Clinical significance of MRI combined with serum BDNF and NSE in the diagnosis and outcome of newborns with hyperbilirubinemia
-
摘要:
目的探索MRI联合血清脑源性神经营养因子(BDNF)、神经元特异性烯醇化酶(NSE)对高胆红素血症患儿诊断及转归的临床意义。 方法选取2017年3月~2019年8月在本院住院患有高胆红素血症的新生儿60例作为研究对象,其中男34例,女26例,胎龄38.4±1.6周;同期选取在本院住院的新生儿40例作为对照组,男19例,女21例,胎龄37.8±1.5周,比较两组新生儿血清BDNF、NSE水平及转归情况;根据MRI影像学表现,将高胆红素血症患儿分为MRI异常组和MRI正常组,比较血清BDNF、NSE水平;考察MRI、BDNF、NSE作为诊断高胆红素血症的诊断价值。 结果高胆红素血症组临床转归总有效率为50.00%,低于对照组的75.00%,两组转归有效率的差异具有统计学意义(P < 0.05)。高胆红素血症组中54例(90.00%)患儿见MRI信号异常;对照组中6例(15.00%)见头颅MRI异常,差异有统计学意义(P < 0.05)。高胆红素血症组患儿NSE、BDNF表达均高于对照组(P < 0.05)。MRI异常组患儿血清NSE和BDNF水平高于MRI正常组(P < 0.05)。MRI联合血清BDNF、NSE对高胆红素血症的诊断效果高于单因素诊断。 结论MRI联合血清NSE、BDNF可为高胆红素血症患儿的早期诊断及转归提供观察依据。 -
关键词:
- MRI /
- 神经元特异性烯醇化酶 /
- 脑源性神经营养因子 /
- 高胆红素血症 /
- 新生儿
Abstract:ObjectiveTo explore the clinical significance of MRI combined with serum brain-derived neurotrophic factor (BDNF) and neuron-specific enolase (NSE) in the diagnosis and outcome of newborns with hyperbilirubinemia. MethodsSixtycases of newborns with hyperbilirubinemia in our hospital from March 2017 to August 2019 were selected as the research group, including 34 males and 26 females, with the age of 38.4±1.6 weeks. In the same period, 40 newborns in our hospital were selected as the control group, including 19 males and 21 females, with the age of 37.8±1.5 weeks. The serum BDNF and NSE levels of two groups were compared. According to MRI imaging findings, patients in research group was divided into MRI abnormal group and MRI normal group. The serum BDNF and NSE levels of the subgroup were compared. Finally, the diagnostic value of MRI, BDNF and NSE as the diagnosis of hyperbilirubinemia were analyzed. ResultsThe total effective rate of clinical outcomes in the hyperbilirubinemia group was 50.00%, which was lower than that in the control group (75.00%). The difference of the effective rates between two groups was significant(P < 0.05). In the hyperbilirubinemia group, 54 children with abnormal MRI were accounting for 90.00%. Six patients in the control group with abnormal MRI were accounting for 15.00%, and the difference between two subgroups was significant (P < 0.05). The level of serum NSE and BDNF in the research group were significantly higher than those in the control group (P < 0.05). Serum NSE and BDNF levels in children with abnormal MRI were significantly higher than those in normal MRI (P < 0.05). The diagnostic effect of MRI combined with serum BDNF and NSE on hyperbilirubinemia was higher than single factor diagnosis. ConclusionMRI combined with serum NSE and BDNF can provide observational basis for the early diagnosis and outcome of children with hyperbilirubinemia. -
Key words:
- MRI /
- neuron-specific enolase /
- brain-derived neurotrophic factor /
- hyperbilirubinemia /
- newborn
-
表 1 两组患儿转归情况比较[n(%)]
Table 1. Comparison of outcomes between two groups of children
组别 转归 有效率(%) 痊愈 好转 无效 高胆红素血症组 10 (16.67) 20 (33.33) 30 (50.00) 50.00 对照组 10 (25.00) 20 (50.00) 10 (25.00) 75.00 χ2 - - - 6.25 P - - - 0.012 表 2 两组患儿MRI检查结果比较[n (%)]
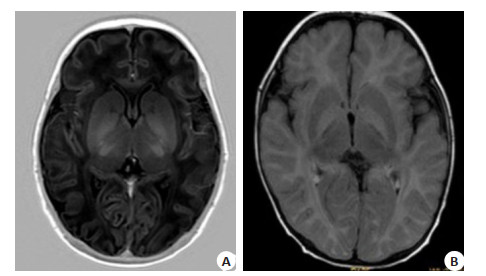
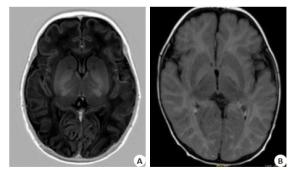
Table 2. Comparison of MRI results of two groups of children
组别 头颅MRI 正常 异常 高胆红素血症组(n=60) 22 (36.67) 38 (63.33) 对照组(n=40) 34 (85.00) 6 (15.00) χ2 22.754 P 0.000 表 3 两组患儿血清NSE和BDNF水平比较(Mean±SD, μg/L)
Table 3. Comparison of serum NSE and BDNF levels in three groups of children
组别 NSE BDNF 高胆红素血症组(n=60) 132.69±16.05 9.91±1.23 对照组(n=40) 79.71±7.67 6.45±0.78 χ2 19.427 15.786 P 0.000 0.000 表 4 高胆红素血症患儿中MRI异常组与正常组血清NSE和BDNF水平比较(Mean±SD, μg/L)
Table 4. Comparison of serum NSE and BDNF levels in MRI abnormal group and normal group in children with hyperbilirubinemia
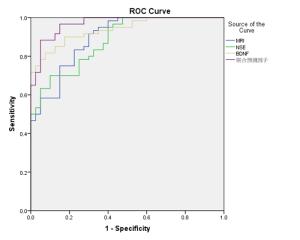
组别 NSE BDNF MRI异常组(n=38) 139.38±16.64 10.70±0.73 MRI正常组(n=22) 121.14±3.91 8.55±0.47 t 5.044 12.384 P 0.000 0.000 表 5 高胆红素血症患儿NSE、BDNF和MRI诊断及3个指标联合诊断特征分析
Table 5. NSE, BDNF and MRI diagnosis of children with hyperbilirubinemia
指标 AUC 95%置信区间 敏感性(%) 特异性(%) 下限 上限 MRI 0.895 0.834 0.956 91.7 70.0 NSE 0.882 0.819 0.945 70.0 90.0 BDNF 0.937 0.894 0.980 78.3 99.5 联合预测因子 0.969 0.941 0.997 88.3 99.5 -
[1] 王世界, 李操, 李明星.回顾性分析43例足月窒息新生儿脑血流动力学与血清神经元特异性烯醇化酶(S-NSE)动态变化的临床意义[J].中国临床医学影像杂志, 2017, 28(7): 466-70. doi: 10.3969/j.issn.1008-1062.2017.07.003 [2] 李金胜. MRI在新生儿胆红素脑病患儿诊断中的应用价值[J].医疗装备, 2017, 30(19): 49-50. doi: 10.3969/j.issn.1002-2376.2017.19.027 [3] 张玉琴, 马君芳, 孟艳艳.中度创伤性脑损伤患者血清神经元特异性烯醇化酶、S100-β蛋白变化及其与认知功能障碍的相关性[J].中华创伤杂志, 2017, 33(10): 886-9. doi: 10.3760/cma.j.issn.1001-8050.2017.10.006 [4] 汪鸿, 王小燕, 吴梅荣, 等.儿童孤独症外周血生物学标记物研究[J].中国妇幼卫生杂志, 2018, 9(4): 15-9. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=zgfywszz201804004 [5] 杜志方, 杨素艳, 刘芳, 等.新生儿高胆红素血症血清脑源性神经营养因子的变化及意义[J].中国综合临床, 2016, 32(7): 654-6. doi: 10.3760/cma.j.issn.1008-6315.2016.07.022 [6] 邵肖梅, 叶鸿瑁, 丘小汕.实用新生儿学[M].北京:人民卫生出版社, 2011: 273. [7] 中华医学会儿科学分会新生儿学组, 《中华儿科杂志》编辑委员会.新生儿高胆红素血症诊断和治疗专家共识[J].中华儿科杂志, 2014, 52 (10): 745-8. doi: 10.3760/cma.j.issn.0578-1310.2014.10.006 [8] Sullivan J, Rockey DC. Diagnosis and evaluation of hyperbilirubinemia[J]. Curr Opin Gastroenterol, 2017, 33(3): 164-70. doi: 10.1097/MOG.0000000000000354 [9] 蒋宇桐.新生儿高胆红素血症的病因及相关因素研究[J].健康必读, 2019(31): 264-5. http://d.old.wanfangdata.com.cn/Periodical/lchc201703014 [10] 陈华友.神经元特异性烯醇化酶浓度变化与高胆红素血症后遗症的关系探究[J].吉林医学, 2017, 38(8): 1414-6. doi: 10.3969/j.issn.1004-0412.2017.08.007 [11] 王吉, 徐巧, 李超, 等.血清神经元特异性烯醇化酶在新生儿高胆红素血症脑损伤中的表达及对预后的影响[J].中国妇幼保健, 2016, 31(4): 770-1. http://d.old.wanfangdata.com.cn/Periodical/zgfybj201604041 [12] 李建瑜.游离胆红素预测新生儿胆红素脑病的研究进展[J].国际儿科学杂志, 2019, 46(8): 575-9. doi: 10.3760/cma.j.issn.1673-4408.2019.08.009 [13] 邬剑, 李慧玲.血清NSE及UCB检测新生儿高胆红素血症脑损伤的价值[J].医学信息, 2018, 31(15): 158-60. doi: 10.3969/j.issn.1006-1959.2018.15.052 [14] Tawk RG, Grewal SS, Heckman MG, et al. The relationship between serum neuron-specific enolase levels and severity of bleeding and functional outcomes in patients with nontraumatic subarachnoid hemorrhage[J]. Neurosurgery, 2016, 78(4): 487-91. doi: 10.1227/NEU.0000000000001140 [15] Haupt WF, Chopan G, Sobesky J, et al. Prognostic value of somatosensory evoked potentials, neuron-specific enolase, and S100 for short-term outcome in ischemic stroke[J]. J Neurophysiol, 2016, 115(3): 1273-8. doi: 10.1152/jn.01012.2015 [16] Parry SM, Peeples ES. The impact of hypoxic-ischemic brain injury on stem cell mobilization, migration, adhesion, and proliferation[J]. Neural Regen Res, 2018, 13(7): 1125-35. doi: 10.4103/1673-5374.235012 [17] 王琦, 张岩, 王文璐.新生儿胆红素脑病的危险因素及防治[J].中国妇幼保健, 2018, 33(22): 5153-5. http://d.old.wanfangdata.com.cn/Periodical/zgfybj201822034 [18] 徐晓妮, 张苏红, 王卫华, 等.新生儿急性胆红素脑病危险因素分析[J].医学临床研究, 2016, 33(4): 719-21. http://d.old.wanfangdata.com.cn/Periodical/xsekzz201404007 [19] Goksuluk H, Gulec S, Ozcan OU, et al. Usefulness of neuronspecific enolase to detect silent neuronal ischemia after percutaneous coronary intervention[J]. Am J Cardiol, 2016, 117 (12): 1917-20. doi: 10.1016/j.amjcard.2016.03.037 [20] 孙培丽.参芎注射液治疗急性脑梗死的临床疗效及对患者血清神经元特异性烯醇化酶、血清神经肽Y、S-100β水平的影响[J].中国临床医生杂志, 2017, 45(11): 47-9. doi: 10.3969/j.issn.2095-8552.2017.11.017 -






 下载:
下载: