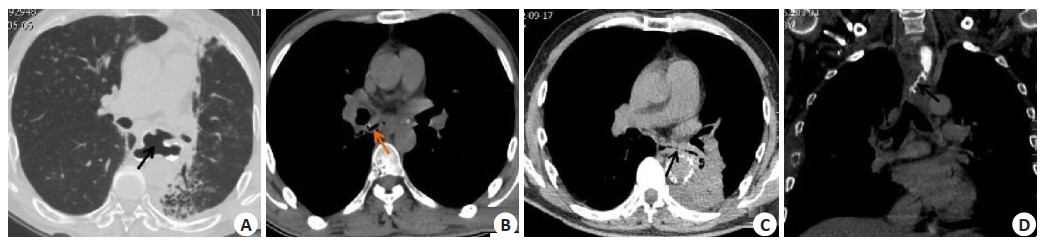
Comparison of MSCT scan and upper gastrointestinal angiography in diagnosis and treatment of acquired esophagus and bladder
-
摘要:
目的探讨多层螺旋CT(MSCT)扫描与上消化道造影检查在获得性食管瘘诊疗中的价值差异。 方法选取高度怀疑可能发生放化疗后食管瘘的患者81例作为研究对象,经胃食管镜检查,其中56例确诊为放疗后继发性食管瘘,25例患者未发生继发性食管瘘;所有患者均在接受胃食管镜检查前接受了上消化道造影、MSCT扫描检查,以胃食管镜检查 结果作为金标准进行判断,计算上消化道造影、MSCT扫描诊断放疗后食管瘘的价值差异。 结果确诊继发性食管瘘56例患者中,以胃食管镜检查 结果作为金标准,MSCT对瘘口位置分布在气管、左主支气管、右主支气管、左中肺支气管、右上肺支气管的符合率均达到100%,上消化道造影检查仅对瘘口位置分布在气管的诊断符合率达到100%;整体上看,MSCT诊断瘘口位置的符合率96.43%高于上消化道造影检查的80.36%,差异具有统计学意义(P < 0.05);MSCT对窗型瘘、管型瘘、线型食管瘘、不规则形状食管瘘的检出率分别为50.00%、23.21%、12.50%、10.71%,上消化道造影检查对窗型瘘、管型瘘、线型食管瘘、不规则形状食管瘘的检出率分别为44.64%、19.64%、8.93%、7.14%;以胃食管镜检查 结果作为金标准建立四格表,MSCT诊断食管瘘的灵敏度为96.43%、特异度为96.00%;上消化道食管造影诊断食管瘘的灵敏度为80.36%、特异度为88.00%。 结论MSCT扫描与上消化道造影检查在获得性食管瘘相比较,前者的检出率、诊断价值更高,且具有无创、检查快捷方便的特点。 Abstract:ObjectiveTo explore the value difference between multi- slice spiral CT (MSCT) scan and upper gastrointestinal angiography in the diagnosis and treatment of acquired esophageal fistula. MethodsEighty-one patients with high suspicion of esophageal fistula after radiotherapy and chemotherapy were selected as the research objects. After gastroesophageal examination, 56 patients were diagnosed as secondary esophageal fistula after radiotherapy, and 25 patients did not develop secondary esophageal fistula. All patients before receiving gastroesophageal examination received upper gastrointestinal angiography and MSCT scan. The gastroesophageal examination results were used as the gold standard to determine the value of upper gastrointestinal angiography and MSCT scan in diagnosing esophageal fistula after radiotherapy. ResultsAmong 56 patients diagnosed with secondary esophageal fistula, the results of gastroesophageal endoscopy were used as the gold standard. MSCT's coincidence rate of fistula location in trachea, left main bronchus, right main bronchus, left middle lung bronchus, and right upper lung bronchus were all reaching 100%. The upper gastrointestinal angiography only diagnosed the fistula location in the trachea with a diagnostic coincidence rate of 100%. Overall, the MSCT diagnosis of the fistula location was higher than the upper gastrointestinal angiography (P < 0.05). The detection rates of MSCT for window fistula, tract fistula, linear esophageal fistula, and irregular- shaped esophageal fistula were 50.00%, 23.21%, 12.50%, 10.71%, respectively. The detection rates of window fistulas, tube fistulas, linear esophageal fistulas, and irregular-shaped esophageal fistulas by gastrointestinal angiography were 44.64%, 19.64%, 8.93%, and 7.14%, respectively. The results of gastroesophageal endoscopy were used as the gold standard Establishing a four-grid table. MSCT had a sensitivity of 96.43% and a specificity of 96.00% in diagnosing esophageal fistula. The upper gastrointestinal esophagography had a sensitivity of 80.36% and a specificity of 88.00%. ConclusionCompared with MSCT scanning and upper gastrointestinal angiography in acquired esophageal fistula, the former has higher detection rate and diagnostic value, and has the characteristics of non-invasive, quick and convenient examination. -
表 1 一般资料分布情况
Table 1. General information distribution
一般资料 例数 构成比(%) 年龄(岁) ≥60 43 53.09 < 60 38 46.91 性别 男 43 53.09 女 38 46.91 食管癌位置 上段 17 20.99 中段 58 71.60 下段 6 7.41 临床症状 反复咳嗽咳痰 55 67.90 进食后突发咳嗽 23 28.40 咯血 3 3.70 确诊病因 继发性食管瘘 56 69.14 肺隔离症 17 20.99 假性动脉瘤破裂 8 9.88 表 2 两种检测方法对食管瘘瘘口位置分布检测对比
Table 2. Comparison of two methods for detecting the location distribution of esophageal fistula
瘘口位置分布 MSCT检查符合率 上消化道造影符合率 χ2 P 例数 构成比(%) 例数 构成比(%) 气管(n=23) 23 100.00 23 100.00 - - 左主支气管(n=7) 7 100.00 6 85.71 1.077 0.299 右主支气管(n=8) 8 100.00 5 62.50 3.692 0.055 左下肺支气管(n=5) 4 80.00 3 60.00 0.476 0.490 右下肺支气管(n=8) 7 87.50 5 62.50 1.333 0.248 左中肺支气管(n=3) 3 100.00 2 66.67 1.200 0.273 右上肺支气管(n=2) 2 100.00 1 50.00 1.333 0.248 合计(n=56) 54 96.43 45 80.36 5.238 0.022 MSCT: 多层螺旋CT. 表 3 两种检测方法对食管瘘瘘口分型的检出情况对比
Table 3. Comparison of the two methods for detecting esophageal fistula
食管瘘分型 MSCT诊断 上消化道造影诊断 例数 构成比(%) 例数 构成比(%) 窗型 28 50.00 25 44.64 管型 13 23.21 11 19.64 线型 7 12.50 5 8.93 不规则型 6 10.71 4 7.14 合计 54 96.43 45 80.36 表 4 两种检测方法对食管瘘诊断的四格表
Table 4. Four tables for diagnosis of esophageal fistula by two detection methods (n)
MSCT 胃食管镜确诊 合计 上消化道造影 胃食管镜确诊 合计 阳性 阴性 阳性 阴性 阳性 54 1 55 阳性 45 3 48 阴性 2 24 26 阴性 11 22 33 合计 56 25 81 合计 56 25 81 表 5 两种检测方法对食管瘘的诊断价值
Table 5. Diagnostic value of two methods for esophageal fistula (%)
诊断方法 灵敏度 特异度 漏诊率 误诊率 MSCT 96.43 96.00 3.57 4.00 上消化道造影 80.36 88.00 19.64 12.00 -
[1] 章婷婷, 姚玲雅, 方昊, 等. 气管食管瘘的内镜下治疗[J]. 临床消化病杂志, 2018, 30(4): 264-6. doi: 10.3870/lcxh.j.issn.1005-541X.2018.04.17 [2] Parolini F, Morandi A, Macchini F, et al. Esophageal atresia with proximal tracheoesophageal fistula: a missed diagnosis[J]. J Pediatr Surg, 2013, 48(6): E13-7. doi: 10.1016/j.jpedsurg.2013.04.018 [3] Beasley SW. Oesophageal atresia and tracheo-oesophageal fistula [J]. Surg Oxf, 2019, 37(11): 623-7. http://www.ncbi.nlm.nih.gov/pubmed/3416169 [4] 陈云, 杨绍军, 王家平, 等. 获得性气管、支气管食管瘘外科治疗进展[J]. 中国现代手术学杂志, 2018, 22(6): 472-5. https://www.cnki.com.cn/Article/CJFDTOTAL-XDSS201806018.htm [5] Forero ZL, Pappagallo M. Esophageal atresia and tracheoesophageal fistula[J]. N Engl J Med, 2018, 379(7): e11. doi: 10.1056/NEJMicm1801712 [6] Wu R, Geng LD, Zhao ZH, et al. Clinical application of oral meglumine diatrizoate esophagogram in screening for esophageal fistula during radiotherapy or chemoradiotherapy for esophageal cancer[J]. Front Oncol, 2020, 10: 562147. doi: 10.3389/fonc.2020.562147 [7] Xu YY, Wang LL, He B, et al. Development and validation of a risk prediction model for radiotherapy- related esophageal fistula in esophageal cancer[J]. Radiat Oncol, 2019, 14(1): 181. doi: 10.1186/s13014-019-1385-y [8] Hiroyuki K, Atsuyuki Y. Minimally Invasive Advanced Surgery for Esophageal Atresia with Tracheoesophageal Fistula and Biliary Atresia[J]. Juntend Med J, 2018, 64(1): 31-6. doi: 10.14789/jmj.2018.64.JMJ18-R01 [9] Kammerer S, Schuelke C, Berkemeyer S, et al. The role of multislice computed tomography (MSCT) angiography in the diagnosis and therapy of non-occlusive mesenteric ischemia (NOMI): Could MSCT replace DSA in diagnosis?[J]. PLoS One, 2018, 13(3): e0193698. doi: 10.1371/journal.pone.0193698 [10] 鲍燕敏, 李晶, 赵海霞, 等. 胃管内灌注美兰支气管镜观察法对儿童先天性气管食管瘘诊断价值分析[J]. 中国实用儿科杂志, 2017, 32 (3): 209-14. https://www.cnki.com.cn/Article/CJFDTOTAL-ZSEK201703016.htm [11] 刘永熙, 郭庆禄, 陈文俊, 等. 多层螺旋CT在先天性食管闭锁及气管食管瘘中的应用[J]. 影像诊断与介入放射学, 2013, 22(5): 336-9. doi: 10.3969/j.issn.1005-8001.2013.05.004 [12] 范磊, 尹传高, 朱立春, 等. MSCT在新生儿Ⅲ型食管闭锁检查中的应用[J]. 实用放射学杂志, 2018, 34(5): 753-5. doi: 10.3969/j.issn.1002-1671.2018.05.027 [13] 方涛. 多层螺旋CT检查对食管癌放疗后并发食管瘘小瘘口的诊断价值[J]. 中国基层医药, 2019, 26(11): 1297-300. doi: 10.3760/cma.j.issn.1008-6706.2019.11.005 [14] 徐超, 张欣贤, 李成龙, 等. 矢状位CT扫描技术在新生儿食管闭锁并食管气管瘘中的临床价值[J]. 实用放射学杂志, 2018, 34(4): 582-5. doi: 10.3969/j.issn.1002-1671.2018.04.025 [15] 段青松. 多层螺旋CT在食管瘘诊断中的应用价值[J]. 临床医学研究与实践, 2020, 5(34): 138-9. https://www.cnki.com.cn/Article/CJFDTOTAL-YLYS202034050.htm [16] 潘壬清, 曾红辉, 邓周强, 等. 上消化道异物的多层螺旋CT诊断价值[J]. 深圳中西医结合杂志, 2018, 28(15): 95-7, 199. https://www.cnki.com.cn/Article/CJFDTOTAL-SZZX201815044.htm [17] 陈华. 多层螺旋CT检查对食管癌放疗后并发食管瘘小瘘口的诊断价值研究[J]. 影像研究与医学应用, 2020, 4(19): 45-6. https://www.cnki.com.cn/Article/CJFDTOTAL-YXYY202019025.htm [18] 王力, 苏雪娟, 陈体, 等. 胸部CT在食管癌支架植入术后诊断食管气管瘘中的价值分析[J]. 数理医药学杂志, 2019, 32(12): 1796-7. doi: 10.3969/j.issn.1004-4337.2019.12.028 [19] 加静, 肖高社. C臂引导下介入造影诊断和营养管植入治疗食管瘘的临床价值[J]. 现代肿瘤医学, 2018, 26(23): 3768-71. https://www.cnki.com.cn/Article/CJFDTOTAL-SXZL201823016.htm [20] 蒋呈欣. CT对食管癌术后吻合口瘘的诊断价值分析[J]. 现代医学与健康研究电子杂志, 2018, 2(13): 57, 59. https://www.cnki.com.cn/Article/CJFDTOTAL-XYJD201813043.htm [21] Gawad N, Wayne C, Bass J, et al. A chest tube may not be needed after surgical repair of esophageal atresia and tracheoesophageal fistula[J]. Pediatr Surg Int, 2018, 34(9): 967-70. doi: 10.1007/s00383-018-4307-4 [22] Sinha M, Pandey NN, Sharma A. Left circumflex artery to left atrial fistula: a rare entity diagnosed on computed tomography angiography[J]. J Cardiovasc Comput Tomogr, 2020, 14(6): e120-1. http://www.ncbi.nlm.nih.gov/pubmed/31420307 [23] Taniyama TK, Tsuda T, Miyakawa K, et al. Analysis of fistula formation of T4 esophageal cancer patients treated by chemoradiotherapy[J]. Esophagus, 2020, 17(1): 67-73. http://www.researchgate.net/publication/335726864_Analysis_of_fistula_formation_of_T4_esophageal_cancer_patients_treated_by_chemoradiotherapy -







 下载:
下载: