated with Lysholm knee joint score and Tegner knee joint motor score (r=0.675, 0.742, P < 0.05). ConclusionACL reconstruction combined with partial synovectomy has good therapeutic effects on patients with ACL injury. It can restore knee joint function and stability. MRI is a powerful tool for preoperative guidance and evaluation of postoperative surgical effects. -
表 1 观察组手术前后与对照组MRI检查结果比较
Table 1. Comparison of MRI examination results between observation group and control group before and after surgery (Mean±SD)
项目 对照组(n=40) 观察组(n=80) 术前 术后 ACL角(°) 52.31±7.95 34.62±6.14# 50.16±8.37* PCL夹角(°) 130.32±15.91 121.35±16.74# 137.23±15.27*# PCL指数 0.27±0.06 0.39±0.06# 0.29±0.05* Blumensaat角(°) -10.96±2.10 8.95±1.31# -11.78±2.57* 胫骨前移(cm) 1.19±0.15 5.89±0.95# 1.28±0.20* *P < 0.05 vs观察组术前; #P < 0.05 vs对照组. -
[1] Dhawan A, Gallo RA, Lynch SA. Anatomic tunnel placement in anterior cruciate ligament reconstruction[J]. J Am Acad Orthop Surg, 2016, 24(7): 443-54. doi: 10.5435/JAAOS-D-14-00465 [2] Desai N, Andernord D, Sundemo D, et al. Revision surgery in anterior cruciate ligament reconstruction: a cohort study of 17, 682 patients from the Swedish National Knee Ligament Register[J]. Knee Surg Sports TraumatolArthrosc, 2017, 25(5): 1542-54. doi: 10.1007/s00167-016-4399-0 [3] Svantesson E, Sundemo D, Hamrin Senorski E, et al. Double-bundle anterior cruciate ligament reconstruction is superior to single-bundle reconstruction in terms of revision frequency: a study of 22, 460 patients from the Swedish National Knee Ligament Register[J]. Knee Surg Sports TraumatolArthrosc, 2017, 25(12): 3884-91. doi: 10.1007/s00167-016-4387-4 [4] Prentice HA, Lind M, Mouton C, et al. Patient demographic and surgical characteristics in anterior cruciate ligament reconstruction: a description of registries from six countries[J]. Br J Sports Med, 2018, 52(11): 716-22. doi: 10.1136/bjsports-2017-098674 [5] Lai CCH, Ardern CL, Feller JA, et al. Eighty-three per cent of elite Athletes return to preinjury sport after anterior cruciate ligament reconstruction: a systematic review with meta- analysis of return to sport rates, graft rupture rates and performance outcomes[J]. Br J Sports Med, 2018, 52(2): 128-38. doi: 10.1136/bjsports-2016-096836 [6] 张南, 钱学江, 刘中冲, 等. MRI对膝关节前交叉韧带损伤诊断的假阳性及假阴性的病例分析[J]. 医学影像学杂志, 2017, 27(5): 887-91. https://www.cnki.com.cn/Article/CJFDTOTAL-XYXZ201705031.htm [7] Leiter J, Elkurbo M, McRae S, et al. Using pre-operative MRI to predict intraoperative hamstring graft size for anterior cruciate ligament reconstruction[J]. Knee Surg Sports Traumatol Arthrosc, 2017, 25(1): 229-35. doi: 10.1007/s00167-016-4205-z [8] 吴冰, 陆伟, 王大平, 等. 前交叉韧带重建术后MRI评分与临床膝关节主、客观功能评分的对比研究[J]. 中国临床解剖学杂志, 2016, 34 (6): 677-84. https://www.cnki.com.cn/Article/CJFDTOTAL-ZLJZ201606018.htm [9] 张君, 郑奎宏, 文涛. MRI评估官兵前交叉韧带重建术后修复价值研究[J]. 人民军医, 2016, 59(3): 226-8. https://www.cnki.com.cn/Article/CJFDTOTAL-RMJZ201603010.htm [10] 王志斌, 马春忠, 于明珠, 等. 前交叉韧带损伤: MRI征象相关性分析[J]. 临床放射学杂志, 2017, 36(10): 1472-6. https://www.cnki.com.cn/Article/CJFDTOTAL-LCFS201710023.htm [11] 王道安. MRI对前交叉韧带损伤的诊断意义及其与关节镜比较研究[J]. 中国CT和MRI杂志, 2017, 15(7): 146-9. doi: 10.3969/j.issn.1672-5131.2017.07.046 [12] 王健, 王海军, 林霖, 等. 前交叉韧带重建失败的影响因素分析[J]. 中国修复重建外科杂志, 2019, 33(12): 1543-6. https://www.cnki.com.cn/Article/CJFDTOTAL-ZXCW201912015.htm [13] Galanis N, Savvidis M, Tsifountoudis I, et al. Correlation between semitendinosus and gracilis tendon cross-sectional area determined using ultrasound, magnetic resonance imaging and intraoperative tendon measurements[J]. J Electromyogr Kinesiol, 2016, 26: 44-51. doi: 10.1016/j.jelekin.2015.11.006 [14] Tsifountoudis I, Bisbinas I, Kalaitzoglou I, et al. The natural history of donor hamstrings unit after anterior cruciate ligament reconstruction: a prospective MRI scan assessment[J]. Knee Surg Sports TraumatolArthrosc, 2017, 25(5): 1583-90. doi: 10.1007/s00167-015-3732-3 [15] Thwin L, Ho SW, Tan TJL, et al. Pre-operative MRI measurements versus anthropometric data: Which is more accurate in predicting 4- stranded hamstring graft size in anterior cruciate ligament reconstruction?[J]. Asia Pac J Sports Med Arthrosc Rehabil Technol, 2020, 22: 5-9. http://www.sciencedirect.com/science/article/pii/S2214687320300133 [16] Konrath JM, Vertullo CJ, Kennedy BA, et al. Morphologic characteristics and strength of the hamstring muscles remain altered at 2 years after use of a hamstring tendon graft in anterior cruciate ligament reconstruction[J]. Am J Sports Med, 2016, 44(10): 2589-98. doi: 10.1177/0363546516651441 [17] 高丽香, 袁慧书. 前交叉韧带重建术后关节感染与粘连的MRI征象[J]. 中国医学影像技术, 2018, 34(6): 915-8. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYXX201806043.htm [18] Buckthorpe M, Danelon F, la Rosa G, et al. Recommendations for hamstring function recovery after ACL reconstruction[J]. Sports Med, 2020. doi: 10.1007/s40279-020-01400-x [19] 张壮岱, 金社辉, 冯志军, 等. 解剖型前交叉韧带重建术前、术后MRI与正常膝关节MRI比较分析[J]. 解放军医药杂志, 2016, 28(8): 39-43. https://www.cnki.com.cn/Article/CJFDTOTAL-HBGF201608010.htm [20] 张君, 郭勇, 林建宁. 前交叉韧带重建术后MRI评价和临床评估的相关性分析[J]. 局解手术学杂志, 2016, 25(2). https://www.cnki.com.cn/Article/CJFDTOTAL-JJXZ201602006.htm -







 下载:
下载: