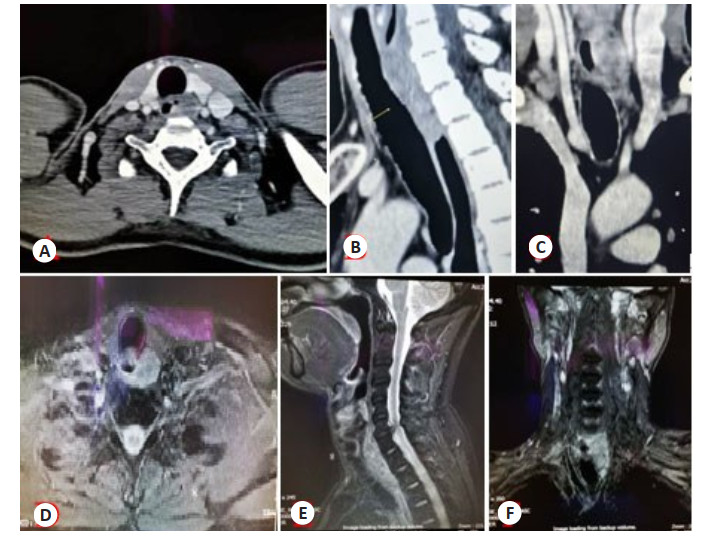
Application value of CT and MRI-DWI in preoperative evaluation of esophageal cancer
-
摘要:
目的探究CT以及磁共振扩散加权成像(MRI-DWI)在食管癌术前评估中应用价值。 方法回顾性分析我院2017年8月~ 2019年7月期间收治107例食管癌患者相关资料,患者均接受手术治疗,手术前行CT以及MRI-DWI检查,术后行病理检查,分析CT与MRI-DWI判断T分期以及N分期价值,比较CT与MRI-DWI判断食管癌病变长度及其与实际病变长度相关性。 结果以病理诊断作为金标准,CT诊断T1、T2、T3及T4分期Kappa值分别为0.719、0.695、0.843、0.851,MRI-DWI诊断T1、T2、T3及T4分期Kappa值分别为0.958、0.948、0.925、0.921;CT诊断N分期Kappa值为0.806,MRI-DWI诊断N分期Kappa值为0.977;CT测定食管癌病变长度高于MRI-DWI测定以及标本实际病变长度(P < 0.05),MRI-DWI测定食管癌病变长度与标本实际长度比较,差异无统计学意义(P>0.05);Pearson相关性分析 结果显示,CT、MRI-DWI测定食管癌病变长度与实际样本病变长度相关性较高(r=0.816、0.991;P < 0.05)。 结论CT、MRI-DWI均可用于评估食管癌患者术前分期以及病变长度,但是MRI-DWI在术前分期与病变长度评估中价值更佳。 Abstract:ObjectiveTo explore the application value of CT and magnetic resonance diffusion weighted imaging (MRI-DWI) in preoperative evaluation of esophageal cancer. MethodsRelevant data of 107 patients with esophageal cancer who were treated at the hospital from August 2017 to July 2019 were retrospectively analyzed. All patients underwent surgical treatment. CT and MRI-DWI were performed before surgery, and pathological examinations were performed after surgery. Value of CT and MRIDWI in T staging and N staging were analyzed. Lengths of esophageal cancer measured by CT and MRI-DWI were compared with the actual length. ResultsUsing pathological diagnosis as the golden standard, Kappa values of CT in diagnosis of T1, T2, T3 and T4 stages were 0.719, 0.695, 0.843 and 0.851, which of MRI-DWI were 0.958, 0.948, 0.925 and 0.921. Kappa values of CT and MRI-DWI in diagnosis of N stage were 0.806 and 0.977, respectively. Length of esophageal cancer measured by CT was significantly larger than that by MRI- DWI. There was no significant difference between the length of esophageal cancer measured by MRI-DWI and the actual length (P>0.05). Pearson correlation analysis showed that lengths of esophageal cancer measured by CT and MRI-DWI were highly correlated with the actual length (r=0.816, 0.991, P < 0.05). ConclusionBoth CT and MRI-DWI can be used to evaluate preoperative staging and lesion length of patients with esophageal cancer, but MRI-DWI is better for preoperative staging and lesion length evaluation. -
Key words:
- CT /
- MRI-DWI /
- esophageal cancer /
- preoperative evaluation /
- application value
-
表 1 CT与MRI-DWI判断患者T分期价值分析
Table 1. Value of CT and MRI-DWI in T staging
病理检查 CT 合计 MRI-DWI 合计 T1 T2 T3 T4 T1 T2 T3 T4 T1 9 5 0 0 14 13 1 0 0 14 T2 1 20 2 2 25 0 24 1 0 25 T3 0 2 38 3 43 0 1 41 1 43 T4 0 0 1 24 25 0 0 2 23 25 合计 10 27 41 29 107 13 26 44 24 107 灵敏度 64.29 80.00 88.37 96.00 92.86 96.00 95.35 92.00 特异度 98.92 91.46 95.31 93.90 100.00 98.78 95.24 98.78 准确度 94.39 88.79 92.52 94.39 99.07 98.13 95.28 97.20 Kappa值 0.719 0.695 0.843 0.851 0.958 0.948 0.925 0.921 表 2 CT与MRI-DWI判断患者N分期价值分析
Table 2. Value of CT and MRI-DWI in N staging
病理检查 CT 合计 MRI-DWI 合计 N0 N1 N0 N1 N0 29 2 31 30 1 31 N1 7 70 76 0 76 76 合计 36 71 107 30 77 107 灵敏度 93.55 96.77 特异度 90.91 100.00 准确度 91.67 99.07 Kappa值 0.806 0.977 表 3 CT与MRI-DWI测定病变长度情况比较
Table 3. Lengths of esophageal cancer measured by CT and MRI-DWI (n=107, Mean±SD)
方法 病变长度 CT 5.76±2.14 MRI-DWI 4.92±1.57a 标本长度 4.69±1.38a F 11.379 P < 0.001 aP < 0.05 vs CT. -
[1] Long L, Pang XX, Lei F, et al. SLC52A3 expression is activated by NF-κB p65/Rel-B and serves as a prognostic biomarker in esophageal cancer[J]. Cell Mol Life Sci, 2018, 75(14): 2643-61. doi: 10.1007/s00018-018-2757-4 [2] Arnold M, Laversanne M, Brown LM, et al. Predicting the future burden of esophageal cancer by histological subtype: international trends in incidence up to 2030[J]. Am J Gastroenterol, 2017, 112(8): 1247-55. doi: 10.1038/ajg.2017.155 [3] Cai WJ, Lu JJ, Xu RY, et al. Survival based radiographic-grouping for esophageal squamous cell carcinoma may impact clinical T stage[J]. Oncotarget, 2018, 9(10): 9512-30. doi: 10.18632/oncotarget.24056 [4] 胡超月, 李建彬, 王金之, 等. 基于增强三维CT、四维CT及锥形束CT确定食管癌原发肿瘤大体肿瘤体积的比较[J]. 中华放射医学与防护杂志, 2017, 37(6): 430-6. doi: 10.3760/cma.j.issn.0254-5098.2017.06.006 [5] Sun NN, Liu C, Ge XL, et al. Dynamic contrast-enhanced MRI for advanced esophageal cancer response assessment after concurrent chemoradiotherapy[J]. Diagn Interv Radiol, 2018, 24(4): 195-202. doi: 10.5152/dir.2018.17369 [6] Goense L, Borggreve AS, Heethuis SE, et al. Patient perspectives on repeated MRI and PET/CT examinations during neoadjuvant treatment of esophageal cancer[J]. Br J Radiol, 2018, 91(1086): 1-6. http://europepmc.org/abstract/MED/29498535 [7] 郑向东, 李天然, 郑志铖, 等. 磁共振弥散加权成像测量食管癌病变长度的应用价值[J]. 功能与分子医学影像学: 电子版, 2015, 4(2): 661-5. doi: 10.3969/j.issn.2095-2252.2015.02.008 [8] 黄一凡, 方昕, 董江宁, 等. 3.0T MRI和能谱CT对食管癌术前分期的比较[J]. 中国医学影像技术, 2015, 31(1): 52-6. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYXX201501021.htm [9] Tachimori Y, Ozawa S, Numasaki H, et al. Comprehensive registry of esophageal cancer in Japan, 2010[J]. Esophagus, 2017, 14(3): 189- 214. doi: 10.1007/s10388-017-0578-4 [10] Lee KD, Wang TY, Lu CH, et al. The bidirectional association between oral cancer and esophageal cancer: a population- based study in Taiwan over a 28-year period[J]. Oncotarget, 2017, 8(27): 44567-78. doi: 10.18632/oncotarget.17818 [11] 李慧敏, 李建彬, 李奉祥, 等. 4DCT、PET-CT与MRI勾画胸段食管癌大体肿瘤体积比较研究[J]. 中华放射肿瘤学杂志, 2020, 29(7): 508- 12. doi: 10.3760/cma.j.cn113030-20191008-00405 [12] Bogach J, Tsai S, Zbuk K, et al. Quality of preoperative pelvic computed tomography (CT) and magnetic resonance imaging (MRI) for rectal cancer in a region in Ontario: a retrospective populationbased study[J]. J Surg Oncol, 2018, 117(5): 1038-42. doi: 10.1002/jso.25000 [13] Jin XC, Zheng XM, Chen DD, et al. Prediction of response after chemoradiation for esophageal cancer using a combination of dosimetry and CT radiomics[J]. Eur Radiol, 2019, 29(11): 6080-8. doi: 10.1007/s00330-019-06193-w [14] Shen C, Liu ZY, Wang ZQ, et al. Building CT radiomics based nomogram for preoperative esophageal cancer patients lymph node metastasis prediction[J]. Transl Oncol, 2018, 11(3): 815-24. doi: 10.1016/j.tranon.2018.04.005 [15] Qu JR, Zhang HK, Wang ZQ, et al. Comparison between freebreathing radial VIBE on 3-T MRI and endoscopic ultrasound for preoperative T staging of resectable oesophageal cancer, with histopathological correlation[J]. Eur Radiol, 2018, 28(2): 780-7. doi: 10.1007/s00330-017-4963-0 [16] 常晓斌, 吴湘阳, 袁渊. 核磁共振弥散加权成像对局部晚期食管癌放疗靶区勾画的作用[J]. 西安交通大学学报: 医学版, 2017, 38(4): 611-6. https://www.cnki.com.cn/Article/CJFDTOTAL-XAYX201704030.htm [17] 赵醒艳. ADC值和标化ADC值对前列腺癌患者盆腔转移性淋巴结的诊断价值[J]. 临床放射学杂志, 2019, 38(1): 122-5. https://www.cnki.com.cn/Article/CJFDTOTAL-LCFS201901028.htm [18] 马晓超, 王盈舒, 王瑞, 等. 三维重建技术在食管癌术前诊断的临床应用价值[J]. 中国实验诊断学, 2019, 23(2): 203-6. https://www.cnki.com.cn/Article/CJFDTOTAL-ZSZD201902005.htm [19] 汪春, 孙华. DWI在食管癌放疗疗效及预后判定中的应用价值探讨[J]. 中国地方病防治杂志, 2017, 32(12): 1398-9. https://www.cnki.com.cn/Article/CJFDTOTAL-DYBF201712045.htm -







 下载:
下载: