Value of CT enhanced image texture analysis for predicting lymph node metastasis of esophageal squamous cell carcinoma
-
摘要:
目的探讨增强CT图像的纹理参数的预测食管鳞癌患者淋巴结转移的可行性。 方法选取本院在治疗之前行胸部CT增强扫描的食管鳞癌患者,共纳入51例患者,以术后病理结果为标准,依据有无淋巴结转移分为非淋巴结转移组、淋巴结转移组两组。非淋巴结转移组共24例,其中男20例,女4例,年龄40~77岁(63.5±9.4岁);淋巴结转移组共27例,其中男25例,女2例,年龄48~74岁(63.4±6.5岁)。将增强CT 图像(动脉期和静脉期)数据导入FireVoxel软件进行纹理分析,记录各纹理参数值包括均值、中位数、标准差、异质性、偏度、峰度、熵值。依据术后病理结果分为淋巴结转移组、非转移组,比较两组间纹理参数差异,利用ROC曲线分析CT纹理参数鉴别淋巴结转移的价值。 结果动脉期不均匀度、熵值在两组之间的差异有统计学意义(P<0.05);静脉期标准差、不均匀度、熵值纹理参数在两组之间的差异具有统计学意义(P<0.05)。动脉期不均匀度、熵值鉴别食管癌淋巴结转移的最佳临界值分别为0.017、3.891,曲线下面积为0.685、0.674。静脉期标准差、不均匀度及熵值对于鉴别食管癌淋巴结转移具有显著性意义,其中以熵值的曲线下面积最大(0.704),其最佳临界值为3.842,敏感度为70.4%,特异度为75%,对于食管癌淋巴结转移的鉴别具有一定的准确性。 结论增强CT图像(尤其是静脉期)的纹理分析有助于鉴别食管癌淋巴结转移,为食管癌术前无创性预测淋巴结转移提供帮助。 Abstract:ObjectiveTo explore the feasibility of texture analysis of enhanced CT images to predict the metastasis of lymphonodus in patients with esophageal squamous cell carcinoma. MethodsThe patients of esophageal squamous cell carcinoma in our hospital were selected. According to the pathological results, the patients were divided into lymphonodus metastasis group and non metastasis group. 51 patients with esophageal squamous cell carcinoma were included, 27 in lymphonodus metastasis group (25 males and 2 females with an average age of 63.4±6.5 years old) and 24 in non metastasis group (20 males and 4 females with an average age of 63.5±9.4 years old). The chest CT enhancement were performed before treatment. The enhanced CT images (arterial phase and venous phase) were imported into the Firevoxel software for texture analysis. The texture parameters were recorded including mean, median, standard deviation, heterogeneity, skewness, kurtosis and entropy. The differences of texture parameters between the two groups were analyzed. The value of CT texture parameters in identifying lymphonodus metastasis was analyzed by ROC curve. ResultsThere were significant differences in heterogeneity and entropy between the two groups in arterial phase (P< 0.05). There were significant differences in standard deviation, heterogeneity and entropy between the two groups in venous phase (P< 0.05). In arterial phase, the optimal cut-off values for the diagnosis of lymph node metastasis of esophageal cancer were heterogeneity and entropy and the areas under the curve were 0.685 and 0.674, respectively. In venous phase, the standard deviation, inhomogeneity and entropy had significant significance in distinguishing lymph node metastasis of esophageal cancer. Among them, the area under the curve of entropy was the largest (0.704), the best critical value was 3.842, the sensitivity was 70.4%, and the specificity was 75%. It had a certain accuracy for the diagnosis of lymph node metastasis of esophageal cancer. ConclusionThe texture analysis of enhanced CT images (especially the venous phase) is helpful to identify lymph node metastasis of esophageal cancer and provides help for noninvasive evaluation of lymph node metastasis before surgery. -
Key words:
- esophageal carcinoma /
- squamous cell carcinoma /
- lymph node metastasis /
- enhanced CT /
- texture analysis
-
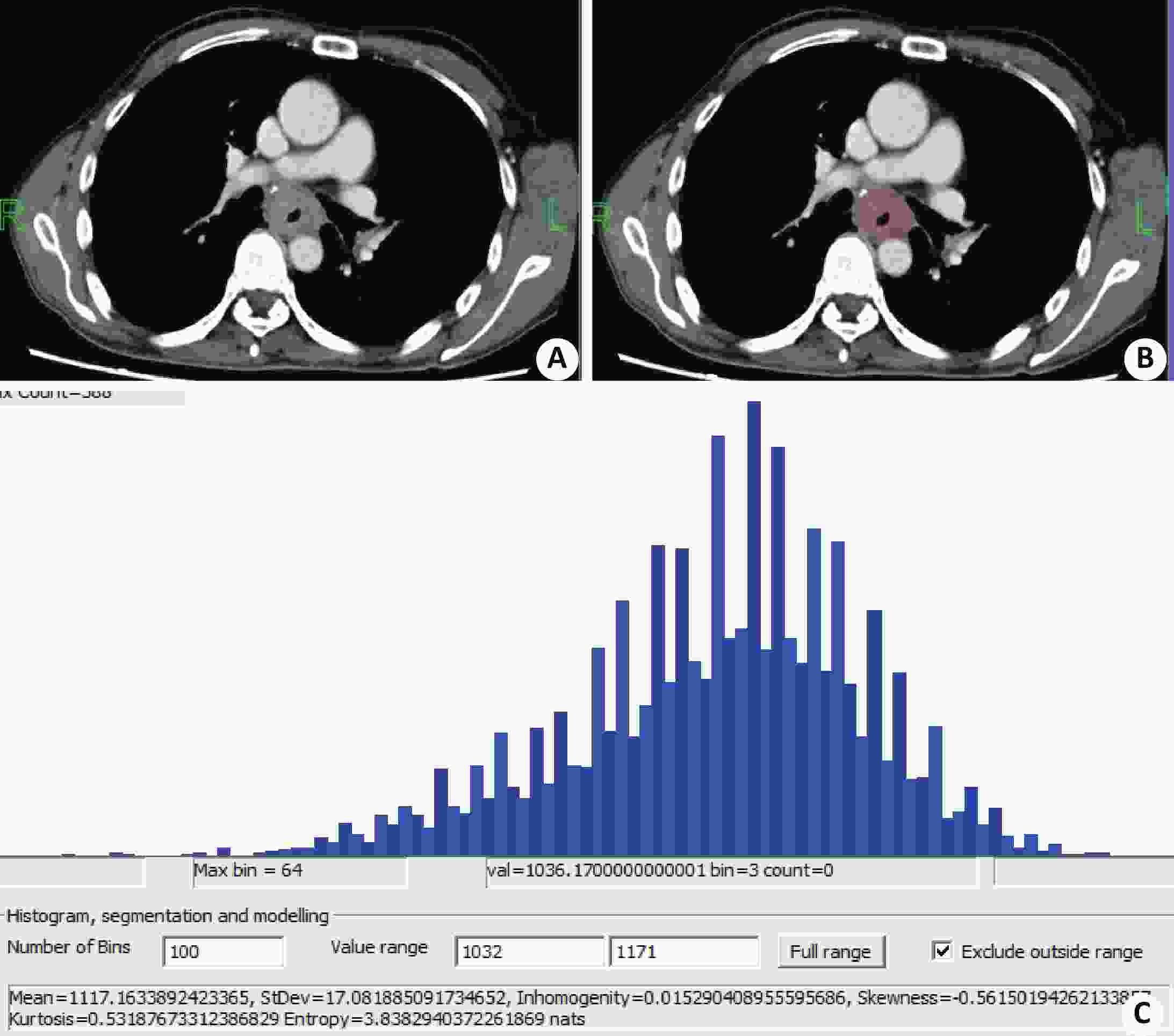
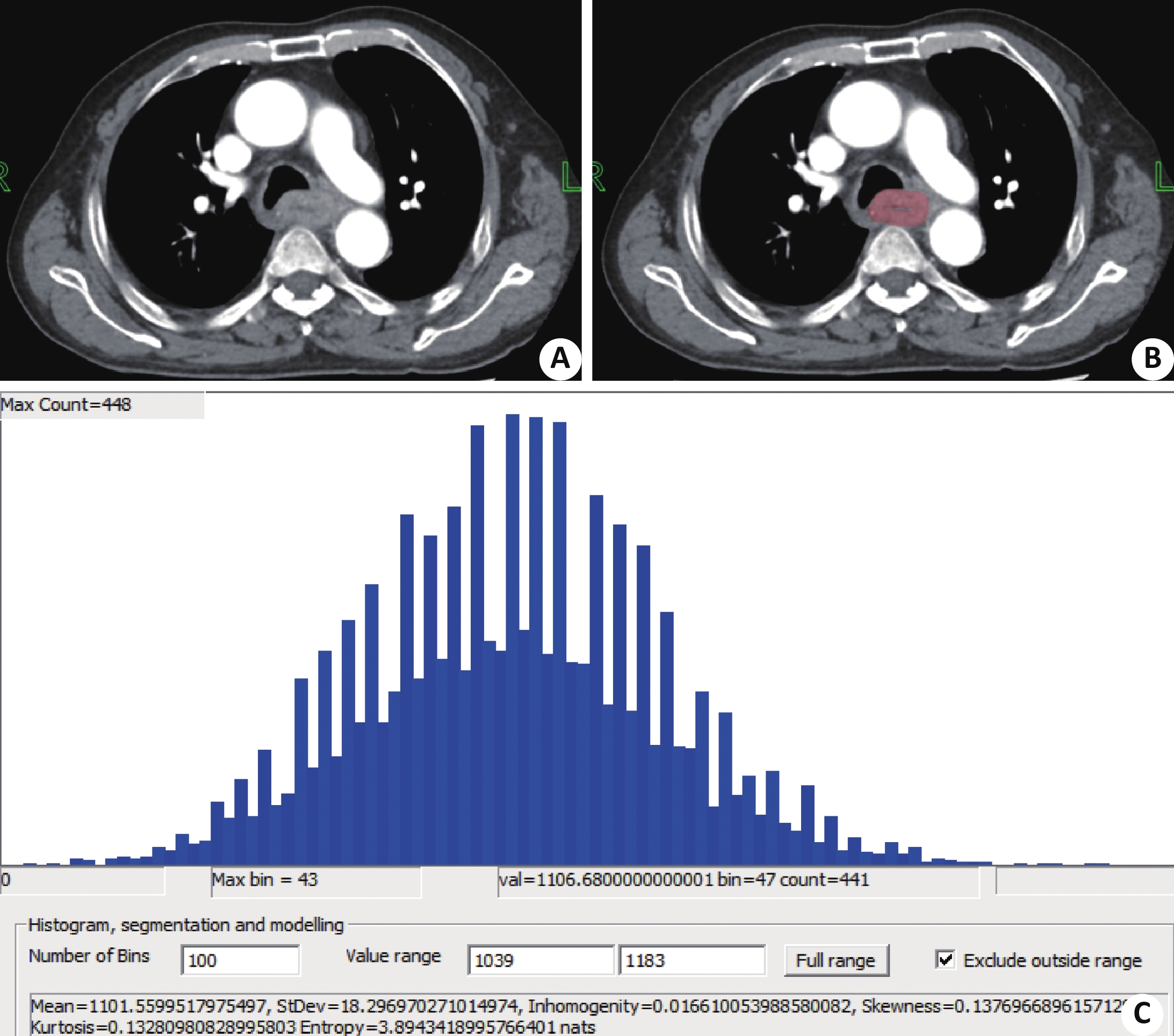
图 3 静脉期CT 纹理特征(转移组患者)
同图1患者;A:静脉期轴位图像;B:勾画示意图;C:及纹理分析输出结果.
Figure 3. CT texture features during venous phase (patients in metastatic group)
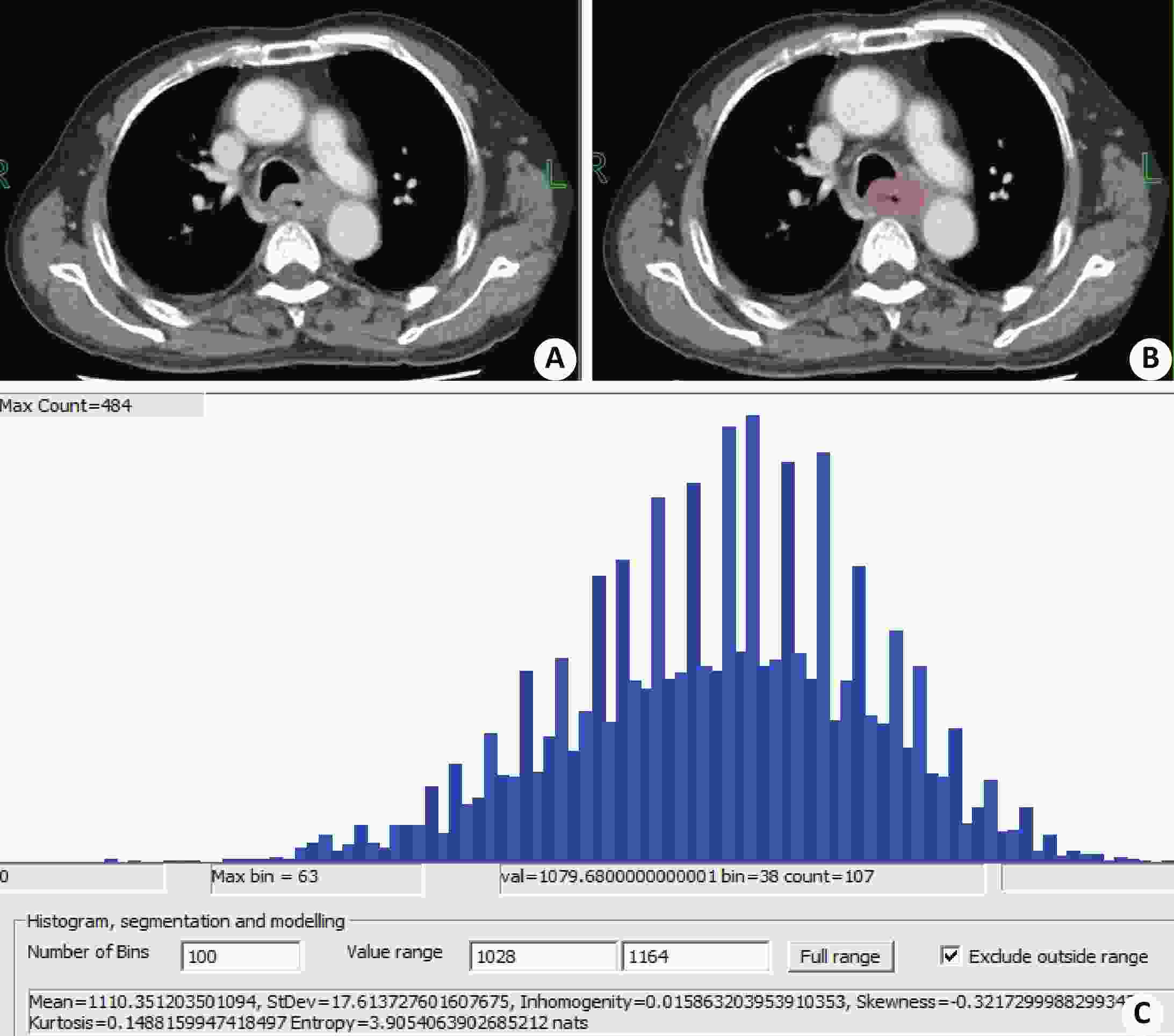
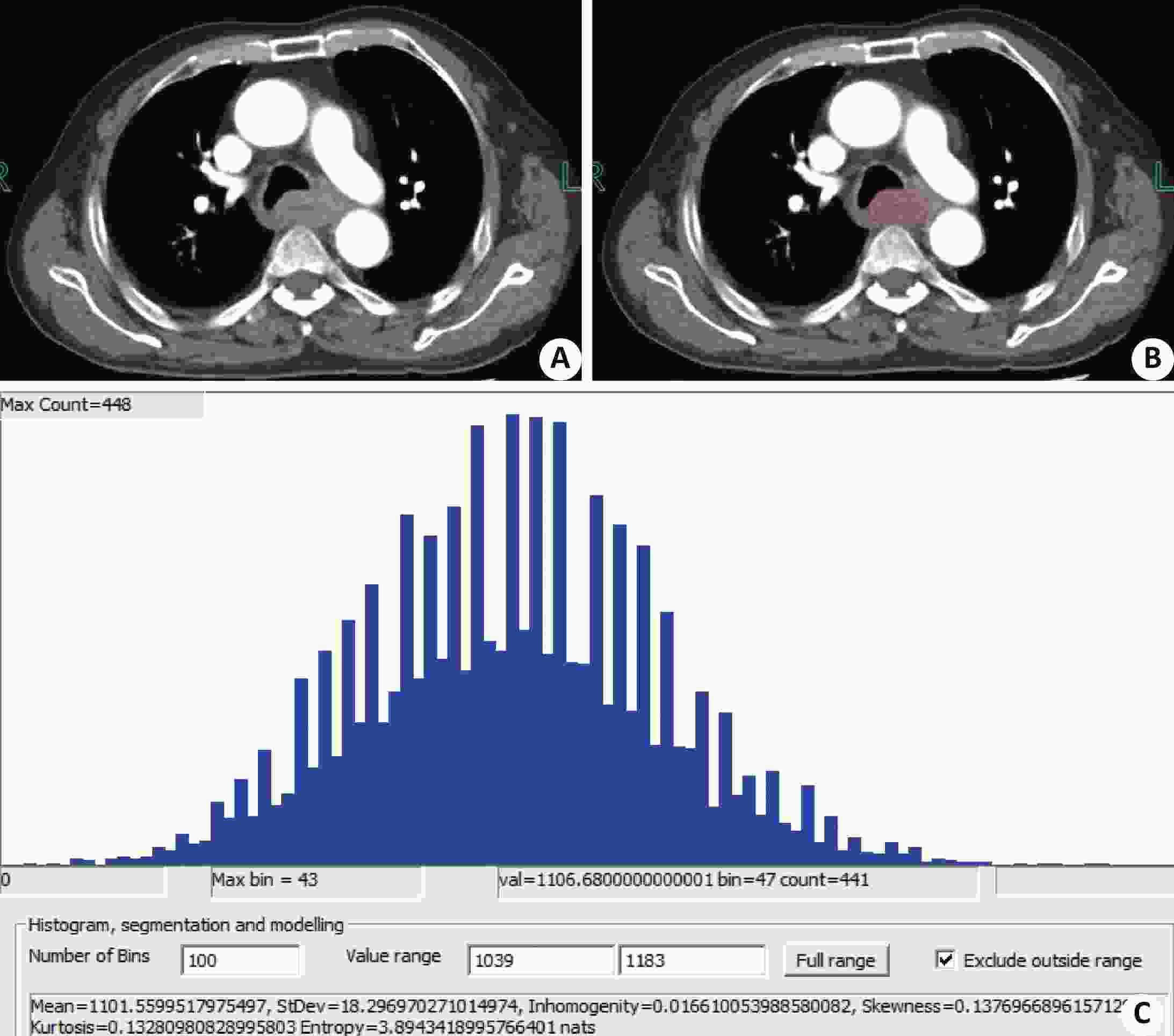
图 4 静脉期CT 纹理特征(非转移组患者)
同图2患者;A:静脉期轴位图像;B:勾画示意图;C:及纹理分析输出结果.
Figure 4. CT texture features during venous phase (non-metastatic patients)
表 1 动脉期食管癌淋巴结转移组与非转移组间纹理特征值比较(Mean±SD)
Table 1. Comparison of texture characteristic values between lymph node metastasis group and non-metastatic group in arterial esophageal carcinoma
分组 均值 中位数 标准差 不均匀度 偏度 峰度 熵值 非转移组 1 096.84±13.05 1 097.08±12.86 18.37±2.47 0.016±0.002 −0.119±0.340 0.843±0.611 3.696±0.206 转移组 1 094.44±14.02 1 094.30±13.77 19.66±3.83 0.019±0.005 −0.113±0.669 1.548±2.737 3.832±0.174 Z/t 0.629 0.744 −1.019 −2.265 −0.642 −0.189 −2.132 P 0.532 0.460 0.308 0.024 0.521 0.850 0.033 表 2 静脉期食管癌淋巴结转移组与非转移组间纹理特征值比较(Mean±SD)
Table 2. Comparison of texture characteristic values between lymph node metastasis group and non-metastatic group in vesophageal carcinoma at venous phase
分组 均值 中位数 标准差 不均匀度 偏度 峰度 熵值 非转移组 1 105.50±13.72 1 106.38±14.02 16.78±2.29 0.015±0.002 −0.359±0.302 0.727±0.692 3.797±0.142 转移组 1 100.82±11.84 1 101.74±11.57 18.46±2.56 0.017±0.003 −0.330±0.414 0.763±1.103 3.902±0.150 Z/t −0.811 0. 625 −2.462 −2.537 −0.277 −0.981 −2.541 P 0.417 0.189 0.017 0.014 0.783 0.326 0.014 表 3 动脉期CT纹理参数鉴别食管癌淋巴结转移的效能
Table 3. Effect of arterial CT texture parameters on differentiation of lymph node metastasis in esophageal carcinoma
纹理参数 界值 ROC曲线下面积 敏感度(%) 特异度(%) P 不均匀度 0. 017 0.685 66.7 66.7 0.024 熵值 3.891 0.674 44.4 95.8 0.033 表 4 静脉期CT纹理参数鉴别食管癌淋巴结转移的效能
Table 4. Efficacy of CT texture parameters in differentiating lymph node metastasis from esophageal carcinoma
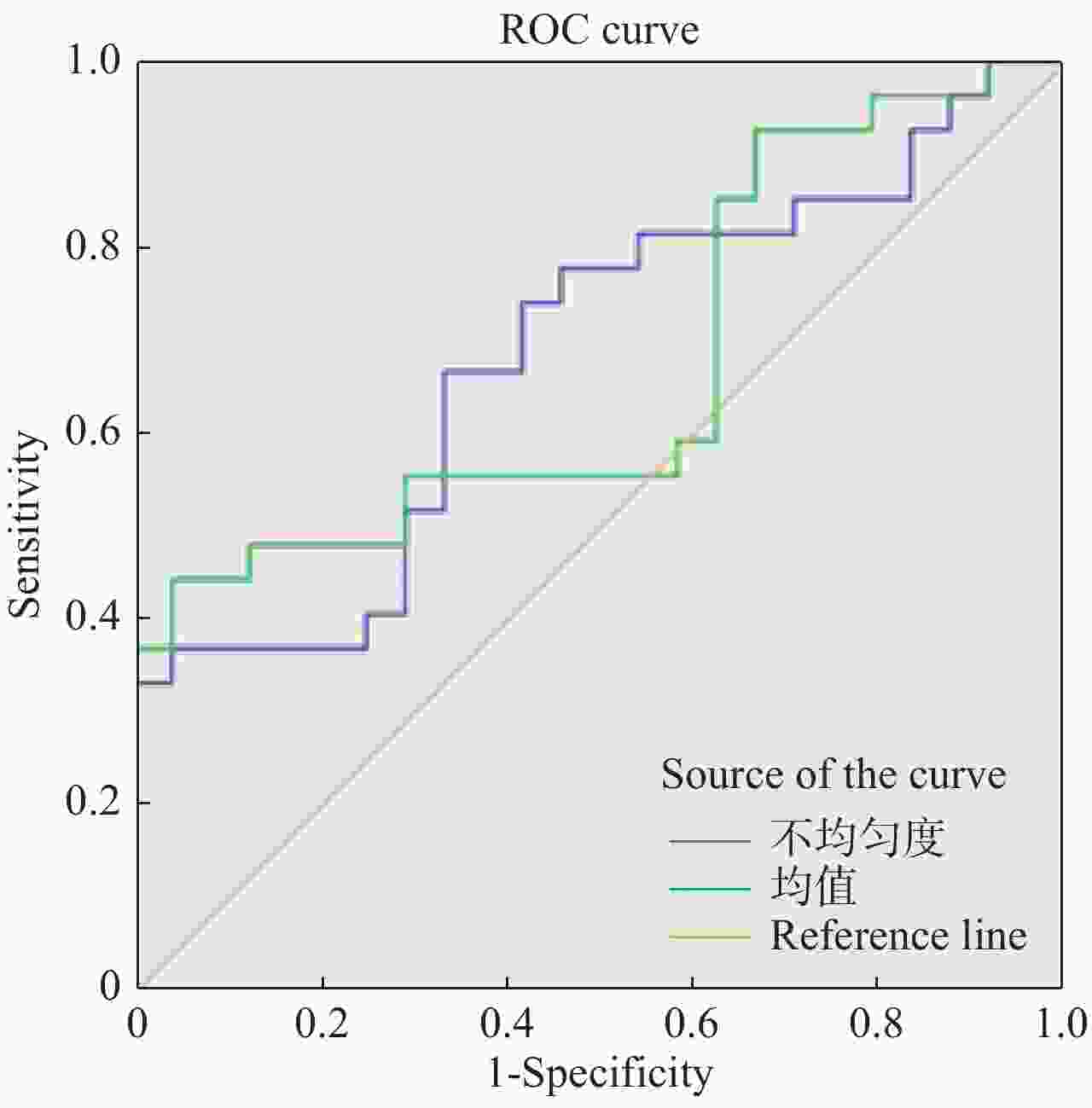
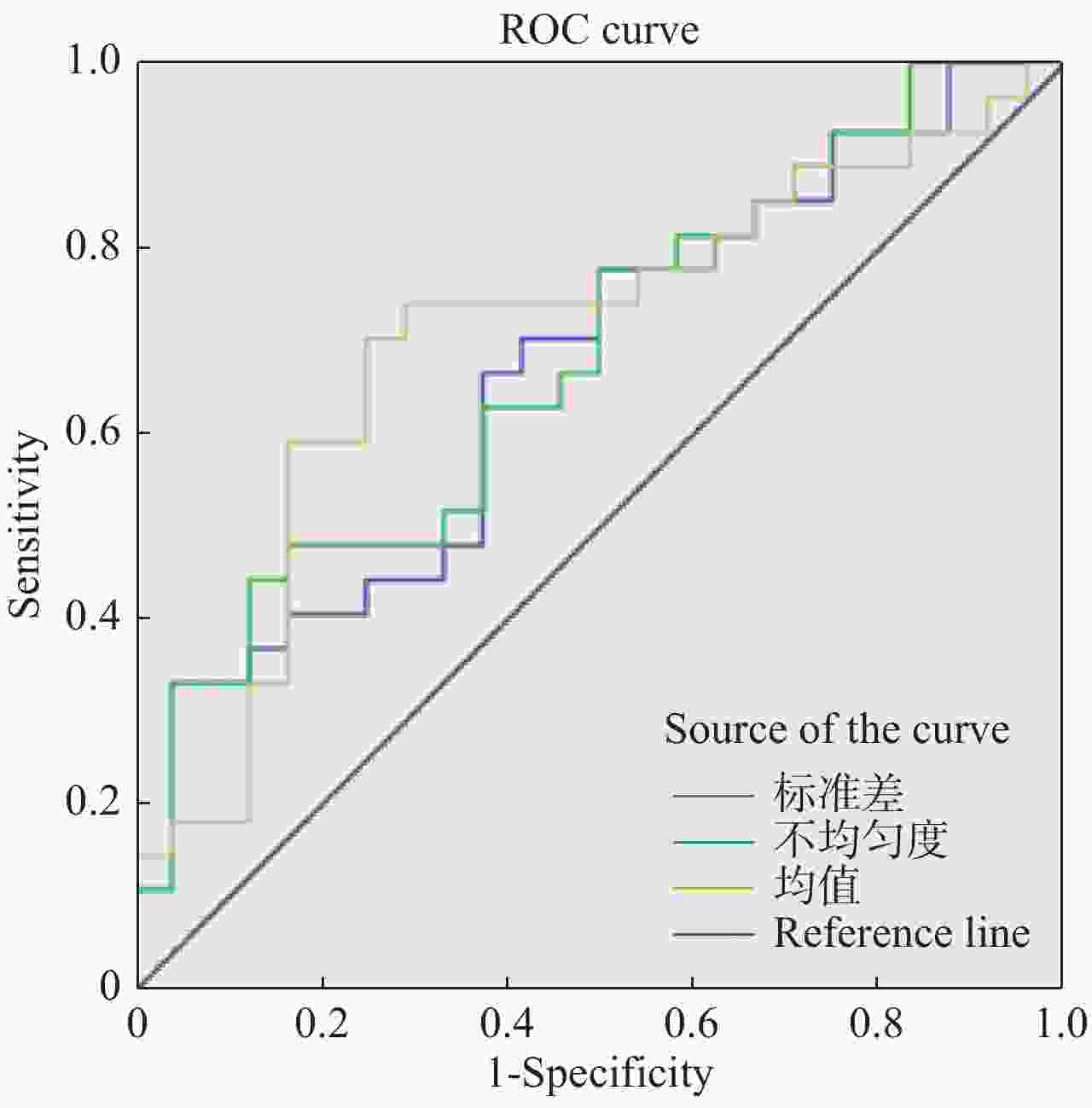
纹理参数 界值 ROC曲线下面积 敏感度(%) 特异度(%) P 标准差 17.538 0.668 66.7 62.5 0.040 不均匀度 0. 017 0.682 44.4 87.5 0.026 熵值 3.842 0.704 70.4 75 0.013 -
[1] Li Q, Wu SG, Gao JM, et al. Impact of esophageal cancer staging on overall survival and disease-free survival based on the 2010 AJCC classification by lymph nodes[J]. J Radiat Res, 2013, 54(2): 307-14. doi: 10.1093/jrr/rrs096 [2] 邓文英, 魏 辰, 李 宁, 等. 食管癌根治术后患者淋巴结转移与预后的关系[J]. 中华医学杂志, 2016, 96(47): 3829-32. doi: 10.3760/cma.j.issn.0376-2491.2016.47.013 [3] Cho JW, Choi SC, Jang JY, et al. Lymph node metastases in esophageal carcinoma: an endoscopist's view[J]. Clin Endosc, 2014, 47(6): 523-9. doi: 10.5946/ce.2014.47.6.523 [4] 陈文静, 牟 伟, 张文馨. 平扫T2脂肪抑制序列图像纹理可提高诊断乳腺良恶性结节的准确率[J]. 分子影像学杂志, 2019, 39(4): 453-6. [5] Ganeshan B, Miles KA. Quantifying tumour heterogeneity with CT[J]. Cancer Imaging, 2013, 13(1): 140-9. doi: 10.1102/1470-7330.2013.0015 [6] Feng Z, Rong P, Cao P, et al. Machine learning-based quantitative texture analysis of CT images of small renal masses: Differentiation of angiomyolipoma without visible fat from renal cell carcinoma[J]. Eur Radiol, 2018, 28(4): 1625-33. doi: 10.1007/s00330-017-5118-z [7] 刘震昊, 石家源, 王海屹, 等. 基于CT图像的纹理分析在膀胱癌不同病理级别鉴别中的价值[J]. 中华肿瘤杂志, 2018, 40(5): 379-83. doi: 10.3760/cma.j.issn.0253-3766.2018.05.011 [8] Fu SR, Chen ST, Liang CH, et al. Texture analysis of intermediate-advanced hepatocellular carcinoma: prognosis and patients' selection of transcatheter arterial chemoembolization and sorafenib[J]. Oncotarget, 2017, 8(23): 37855-65. [9] 徐敬慈, 潘自来, 王胜裕, 等. 增强CT纹理分析对食管鳞癌转移性淋巴结的诊断价值[J]. 中国医学计算机成像杂志, 2019, 25(1): 27-31. doi: 10.3969/j.issn.1006-5741.2019.01.007 [10] 吴 标, 李月月, 兰 勇, 等. 螺旋CT增强扫描评价食管癌分化程度的价值[J]. 河北医药, 2018, 40(17): 2639-42. [11] 刘剑芳, 邵华飞, 屈 东, 等. 食管癌转移淋巴结多层螺旋CT诊断标准探讨[J]. 癌症进展, 2016, 14(1): 56-8. [12] Sgourakis G, Gockel I, Lyros O, et al. Detection of lymph node metastases in esophageal Cancer[J]. Expert Rev Anticancer Ther, 2011, 11(4): 601-12. doi: 10.1586/era.10.150 [13] 余莹莹, 赵艳萍, 周 永, 等. CT诊断早期宫颈癌淋巴结转移的价值[J]. 中国临床医学影像杂志, 2016, 39(8): 565-9. [14] 吴佩琪, 刘再毅, 何 兰, 等. 影像组学与大数据结合的研究现状[J]. 中华放射学杂志, 2017, 51(7): 554-8. doi: 10.3760/cma.j.issn.1005-1201.2017.07.023 [15] Lee J, Jain R, Khalil K, et al. Texture feature ratios from relative CBV Maps of perfusion MRI are associated with patient survival in glioblastoma[J]. Am J Neuroradiol, 2016, 37(1): 37-43. doi: 10.3174/ajnr.A4534 [16] 刘小静, 苗重昌, 周胜利. 双源 CT 能谱曲线在食管癌诊断及其病理分级中的应用价值[J]. 临床和实验医学杂志, 2016, 15(7): 692-5. doi: 10.3969/j.issn.1671-4695.2016.07.026 [17] 唐彩银, 张 继, 田为中. CT纹理分析在量化食管鳞状细胞癌T、N分期方面的评价[J]. 中国医疗设备, 2018, 33(11): 73-5, 98. doi: 10.3969/j.issn.1674-1633.2018.11.020 [18] Chen XH, Ren K, Liang P, et al. Spectral computed tomography in advanced gastric cancer: can Iodine concentration non-invasively assess angiogenesis[J]. World J Gastroenterol, 2017, 23(9): 1666-75. doi: 10.3748/wjg.v23.i9.1666 [19] 熊 瑶. CT纹理分析在评价胃癌TN分期及分化程度的应用研究[D]. 宁夏: 宁夏医科大学, 2019. [20] 彭文静, 徐 凯, 刘正立, 等. 乳腺X线图像纹理分析鉴别乳腺小结节良恶性的价值[J]. 中国医学影像学杂志, 2018, 26(12): 890-3, 898. doi: 10.3969/j.issn.1005-5185.2018.12.003 [21] 颜智敏, 冯智超, 曹 鹏, 等. 多层螺旋CT图像纹理分析对直肠癌转移性淋巴结的诊断价值[J]. 中华放射学杂志, 2017, 51(6): 432-6. doi: 10.3760/cma.j.issn.1005-1201.2017.06.007 [22] 谭红娜, 武明辉, 顾建钦, 等. 乳腺X线图像纹理特征预测乳腺癌腋窝淋巴结转移[J]. 中国医学影像技术, 2017, 33(12): 1774-8. -






 下载:
下载: