Expression of EFNA3 in colon cancer and its clinical significance
-
摘要:
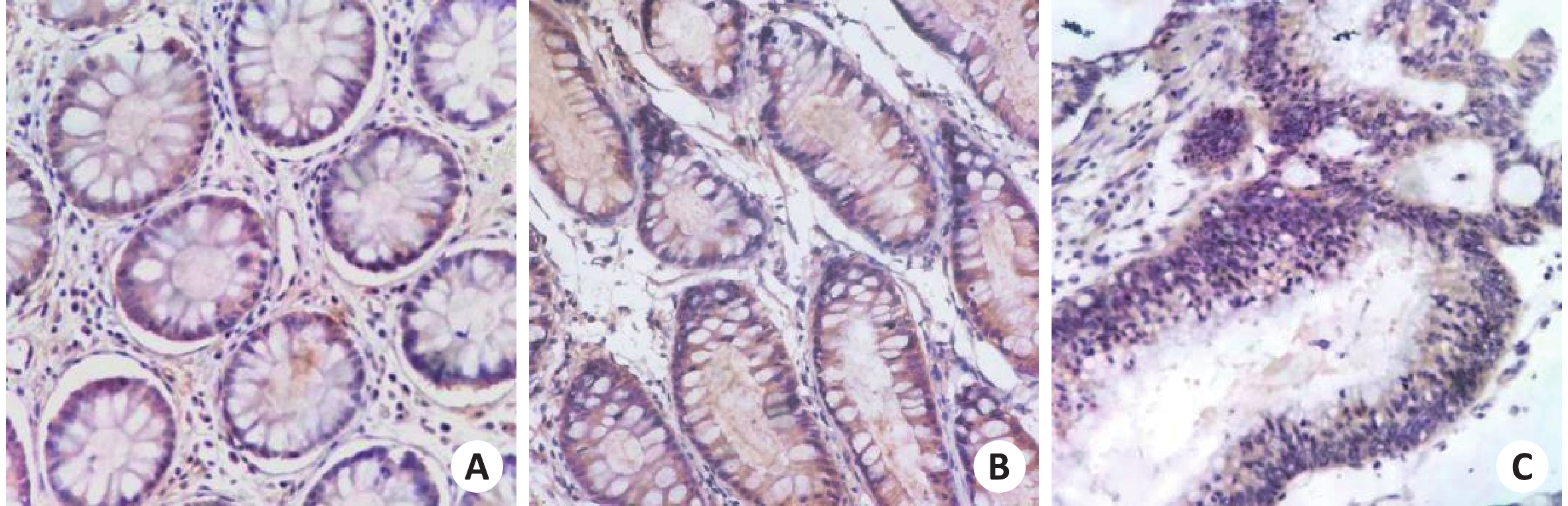
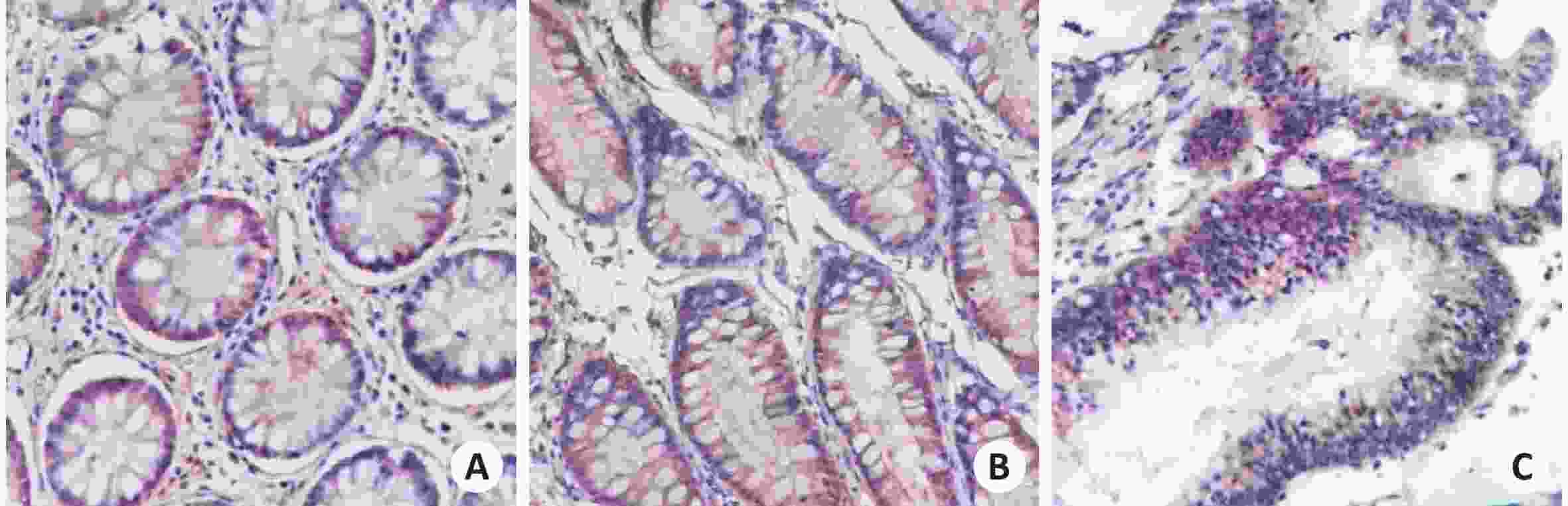
目的研究EFNA3在结直肠癌中的表达及关系。 方法随机选取湘南学院附属医院84例结直肠病例,分结直肠癌、结直肠良性肿瘤和正常结直肠组织3组,采用免疫组织化学方法分别检测3组中EFNA3的表达情况。 结果EFNA3在结直肠癌组中的表达强度为3.6±1.3,相比良性结直肠肿瘤组(5.1±0.6)和正常结直肠组(4.9±1.3)较低(P<0.05)。高分化组EFNA3表达量高于低分化组(4.2±0.4 vs 3.3±1.6,P<0.05);有淋巴结转移组肿瘤组织中EFNA3的表达量低于无淋巴结转移组(3.3±1.7 vs 4.13±0.28,P<0.05);TNM分期Ⅲ+Ⅳ者肿瘤组织中 EFNA3表达量低于Ⅰ+Ⅱ者(3.3±1.7 vs 4.13±0.28,P<0.05)。 结论EFNA3随着癌症发生过程的逐渐深入而表达递减,表明可能与结直肠癌的发生过程有关并在其中起到了类似抑癌基因的作用。 Abstract:ObjectiveTo investigate the expression of EFNA3 in colorectal cancer preliminary to explore the relationship between EFNA3 and colorectal cancer. MethodsA total of 84 colorectal cancer cases in XiangNan University affiliated hospital were randomly selected. They were divided into 3 groups: colorectal cancer, colorectal benign tumor and normal colorectal tissue. Immunohistochemistry was used to detect the expression of EFNA3 in 3 groups. ResultsExpression intensity of EFNA3 in colorectal cancer (3.6±1.3) was lower than that in colorectum benign tumor (5.1±0.6, P<0.05) and Normal colorectum (4.9±1.3, P<0.05). Compared with the expression of EFNA3 in the tumor tissues of well-differentiated group (4.2±0.4) and poorly differentiated group (3.3±1.6), the former was lower than the latter (P<0.05). The expression of EFNA3 in the tumor tissues in the lymphatic metastasis group (3.3±1.7) was lower than not (4.13±0.28) (P<0.05). Compared with the expression of EFNA3 in the tumor tissues people at Ⅲ+Ⅳ (3.3±1.7) and Ⅰ+Ⅱ (4.13±0.28) TNM staging, the former was lower than the latter (P<0.05). ConclusionThe expression of EFNA3 is lower in Colorectal cancer. Colorectum benign tumor and Normal colorectum have no significant difference. -
Key words:
- EFNA3 /
- colorectum cancer /
- immunohistochemistry
-
表 1 EFNA3的表达与结直肠癌临床病理特点的关系
组别 例数 EFNA3阳性评分(Mean±SD,分) P 临床分期 0.041 Ⅰ~Ⅱ期 18 4.13±0.28 Ⅲ~Ⅳ期 26 3.3±1.7 组织学分级 0.025 高分化 17 4.2±0.4 中低分化 27 3.3±1.6 淋巴结转移 0.041 是 26 3.3±1.7 否 18 4.13±0.28 -
[1] Bi CY. Correlation between preoperative serum LDL-C and HDL-C levels in patients with colorectal cancer and patho-logical staging of colorectal cancer[J]. JTCMUniv Hunan, 2016, 36(A01): 127-36. [2] Austin H, Henley SJ, King J, et al. Changes in colorectal cancer incidence rates in young and older adults in the United States: what does it tell us about screening[J]. Cancer Causes Control, 2014, 25(2): 191-201. doi: 10.1007/s10552-013-0321-y [3] Wan DS. Epidemiologic trend and strategies for colorectal cancer[J]. Chin J Cancer, 2009, 28(9): 897-902. doi: 10.5732/cjc.008.10833 [4] Parkin DM, Bray F, Ferlay J, et al. Global cancer statistics, 2002[J]. CA Cancer J Clin, 2005, 55(2): 74-108. doi: 10.3322/canjclin.55.2.74 [5] 孔 雁, 徐建梅, 刘风玲, 等. 直乙肠交界处癌与直肠癌及乙状结肠癌的预后比较[J]. 中国全科医学, 2015, 45(23): 2783-6. doi: 10.3969/j.issn.1007-9572.2015.23.009 [6] Luo H, Yu G, Wu Y, et al. EphB6 cross linking results in costimulation of T cells[J]. J Clin Invest, 2002, 110(8): 1141-50. doi: 10.1172/JCI0215883 [7] 傅 亚, 汤永红. miR-210在神经系统常见疾病中的研究进展[J]. 中南医学科学杂志, 2016, 44(4): 474-7. [8] Lisle JE, Mertens-Walker I, Rutkowski R, et al. Eph receptors and their ligands: promising molecular biomarkers and therapeutic targets in prostate cancer[J]. Biochim Biophys Acta, 2013, 1835(2): 243-57. [9] Oricchio E, Nanjangud G, Wolfe AL, et al. The Eph-receptor A7 is a soluble tumor suppressor for follicular lymphoma[J]. Cell, 2011, 147(3): 554-64. doi: 10.1016/j.cell.2011.09.035 [10] Pasquale EB. Eph-ephrin bidirectional signaling in physiology and disease[J]. Cell, 2008, 133(1): 38-52. doi: 10.1016/j.cell.2008.03.011 [11] Klein R. Bidirectional modulation of synaptic functions by Eph/ephrin signaling[J]. Nature, 2009, 12(1): 15-20. [12] Pasquale EB. Eph receptors and ephrins in cancer: bidirectional signalling and beyond[J]. Nature, 2010, 10(3): 165-80. [13] Fasnaaro P, Yuri O, Di Stefano. MicroRNA-210 modulates endothelial cell response to hyporia and inhibits the receptor tyrosine kinase ligand EphrinA3[J]. J Biol Chem, 2008, 23(19): 15878-83. [14] Devlin C, Greco S, Martelli F, et al. miR-210: more than a silent player in hypoxia[J]. IUBMB Life, 2011, 63(2): 94-100. [15] Iiizumi M, Hosokawa M, Takehara A, et al. EphA4 receptor, overexpressed in pancreatic ductal adenocarcinoma, promotes cancer cell growth[J]. Cancer Sci, 2006, 97(11): 1211-6. doi: 10.1111/j.1349-7006.2006.00313.x [16] 鲍留平, 仲建新. 卵巢癌中EphrinA3的表达及其意义的分析[J]. 国际妇产科学杂志, 2014, 41(2): 184-5, 209. [17] Kosaka N, Iguchi H, Hagiwara K, et al. Neutral sphingomyelinase 2 (nSMase2)-dependent exosomal transfer of angiogenic microRNAs regulate cancer cell metastasis[J]. J Biol Chem, 2013, 288(15): 10849-59. doi: 10.1074/jbc.M112.446831 [18] Fox BP, Kandpal RP. Invasion of breast carcinoma cells and transcript profile: Eph receptor and ephrin ligands and molecular markers of potential diagnostic and prognostic application[J]. Biochem Biophys Res Commun, 2004, 318(4): 882-92. doi: 10.1016/j.bbrc.2004.04.102 [19] Varelias A, Koblar SA, Cowled PA, et al. Human osteosarcoma expresses specific ephrin profiles: implications for tumorigenicity and prognosis[J]. Cancer, 2002, 95(4): 862-9. doi: 10.1002/cncr.10749 [20] Fox BP, Tabone CJ, Kandpal RP. Potential clinical relevance of Eph receptors and ephrin ligands expressed in prostate carcinoma cell lines[J]. Biochem Biophys Res Commun, 2006, 342(4): 1263-72. doi: 10.1016/j.bbrc.2006.02.099 -






 下载:
下载: