Predictive effect of fetal heart rate in early pregnancy on pregnancy outcome in patients with RSA by ultrasonography
-
摘要:
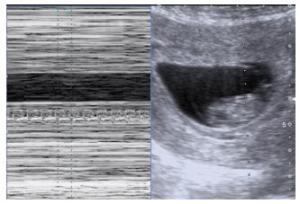
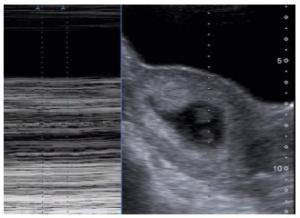
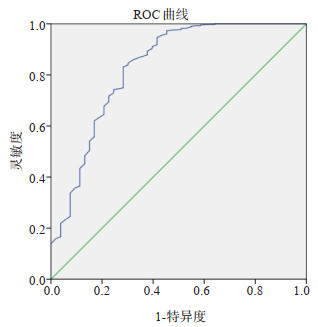
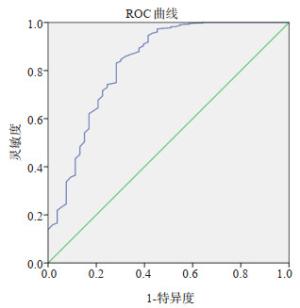
目的探讨超声检查习惯性流产(RSA)患者早孕期胎心率变化在妊娠结局预测中的作用。 方法收集行超声检查的妊娠42~69 d的孕妇,其中,有RSA病史孕妇255例,无RSA病史孕妇201例。根据妊娠42~196 d(即6~28周)期间妊娠结局分为3组:RSA异常妊娠组(有RSA病史孕妇本次妊娠期间发生自然流产);RSA正常妊娠组(有RSA病史孕妇本次妊娠至28周以上);非RSA正常妊娠组(无RSA病史孕妇本次妊娠至28周以上)。孕妇经腹或经阴道超声测量孕囊大小及胚芽、胎儿头臀长,启用M取样并放大模式测量胎心率,连续测量3次,取均值,记录孕囊大小、头臀长及胎心率,追踪随访至妊娠28周,比较各组间资料。 结果255例RSA孕妇中,83.0%的胚胎停育发生在55 d前,胎心率越低,胚胎停育发生率越高。超声检查与胚胎停育时间相隔越短,胎心率缓慢发生率越高。RSA正常妊娠组与非RSA正常妊娠组各孕龄平均胎心率的差异无统计学意义(P > 0.05)。RSA异常妊娠组与非RSA正常妊娠组孕49~62 d平均胎心率差异有统计学意义(P < 0.05),孕42~48 d和孕63~69 d平均胎心率之间差异无统计学意义(P > 0.05)。用胎心率为检验变量,妊娠结局为金标准,预测胎心率诊断的价值,曲线面积为0.831,结果具有统计学意义(P < 0.05)。 结论超声检查发现RSA患者早孕期胎心率缓慢对不良妊娠结局有一定的预测价值。 Abstract:ObjectiveTo explore the predictive effect of fetal heart rate in early pregnancy on pregnancy outcome in patients with RSA by ultrasonography. MethodsThe pregnant women with 42-69 days of gestation who were examined by ultrasound were collected. Among them, 255 pregnant women with RSA history and 201 pregnant women without RSA history were enrolled. According to the pregnancy outcome during 42-196 days (Pregnancy 6-28 weeks), the patients were divided into three groups: RSA abnormal pregnancy group: spontaneous abortion occurred during the pregnancy of the pregnant women with previous RSA history; RSA normal pregnancy group: the pregnancy of the pregnant women with previous RSA history was more than 28 weeks; non RSA normal pregnancy group: the pregnancy of the pregnant women without previous RSA history was more than 28 weeks. The size of gestational sac and the length of head and buttock (CRL) were measured by transabdominal or transvaginal ultrasound, and the fetal heart rate was measured by M sampling and amplification mode. The mean value was measured three times continuously, and the size of gestational sac, CRL and fetal heart rate were recorded. The data of each group were followed up to 28 weeks of gestation. The data of each group were compared. ResultsIn 255 cases of RSA, 83.0% of the pregnancies were terminated 8 weeks ago. The lower the fetal heart rate, the higher the rate of embryo termination. There was no significant difference between RSA normal pregnancy group and non RSA normal pregnancy group (P > 0.05). In RSA abnormal pregnancy group and non RSA normal pregnancy group, there was significant difference between the mean fetal heart rate at 7 and 8 weeks of gestation (P < 0.05), and there was no significant difference between the mean fetal heart rate at 6 and 9 weeks of gestation (P > 0.05). The fetal heart rate was used as the test variable, the pregnancy outcome was the gold standard, the diagnostic value of fetal heart rate was predicted, the area of the curve was 0.831, the results were statistically significant (P < 0.05). ConclusionThe slow fetal heart rate in early pregnancy of patients with RSA has a certain predictive value for the adverse pregnancy outcome. -
Key words:
- recurrent spontaneous abortion /
- fetal heart rate /
- early pregnancy /
- ultrasonography
-
表 1 3组孕妇孕龄和年龄的比较(Mean±SD)
Table 1. Comparison of gestational age and age among three groups of pregnant women
组别 孕龄(d) 年龄(岁) RSA异常妊娠组(n=53) 50.98±0.89 29.17±5.56 RSA正常妊娠组(n=202) 52.33±0.99 28.83±5.24 非RSA正常妊娠组(n=201) 50.78±0.99 27.80±4.69 F 2.723 2.749 P 0.067 0.065 表 2 非RSA正常妊娠组与RSA正常妊娠组各孕龄胎心率的比较(次/min, Mean±SD)
Table 2. The comparison of mean fetal heart rate between non RSA normal pregnancy group and RSA normal pregnancy group
孕龄(d) 非RSA正常妊娠组(n=201) RSA正常妊娠组(n=202) t P 42~48 124.39±16.78 121.79±16.09 0.750 0.455 49~55 146.48±17.83 140.73±17.07 1.843 0.068 56~62 161.15±20.44 162.71±14.13 -0.489 0.626 63~69 169.71±12.74 167.36±14.41 0.647 0.520 表 3 非RSA正常妊娠组与RSA异常妊娠组各孕龄胎心率的比较(次/min, Mean±SD)
Table 3. Comparison of the mean fetal heart rate of the non RSA normal pregnancy group and the RSA abnormal pregnancy group
孕龄(d) 非RSA正常妊娠组(n=201) RSA异常妊娠组(n=53) t P 42~48 124.39±16.78 112.50±31.35 1.873 0.066 49~55 146.48±17.83 111.76±31.03 5.964 < 0.000 56~62 161.15±20.44 95.24±23.65 12.172 < 0.000 63~69 169.71±12.74 168.00±7.55 0.225 0.824 -
[1] 谢幸, 孔北华, 段涛.妇产科学.第9版[M].北京:人民卫生出版社, 2018: 72. [2] 张丽梅, 杨燕宁, 张瑞晓, 等.自然流产两次与三次及以上的早期复发性流产患者病因构成的比较[J].中华妇产科杂志, 2018, 53(12): 855-9. doi: 10.3760/cma.j.issn.0529-567x.2018.12.010 [3] 赵鑫鑫, 张玉泉, 杨晓清.免疫相关的复发性流产治疗研究进展[J].中国计划生育和妇产科, 2020, 12(1): 20-4, 33. [4] 吴佩蔚, 胡旭, 崔莹, 等.复发性流产与夫妇染色体异常及多态性的关系[J].实用预防医学, 2020, 27(1): 78-80. doi: 10.3969/j.issn.1006-3110.2020.01.021 [5] Wu MJ, Liu P, Cheng LC. Galectin-1 reduction and changes in T regulatory cells may play crucial roles in patients with unexplained recurrent spontaneous abortion[J]. Int J Clin Exp Pathol, 2015, 8(2): 1973-8. http://cn.bing.com/academic/profile?id=3ccc947e7872bc58efd539fdacd24303&encoded=0&v=paper_preview&mkt=zh-cn [6] 乔杰.复发性流产孕前管理[J].中国实用妇科与产科杂志, 2018, 34 (12): 1309-14. http://d.old.wanfangdata.com.cn/Periodical/hbyx201606013 [7] 李朝媛, 蔡建姝.妊娠4周~9周不同妊娠结局者血清相关激素水平的变化[J].中国卫生检验杂志, 2017, 27(18): 2651-3, 2657. http://cdmd.cnki.com.cn/Article/CDMD-10081-1015016522.htm [8] 吕会娟, 刘玉玲, 陈瑞红, 等.血清孕酮、胰岛素生长因子-Ⅱ在预测妊娠早期不良结局中的作用[J].实用医学杂志, 2015, 31(8): 1251-3. doi: 10.3969/j.issn.1006-5725.2015.08.015 [9] 黄烨, 陈纬, 刁军成. Ca125、HCG、P对早期先兆流产患者妊娠结局预测的比较[J].重庆医科大学学报, 2016, 41(3): 253-6. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=cqykdxxb201603008 [10] 郑明明.早孕期超声胎儿结构筛查的效率及意义[J].实用妇产科杂志, 2018, 34(11): 809-11. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=syfckzz201811004 [11] 王晓红, 金雪鸿, 陈鹏龙, 等.妊娠第7周超声检查指标和血清孕酮水平对自发性流产的预测价值研究[J].中国全科医学, 2017, 20(13): 1582-6. doi: 10.3969/j.issn.1007-9572.2017.13.011 [12] 莫秀梅.自发性流产患者妊娠第7周超声检查指标的变化及意义[J].河北医学, 2018, 24(9): 1571-4. doi: 10.3969/j.issn.1006-6233.2018.09.044 [13] 龚晓萍, 王冠杰, 王海飞, 等.超声监测早孕期胚胎心率对妊娠结局的预测价值[J].中华超声影像学杂志, 2018, 27(11): 982-5. doi: 10.3760/cma.j.issn.1004-4477.2018.11.014 [14] 李胜利.对中国医师协会超声医师分会《产前超声检查指南(2012)》的深入解读[J].中华医学超声杂志:电子版, 2014, 11(4): 266-82. http://d.old.wanfangdata.com.cn/Periodical/zhyxcszz201404001 [15] 沈洁, 陈松, 张晓航, 等.孕早期胎儿心脏结构的超声筛查[J].中国介入影像与治疗学, 2016, 13(5): 293-6. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=zgjryxyzlx201605009 [16] 李胜利, 罗国阳.胎儿畸形产前超声诊断学[M].北京:科学出版社, 2017: 137. [17] Hanprasertpong T, Phupong V. First trimester embryonic/fetal heart rate in normal pregnant women[J]. Arch Gynecol Obstet, 2006, 274 (5): 257-60. doi: 10.1007/s00404-006-0176-5 [18] 李喜红, 殷斌, 欧阳妍, 等.早孕期胎心率与妊娠结局的相关性[J].中国现代医学杂志, 2013, 23(28): 76-9. doi: 10.3969/j.issn.1005-8982.2013.28.019 [19] 马西蕊, 刘纯钢.超声检查孕早期胎心率对妊娠结局的预测价值[J].临床超声医学杂志, 2008, 10(6): 429, 431. http://d.old.wanfangdata.com.cn/Periodical/lccsyxzz200806027 [20] 兖娜娜, 杨菁.复发性流产的治疗进展[J].中华生殖与避孕杂志, 2018, 38(11): 951-6. http://d.old.wanfangdata.com.cn/Periodical/zgsyjkzz201701026 [21] 冯卫彤, 王欢华, 古衍.不明原因早期复发性流产患者的宫腔镜检查[J].分子影像学杂志, 2015, 38(3): 239-41. doi: 10.3969/j.issn.1674-4500.2015.03.20 [22] ESHRE Guideline Group on RPL, Bender Atik R, Christiansen OB, et al. ESHRE guideline: recurrent pregnancy loss[J]. Hum Reprod Open, 2018, 2018(2): 1-12. http://d.old.wanfangdata.com.cn/NSTLQK/NSTL_QKJJ0234114571/ [23] 郭松, 张建平.复发性流产患者早期妊娠胚胎丢失的预测[J].中国实用妇科与产科杂志, 2017, 33(11): 1112-7. http://d.old.wanfangdata.com.cn/Conference/8877752 [24] 李荣, 漆洪波. 2018年ACOG"早孕期妊娠丢失指南"解读[J].中国实用妇科与产科杂志, 2019, 35(11): 1229-32. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=zgsyfkyckzz201911012 [25] 冯敏芝, 伍诗媚, 李建聪.超声在妊娠合并卵巢肿瘤患者的诊断价值[J].分子影像学杂志, 2019, 42(4): 439-43. doi: 10.12122/j.issn.1674-4500.2019.04.04 -






 下载:
下载: